Issue No. 5 - Winter/Spring 2007
Table of Contents
- Breast Cancer
- Mammograms and Breast Cancer
- The Best Way to Examine Your Breasts
- Herceptin
- Silicone Gel-Filled Breast Implants
- Cancer of the Uterus
- Medical Devices and Uterine Cancer
- Cervical Cancer
- Ovarian Cancer
- Additional Resources
Editors’ Note: We have chosen to devote this issue on female cancers to help educate our readers about the most common female cancers; breast cancer, uterine cancer, cervical cancer and ovarian cancer. This issue will also provide information about ways to prevent, diagnose and treat cancers.
According to the Centers for Disease Control and Prevention (CDC), breast cancer is one of the most common cancers in women in the United States. It is more common in older women than in younger women and is the most common cause of death from cancer among Hispanic women and the second most common cause of death from cancer among white, black, Asian/Pacific Islander, and American Indian/Alaska Native Women. In 2003, over 181,000 women developed breast cancer and over 41,000 women died, making it the sixth leading cause of death for women in the United States. And more than 72,000 women were diagnosed with a cancer affecting the reproductive organs and more than 27,000 women died.
Breast Cancer: The Basics
Growth of Tumors
Breast cancer occurs when normal breast cells divide without control or order. Normally, cells divide in a regulated manner. If cells keep dividing uncontrollably when new cells are not needed, a mass of tissue forms, called a growth or tumor.
There are two types of tumors, a benign tumor (not cancerous) and malignant tumor (cancerous). A benign tumor does not invade or spread. A malignant tumor can invade nearby tissues and spread to other parts of the body.
Although most people think of breast cancer as affecting only women, men can develop breast cancer as well, and breast cancer in men can spread faster than in women.
Risk Factors
The cause of breast cancer is unknown, but research shows that certain risk factors are associated with the disease. A risk factor is something that increases your chance of getting a disease or condition.
Risk Factors for Breast Cancer Include:
|
Symptoms
When breast cancer first develops, there may be no symptoms at all. But as the cancer grows, it can cause the following changes:
- A lump or thickening in or near the breast or in the underarm or neck area
- A change in the size or shape of the breast
- Nipple discharge, bleeding, tenderness, or the nipple pulled back (inverted) into the breast
- Ridges or pitting of the breast skin (like the skin of an orange)
- A change in the looks of the skin of the breast, the dark skin around nipple (areola), or of the nipple (for example, warm, swollen, red, or scaly).
Note: These symptoms may also be caused by other, less serious health conditions. Anyone experiencing these symptoms should see a doctor.
Diagnosis
The doctor will ask about your symptoms and medical history, and perform a physical exam.
Tests may include:
- Clinical Breast Exam: The doctor carefully checks for lumps, feels any lump and the tissue around it, checks the size and texture of the lump, and sees if the lump moves easily.
- Mammography: X-rays of the breast are used to check for lumps or other changes in breast tissue.
- Ultrasound: High-frequency sound waves are used to check whether a lump is a fluid-filled cyst (usually not cancer) or a solid mass (which may or may not be cancer).
- Biopsy: Tumor tissue is removed to test for cancer cells. Types of biopsies for breast cancer include:
- Fine-needle aspiration-removal of fluid and/or cells from a breast lump using a thin needle
- Needle biopsy-removal of tissue with a needle from an area that looks suspicious on a mammogram but cannot be felt
- Surgical biopsy:
- Incisional biopsy-cutting out a sample of a lump or suspicious area
- Excisional biopsy-cutting out all of a lump or suspicious area and an area of healthy tissue around the edges
- Hormone Status Evaluation: Breast cancer tissue is tested for the presence of estrogen and progesterone receptors. The results are used to help plan therapy.
 Treatment
Treatment
Types of treatments can include:
- mastectomy
- lumpectomy
- lymph node removal
- radiation therapy
- chemotherapy
- biologic therapy
Patients should discuss these treatments with their cancer doctor (oncologist).
