2.
STATE SUPPORT FOR NURSING EDUCATION
Every
State studied here gives financial and
other types of support for expanding nursing
education programs. Certain States are
doing better than others at expanding
their pipeline of nurses. This chapter
examines how States and other stakeholders
fund and support nursing education—directly
and indirectly—and what effect those strategies
are having on the State’s nursing supply.
INTRODUCTION
Schools
of nursing receive funding from various
sources, including State appropriations;
other Federal, State and local funds;
student tuition; and direct financial
assistance from private and foundation
sources. In addition to State appropriations
to higher education, States also channel
additional Federal or State funds to nursing
education, and some earmark certain funds—such
as lottery or gaming funds—for a specific
purpose, such as increasing enrollment
or supporting faculty salaries.
States
are not alone in supporting nursing education.
Schools of nursing rely heavily upon contributions
from the private sector—including hospitals,
health systems and foundations—to expand
their capacity. These groups invest financial
and human resources in nursing education
in each of the five States. For example,
a group of Texas hospitals in the Gulf
Coast region are working together to “loan”
their staff to teach in area schools of
nursing. This arrangement provided approximately
18 full-time instructors for an overall
contribution of almost $2 million annually.
[1]
Coupled
with targeted State investments in nursing
education, some States are seeing improvements
in their nursing supply. This chapter
describes State and other support for
expanding the pipeline in each of the
five States. The first section gives
an overview of State financing for higher
education: how higher education is funded
and how decisions are made about allocating
funds. The next section examines other,
more direct, funding for nursing education,
including State support and public and
private support for expanding the nursing
pipeline. The final section examines
nursing education trends in each of the
five States and, whenever data exists,
ties State and other investments to outcomes,
such as increased enrollment and graduations.
State
Funding of Higher Education
States
fund higher education through appropriations
of State taxes, non-tax appropriations
and other methods. Although State funding
of higher education does not indicate
how much funding actually reaches schools
of nursing, it does describe the funding
pool from which nursing education—among
other disciplines—receives a large portion
of its funds. In Texas, for example,
formula funding accounts for approximately
95 percent of all State funding of professional
nurse education in 2004-2005. [2]
Therefore, the State’s overall funding
of higher education is a rough measure
of its funding for nursing education.
State
budgets are showing signs of improvement;
however, the American Association of State
Colleges and Universities reports that
colleges and universities “ … top the
list of State spending cuts, with total
State appropriations for higher education
down for a second year in FY 04.” Enrollment
levels are up in many States, leading
colleges and universities to increase
tuition and fees and implement program
cutbacks. [3]
Higher
education institutions rely heavily on
State funding sources. State and local
governments provided nearly $68 billion
to public and independent higher education
in 2003, accounting for 71 percent of
all tuition revenue. The remaining $28
billion from net tuition revenue (that
is, money from student tuition and fees)
brought to $95.5 billion the amount available
from State, local and student sources.
The proportion of funding from State and
local appropriations and student sources
(i.e., fees and tuition) are illustrated
in figure 26.
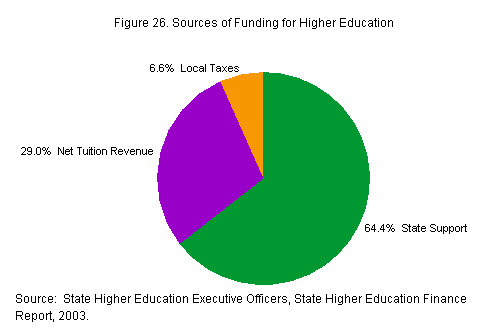 [D] [D]
Among
the five States studied here, the proportion
of State support varies from a low of
57 percent in Indiana to a high of 86
percent in Georgia. As shown in Table
4, Indiana receives a higher percentage
of total revenues from tuition than do
other States, while California receives
the smallest percentage.
Table
4. State, Local, and Net Tuition Revenue,
by State, FY 2003
|
State |
Total
State, local and net tuition revenue |
Total
State sources (%) |
Local
tax appropriations (%) |
Net
tuition revenue (%) |
|
California |
$13,225,064 |
73.1% |
15.0% |
11.9% |
|
Georgia |
$2,396,850 |
86.1% |
-- |
13.9% |
|
Indiana |
$2,313,569 |
57.3% |
-- |
42.7% |
|
Texas |
$7,687,356 |
64.8% |
7.9% |
27.3% |
|
Utah |
$863,532 |
71.1% |
-- |
28.9% |
Source:
State Higher Education Executive Officers,
State Higher Education Finance Report,
2003.
Appropriating
State Funds to Higher Education
Beginning
in the 1950s, State legislatures began
providing support to nursing programs
offered at higher education institutions.
A variety of mechanisms are used to appropriate
funds. In many States, funds are allocated
to an institution as a block grant to
support several disciplines, including
nursing. The amount of these block grants
is based on a number of factors, such
as the historical and actual costs for
existing faculty and academic programs,
plus a percentage for support services
and administration. Once a college or
university receives the grant funds, local
institutional policies and procedures
determine the allocation of the block
grant among the schools, colleges and
departments.
Recognizing
the needs and costs associated with various
types of programs and institutions, many
States developed a formula funding mechanism
that attempts to objectively and fairly
distribute State funds to educational
institutions that teach similar disciplines
but have different missions. [4]
The factors in a State’s formula might
include head count, number of positions,
full-time students, and staff and credit
hours.
On
the one hand, formula funding is an equitable
process for distributing State funds and
minimizing the political battles over
limited State resources. On the other
hand, however, some argue that formula
funds do not allow States to direct funding
to programs and initiatives that reflect
the State’s needs and priorities. In
response, many States determine a “base”
level (based on quantitative factors,
such as number of students or credit hours)
and then use different non-formula means
to provide additional funds. The five
States’ processes for funding higher education
are described below.
California
The
three separate public systems in California
include the University of California,
California State University and the community
college system. The State provides about
75 percent of the necessary funding to
support these three systems. According
to the Legislative Analyst’s Office, funding
for the University of California and California
State University is developed by using
the previous year’s base funding and adjusting
it to reflect inflation. A formula is
then used to determine the cost of funding
enrollment growth, and this cost is added
to the base appropriation.
In
addition to State appropriations, the
systems receive student fees that supplement
the State’s contribution and account for
about 40 percent of total funding for
education. The regents of the university
system set fees for the University of
California and the California State system,
while the Legislature sets fees for the
community colleges. [5]
California
differentiates funding by credit status
and institution. Therefore, students
enrolled in noncredit courses—such as
basic skills and English as a Second Language—receive
a lower per-student funding rate than
those enrolled in credit courses. Moreover,
the State provides a different per-student
funding rate for each system, with the
highest funding rate for students at the
University of California, a lower rate
for students enrolled in the California
State University system, and the lowest
for California community college students.
