|
Statistics were not available on the
number or type of CHW employers. Therefore,
estimates were derived from the data used
to identify the total of paid and volunteer
CHWs engaged to assist in the delivery
of care to underserved communities.
Industry and Size
Estimates
The number of organizations employing
community health workers was estimated
to be approximately 6,300 for the Nation
as a whole. This is a rough approximation
obtained when the estimated national total
of CHWs is divided by the average number
of CHWs engaged by the employers surveyed
for the CHW National Employer Inventory
(CHW/NEI).[1]
The industries found to be more likely
to employ CHWs were "Individual and
Family Services" (21 percent), "Social
Advocacy Organizations" (14.2 percent),
"Outpatient Care Centers" (13.3
percent), and "Administration of
Education Programs" (12.9 percent).
Additional industries found to have CHWs
among their personnel, although less often,
included "Other Ambulatory Health
Care Services" (8.4 percent) and
"Office of Physicians" (5.3
percent).[2]
The sizes of the organizations engaging
CHWs are shown in Figure 5.1. The largest
percentage (43 percent) were firms employing
between five and 19 employees, 20 percent
had between 20 and 49 individuals on the
payroll, and another 19.1 percent fell
in the 50 to 249 employees category. Few
were "large" employers: 2.8
percent employed 250 to 499 individuals
and 2.3 percent had 500 or more employees.
About 12.5 percent of the firms had fewer
than five employees.
 [D] [D]
Source: Study file of CHW employers
whose industry affiliation could be verified
-- N=744
Perceived Benefits
of Hiring CHWs
The occupational characteristics of CHWs
that have been motivating employers to
hire them were identified by combining
findings from the employers' interviews
and information gleaned from the review
of the literature.
Generally, employers have hired community
health workers because they (a) learned
about their successful utilization in
professional journals,[3]
(b) believed that they were cost effective,[4]
(c) found that CHWs were capable of organizing
communities in developing comprehensive
health action plans,[5]
or (d) discovered that programs addressing
health disparities were more effective
when using one-to-one outreach by CHWs.[6]
Community health workers were viewed
as having contributed to more effective
delivery of health-related services because
they were (1) uniquely effective in gaining
access to hard-to-reach populations that
had been avoided by other health workers;[7]
(2) able to patiently coach clients in
culturally appropriate terms and induce
behavioral changes;[8]
(3) able to successfully communicate with
clients, by developing trusting and caring
relationships, to impart or gather information[9]
and motivate key decisions such as participating
in immunization programs;[10]
and (4) able to address certain client
needs such as adapting health regimens
to family and community dynamics.[11]
Recruitment
Strategies
Networking
has been the recruitment strategy used
most often by employers (74 percent).[12]
Churches and local businesses have been
successful intermediaries in attracting
qualified candidates, and clinic-based
programs have recruited among patients.[13]
Other recruitment methods ranged from
mass mailings[14]
to partnerships with existing volunteer
organizations.[15]
Fifty percent of the respondents to the
CHW/NEI reported referrals by community
members or CHW staff. Many employers (69
percent) complemented networking with
traditional advertising.
Funding Sources
Consistently,
in the national Inventory, in employers'
interviews and in the literature, the
prevalence of short-term funding and the
necessary reliance on multiple funding
sources were cited by employers and other
observers as a major barrier to the development
of the CHW workforce.[16]
Figure 5.2 shows that 66 percent of the
employers surveyed for the national Inventory
reported two or more sources of funding.