Early Diagnosis
Because the cause of breast cancer is unknown, finding it early and treating it is the best way to prevent dying from the disease. And because it does not cause symptoms in the early stages, it is important to have screening tests to find the cancer before symptoms appear.
Here are some general guidelines:
- Women 20 and older should perform a breast self-exam every month. Some women find it easier to perform a self-exam at the same time each month, for example, when your menstrual period ends.
- Women between the ages of 20-39 should have a clinical breast exam by a health professional every three years. A breast exam should be performed more regularly if there is a family history of breast cancer or there have been previous breast biopsies.
- Women age 40 and older should have a mammogram every year. Healthcare professionals encourage women to have a mammogram sooner for those with a strong family history of breast cancer or who have had previous breast biopsies performed.
- After age 40, women should have a breast exam by a medical professional every year.
Source: Breast Cancer Information, U.S. Health and Human Services (Spanish Version) - Revised June 2005
Mammograms and Breast Cancer
 A Mammogram Is a Type of X-ray
A Mammogram Is a Type of X-ray
A mammogram is a special kind of x-ray exam of the breasts. Mammograms are used to help find breast cancer early, when it can still be cured. Mammograms are recommended for women older than 40, even if they have no signs of breast cancer.
Mammograms are also recommended for younger women who have symptoms of breast cancer or who have a high risk of breast cancer. But mammograms can miss cancer, so it’s important to follow the general guidelines above.
Mammograms Are Important
A mammogram can save your life. Mammograms can show tumors that may be cancer long before they can be felt. Treating tumors when they are still small makes curing cancer easier.
If you have a mammogram that does not look normal, you may need additional radiological exams to better evaluate the area. These can include additional mammograms or ultrasound exams. If the area still looks abnormal, your doctor will probably suggest a biopsy -- a tissue sample of the breast. A biopsy is minor surgery. The breast tissue from a biopsy is tested in a laboratory to see if it's cancerous.
Remember, just because a problem area shows up on your mammogram does not mean you have cancer. Cancer can be diagnosed only by a lab test on tissue from your breast.
|
Both digital and film mammography use x-ray radiation to produce an image of the breast. However, film mammography stores the image directly on film, whereas digital mammography takes an electronic image of the breast and stores it directly in a computer. This allows the recorded data to be enhanced, magnified, or adjusted for further evaluation. The difference between film mammography and digital mammography is like the difference between a traditional film camera and a new digital camera. Aside from the difference in how the image is recorded and stored, there is no other difference between the two. |
Getting a High-Quality Mammogram
The Mammography Quality Standards Act (MQSA) is a federal law that requires every mammography facility to meet quality standards. The FDA ensures that all the facilities in the United States meet MQSA standards. These standards apply to the following professionals who must have special training and education:
- the technologist who takes your mammogram
- the physician who reads your mammogram
- the medical physicist who tests the mammography equipment
MQSA also requires that the mammography equipment in the facility you go to is tested regularly and is maintained to operate properly. The FDA is the certifying agency of all states except for Iowa, Illinois, and South Carolina who are certifying agencies under the MQSA States As Certifiers Program.
Look for the Certified Mammography Facility certificate at your mammography facility. The certificate means that the facility has had regular inspections to meet quality standards.
 Sample of Certified Mammography Facility certificate. Certificates may vary in some states. |
FDA Has a List of Certified Clinics
To find the MQSA certified mammography facilities in your area, call (800) 4-CANCER (422-6237) or a local chapter of the American Cancer Society listed in your phone book. If you are hearing impaired, you can call (800) 332-8615 (TTY).