California
does not have different funding rates
for different educational levels and programs;
therefore, a student enrolled in a school
of nursing is funded at the same level
as a student enrolled in English, and
a graduate student is funded at the same
rate as an undergraduate student. [6]
Although this process may result in
under-funding of certain higher-cost programs,
it also over-funds other lower-cost programs.
As a result, funds from lower-cost programs
subsidize higher cost programs.[7]
Georgia
In
Georgia, State appropriations for higher
education include appropriations to the
University System of Georgia, the Georgia
Student Finance Commission (which provides
State scholarship programs) and the Department
of Technical and Adult Education. The
majority of the budget is calculated according
to a quantitative formula that includes
enrollment, faculty salaries and square
footage. The remaining non-formula portion
funds special initiatives at institutions.
[8]
Following
budget cuts in higher education—totaling
$68.7 million in 2004 [9]
—the Governor’s 2006 budget proposal would
invest more than half the State’s budget
in education. Among the Governor’s recommendations:
fully funding the university system’s
enrollment growth and maintenance and
operation of the system’s facilities.
[10]
The
State Board of Regents also provides financial
rewards to innovative and efficient programs.
These “Best Practices” awards reward programs
of excellence in finance and business,
academic affairs, student services and
information technology. Among the recipients
in 2004 was the Georgia Perimeter College’s
Hybrid Fellowship Program, which combines
face-to-face classes with on-line instruction,
reducing classroom space requirements
by 50 percent. [11]
Indiana
Indiana
uses a mix of block grant and formula
funding for its institutions of higher
education. The budget is based on previous
appropriations and these funds are added
to (or subtracted from, in cases of enrollment
decreases), based on several formula and
non-formula components, such as growth
in enrollment, research expenditures,
new facilities operations and other items.
In addition, the legislature sometimes
provides additional appropriations for
new or expanded programs; in 2005, when
it added $1.5 million to Ivy Tech State
College’s base appropriation to expand
its associate degree nursing program Statewide.
[12]
Texas
The
Texas Higher Education Coordinating Board
administers traditional formula funding
for 62 nursing education programs. The
main mechanism for funding public higher
education is driven by a formula based
on several factors, such as instructional
cost and institutional support. In addition
to the formula-driven funding base, State
appropriations also provide non-formula-based
supplemental funding for special items.
[13] Formula
funding for community colleges, academic
universities and health-related institutions
increased from $197 million in 2002-2003
to $207 million in 2004-2005.
Utah
In
Utah, institutions of higher education
distribute funds to nursing programs based
on a State funding base that also accounts
for credit hours. If a program grows
over the base level, the program will
receive additional funding for the growth.
However, the State has not been fully
funding growth to higher education institutions;
thus, the nursing programs are not receiving
full funding for the growth.
Other
State Processes
In
response to concerns that State appropriations
be directed toward specific priorities
and outcomes—such as meeting the State’s
economic and workforce needs—some States
have considered funding based on institutional
performance. In 2002, the New Mexico
Commission on Higher Education named a
Blue Ribbon Task Force to evaluate the
current funding method and recommend changes
to reward successful institutions that
are meeting the State’s economic needs.
The task force developed a base-plus-incentives
funding model—comprised of several base
or formula factors—that includes current
appropriations, compensation and inflation.
In addition to the base funding, the formula
would provide incentives to address the
nursing and teacher shortage and would
allocate funds to institutions through
a competitive proposal process. Virginia
developed a similar funding formula that
offers incentive funding for performance
on outcome measures such as graduation
and retention rates, exam passing rates,
post-graduate placement and faculty productivity.
In
California, the Legislature recently directed
the Chancellor of California State University
to provide supplemental funds to universities
to establish an entry-level master’s program
in nursing. The Governor signed into
law the Entry Level Master’s Nursing Programs
Act in 2004.
A
Closer Look at State Funding for Nursing
Education
The
methods by which States fund higher education
and specific disciplines such as nursing
vary considerably. In some cases, for
example, schools of nursing receive more
funds than other programs because they
are costly to operate; in other cases,
nursing is funded at the same level as
other disciplines.
Targeted
Funding and Support for Nursing Education
Although
State appropriations to higher education
account for the majority of nursing education
funds, many States are finding ways to
channel additional State funds directly
to nursing education to help programs
increase their capacity and to help recruit
and retain students and faculty.
Assessing
the effects of State programs and resources
on the nursing supply is difficult for
two major reasons. First, many examples
of targeted State support for nursing
education have occurred recently; therefore,
not enough time has elapsed to evaluate
the effect of State funding on supply.
Second, as described earlier in this section,
States are implementing strategies in
conjunction with other public and private
stakeholders, including hospitals and
other employers, schools of nursing and
higher education, and the Federal government.
Although these partnerships are proving
successful, detecting the effect of State
funds or other support is difficult. Some
concrete examples exist where a State’s
investment is producing positive outcomes.
Georgia’s Health Professions Initiative,
for example—a public-private partnership—is
expected to produce more than 1,300 new
nurses.
This
section examines pertinent trends in the
nursing supply in each State—specifically
in admissions, enrollment and graduations—and,
whenever possible, identifies successful
approaches. The section also includes
summaries of the major challenges and
opportunities present in each State.
Expanding
Program Capacity
Demand
for nurses is high; so, too, is the demand
for nursing education “slots.” At the
center is a bottleneck that turns away
qualified students on the one end and
that fails to produce the number of nurses
needed by tomorrow’s health care system
on the other. To address this bottleneck,
States are attempting to expand nursing
school capacity to allow for expanded
enrollments. Standing in the way of program
expansion, however, is a lack of faculty
to teach the increased numbers of courses
and students. Lacking more qualified
faculty, programs continue to limit enrollment
(since the faculty-to-student ratio largely
determines program capacity). As a result,
some States are taking legislative and
other steps to increase the pool of current
and future faculty members.
States
also are targeting funds to increase financial
assistance for potential nursing students,
and therefore, remove a formidable obstacle
for many. By offering certain incentives—such
as loan repayment and scholarships—States
are attracting a larger and more diverse
pool of students. In addition, these
programs can help to ensure that recipients
practice in shortage areas or work for
a certain number of years in order to
receive all the financial benefits.
Faced
with serious budget constraints, many
States are finding ways to direct existing
Federal funds into nursing education efforts.
For example, most State Medicaid programs
voluntarily pay for graduate medical education
(GME) as part of their service payments
to teaching hospitals (similar in methodology
to how Medicare pays for physician training).
Medicaid programs in as many as 12 States—Iowa,
Indiana, Louisiana, Maine, Minnesota,
Mississippi, Missouri, New Hampshire,
New Jersey, North Dakota, Oregon and South
Carolina [14]
—also allow or require that such payments
be directed to support clinical training
of graduate nurses in programs affiliated
with or operated by teaching hospitals.