 [D] [D]
Source: CHW National Employer Inventory
(CHW/NEI) (2006), N=527
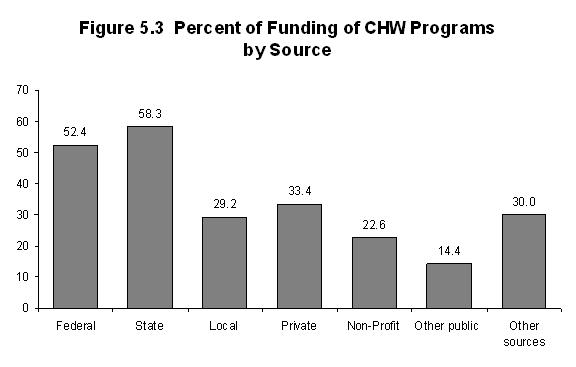
Figure 5.3 shows the percent of employers
by the type of agency that gave financial
support to the CHW programs. Federal and
State governments provided most of the
funds. Private organizations, local governments,
and other sources supported about one-third
of the employers. Similar patterns of
funding were found in most recent State
and local workforce studies on CHWs.[17]
 [D] [D]
Source: CHW/NEI (2006), N=527 - multiple
responses permitted
A 2006 study by the National Fund for Medical
Education (NFME) of the University of California
at San Francisco was the most current and
comprehensive account of how CHW programs
are financed.[18]
The study, titled Advancing Community
Health Worker Practice and Utilization,
The Focus on Financing, relied on a
comprehensive review of the literature and
structured interviews with 25 knowledgeable
informants representing 14 States plus the
District of Columbia who were either employers
or directly involved in educating, training,
financing, managing, or studying the CHW
workforce. The NFME study, confirming findings
from the CHW/NEI, concluded that prevailing
short-term funding induced frequent modifications
in program focus in response to changes
in priorities of funding sources. This hindered
the evolution of the CHW workforce.
The NFME study predicted that charitable
foundations, government grants, Medicaid,
State/Federal government general fund
appropriations, and private companies
will be the major potential funding sources
of the future.
The most successful CHW programs, reported
the NFME researchers, are those that (1)
have the mission of providing specific
services to underserved target populations,
(2) address the delivery of health care
holistically, that is, attending to the
total health needs of the population being
served, (3) have clearly identified unmet
health needs and intervention strategies,
(4) can document outcomes with solid data
indicating favorable changes in access,
cost, or health status, (5) are able to
attract the assistance of "champions"
who have leverage for winning support
for CHWs, and (6) can offer training to
the CHWs on the specific services needed.[19]
Sources of
Long-term Support
Health Resources
and Services Administration (HRSA)
HRSA funding has supported many CHW programs
nationally, principally through Federally
Qualified Health Centers of the Bureau
of Primary Health Care (BPHC) and Healthy
Start Programs of the Maternal and Child
Health Bureau (MCHB). Some of the programs
supported by the HIV/AIDS Bureau included
CHWs as "peer educators" or
"peer outreach workers." About
one-fourth of employers responding to
the "funding" section of the
national Inventory survey reported receiving
funding from HRSA or having a HRSA-sponsored
program (26 percent, N=634). A 2002 report
from the Health Resources and Services
Administration, MCHB listed examples of
programs from four Bureaus, and a partial
list of shorter-term project grants from
the Office of Rural Health Policy.[20]
The Health Education Training Centers
(HETC) program of the Bureau of Health
Professions (BHPr) was the only program
in HRSA with a specific legislative mandate
to support the CHW workforce. A report
for the 2004 National HETC Annual Meeting
described 42 CHW programs supported by
HETCs as "best practices."[21]
In conducting the in-depth investigations
of the selected States reported in Chapter
8, the following examples of HRSA support
were found.
Centro Familiar de Salud San Vicente
in El Paso, Texas, was a Federally Qualified
Health Center supporting promotor(a)
de salud (CHW) services in part from
its Public Health Service Act (PHSA) Section
330 funding. San Vicente's "Puente
de Salud" (Bridge of Health) program
received a 2003 Border Models of Excellence
award from the U.S.-Mexico Border Health
Commission. Promotoras served primarily
Hispanic residents who were economically
disadvantaged and uninsured by providing
community outreach education, access to
referral services, counseling, and group
presentations.[22]
Three Healthy Start grantees (HRSA/MCHB)
in Texas provided examples of how the
same funding source could support different
locally determined objectives and approaches.[23]
In Dallas, the objectives included reduction
of infant mortality, low birth-weight
and teen pregnancy. "Outreach Care
Workers" (another term for CHWs)
were used for case-finding, enrollment
and follow-up visits. Fort Worth's objectives
involved improving care coordination,
increasing rates of early prenatal care,
and increasing rates of immunization and
screening for post-partum depression;
there, the role of Outreach Workers was
limited to case-finding and enrollment
in informal community settings. In San
Antonio, the objectives included those
adopted by Dallas and Fort Worth, plus
maintenance of participants in interconceptional
care[24] for
up to 24 months post-delivery.