If you have access to the Internet, you can find a list of MQSA certified facilities at:
http://www.accessdata.fda.gov/scripts/cdrh/ cfdocs/cfMQSA/mqsa.cfm
The Best Way To Examine Your Breasts
1. Look at your breasts in a mirror to see if there is anything you have not noticed before such as:
|
 |
2. While still looking in the mirror, join your hands behind your head and press them gently against the back of your neck. Are there any changes from last month in how your breasts look? |
 |
3. While still looking in the mirror, press your hands on your hips. Bow slightly forward, pulling your shoulders and elbows forward. Look for changes since last month in how your breasts look. |
 |
| 4. When you are in the shower and your skin is soapy, do this exam. Raise your left arm. Using 3 or 4 fingers of your right hand, begin at the outer edge of your breast. Press your fingers firmly into your breast and slowly move your hand in circles until you reach the nipple. Make sure you examine the entire breast. In the same way, examine the area between the breast and armpit, and then the armpit itself. Do you feel any lump under the skin? Gently squeeze the nipple. Is there any discharge? Do the same thing with your right arm raised and your left hand examining your right breast. |
 |
| 5. Get out of the shower, dry off, and lie down on your back. Repeat the same exam as in #4. |  |
Source: FDA's Mammograms and Breast Cancer
Use of Herceptin For Early Stage Breast Cancer
Recently, FDA expanded the approved use of Herceptin, a biological cancer drug. The recent approval is for Herceptin to be used in combination with other cancer drugs for the treatment of HER2 positive breast cancer after a lumpectomy or a mastectomy.
 Herceptin is a targeted therapy against the HER2 protein on cancer cells. When an excessive amount of HER2 protein is present, it causes cancer cells to grow more rapidly and standard chemotherapy may be less effective. In 1998, FDA approved Herceptin for the treatment of metastatic breast cancer (cancer that has spread to other sites in the body). This recent approval expands its use to women with cancer in the breast and regional lymph nodes that have been removed with surgery. Herceptin should be prescribed only for women diagnosed with HER2 positive breast cancer.
Herceptin is a targeted therapy against the HER2 protein on cancer cells. When an excessive amount of HER2 protein is present, it causes cancer cells to grow more rapidly and standard chemotherapy may be less effective. In 1998, FDA approved Herceptin for the treatment of metastatic breast cancer (cancer that has spread to other sites in the body). This recent approval expands its use to women with cancer in the breast and regional lymph nodes that have been removed with surgery. Herceptin should be prescribed only for women diagnosed with HER2 positive breast cancer.
According to FDA's Center for Drug Evaluation and Research, this is especially good news for women who have breast cancer caused by excessive amounts of the HER2 protein because this cancer typically has a poor prognosis.
Source: FDA Press Release November 16, 2006
Silicone Gel-filled Breast Implants
Women who have had their breasts removed because of cancer may consider having breast implants.
In November 2006, after a strict scientific review, the FDA approved the marketing of silicone gel-filled breast implants made by two companies for:
- breast reconstruction in women of all ages
- breast augmentation (enlargement) in women ages 22 and older.
FDA is, however, requiring the two companies to conduct 10 years of patient follow-up to include:
- conducting a large post-approval study (follow-up with patients who have implants)
- continuing its CORE study through 10 years (an FDA clinical trial-see below)
- conducting a focus group study of the patient labeling (to identify problems with labeling in order to improve it)
- continuing laboratory studies to further identify types of device failure
- tracking each implant so that healthcare professionals and patients can be notified of updated product information if needed
The products are manufactured for Allergan Corp. (formerly Inamed Corp.), Irvine, California, and for Mentor Corp., Santa Barbara, California.
Sources: FDA Press Release; FDA Consumer magazine, January/February 2007: Silicone Gel-Filled Breast Implants Approved
Cancer of the Uterus
Cancer of the uterus is the most common gynecologic cancer in the U.S. There are several types of uterine cancers. Two types are endometrial cancer and uterine sarcoma. Endometrial cancer begins in the tissue that lines the uterus (endometrium). Uterine sarcoma occurs when cancer cells grow in the smooth muscle or connective tissue of the uterus. Uterine sarcomas account for only a small portion of cancers of the uterus.