This precedent provides the opportunity
in many States for Medicaid to pay for
graduate nursing education, particularly
if a State uses the intergovernmental
transfer of State funds to capture additional
Federal Medicaid matching funds for this
purpose.
The
following are examples of strategies States
are using to invest directly—with Federal
and State funds— in nursing education.
California.
The California Health Professions Education
Foundation is a nonprofit organization
that administers scholarships and loan
repayment grants to underrepresented and
economically disadvantaged students.
The foundation awards scholarships and
loan repayment grants through two funds:
the Health Professions Education Fund,
which is largely funded through private
and foundation sources, and the Registered
Nurse Education Fund, supported through
a $10 surcharge on RN license renewals.
The RN Education Fund pays for the following
three scholarship and loan repayment programs:
-
The Associate Degree Nursing Scholarship
Program, established through a 2003
law, provides recipients up to $8,000
per year to help associate degree students
located in shortage areas obtain a B.S.N.
degree within five years of obtaining
an associate degree.
-
The Registered Nurse Education Scholarship
Program offers up to $10,000 to students
in baccalaureate degree nursing programs
who agree to practice in underserved
areas.
-
The Registered Nurse Education Loan
Repayment Program provides up to $10,000
over a two-year period to repay loans
in exchange for practice in an underserved
area.
California
also directs significant Federal funding
to nurse and health care worker training.
All States receive Federal Workforce Investment
Act (WIA) funds and allocate the money
to support worker training programs for
entry-level occupations. Many of the
program’s recipients are displaced workers
or are enrolled in welfare programs.
States are actively working to help these
individuals secure employment through
training or retraining. Among the job
classifications targeted for the training
programs are nurse aides and practical
nurses (As many as 12 States also have
used WIA funds to provide job training
for RNs.).
In
2002, the Governor announced a $60 million
Nurse Workforce Initiative that used Federal
WIA funds to address the State’s growing
nurse shortage. The State distributed
$27 million in grants to 21 regional partnerships
with the goal of producing 5,000 new vocational
and registered nurses. In addition, the
initiative provided $6 million to address
local needs for psychiatric technicians
in the Central Valley.
The
WIA funds continue to be an important
and stable source of funding for nursing
education efforts in California. The
California 2005-2006 budget proposes to
use $35.8 million of WIA funds to train
nurses and other health care workers.
Specifically, the Governor proposes using
the funds to expand the capacity of community
college nursing programs and to expand
the supply of nursing faculty. [15]
Georgia.
In Georgia, the State Department of Labor
and the Woodruff Foundation combined funds
to provide service cancelable loans to
prospective nurse faculty. The Georgia
Nursing Faculty Scholarship Program, managed
by the Georgia Student Finance Authority,
is “ … designed to encourage Georgians
to enter—and remain in—the nursing education
profession.” [16]
Funded with $1.1 million from the Department
of Labor, $500,000 from the Woodruff Foundation
and an in-kind contribution from the Georgia
Student Finance Authority, the program
provides funding for students to enroll
in graduate level programs at public or
private universities in Georgia. After
graduating, recipients can repay the loan
by serving as a faculty member in Georgia;
for every year of teaching, they are eligible
to cancel $2,500 in loans. Over a five-year
period, this public-private partnership
will produce an additional 25 faculty.
Another positive outcome is that, since
programs are spread throughout the State,
the program should provide faculty members
ready for hire across Georgia, particularly
in shortage areas.
In
an effort to expand faculty and student
enrollment in Georgia, lawmakers directed
State funds into nursing education through
the State’s Intellectual Capital Partnership
Program (ICAPP). Beginning in 2002, the
program leveraged $2.1 million in State
funding with $2.4 in private funding,
resulting in a $4.55 million public-private
partnership between Georgia health care
employers and State universities. The
program matches employers with public
colleges and universities to produce graduates
in nursing and other fields. State funds
are used for instruction and expenses,
while schools of nursing provide the education
and clinical experiences. Health care
providers make in-kind contributions of
equipment, staff time, laboratory and
classroom space—valued at $2.45 million—and
agree to hire graduates when they complete
the program.
State
and private sector investments, joined
through the ICAPP Health Professions Initiative,
are producing more nursing graduates in
Georgia. The Intellectual Capital Partnership
Program is expected to produce more than
1,300 new graduates by 2006. As shown
in Table 5, schools of nursing will produce
up to 635 nurses and other specialists
as a result of the State’s first-year,
$2.1 million commitment. With the 2004
announcement of the State’s $2.05 million
investment in the program’s second phase,
another 700 nurses are expected to be
ready for hire in 2006. [17]
Employers will hire these program graduates
in 19 communities throughout the State
at program completion.
Table
5. Georgia Nursing Graduate Outcomes:
Phase One and Phase Two
|
Schools |
Program
Type |
Phase
1 (2002) |
Phase
2 (2004) |
|
Total
Graduates Produced* |
Expected
Graduates at Program End |
|
Abraham
Baldwin Agricultural College |
Associate
|
46 |
23 |
|
Armstrong
Atlantic State University |
BSN |
38 |
266 |
|
Augusta
State University (added in 2003) |
|
80 |
|
|
Clayton
College and State University |
BSN |
40 |
60 |
|
Columbus
State University |
BSN |
95 |
114 |
|
Darton
College |
Associate
|
108 |
|
|
Floyd
College |
Associate
|
32 |
55** |
|
Georgia
Perimeter College |
Associate
|
24 |
20 |
|
Georgia
State University |
BSN |
24 |
48 |
|
Gordon
College (added in 2003) |
LPN |
30 |
|
|
Kennesaw
State University |
BSN |
71 |
25 |
|
Middle
Georgia College |
Associate
|
47 |
60 |
|
Total |
|
635 |
671 |
*Includes
graduates who have already completed program
and those expected to complete by program’s
end.
**In
phase two, Floyd College will create 30
associate degree graduates and another
25 in partnership with Kenn esaw State
University.
Source:
Board of Regents of the University System
of Georgia, August 2004.
Georgia
invests significant funds in raising academic
performance in all educational phases
and targets resources to boost achievement
among racial and ethnic minorities. The
University System’s P-16 Initiatives received
a $34.6 million grant from the National
Science Foundation to fund the Partnership
for Reform in Science and Mathematics
(PRISM) Program. Its goal is to improve
educational achievement levels and close
the performance gaps in science and math
among Georgia’s students
Georgia
also earmarks a portion of State lottery
funds for higher education, including
nursing education, through its Helping
Outstanding Pupils Educationally (HOPE)
scholarship program and its service cancelable
loan program. The HOPE scholarship program
is funded completely through lottery funds.
Eligible residents may receive financial
aid plus a $300 book allowance (up to
$3,000 annually for those enrolled in
an eligible private college or university
in the State).