The New York State Department of Health
managed several streams of HRSA funding
including maternal and child health services
grants and maternal and child health community-integrated
services funds.[25]
The programs employed CHWs for outreach
to pregnant and parenting women, to newborns,
and to young children. The New York State
"Community Health Worker Program,"
addressing maternal and child health,
was perhaps the most widely recognized
CHW program in the State. This may have
been due to the fact that the program
had long-term funding.[26]
The AIDS Institute of the New York State
Department of Health (NYS DOH) managed
Federal funds from the Ryan White CARE
Act through contracts with community agencies
throughout the State. The Finger Lakes
Migrant Health Project in Rushville, New
York, employed CHWs in a promotor(a)
model, recruited from migrant camps. The
program was originally funded by the March
of Dimes and later by a Medical Expansion
Grant administered by HRSA. CHWs worked
in prenatal clinics to provide education
on infant and women's health issues and
assisted in outreach services to migrant
camps.[27]
Community health centers of Franklin
County, Massachusetts, received a Health
Center Cluster grant under the Section
330 Healthy Communities Access Program
(HCAP) from HRSA. The health center employed
two full-time "outreach representatives,"
both of whom were bilingual.[28]
One of the CHWs worked with seasonal migrant
farmworkers for half of the year, dedicating
the other half to the general population
of the health center. The outreach worker
assisted migrant workers by providing
transportation to health care appointments.
Outreach to the community was conducted
to inform residents about multiple issues
including insurance enrollment, housing,
nutrition, and other social and health
service needs.[29]
Community health centers in Arizona received
funding from HRSA for services that included
CHWs. The Mariposa Community Health Center's
Women's Health Program was partially funded
by HRSA/MCHB. Its CHWs provided linguistically
and culturally appropriate health information,
education, and referral, and led activities
with community members, especially new
community members, aimed at changing health
behaviors.[30]
The CHW programs at Chiricahua Community
Health Center and other community health
centers in Arizona provided health education
and home visitation.[31]
The
Office of Family Planning of the Office
of Population Affairs (OPA), United States
Department of Health and Human Services
(USDHHS)[32]
The Family Planning Program is administered
within the OPA, although its budget line
is located within HRSA. In addition to
family planning services and related counseling,
Title X[33]
supported clinics and provided preventive
health services. For many clients, Title
X clinics were the only continuing source
of care and health education. The program
supported a nationwide network of approximately
4,600 clinics delivering reproductive
health services to approximately 5 million
persons each year.[34]
Planned Parenthood was an example of a
Title X Family Planning Delegate that
received funds and employed CHWs at clinics
throughout the country, including California,
New York, and Texas.