High risk factors for uterine cancer may include obesity and never being pregnant. Certain types of hormone therapy may also increase the risk of uterine cancer. But there are women who get uterine cancer who do not have any of these high risk factors. Uterine cancer usually occurs after menopause or around the time that menopause begins.
Abnormal vaginal bleeding is the most common symptom of uterine cancer. Bleeding may start as a watery, blood-streaked flow that gradually contains more blood. Women should not assume that abnormal vaginal bleeding is part of menopause. If you have ANY abnormal vaginal bleeding, talk with your medical professional immediately.
To learn more about cancer of the uterus, contact the National Cancer Institute (NCI) at 800-4-CANCER (800-422-6237) or go to the following web site: http://www.cancer.gov/cancerinfo/wyntk/uterus. You can also find out more about cancer of the uterus by contacting the National Women's Health Information Center (800-994-9662).
Source: womenshealth.gov, Cancer of the Uterus
Medical Devices and Uterine Cancer
Medical devices are used to diagnose uterine and other cancers. These devices include instruments used in pelvic exams, radiology exams, and laboratory tests (such as blood and urine). The doctor may use medical devices to perform one or more of the following exams or tests.
- Pelvic exam -- A woman has a pelvic exam to check the vagina, cervix, uterus, ovaries, and fallopian tubes. The doctor feels these organs for any lumps or changes in their shape or size. To see the upper part of the vagina and the cervix, the doctor inserts an instrument called a speculum into the vagina.
- Pap test -- The doctor scrapes a sample of cells from the cervix and upper vagina. A medical laboratory checks the sample for abnormal cells. Although the Pap test (also called Pap smear) can detect cancer of the cervix, cells from inside the uterus usually do not show up on a Pap test. The test can also show non-cancerous conditions, such as an infection or inflammation.
- Transvaginal ultrasound -- The doctor inserts an instrument into the vagina that aims high-frequency sound waves at the uterus. The pattern of the echoes they produce creates a picture. If the endometrium looks too thick (hyperplasia), the doctor may perform a biopsy.
- Biopsy -- The doctor removes a small piece of tissue from the uterine lining. This usually can be done in the doctor's office. In some cases, however, a woman may need to have a dilation and curettage (D&C) (tissue is scraped from the inner lining of uterus and biopsied). A D&C is usually done as a same-day surgery with anesthesia in a hospital. A pathologist examines the tissue to check for cancer cells, hyperplasia, and other conditions. For a short time after the biopsy, some women may have cramps and vaginal bleeding
Source: Excerpt from NCI's Cancer of the Uterus
Cervical Cancer
Cervical cancer is a disease in which malignant cells form in the tissue of the cervix. The cervix is the lower, narrow end of the uterus. The cervix leads from the uterus to the vagina (birth canal).
Cervical cancer usually develops slowly over time. Before the cancer appears in the cervix, the cells of the cervix go through changes known as dysplasia, in which cells that are abnormal begin to appear. Later, these abnormal cells change to cancer cells, start to grow, and spread more deeply into the cervix and to surrounding areas.
Human papillomavirus (HPV) infection of the cervix is the most common cause of cervical cancer. HPV is transmitted through sexual intercourse. Although most women with HPV infection will not develop cervical cancer, some women with certain high risk strains of HPV will have an increased risk to develop cervical cancer. Women who do not regularly have a Pap test to detect HPV or abnormal cells in the cervix are at increased risk of cervical cancer.
The chance of recovery is better when the cancer is found early. There are usually no early signs of cervical cancer, but it can be detected with regular check-ups including a Pap test to check for abnormal cells and any infection in the cervix. Most women should have yearly check-ups. Others may only need to have a Pap test every few years (if there are no signs of cervical cancer or infection for 3 years in a row). It is best to follow your healthcare professional's advice.
As cervical cancer progresses, some possible signs of cancer may include vaginal bleeding and pelvic pain. Other conditions may cause the same symptoms. A doctor should be consulted if any of the following problems occur:
- Vaginal bleeding
- Unusual vaginal discharge
- Pelvic pain
- Pain during sexual intercourse
The following test and procedures may be used to find and diagnose cervical cancer:
- Pap test
- Colposcopy (viewing the vagina and cervix with a special instrument).
