
|
 |
Lassa Fever
 View PDF (35KB View PDF (35KB
| What
is Lassa fever? |
 |
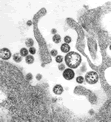 |
| Lassa
virus electron micrograph. Image courtesy, C.S. Goldsmith and M. Bowen
(CDC). |
Lassa fever is an
acute viral illness that occurs in West Africa. The illness was discovered
in 1969 when two missionary nurses died in Nigeria, West Africa. The cause
of the illness was found to be Lassa virus, named after the town in Nigeria
where the first cases originated. The virus, a member of the virus family
Arenaviridae, is a single-stranded RNA virus and is zoonotic, or animal-borne.
In areas of Africa
where the disease is endemic (that is, constantly present), Lassa fever
is a significant cause of morbidity and mortality. While Lassa fever is
mild or has no observable symptoms in about 80% of people infected with
the virus, the remaining 20% have a severe multisystem disease. Lassa
fever is also associated with occasional epidemics, during which the case-fatality
rate can reach 50%.
| Where
is Lassa fever found? |
 |
Lassa fever is an
endemic disease in portions of West Africa. It is recognized in Guinea,
Liberia, Sierra Leone, as well as Nigeria. However, because the rodent
species which carry the virus are found throughout West Africa, the actual
geographic range of the disease may extend to other countries in the region.
| How
many people become infected? |
 |
The number of Lassa
virus infections per year in West Africa is estimated at 100,000 to 300,000,
with approximately 5,000 deaths. Unfortunately, such estimates are crude,
because surveillance for cases of the disease is not uniformly performed.
In some areas of Sierra Leone and Liberia, it is known that 10%-16% of
people admitted to hospitals have Lassa fever, which indicates the serious
impact of the disease on the population of this region.
| In
what animal host is Lassa virus maintained? |
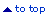 |
 |
 |
| |
Mastomys
rodent, also known as the "multimammate rat". Note
the hairless tail. |
The reservoir, or
host, of Lassa virus is a rodent known as the "multimammate rat"
of the genus Mastomys. It is not certain which species of Mastomys
are associated with Lassa; however, at least two species carry the
virus in Sierra Leone. Mastomys rodents breed very frequently,
produce large numbers of offspring, and are numerous in the savannas and
forests of West, Central, and East Africa. In addition, Mastomys
generally readily colonize human homes. All these factors together contribute
to the relatively efficient spread of Lassa virus from infected rodents
to humans.
| How
do humans get Lassa fever? |
 |
There are a number
of ways in which the virus may be transmitted, or spread, to humans. The
Mastomys rodents shed the virus in urine and droppings. Therefore,
the virus can be transmitted through direct contact with these materials,
through touching objects or eating food contaminated with these materials,
or through cuts or sores. Because Mastomys rodents often live in
and around homes and scavenge on human food remains or poorly stored food,
transmission of this sort is common. Contact with the virus also may occur
when a person inhales tiny particles in the air contaminated with rodent
excretions. This is called aerosol or airborne transmission. Finally,
because Mastomys rodents are sometimes consumed as a food source,
infection may occur via direct contact when they are caught and prepared
for food.
Lassa fever may also
spread through person-to-person contact. This type of transmission occurs
when a person comes into contact with virus in the blood, tissue, secretions,
or excretions of an individual infected with the Lassa virus. The virus
cannot be spread through casual contact (including skin-to-skin contact
without exchange of body fluids). Person-to-person transmission is common
in both village and health care settings, where, along with the above-mentioned
modes of transmission, the virus also may be spread in contaminated medical
equipment, such as reused needles (this is called nosocomial transmission).
| What
are the symptoms of Lassa fever? |
 |
Signs and symptoms
of Lassa fever typically occur 1-3 weeks after the patient comes into
contact with the virus. These include fever, retrosternal pain (pain behind
the chest wall), sore throat, back pain, cough, abdominal pain, vomiting,
diarrhea, conjunctivitis, facial swelling, proteinuria (protein in the
urine), and mucosal bleeding. Neurological problems have also been described,
including hearing loss, tremors, and encephalitis. Because the symptoms
of Lassa fever are so varied and nonspecific, clinical diagnosis is often
difficult.
| How
is the disease diagnosed in the laboratory? |
 |
Lassa fever is most
often diagnosed by using enzyme-linked immunosorbent serologic assays
(ELISA), which detect IgM and IgG antibodies as well as Lassa antigen.
The virus itself may be cultured in 7 to 10 days. Immunohistochemistry
performed on tissue specimens can be used to make a post-mortem diagnosis.
The virus can also be detected by reverse transcription-polymerase chain
reaction (RT-PCR); however, this method is primarily a research tool.
| Are
there complications after recovery? |
 |
The most common complication
of Lassa fever is deafness. Various degrees of deafness occur in approximately
one-third of cases, and in many cases hearing loss is permanent. As far
as is known, severity of the disease does not affect this complication:
deafness may develop in mild as well as in severe cases. Spontaneous
abortion is another serious complication.
| What
proportion of people die from the illness? |
 |
Approximately 15%-20%
of patients hospitalized for Lassa fever die from the illness. However,
overall only about 1% of infections with Lassa virus result in death.
The death rates are particularly high for women in the third trimester
of pregnancy, and for fetuses, about 95% of which die in the uterus of
infected pregnant mothers.
| How
is Lassa fever treated? |
 |
Ribavirin, an antiviral
drug, has been used with success in Lassa fever patients. It has been
shown to be most effective when given early in the course of the illness.
Patients should also receive supportive care consisting of maintenance
of appropriate fluid and electrolyte balance, oxygenation and blood pressure,
as well as treatment of any other complicating infections.
| What
groups are at risk for getting the illness? |
 |
Individuals at risk
are those who live or visit areas with a high population of Mastomys
rodents infected with Lassa virus or are exposed to infected humans. Hospital
staff are not at great risk for infection as long as protective measures
are taken.
| How
is Lassa fever prevented? |
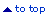 |
 |
 |
| |
Wearing
protective clothing -- an important part of practicing barrier nursing
methods. |
 |
|
Primary transmission
of the Lassa virus from its host to humans can be prevented by avoiding
contact with Mastomys rodents, especially in the geographic regions
where outbreaks occur. Putting food away in rodent-proof containers and
keeping the home clean help to discourage rodents from entering homes.
Using these rodents as a food source is not recommended. Trapping in and
around homes can help reduce rodent populations. However, the wide distribution
of Mastomys in Africa makes complete control of this rodent reservoir
impractical.
When caring for patients
with Lassa fever, further transmission of the disease through person-to-person
contact or nosocomial routes can be avoided by taking preventive precautions
against contact with patient secretions (together called VHF isolation
precautions or barrier nursing methods). Such precautions include wearing
protective clothing, such as masks, gloves, gowns, and goggles; using
infection control measures, such as complete equipment sterilization;
and isolating infected patients from contact with unprotected persons
until the disease has run its course.
| What
needs to be done to address the threat of Lassa fever? |
 |
Further educating
people in high-risk areas about ways to decrease rodent populations in
their homes will aid in the control and prevention of Lassa fever. Other
challenges include developing more rapid diagnostic tests and increasing
the availability of the only known drug treatment, ribavirin. Research
is presently under way to develop a vaccine for Lassa fever.
|
 |
 |
 |
| Related
Links |
|
|
 |
 |
|
| Glossary |
| Unsure
about some of the terms used on this page? Visit our glossary
of terms for help. |
 |
 |
|
|
 |