Although
it is difficult to attribute State actions
to specific outcomes, it does appear that
the combined efforts of the public and
private sectors are making a difference
in Georgia. As a result of increased
admissions standards and the HOPE scholarship,
students who enter the University System
of Georgia are more qualified and more
diverse than in years past. Specifically,
more students who enter the system have
completed the college preparatory curriculum
course requirements, thus reducing the
demand for learning support and remedial
courses. [18]
Nearly 4,000 more students were enrolled
in nursing programs in 2002—an increase
of nearly 50 percent from 2000. This
upward trend reverses an eight-year trend
of declining enrollments.
As
shown in Figure 27, 11,698 students were
enrolled in 2002, driven by significant
increases in both associate and bachelor
degree programs. During that two-year
period, nearly 1,300 more students enrolled
in bachelor degree programs, and more
than 2,600 students were enrolled in associate
degree programs—gains of 33 percent and
65 percent, respectively. For the first
time, baccalaureate level enrollment exceeds
5,000. [19]
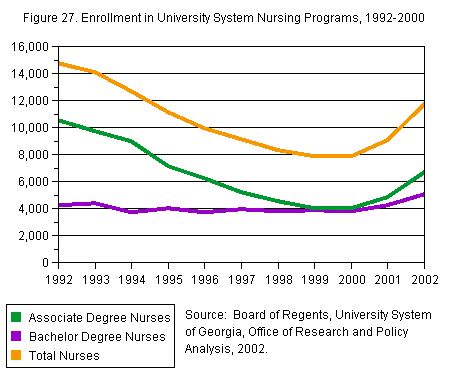 [D] [D]
Although
these trends are promising, they illustrate
the uphill battle many States face as
they attempt to change courses and restore
enrollments to previous levels. Although
2002 enrollment is higher than any year
since 1995, it still falls short of 1993
enrollment, which peaked at more than
14,000.
Still,
the trend is now moving in the right direction
and, as a result of increasing enrollments,
the number of graduates and licensed nurses
is expected to see similar increases as
these students move through the system.
Although
enrollment levels have risen in recent
years, the number of graduates has not.
During the past decade, the number of
nursing graduates from university system
programs has dropped by more than 42 percent,
while the number of LPN graduates from
the State’s technical school system has
dropped by 21 percent (see Figure 28).
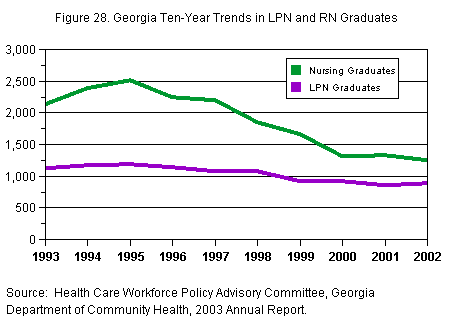 [D] [D]
This
trend is expected to reverse as the higher
number of students enrolled in programs
(Figure 27) moves toward graduation.
As long as programs retain their students,
the graduation trends should begin to
more closely reflect the increasing numbers
of students enrolled in programs.
Obtaining
a license is the final step in becoming
a nurse; therefore, licensure data gives
an estimate of the number of new nurses
available for work. According to Georgia’s
Health Care Workforce Policy Advisory
Committee’s 2002 report, “ … increasing
the rate of licensure through exam is
critical to Georgia’s ability to meet
the long-term health care needs of her
citizens.” [20]
As
shown in Figure 29, the overall licensure
trend is positive—in 2001, the State issued
about 500 more licenses than in the previous
year. However, a closer look shows that
the number of licenses issued through
examination continued a steady five-year
decline. In 2001, 1,775 new graduates
passed the examination (a prerequisite
to obtaining a license), down by more
than 1,000 from 1996.
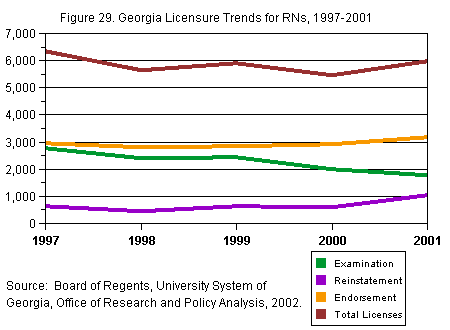 [D] [D]
Indiana.
In 1990, the Indiana General Assembly
created the Nursing Scholarship Fund,
funded through the general fund, which
encourages more people to pursue a nursing
career in Indiana. The State Student
Assistance Commission administers the
program and allots the funds to approved
colleges and universities. To qualify,
students must be Indiana residents and
agree to work as a nurse in Indiana for
at least the first two years following
graduation. In return, students are eligible
to receive up to $5,000 annually for tuition
and fees.
In
2001, the General Assembly adopted many
of the recommendations made by the Health
Care Professional Development Commission,
including one that created the Indiana
Health Care Professional Recruitment and
Retention Fund. The fund provides loan
repayment for professionals, such as primary
care nurse practitioners and certified
nurse midwives, who agree to practice
in shortage areas. In addition, the legislation
allowed the State Department of Health
to apply for grants from Federal or private
sources to supplement the State’s contribution.
As a result, the State received matching
Federal grant funds from HRSA.
Texas.
In response to growing concern about
a worsening nursing shortage and lagging
enrollments, Texas lawmakers found ways
to channel additional State funds—above
and beyond the State’s formula funding—into
schools of nursing that demonstrated high
enrollment increases. In 2001, the Legislature
passed the Nursing Shortage Reduction
Act, which provided new general revenue
to expand nursing enrollments in the State’s
community colleges, universities and health
science centers. The goals of the legislation
were to: [21]
-
Provide resources to increase enrollments
and support faculty salaries;
-
Encourage innovative ways to recruit
and retain students;
-
Amend the nursing financial aid program
to allow more flexibility in how funds
are administered to reach most successful
recruitment and retention strategies;
-
Increase the pool of qualified faculty
by expanding financial aid available
for students to pursue post-graduate
education and enter teaching;
-
Establish a nursing workforce data center
to help policymakers plan and monitor
nursing workforce; and
-
Reallocate money from the tobacco settlement
fund to use exclusively for nursing
education.
The
legislation created a Dramatic Growth
Fund to channel up to $22.5 million of
existing State funds to fast-growing nursing
programs to help increase enrollments
and faculty recruitment and retention.
Although this money already was available
to universities, the law specified that
nursing programs that met certain growth
levels now had first claim to the funds.
Schools could use the funds to support
faculty salaries and operating funds.
To help fill the faculty need, for example,
the legislation permitted nursing programs
to give in-State tuition to out-of-State
nurses who wanted to pursue a post-graduate
degree in Texas; in exchange, they had
to agree to teach at a nursing college
in the State.