Community Health
Representative (CHR) Program of the Indian
Health Service (IHS)
This program is the largest and the longest
standing in the United States. The CHR
Program was initially funded by the Office
of Economic Opportunity (OEO) in 1967
as the Community Health Aide Program,
and was transferred to IHS gradually from
1969 to 1972. The original intent of IHS,
modified somewhat through the years but
retaining its general goal, was for the
community health representatives (the
term used for CHWs) to become community
health promoters, educators, advocates,
and health paraprofessionals who would
regularly visit the homes of clients,
conduct health assessments, and provide
transportation when needed. Today, the
CHR Program has grown to more than 1,400
CHRs representing more than 250 tribes
in 12 service areas.[35]
Annual State Appropriations
A few programs were found to be supported
by annual State appropriations. The largest
of them were the Kentucky Homeplace/SKYCAP[36]
and the Arizona Health Start Program.[37]
Few local health departments employed
CHWs paid from ongoing revenue streams.[38]
Medicaid, State
Children's Health Insurance Program (SCHIP),
and Medicare
While some outreach programs have been
supported by Medicaid administrative
dollars, only a few programs involving
CHWs were established under Medicaid services
funding, generally under waivers or under
Medicaid-managed care plans. Of those
employers responding to the Inventory,
18.0 percent included reimbursement by
Medicaid and/or SCHIP.[39]
Perhaps the largest identified CHW programs
funded under Medicaid waivers have been
California's Family PACT Program, which
provided, among other services, family
planning under a waiver,[40]
and Alaska's Community Health Aide/Practitioner
(CHA/P) Program, primarily funded by the
Indian Health Service CHR Program and
authorized to bill Alaska Medicaid for
CHA/P services.[41]
Many community-based programs had contracts
with Medicaid and SCHIP managed care organizations
(MCOs) to provide CHW services. Some specific
programs were identified in rural New
Mexico[42]
and Rochester, New York.[43]
Medicaid and SCHIP MCOs typically have
wide latitude in the use of funding received
as capitation payments. At least one Medicaid
MCO had directly hired 50 CHWs on the
basis of internal return on investment.[44]
Another (CareFirst) received recognition
in 2006 from the National Committee for
Quality Assurance (NCQA) for its "Closing
the Gaps" program, which utilizes
CHWs, as an example of innovation in serving
linguistically and culturally diverse
populations.[45]
A 1997 study by Seedco for the Annie E.
Casey Foundation suggested that Medicaid-managed
care organizations (MCOs) would be amenable
to contracting for CHW services with community-based
agencies if agency capacity and CHW skills
standards were sufficiently high and,
further, that this "could provide
substantial revenues to support"
CHW positions.[46]
Other Medicaid support of CHW services
has followed different paths. For example,
the New York State Department of Health
funded local CHW services in 41 sites
in 2006 under its Prenatal Care Assistance
Program, which is part of the Medicaid
Program.[47]
Billing guidelines for HIV case management
programs funded by the State of New York,
as in other States, were specific in requiring
that only the services of the case manager
and the case management technician on
the service team were directly billable
to Medicaid. However, program guidelines
allowed the services of a community follow-up
worker (the equivalent of a CHW).[48]
Pilot projects for CHW Medicaid services
in Texas were authorized under House Bill
1864 in 1999, and the State Department
of Health committed $1 million per year
in combined Federal and State support
for five sites in 2001.[49]
The State sought and obtained approval
from the Centers for Medicare and Medicaid
Services (CMS) in 2003[50]
to use private matching funds for one
pilot site in Houston, but none of the
other sites received funding. A similar
situation arose for the "Community
Connectors" program serving mainly
the African-American elderly in rural
Southeastern Arkansas; the pilot program
was initially supported under Medicaid
administrative funding with private foundation
matching funds used for the Federal share
of funding.[51]
In 2006, the CMS funded six Cancer Patient
Navigator demonstration sites for assistance
to minority cancer patients on Medicare
fee-for-service benefits, although navigator
services were not a regular feature of
fee-for-service Medicare.[52]
No other examples of Medicaid, SCHIP,
and Medicare financing of services were
found.
For-Profit Firms
A growing area of support for CHWs was
found to be for-profit firms, both through
outsourcing and direct employment. The
increasingly large chronic disease management
industry has changed both the structure
of health care finance[53]
and the practice of medicine.[54]
In 2005, two for-profit disease management
firms known to be actively pursuing the
use of CHWs were among seven firms receiving
annual excellence awards from the Disease
Management Association of America.[55]
It is also conceivable that for-profit
health insurers in the Medicaid, Medicare,
and SCHIP programs may follow the lead
of non-profit insurers in utilizing CHWs.
