Agency for Toxic Substances and Disease Registry
|
|||||||||||||||||||||||||||||||||||||||||||||
Learning Objectives |
At the completion of this section, the reader will be able to describe:
|
Sympathetic vs. Parasympathetic Effects |
Nicotinic and muscarinic receptor stimulation results in a mixture of their sympathetic and parasympathetic effects. (Erdman 2004) Cholinergic stimulation of the nicotinic receptors in the sympathetic autonomic ganglia may cause adrenal medullary catecholamine release leading to increased heart rate, and blood pressure, and (in about 13% of the time) mydriasis (pupillary dilation). (Erdman 2004) More often, however, autonomic findings of parasympathetic stimulation predominate over sympathetic findings. (Erdman 2004) NOTE: For reasons which are presently unclear, nicotinic signs predominate in pediatric cholinesterase inhibitor poisoning. (More on this later.) The differences in nicotinic and muscarinic structure and function explain why cholinesterase inhibitor toxicity results in muscarinic stimulation of the cardiac conduction system, smooth muscle, and exocrine glands but nicotinic stimulation, then subsequent weakness and paralysis of skeletal muscles. |
Central Nervous System (CNS) Effects |
The pathophysiology of cholinesterase inhibitors on the CNS is complex and poorly understood. Both Nicotinic and muscarinic receptors are involved. (Erdman 2004) CNS findings that have been reported include |
| Anxiety (Carlton, Simpson et al. 1998) | Arreflexia (Carlton, Simpson et al. 1998) | Circulatory depression (Carlton, Simpson et al. 1998) |
| Coma (Clark 2002) | Confusion (Ecobichon 1996; Clark 2002) | Convulsions |
| Depression (Reigart and Roberts 1999) | Drowsiness (Ecobichon 1996) | Emotional lability (Sidell 1997; Romano, McDonough et al. 2001) |
| Excess dreaming (Romano, McDonough et al. 2001) | Fatigability (Sidell 1997) | Hallucinations (Clark 2002) |
| Headache (Ecobichon 1996) | Insomnia (Sidell 1997; Carlton, Simpson et al. 1998) | Lethargy (Ecobichon 1996) |
| Memory loss (Reigart and Roberts 1999) | Nightmares (Sidell 1997) | Restlessness (Carlton, Simpson et al. 1998) |
| Respiratory depression (Carlton, Simpson et al. 1998) | Tension (Sidell 1997) | Tremulousness, jitteriness (Sidell 1997) |
| Note: Psychological and behavioral effects have been noted to precede physical symptoms. (Romano, McDonough et al. 2001) [Although rapid onset of severe poisoning may obscure this.] | ||
Cause of Death |
Death is usually due to respiratory failure from: (Zwiener and Ginsburg 1988; Sofer, Tal et al. 1989; Reigart and Roberts 1999)
|
Frequency of Signs and Symptoms |
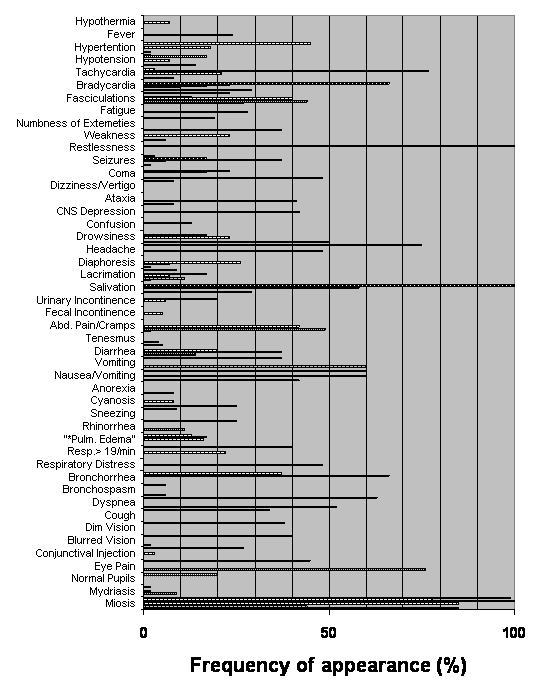
The likelihood of signs and symptoms of cholinesterase toxicity in a given individual depends on the specific chemical, the dose, and the route of exposure. (See more about this in the Optional Reading in the following section.) These may range from a mild, flu-like syndrome to rapid collapse, paralysis, respiratory arrest, and death. (Carlton, Simpson et al. 1998) Figure 8 in the following Optional Reading shows the frequency of signs and symptoms from eight case series of cholinesterase inhibitor poisoning. (Tsachalinas, Logaras et al. 1971; Hayes, van der Westhuizen et al. 1978; Hirshberg and Lerman 1984; Midtling, Barnett et al. 1985; Goswamy, Chaudhuri et al. 1994; Nouira, Abroug et al. 1994; Singh, Batra et al. 1995; Okumura, Takasu et al. 1996) |
Frequency of Signs and Symptoms in Cholinesterase Inhibitor Toxicity (Optional Reading) |
Figure 8. Frequency of Signs and Symptoms in Cholinesterase Inhibitor Toxicity |
Misconception | As noted in the mnemonics, SLUDGE AND DUMBELS, diarrhea, urinary incontinence, and excessive lacrimation are common signs of cholinesterase inhibitor poisoning. |
Reality | Although nausea and vomiting are common with moderate exposures, diarrhea (listed as “defecation” in the above mnemonics), and urination are infrequent. (Leikin, Thomas et al. 2002) As noted in the table above, Lacrimation is also not a common finding. |
Key Points |
|
Progress Check |