In
addition to the Dramatic Growth Fund,
the law reallocated tobacco settlement
funds into nursing innovation grants that
provided $3.1 million for enrollment and
faculty recruitment and retention. All
the tobacco settlement funds were awarded
in 2001-2003.
In
2003, lawmakers passed legislation that
continued dramatic growth funding for
community colleges and academic universities.
Facing a growing budget deficit, the amount
of dramatic growth funds available to
schools of nursing dropped significantly
in the 2003-2005 biennium—to $5.6 million,
of which $1.6 million is available for
community colleges and $4 million for
general academic institutions. During
this biennium, the amount available from
the tobacco settlement funds, however,
increased slightly to $4.9 million.
In
addition to regular formula funding—totaling
$207 million in 2004-2005—the State provides
special item funding for professional
nurse education. As shown in Table 6,
more than $10 million in dramatic growth
funds were available in 2002-2003, along
with $3 million in tobacco fund earnings.
Up to $22.6 million in Dramatic Growth
funds were available in the 2001-2003
biennium; however, schools did not receive
the maximum amount available because,
in part, they did not increase enrollment
enough to earn all the allocated funds.
To be eligible, institutions had to increase
enrollment by 3 percent over 2000 levels
in 2001, and by 6 percent over fall 2000
levels in 2002. Table 6 shows the amount
of dramatic growth funds available to
schools of nursing and the actual amounts
awarded.
Table
6. Texas State Funding for Professional
Nurse Education (in millions)
|
TYPE
OF FUNDING |
FY
2002 - 2003 |
FY
2004 - 2005 |
FY
2006-2007 (projected) |
|
Regular
Formula Funding |
|
Community and Technical Colleges |
$77.3 |
$83.1 |
|
|
General Academic Universities |
72 |
75.9 |
|
|
Health-related Institutions |
47.5 |
47.8 |
|
| Subtotals |
$196.8 |
$206.8 |
|
|
Special-Item
Funding |
|
Dramatic
Growth |
|
Community and Technical Colleges |
$5.6 |
$1.2 |
$7.1 |
|
General Academic Universities |
3.7 |
4 |
5.3 |
|
Health-related Institutions |
1.6 |
|
5 |
| Subtotals |
$10.9 |
$5.2 |
$17.4 |
|
Tobacco
Fund Earnings |
|
|
|
|
Community and Technical Colleges |
$1.8 |
$1.2 |
|
|
General Academic Universities |
0.7 |
2 |
|
|
Health-related Institutions |
0.6 |
0.7 |
|
| Subtotals |
$3.1 |
$3.9 |
$4 |
|
Nurse
Success Supplement |
|
|
|
| Community
and Technical Colleges |
|
|
$8 |
| General
Academic Universities |
|
|
8 |
| Health-related
Institutions |
|
|
4 |
| Subtotals |
|
|
$20 |
|
Scholarship
and Loan Programs |
$0.8 |
$0.5 |
$4.9 |
|
Higher
Graduate Education Rates |
|
|
$1.4 |
| GRAND
TOTALS |
$211.6 |
$216.4 |
$47.7 |
Source:
Texas Higher Education Coordinating Board
and the WorkSource for the
Gulf Coast Region's Health Services Steering
Committee, January 2005
Although
it is too soon to evaluate the effect
of the additional special item funds on
expanding the nursing supply, anecdotal
evidence suggests that the increased funds
have made it possible for schools of nursing
to increase enrollment. [22]
According to the Texas Higher Education
Coordinating Board, the State’s nursing
programs “ … have done a good job of increasing
interest in nursing, admitting more students,
and graduating more RNs.” [23]
Moreover,
the trends indicate that the State’s schools
of nursing have seen a turnaround in enrollments
and graduations. According to the Texas
Nurses Association, enrollment levels
began climbing between 2000 and 2003,
from 11,589 to 14,850—for a growth of
28 percent. This followed a 3 year decline
in enrollment from 1997 through 2000,
as shown in Figure 30.
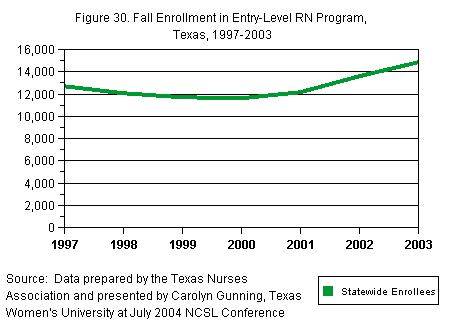 [D] [D]
Entry
level gains are occurring in all RN levels,
including diploma and associate degree
programs, where first-year enrollment
nearly doubled from 2,653 in 1999 to 5,181
in 2003. Among BSN programs, first- year
enrollment jumped from 1,434 to 3,404.
When combined, first-year entering enrollment
in RN programs increased by 87 percent
between 1997 and 2003, according to the
Texas Higher Education Coordinating Board.
Similarly,
as shown in Figure 31, graduation levels
in programs leading to initial RN licensure—that
had declined every year from 1997 through
2002—increased between 2002 and 2003,
when graduations jumped by 17 percent,
from 4,495 to 5,243.
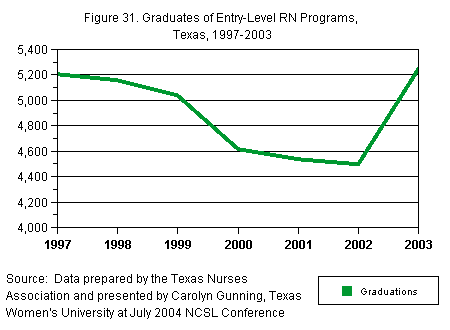 [D] [D]
Source:
Data prepared by the Texas Nurses Association
and presented by Carolyn Gunning, Texas
Woman’s University at July 2004 NCSL conference.
In
the 1 year period between 2002 and 2003,
the AACN reported that enrollment in Texas
nursing programs increased significantly,
by almost 11 percent in entry-level programs,
by 16 percent in master’s degree programs
and by 25 percent in doctoral programs.
Despite
the good news, the faculty shortage persists
in Texas. According to the Texas Higher
Education Coordinating Board, graduates
from master’s and doctoral programs declined
by 23 percent between 1994 and 2003.
So, although enrollment in graduate nursing
programs is increasing, the “total number
of graduates is at a 10 year low.” [24]
Moreover, of those seeking higher degrees,
just 1 percent is pursuing teaching.
In sum, the faculty shortage persists.
-
Three health-related institutions that
offer doctoral degrees graduated only
44 graduates between 1994 and 2003,
according to the Texas Higher Education
Board. [25]
(These three institutions represent
half of all the state institutions that
offer a doctoral degree in nursing.)
-
Average entering class size of RN licensure
programs increased by 108 percent from
1999 to 2003; however, the average FTE
faculty increased only by 13 percent.