However, most of the information on the
utilization of CHWs by for-profit organizations
has been treated as proprietary, sensitive
from a competitive viewpoint, and has
not been available for public dissemination.
Finally, private insurers may be considering
utilizing CHWs. They are already investing
heavily in wellness incentives, care management,
and the use of paraprofessionals. It is
likely that, as CHW capabilities and potential
become better known and documented, models
of CHW utilization may be considered for
health benefit plans for industries with
a high percentage of low-wage jobs. However,
no current examples of this type of CHW
employment could be located.
[1]
The estimates and the Inventory are discussed
in Chapter 3 and the methodologies employed
in each are explained in Appendix B and
Appendix C, respectively.
[2]
Employers identified during the National
survey were matched against listings from
the American Labor Market Information
System USA-INFO through a special confidentiality
agreement with the Texas Workforce Commission
(TWC) that protected individual firm records
and allowed the use of employers' information
only in large aggregates. These records
contained the North American Industry
Classification System (NAICS) codes of
employers as well as the number of total
employees, thus allowing the identification
of the industries engaging the majority
of paid and volunteer CHWs and their average
size. Of the verified employers in selected
States, 57 percent (759 of 1,327) were
successfully matched against the employer
records database. For the successfully
matched records, 92 percent (701 of 759)
corresponded to the industries identified
for inclusion in the estimates of paid
CHWs. (Additional information on the estimation
process, as well as the identification
of employers' industry, is available in
Appendix B.)
[3] Lam TK, McPhee SJ,
Mock J et al. Encouraging Vietnamese-American
women to obtain Pap tests through lay
health worker outreach and media education.
J Gen Intern Med 2003; 18 (7):516-24;
Baier C, Grant EN, Daugherty SR et al.
The Henry Horner Pediatric Asthma Program.
Chest 1999; 116 (4):204S-6S; Butz AM,
Malveaux FJ, Eggleston P et al. Use of
community health workers with inner-city
children who have asthma. Clin Pediatr
1994; 33 (3):135-41; Krieger JW, Takaro
TK, Song L et al. The Seattle-King County
Healthy Homes Project: a randomized, controlled
trial of a community health worker intervention
to decrease exposure to indoor asthma
triggers. Am J Public Health 2005; 95
(4):652-9; Stout J, White L, Rogers L
et al. The asthma outreach project: a
promising approach to comprehensive asthma
management. J of Asthma 1998; 35 (1):119-27.
[4] Findings from this
study's 36 employer interviews (CHW National
Workforce Study Interviews (CHW/NWSI))
conducted in four selected States. Note:
See also Barnes K, Friedman S, Namerow
P et al. Impact of community volunteers
on immunization rates of children younger
than 2 years. Arch Pediatr Adolesc Med
1999; 153 (5):518-24.
[5] Friedman AR, Butterfoss
FD, Krieger JW et al. Allies community
health workers: bridging the gap. Health
Promot Pract 2006; 7 (2 Suppl):96S-107S.
Note: In one example, seven local sites
of a national asthma control program independently
developed comprehensive community action
plans. The plans varied in approach; all
included significant roles for CHWs.
[6] Siegel B, Berliner
H, Adams A et al. Addressing Health Disparities
In Community Settings: An Analysis of
Best Practices in Community-Based Approaches
to Ending Disparities in Health Care.
Final Report to The Robert Wood Johnson
Foundation. Program In Health Services
Management and Policy, Robert J. Milano
Graduate School of Management and Urban
Policy, New School University & The
Robert Wood Johnson Foundation, December
20, 2001; Revised and Updated October,
2003.
[7] CHW/NWSI (2006);
Love MB, Gardner K. The Emerging Role
of the Community Health Worker in California.
Results of a Statewide Survey and San
Francisco Bay Area Focus Groups on the
Community Health Workers in California's
Public Health System. Community Health
Works of San Francisco, California Department
of Health Services, 1992.