- Biopsy
- Pelvic exam
|
A Pap smear is a test for abnormal cells in the cervix. The Pap smear can be done by a doctor, physician's assistant, nurse, nurse practitioner, or midwife. More information is available from: |
After cervical cancer has been diagnosed, tests are done to find out if cancer cells have spread within the cervix or to other parts of the body. The process used to find out if cancer has spread is called staging. Staging for cervical cancer is different from staging for other cancers. It is staged based on a doctor's physical exam and possibly by an exam of the inside of the bladder or rectum. The information gathered from the staging process determines how far into the body the disease has spread. It is important to know the stage in order to plan treatment. The following tests, medical devices, and procedures may be used to discover the extent of the disease and to plan treatment but are not technically part of the staging process:
- Chest X-ray: An X-ray of the organs and bones inside the chest using a type of energy beam that can go through the body and onto film, making a picture of areas inside the body.
- CT scan: A procedure that makes a series of detailed pictures of areas inside the body, taken from different angles. The pictures are made by a computer linked to an x-ray machine. A dye may be injected into a vein or swallowed to help the organs or tissues show up more clearly; also called computed tomography or CAT scan.
- Lymphangiogram: An X-ray of the lymph system which carries body fluid containing white cells (lymphatic). A dye is injected into a lymphatic vessel and travels throughout the lymphatic system. The dye outlines the lymphatic vessels and organs on the X-ray and helps find out whether cancer has spread to the lymph nodes.
- Ultrasound exam: A procedure in which high-energy sound waves are bounced off internal tissues or organs and make echoes. The echoes of sound waves form a picture of body tissues called a sonogram.
- MRI (magnetic resonance imaging): A procedure that uses a magnet, radio waves, and a computer to make a series of detailed pictures of areas inside the body; also called nuclear magnetic resonance imaging (NMRI).
|
FDA recently announced the approval of a new vaccine that will help prevent cervical cancer. Gardasil is the first vaccine developed to prevent cervical cancer, precancerous genital lesions and genital warts due to human papillomavirus (HPV) in females 9-26 years of age. For more on information about Gardasil and HPV visit: |
There are different types of treatment available for patients with cervical cancer. Surgical removal of the cancer is sometimes used to treat early cervical cancer. Talk with your oncologist about the best treatment for you. In more advanced cases, radiation, chemotherapy or both may be used to treat cervical cancer. Some treatments are standard (the currently used treatment), and some are being tested in clinical trials. A treatment clinical trial is a research study meant to help improve current treatments or obtain information on new treatments for patients. Anyone who volunteers to be in a clinical trial will receive information about what to expect from the controlled study. Clinical trials are taking place in many parts of the country. More information about ongoing clinical trials is available from: http://www.cancer.gov/clinicaltrials
Sources: NCI Cervical Cancer; FDA Consumer Magazine, January/February 2004
September and October are Female Cancer Awareness Months
|
Ovarian Cancer
Basic Information
According to the Centers for Disease Control and Prevention, (CDC) ovarian cancer is the seventh most common cancer and the fifth leading cause of cancer death for women in the United States. And from CDC's U.S. Cancer Statistics Working Group, United States Cancer Statistics: 2003 Incidence and Mortality (preliminary data), almost 20,000 women were diagnosed with ovarian cancer in 2003 and almost 15,000 women died from the disease.
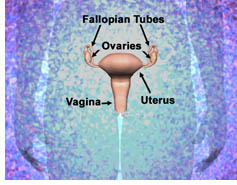 The Ovaries
The Ovaries
The ovaries are part of a woman's reproductive system. The two ovaries
- are in the pelvis
- are about the size of an almond
- make the female hormones - estrogen and progesterone
- release eggs that travel from an ovary through a fallopian tube to the uterus
When a woman goes through her "change of life" (menopause), her ovaries stop releasing eggs and make far lower levels of hormones.