-
A coordinating board survey of State
nursing deans and directors found that
the ability to hire new faculty was
the greatest impediment to increasing
enrollments in nursing programs. Specifically,
the disparate salaries between nurses
in academia versus those in clinical
practice was seen as the greatest hiring
obstacle.
Utah.
In 2004, the Utah Legislature dedicated
funding to Utah’s seven State-funded nursing
programs. The $675,000 appropriation—the
first dedicated to nursing education—was
distributed in varying amounts to associate
and baccalaureate programs with the goal
of expanding the number of nurses in Utah.
The Legislature required schools to match
State funds.
The
State’s largest beneficiary, the Utah
College of Nursing, plans to use its appropriation
of $150,000 to hire two new doctoral-level
faculty who will be able to train 20 additional
people to be nurse educators. [26]
Utah
provides grants to help LPNs and RNs
repay their educational loans in exchange
for practicing in a shortage area for
at least two years. The average grant
amount under the Statewide Nurse Education
Financial Assistance Program is $15,000.
The program is funded by State and Federal
funds, including the National Health Service
Corps’ State Loan Repayment Program (NHSC
SLRP).
In
addition, the Utah State Office of Education
administers the School Nurses Incentive
Program, which provides grants of from
$200 to $26,500—averaging $15,000—to improve
the availability of RNs in public schools.
The State funds do not exceed one-third
of program costs; local districts provide
at least two-thirds of program costs.
Other
Resources for Nursing Education
Schools
of nursing are expanding their capacity
and increasing the diversity of their
students and faculty with the help of
several Federal programs. The Nursing
Reinvestment Act of 2002 (NRA, PL 107-205)
amended the Nursing Education and Practice
Improvement Act of 1998. The legislation.,
which provides support for workforce development,
includes nurse faculty loans, loan repayment
and scholarships, funds for nursing workforce
diversity, and funds for advanced education
nursing.
The
2004 nurse reinvestment appropriations
totaled $141.9 million and funded six
major efforts, including:
-
Advanced Education Nursing, $58.6 million;
-
Nursing Workforce Diversity, $16.4 million;
-
Nurse Education, Practice and Retention,
$31.8 million;
-
Loan Repayment and Scholarships, $26.7
million;
-
Nurse Faculty Loan, $4.9 million; and
-
Comprehensive Geriatric Education, $3.5
million.
Among
the types of programs funded through the
NRA are Web-based accelerated BSN programs,
distance education programs designed to
remove barriers for RNs who do not live
close to a school of nursing, nursing
residency programs to help RNs entering
specialty fields, and career ladder programs.
Each
of the five States received funding from
one or more of the above programs. Some
examples of Federally funded programs
in the five States follow. For example,
the Loma Linda University School of Nursing
in California received funds for its Pipeline
to Registered Nursing program, which has
as its goal the creation of a more diverse
workforce. The university uses the funds
to encourage young, ethnically diverse
elementary, middle and high school students
to pursue a nursing career and also provides
retention activities to help students
succeed in their nursing programs.
The
Medical College of Georgia’s School of
Nursing—the State’s “primary institution
for the training of health professionals”—uses
Federal workforce diversity grant funds
to support various activities aimed at
increasing diversity in the school’s baccalaureate
nursing program. The school uses funds
to help recruit and prepare future nursing
students—in high school and a pre-nursing
program at Paine College—by exposing them
to the profession and providing academic
guidance and support. In addition to
recruitment strategies, the grant also
funds retention strategies aimed at helping
students succeed. One example is a supplemental
instruction course that helps to increase
academic performance and retention through
study strategies and tutoring. [27]
The
Ivy Tech State College in Indiana received
funds for its Nursing Careers Advancement
Program, which helps nurses advance their
education. In addition to helping RNs
advance, the program also focuses on attracting
nontraditional students into the nursing
pipeline, including males and racial and
ethnic minorities. In addition, students
in rural areas will participate via distance
education.
Federal
funds also support the Consortium to Advance
Nursing Diversity and Opportunity at the
University of Texas Health Sciences
Center at Houston, as well as a Closing
the Gap project at the University of Texas
at Arlington, which aims to increase nursing
education opportunities for racial and
ethnic minorities, and for individuals
from disadvantaged backgrounds.
In
2004, HRSA provided $736,831 to the Utah
College of Nursing for its Diversity Recruitment,
Retention and Leadership Development Program.
With these funds, the program will offer
stipends and scholarships of from $3,000
to $5,000 to 44 baccalaureate students
during the next three years. [28]
In
addition to funding from U.S. DHHS, States
also are benefiting from Federal workforce
development support from the U.S. Department
of Labor (DOL). Georgia was one of four
States to receive a Federal grant for
$754,000 to train dislocated workers for
health care jobs where there are shortages.
The Healthcare Retraining Partnership
Initiative Demonstration Grant will support
a number of activities, including attracting
new individuals to the health professions,
providing so-called bridge training (helping
current health care workers upgrade their
skills), faculty training and various
youth activities designed to attract more
students into the pipeline. They also
are working with the Department of Workforce
Services to explore using Federal DOL
funding.
Private
and Other Support for Nursing Education
Each
of the five States has benefited from
private sector and foundation support.
In California, one media source reported
that hospitals alone have helped California’s
community colleges and universities expand
enrollment in nursing programs by up to
20 percent between 1999 and 2000. These
contributions have resulted in improved
enrollment and retention. Some examples
include the following.
-
In 2003, the Gordon and Betty Moore
Foundation approved a $110 million Betty
Irene Moore Nursing Initiative to “improve
the quality of nursing-related patient
care” in the San Francisco Bay area.
The foundation is funding projects that
help increase the supply of RNs and
increase the number of training programs.
In 2004, the initiative awarded a $5.5
million grant to the San Jose State
University School of Nursing to increase
the number of graduates and educate
additional nursing faculty. Among the
outcomes of this project will be an
additional 45 faculty members over a
five-year period. [29]
-
The Washington Hospital District’s board
awarded a $1.5 million grant to Ohlone
College for its nursing program. The
college will use the money to hire two
full-time faculty members, allowing
it to enroll at least 18 additional
students per year.
-
California’s Sutter Roseville Medical
Center donated $750,000 to Sierra College
to expand its online nursing degree
program—enabling the program to add
20 more students per year for two years
to its on-line associate nursing degree
program, beginning in 2006. This donation
follows a $15 million pledge Sutter
made to help Sacramento City College
educate hundreds of new nurses. [30]
A
group of Georgia hospitals contributed
funds to nursing schools for scholarships,
faculty salaries, tuition reimbursement,
lab supplies and other educational resources.
From 1999 to 2002, they provided more
than $21 million in educational support
for nursing students and programs.