[8] Staten LK, Gregory-Mercado
KY, Ranger-Moore J et al. Provider counseling,
health education, and community health
workers: the Arizona WISEWOMAN project.
J Womens Health (Larchmt) 2004; 13 (5):547-56;
Bone LR, Mamon J, Levine DM et al. Emergency
department detection and follow-up of
high blood pressure: use and effectiveness
of community health workers. Am J Emerg
Med 1989; 7 (1):16-20.
[9] Krieger J, Castorina
J, Walls M et al. Increasing influenza
and pneumococcal immunization rates: a
randomized controlled study of a senior
center-based intervention. Am J Prev Med
2000; 18 (2):123-31; Becker J, Kovach
AC, Gronseth DL. Individual empowerment:
how community health workers operationalize
self-determination, self-sufficiency,
and decision-making abilities of low-income
mothers. J Community Psychol 2004; 32
(3):327-42.
[10] Krieger J et al.
(2000).
[11] Rodney M, Clasen
C, Goldman G et al. Three evaluation methods
of a community health advocate program.
J Community Health 1998; 23 (5):371-81;
Meister JS, Warrick LH, de Zapien JG et
al. Using lay health workers: case study
of a community-based prenatal intervention.
J Community Health 1992; 17 (1):37-51.
[12] CHW/NEI (2006).
[13] Keyserling TC,
Ammerman AS, Samuel-Hodge CD et al. A
diabetes management program for African
American women with type 2 diabetes. Diabetes
Educ 2000; 26 (5):796-805.
[14] Andersen M, Yasui
Y, Meischke H et al. The effectiveness
of mammography promotion by volunteers
in rural communities. Am J Prev Med 2000;
18 (3):199-207.
[15] Barnes K et al.
(1999).
[16] Raczynski JM, Cornell
CE, Stalker V et al. Developing community
capacity and improving health in African
American communities. Am J Med Sci 2001;
322 (5):269-75; Rico C. Community Health
Advisors: Emerging Opportunities in Managed
Care. Annie E. Casey Foundation, Seedco--Partnerships
for Community Development, 1997; Rosenthal
EL, Wiggins N, Brownstein JN et al. The
Final Report of the National Community
Health Advisor Study. Tucson (AZ): University
of Arizona, 1998; Pew Health Professions
Commission. Community Health Workers:
Integral Yet Often Overlooked Members
of the Health Care Workforce. San Francisco
(CA): University of California Center
for the Health Professions, 1994; National
Fund for Medical Education. Advancing
Community Health Worker Practice and Utilization:
The Focus on Financing. San Francisco
(CA): Center for the Health Professions,
University of California at San Francisco,
2006; Brownstein JN, Bone LR, Dennison
CR et al. Community health workers as
interventionists in the prevention and
control of heart disease and stroke. Am
J of Prev Med 2005; 29 (5S1):128-33; Blue
Cross Foundation. Critical Links: Study
Findings and Forum Highlights on the Use
of Community Health Workers and Interpreters
in Minnesota. Eagan (MN): Blue Cross and
Blue Shield of Minnesota Foundation, 2003.
[17] Cowans S. Bay Area
Community Health Worker Study. [HED 892
- Final Report]. San Francisco (CA): San
Francisco State University, 2005. 29 p;
Results of the Southwestern Connecticut
Community Outreach Worker Survey. Bridgeport
(CT): Southwestern Area Health Education
Center and Housatonic Community College,
October 2000; Blue Cross Foundation (2003);
Massachusetts Department of Public Health.
Community Health Workers: Essential to
Improving Health in Massachusetts, Findings
from the Massachusetts Community Health
Worker Survey. Boston (MA): Division of
Primary Care and Health Access, Bureau
of Family and Community Health, Center
for Community Health, March 2005; Virginia
Center for Health Outreach. Final Report
on the Status, Impact, and Utilization
of Community Health Workers. Richmond
(VA): James Madison University, Institute
for Innovation in Health and Human Services,
2006; New Mexico Department of Health.