Abnormal Cells in the Ovaries
Certain types of abnormal cells in the ovaries can form a malignant tumor or a benign tumor. If it is malignant, the cancer can invade, shed, or spread to other organs. When cancer spreads (metastasizes) from its original place to another part of the body, the new tumor has the same kind of abnormal cells and the same name as the original tumor. For example, if ovarian cancer spreads to the liver, the cancer cells in the liver are actually ovarian cancer cells. The disease is metastatic or "distant" ovarian cancer, not liver cancer. For that reason, it is treated as ovarian cancer, not liver cancer.
Risk Factors
Doctors cannot always explain why one woman develops ovarian cancer and another does not. However, we do know that women with certain risk factors may be more likely than others to develop ovarian cancer. Studies have found the following risk factors for ovarian cancer:
- Family history of ovarian cancer
- Personal history of cancer
- Age over 55
- Never pregnant
- Menopausal hormone therapy (studies have suggested a link)
Symptoms
Unfortunately, ovarian cancer is rarely diagnosed early, when it is curable. The reason for this is that early ovarian cancer may not cause obvious symptoms. But, as the cancer grows, symptoms may include:
- Pressure or pain in the abdomen, pelvis, back, or legs
- A swollen or bloated abdomen
- Nausea, indigestion, gas, constipation, or diarrhea
- Feeling very tired all the time
Less common symptoms include:
- Shortness of breath
- Feeling the need to urinate often
- Unusual vaginal bleeding (heavy periods, or bleeding after menopause)
Most often these symptoms are not due to cancer, but only a doctor can tell for sure. Any woman with these symptoms should tell her doctor.
Diagnosis
There is no good way to diagnose ovarian cancer. If you have a symptom that suggests ovarian cancer, your doctor must find out whether it is due to cancer or to some other cause. Your doctor may ask about your personal and family medical history.
You may have one or more of the following tests. Your doctor can explain more about each test.
- Physical exam
- Blood tests
- Pelvic exam
- Ultrasound
- Biopsy
- Laparoscopy
- Pathology of cells
Your doctor may order tests to find out whether the cancer has spread (staging):
- CT Scan to show abdominal fluid or tumor
- Chest X-ray to show abdominal fluid or tumor
- Barium Enema to X-ray the intestines to show areas blocked by cancer
- Colonoscopy to see if cancer has spread to rectum or colon
Sources: Excerpt from NCI brochure; Ovarian Cancer Screening.
Additional Resources
Food and Drug Administration:
National Library of Medicine:
- Breast Cancer Interactive Tutorial (also in Spanish)
- Ovarian Cancer Interactive Tutorial (also in Spanish)
Other Sources:
- CDC (open link of interest under 'Health Topics')
- National Cancer Institute - Women's Cancers
Crossword
For the Maturity Health Matters
Crossword Puzzle, see page 13 of the
Printer-Friendly PDF Version.
Maturity Health MattersMaturity Health Matters is an FDA publication for older adults, their families and caregivers. We provide our readers with current information on FDA-regulated medical products. This publication can be reproduced. If you have comments about our publication, please send them to the editors. Editors: Harriet Albersheim and Mary Ann Wollerton
Department of Health and Human Services - Food
and Drug Administration Special thanks to: CDER, CBER, and FDA Consumer for contributing to this issue. If you wish to receive email notification of new issues, go here to subscribe. Links to non-Federal organizations are provided solely as a service to our readers. Links do not constitute an endorsement of any organization by FDA or the Federal Government, and none should be inferred. FDA is not responsible for the content of the individual organizations' web pages found at these links. |
Don’t Miss Future Issues
If you have found this newsletter by "surfing the net," add Maturity Health Matters to your favorites. At the site you can subscribe to the newsletter and receive email notification when new issues are published.
While you are online, check our consumer website where you will find many topics of interest especially for consumers.