The
Health Care Summit Commission in San Antonio,
Texas—a partnership of local and State
governments, foundations, hospitals and
others—committed to raising $750,000 to
increase the number of graduating nurses
at area schools by 500. These funds are
used to finance student scholarships and
new Faculty salaries.
In
Utah, a group of hospitals provided one-time
funding to help fund more nursing program
slots. [31]
In addition, the Emma Eccles Jones Foundation
donated $1 million to renovate the college
for nursing research.
States
and others are addressing the nursing
shortage on various fronts. In addition
to the above financial strategies, States,
health care providers, educational institutions
and others also are attempting to expand
the nursing supply through other approaches,
including improving the workplace, enhancing
data collection and planning efforts,
and streamlining educational requirements.
Strategic
Planning and Data Collection
In
1999, California lawmakers passed Assembly
Bill 655 (1999 Cal. Stats., Chap. 954),
which required the chancellors and presidents
of the four higher education systems in
California to develop a joint strategic
plan for expanding enrollment in basic
RN education programs. The California
Strategic Planning Committee for Nursing
prepared the report in 2000. In response
to the report’s recommendations for more
funding, the Legislature earmarked $18.5
million for implementation; however, the
governor vetoed this increase in July
2000. [32]
Also
in California, the Office of Statewide
Health Planning and Development operates
the Health Careers Training Program, which
is designed to promote public and private
partnerships and develop training and
funding resources and jobs for unemployed
and dislocated workers. The program’s
goals include promoting community collaborations,
identifying funding sources for recruitment
and retention activities, identifying
curriculum and training needs, and developing
innovative employment opportunities. [33]
Several
States, including Georgia, established
workforce commissions or advisory groups
to gather information about nursing supply
and demand and to develop strategies for
workforce planning. The General Assembly
passed legislation in 2001 creating the
Healthcare Workforce Policy Advisory Committee.
The committee was charged with monitoring
and addressing the workforce supply, demand,
distribution, mix and quality of health
care professionals. By the end of its
first year, the committee published a
report, Promoting Health Care Workplace
Excellence and includes among its
accomplishments action by the legislature
to permit a tripling of available funding
for service cancelable loans for health
professions students.
In
1995, the Indiana General Assembly directed
the Indiana Health Care Professional Development
Commission to study the current and future
health care needs, develop long-range
planning goals, and submit recommendations
to the General Assembly on how to best
“ … achieve a continual flow of health
care professionals, appropriately distributed
geographically and by specialty and type.”
[34] At
the commission’s recommendation, for example,
in 1997 and 2001, the Indiana State Department
of Health (ISDH) and the Indiana Health
Professions Bureau (HPB) conducted the
Indiana Registered Nurse Survey. The
goal of the project was to gather data
on the supply and distribution of RNs
in Indiana.
In
2003, the Indiana Nursing Workforce Development
Steering Group, a volunteer body, underwent
a planning and development phase and became
the Indiana Nursing Workforce Development
Coalition Inc. The coalition’s vision
is to develop a “ … collaborative strategic
Statewide plan for nursing resources and
for communicating a consistent message
regarding nursing.” [35]
The
Department of Health set up the Indiana
Health Care Professional Development Commission
to come up with a strategic plan to ensure
an adequate supply and distribution of
health care professionals, including nurses.
In
Texas, the Nursing Shortage Reduction
Act of 2001 created a nursing workforce
data center to inform policymakers about
nursing supply and demand and to help
guide workforce planning efforts. (The
workforce center was authorized but was
not funded until 2003 when lawmakers funded
it through increased licensing fees for
nurses.)
In
Utah, the Nursing Leadership Forum is
comprised of representatives from various
organizations—including deans from all
nursing schools, chief nurse officers
from several hospitals, the Utah Nurses
Association, the Board of Regents, the
Utah Nurse Managers and the State Health
Department.
Schools
of Nursing streamlining requirements
Streamlining
and simplifying academic requirements
represent one approach for expanding the
supply of nurses. By ensuring a standard
set of required courses, States not only
facilitate transfers among State schools
of nursing, but also eliminate redundant
coursework and thus reduce the time needed
to complete a degree for individuals who
switch institutions or upgrade their degree
(from a licensed practical nurse to registered
nurse, for example).
In
2002, the California Legislature passed
a law that encouraged community colleges
and universities within the California
State University system to standardize
all nursing education program prerequisites
and establish articulation agreements
with campuses.
The
Georgia Perimeter College offers two tracks
for students to receive an associate degree
in nursing: a generic, two-year track
and an accelerated bridge track for applicants
who are already LPNs. In addition, graduates
can pursue a BSN degree at a University
System of Georgia College through an
articulation program that facilitates
credit transfer and recognizes the class
and clinical experience graduates bring.
[36]
Similarly,
the community college system in Indiana
is working to improve articulation across
programs, from LPN to RN, associate to
baccalaureate, and baccalaureate to master’s
degree. [37]
In
Texas, the State coordinating board approved
a standard set of courses—the Field of
Study Curriculum—that helps students transfer
to other schools without having to repeat
courses. These changes alone save as
much as two years of repetitive coursework.
[38]
Utah
schools have enacted numerous administrative
changes to expand the number of nurses
who go through the system, including:
-
Develop RN refresher and reactivation
courses, delay retirements, increase
retention, and encourage industry investment
in educating more nurses;
-
Accelerate programs, remove barriers
to obtaining degrees, and import more
nurses;
-
Add summer semester and examine shortening
the curriculum (LFA Report);
-
Offer nurse re-entry program as a joint
effort of the UHA and Weber State to
help former nurses whose licenses have
lapsed regain licensure.
Similarly,
many schools in Georgia have found ways
to enroll more students through fast-track,
slow-track, year-round admissions, satellite
locations, nontraditional schedules and
distance learning. [39]
Workplace
Improvements
Several
States have taken steps to improve the
nurse work environment. Many argue that
these measures are critical because they
help retain nurses who are currently in
the workforce, bring back those who have
left, and, further, help with recruiting
efforts by making nursing an attractive
field to pursue. California lawmakers,
for example, passed legislation to improve
work conditions for nurses who already
are in the workforce and thus aid in retention.
Separate laws enacted restrictions on
mandatory overtime and a 1999 law established
minimum nurse staffing ratios. The Texas
Legislature also enacted whistleblower
protections and workplace safety measures.
Hospitals
and other health care employers also are
taking an active role in improving the
overall working environment. As part
of its recruitment and retention campaign,
the Candler Hospital in Georgia, for example,
sought credentialing as a magnet hospital
in 2002. (Hospitals achieve magnet status
after they meet several quantitative and
qualitative standards developed by the
American Nurses Credentialing Center.
They are associated with increased job
satisfaction and improved health outcomes.)
Among the recruitment and retention efforts
implemented by the hospital: flexible
staffing, financial incentives for nurses
that move from part-time to full-time,
referral bonuses and tuition reimbursement.