Senate Joint Memorial 076 Report on the
Development of a Community Health Advocacy
Program in New Mexico. Santa Fe (NM):
Department of Health, November 24, 2003;
Keane D, Nielsen C, Dower C. Community
health workers and promotores in California.
San Francisco (CA): UCSF Center for the
Health Professions, 2004.
[18] NFME (2006).
[19] Ibid (p.7).
[20] Health Resources
and Services Administration. Directory
of HRSA's Community Health Workers (CHWs)
Programs. Maternal and Child Health Bureau,
Health Resources and Services Administration,
U.S. Department of Health and Human Services
July 5, 2002. Note: Bureau of Health Professions,
Bureau of Primary Health Care, HIV/AIDS
Bureau, and Maternal and Child Health
Bureau.
[21] Health Education
and Training Centers (HETC) Community
Health Worker Best Practices Compendium.
National HETC Annual Meeting, 2004.
[22] United States-Mexico
Community Health Workers Border Models
of Excellence, Transfer/Replication Strategy.
Puente de Salud Model El Paso,
Texas. El Paso (TX): United States-Mexico
Border Health Commission, 2004.
[23] Project Abstract
- H49MC00114, Fort Worth Healthy Start
Initiative. Rockville (MD): Maternal and
Child Health Bureau, Health Resources
and Services Administration, U.S. Department
of Health and Human Services, 2001; Project
Abstract - H49MC00101, San Antonio Healthy
Start Project. Rockville (MD): Maternal
and Child Health Bureau, Health Resources
and Services Administration, U.S. Department
of Health and Human Services, 2001; Project
Abstract - H49MC00157, Dallas Healthy
Start: Eliminating Disparities in Perinatal
Health (General Population). Rockville
(MD): Maternal and Child Health Bureau,
Health Resources and Services Administration,
U.S. Department of Health and Human Services,
2001.
[24] This refers to
the care or services provided to women
between a birth/infant death/fetal loss
and a next pregnancy to address various
health and social conditions.
[25] CHW/NWSI (2006).
[26] Ibid.
[27] Ibid.
[28] Ibid.
[29] Ibid.
[30] United States-Mexico
Community Health Workers Border Models
of Excellence, Transfer/Replication Strategy.
Mariposa Community Health Center of Excellence
in Women's Health Model, Santa Cruz County,
Arizona. El Paso (TX): United States-Mexico
Border Health Commission, 2004.
[31] AACHC Program Overview
[Internet]. Phoenix (AZ): Arizona Association
of Community Health Care; 2006 [updated
2006/cited 2006 May 10]. Available from
http://www.aachc.org/programs.php.
[32] Office of Family
Planning [Internet]. Rockville (MD): Office
of Family Planning, Office of Population
Affairs, Office of Public Health and Science,
U.S. Department of Health and Human Services;
[updated 2006 Sep 16/cited 2006 Sep 26].
Available from http://opa.osophs.dhhs.gov/titlex/ofp.html.
[33] According to the
Office of Family Planning (OFP), Title
X is a Federal program solely dedicated
to family planning and reproductive health
with a mandate to provide a broad range
of acceptable and effective family planning
methods and services.
[34] Office of Family
Planning [Internet]. Rockville (MD): Office
of Family Planning, Office of Population
Affairs, Office of Public Health and Science,
U.S. Department of Health and Human Services;
[updated 2006 Sep 16/cited 2006 Sep 26].
Available from http://opa.osophs.dhhs.gov/titlex/ofp.html.
[35] General CHR Information,
History & Background Development of
the Program [Internet]. Rockville (MD):
Indian Health Service, U.S. Department
of Health and Human Services; [updated
2006 Mar 30/cited 2006 Oct 21]. Available
from http://www.ihs.gov/NonMedicalPrograms/chr/history.cfm.
[36] Center of Excellence
in Rural Health - Kentucky Homeplace [Internet].
Hazard (KY): University of Kentucky Chandler
Medical Center; 1999 [updated 2006 Sep
25/cited 2006 Oct 9]. Available from http://www.mc.uky.edu/RuralHealth/LayHealth/KY_Homeplace.htm.
[37] Office of Women's
and Children's Health - Health Start [Internet].
Phoenix (AZ): Arizona Department of Health
Services, Division of Public Health Services;
2006 [updated 2006 Sep 13/cited 2006 Oct
9]. Available from http://www.azdhs.gov/phs/owch/healthstart.htm.
[38] Fort Worth, TX;
San Francisco and Berkeley, CA.
[39] CHW National Employer
Inventory (CHW/NEI) (2006).
[40]
Gold RB. Special analysis: Medicaid
family planning expansions hit stride.
The Guttmacher Report on Public Policy
2003; 6 (4).
[41] Health Resources
and Services Administration. The Alaska
Community Health Aide Program: an Integrative
Literature Review and Visions for Future
Research. Office of Rural Health Policy,
Health Resources and Services Administration,
U.S. Department of Health and Human Services,
March 2003.
[42] NFME (2006).
[43] CHW/NWSI (2006).
[44] NFME (2006).
[45]
Ten Health Plans Recognized by NCQA
for Bridging Cultural and Linguistic Divides
in Health Care [Internet]. Washington
(DC): National Committee for Quality Assurance;
2006 [updated 2006 Sep 13/cited 2006 Sep
29]. Available from http://www.ncqa.org/Communications/News/CLAS_06.htm.
[46] Rico C (1997).
[47] Governor Pataki
Announces $8 Million in Funding for Family
Health Services, Perinatal Care. Initiative
Supports Expanded Access for Women to
These Vital Services [Internet]. Albany
(NY): New York State Governor's Page;
2006 [updated 2006 May 4/cited 2006 Sep
26]. Available from http://www.ny.gov/governor/press/06/0504061.html.
[48] Welcome to the
COBRA HIV/AIDS Case Management Website!
Who are We? [Internet]. Albany (NY): AIDS
Institute, New York State Department of
Health; 2002 [cited 2006 Sep 26]. Available
from http://www.cobracm.org/whoweare/.
[49] Promotora Program
Development Committee: Promotora Program
Development Committee Meeting Minutes
- for 2000 (August 17, 2000) [Internet].
Austin (TX): Texas Department of State
Health Services; 2000 [updated 2006 Oct
30/cited 2006 Sep 30]. Available from
http://archive.tdh.state.tx.us/legacytdh/ppdc/minutes_2000.htm#August%2017,%202000.
[50] Nichols DC, Berrios
C, Samar H. Texas' community health workforce:
from state health promotion policy to
community-level practice. Prev Chronic
Dis [Serial Online] 2005; 2:1-7.
[51] Rush C. Conversation
with: M. Kate Stewart. 2004 November 8.
Mr. Rush served as a consultant to this
project in 2001-2002 through the University
of Arkansas for Medical Sciences, Center
for Health Improvement.
[52] Awardees Cooperative
Agreement Summaries - Cancer Disparities
Demonstrations [Internet]. Baltimore (MD):
Centers for Medicare and Medicaid Services,
U.S. Department of Health and Human Services;
2005 [updated 2006 Oct 18/cited 2006 Sep
26]. Available from http://www.cms.hhs.gov/DemoProjectsEvalRpts/downloads/CPTD_Awardee.pdf.
[53] Bodenheimer T,
Fernandez A. High and rising health care
costs. Part 4: Can costs be controlled
while preserving quality? Ann Intern Med
2005; 143 (1):26-31.
[54] Casalino L. Disease
management and the organization of physician
practice. JAMA 2005; 293 (4):485-8.
[55] DMAA Recognizes
Excellence in Disease Management [Internet].
Washington (DC): Disease Management Association
of America; 2005 [updated 2006 Oct 18/cited
2006 Sep 26]. Available from http://www.dmaa.org/news_releases/2005/PressRelease10182005Excellence.html.
|