Conclusion
Each
of the five States faces nursing shortages
brought on by a rapidly aging population
and a declining nursing workforce. They
are addressing these problems through
a variety of legislative and other approaches.
Table 7 summarizes the challenges and
opportunities facing each State, which
leads to the next chapter on policy options
and recommendations. Solutions that work
in one State may not be the top priority
of another, so an understanding of the
critical challenges facing each State—as
well as their strong suit—helps to determine
which policy courses they should pursue.
Table
7. Five States’ Challenges and Opportunities
|
State |
Challenges |
Opportunities
and Strengths |
|
California |
- Lack
of institutional capacity:
-
Nursing programs turning away
up to 40 percent of qualified
applicants.
-
Nurses educated elsewhere:
importing from other States
and countries.
-
Waiting lists at all levels;
no entry-level baccalaureate
program in University of California
system.
- Severe
State budget constraints limit
State funding potential.
- Concerns
about workplace environment, including
insufficient staffing, mandatory
overtime, lack of appreciation
and wages and benefits. [40]
|
-
Strong private and foundation
role.
-
Addressing work conditions through
private sector and legislative
initiatives.
-
Targeting WIA funds to nursing
education.
- Modest
enrollment gains.
- Strong
data collection infrastructure.
-
Strong stakeholder relationships;
they assembled to gather data
and conduct strategic planning.
|
|
Georgia |
- Lack
of institutional capacity:
-
Georgia not educating enough
of their own nurses; instead,
the State relies on nurses
who were educated in other
States.
- Insufficient
pipeline despite enrollment gains;
graduations still lagging.
-
Demand for health professionals
—at 37 percent—outpaces National
rate of 30 percent. [41]
- Vacancy
rates for hospitals and long-term
care providers. Private providers
report vacancy rates ranging from
10 percent to 15 percent for RNs.
[42]
-
Financially struggling hospitals:
60 percent of all Georgia hospitals
lost money in 2003 providing patient
care. [43]
|
- Strong
and established models of public-private
partnership, with significant
investments by employers, nursing
schools and the State.
- Significant
foundation and private support
and commitment.
- Strategies
in place—Statewide P-16 Council—to
create a coordinated preschool
through college educational system.
- Efforts
and initiatives in place to recruit
and support at-risk students.
-
Enrollment rising (50 percent
gain between 2000 and 2002 for
gain of 4,000 new RNs).
- Modest
increases in master’s and doctoral
degree enrollment.
- Number
of licensed nurses increasing.
- Public-private
investments producing more nurses—ICAPP
program expected to produce up
to 1,300 new nurses over two years.
- Addressing
faculty shortage directly.
-
Using Federal funds for nursing
education.
|
| Indiana |
- Lack
of institutional capacity:
-
Turning away increasing number
of qualified applicants because
of faculty shortage; Indiana
University School of Nursing
turned away 25 percent of
applicants.
- Insufficient
workforce:
-
Lowest rate of nurse practitioners
and certified nurse-midwives
in the nation; second to lowest
rate of nurse anesthetists
in the nation.
-
Number of new LPNs and RNs
dropped between 1994 and 2001,
with new LPNs dropping by
nearly 30 percent.
-
Expanding available labor pool
is necessary:
-
Shrinking pool of young workers:
while 18- to 24-year olds
decline by 3 percent between
2000 and 2025, the over-65
population will increase by
62 percent.
-
Survey: lack of interest among
high-achieving high school
graduates. [44]
|
-
Increased interest in nursing
education: applications for entry-level
baccalaureate programs up 64 percent
between 2000 and 2002.
- Enrollment
gains at all levels; reversing
negative enrollment trends; entry-level
RN programs up by 11 percent;
2003 enrollment in master’s and
doctoral programs up by 19 percent
and 4 percent, respectively, from
2002 to 2003.
- Number
of RNs practicing in Indiana up
by 18 percent between 1997 and
2001.
-
Increase in doctoral prepared
nurses.
-
Increase in State tax appropriations
for higher education between 2002
and 2004.
- Demand
for nurses growing more slowly
than four other States.
- RNs
per capita best of five States,
but still below National average.
- Improving
articulation among nursing programs.
|
| Texas |
- Lack
of institutional capacity; turning
away one-fifth of applicants.
- Faculty
shortage impeding expansion efforts:
“the lack of budgeted faculty
positions is the greatest impediment
to increasing enrollments.” [45]
-
Declining enrollment in master’s
and doctoral programs, down
23 percent between 1994 and
2003.
-
Faculty salaries not competitive,
especially in the community
colleges.
-
Students in graduate nursing
programs pursuing clinical
practice in greater numbers
than teaching.
|
-
Formula funding for colleges,
universities and health-related
institutions increased between
2002 and 2005.
- Used
existing funds to support nursing
education; targeting recruitment
and retention with dramatic growth
and tobacco settlement funds.
-
Established nursing workforce
center
-
Increasing racial and ethnic diversity
among RN graduates. [46]
-
Developed set of common courses
to ease transfers and eliminate
repeated courses.
|
| Utah |
-
Lack of institutional capacity:
-
Schools accepting only one-third
of qualified applicants (Utah
College of Nursing admitted
just 100 of 266 applicants).
-
One-third of nursing educators
planning to retire in next
five years.
-
Salary inequities thwart recruitment
and retention efforts.
- Inadequate
nursing supply:
-
Ranks third worst in RN per
capita ratio behind Nevada
and California.
-
RN vacancy rate in nursing
homes highest in country at
24 percent.
- Hospitals
spending significant amounts on
traveling nurses and overtime
and limiting patient care as a
result of nursing shortage.
-
Over-65 population growing by
116 percent, while rest of population
growing by 24 percent between
2000 and 2020.
|
-
Associate degrees on the rise.
-
Increased interest in nursing:
53 percent increase in applications
to RN programs between 2000 and
2002.
-
Increased admissions: 2003 admissions
higher than any other year and
70 percent greater than 1995 admissions.
-
Increased enrollment in master’s
and doctoral programs—up by 11
percent and 62 percent, respectively,
between 2002 and 2003.
-
Large, qualified pool of applicants.
- Healthy
State: leads nation in low prevalence
of smoking, low risk for heart
disease and low rate of cancer
cases.
|
Despite
the fact that each of the five States
has different shortage characteristics,
each State faces the same conundrum: they
need to expand their nursing supply, but
their current nursing education resources
are not sufficient to permit the needed
expansion. Standing in the way of this
badly needed expansion is a faculty shortage
that limits the number of students who
can enter the system, as well as other
factors, such as limited State and private
funds to add new nursing programs or expand
existing ones. States have been adapting
to fill some of the gaps—by importing
nurses from other States and countries
as Georgia and California do, for example—but
most recognize that these measures are
not long-term solutions.
Chapter
3 outlines policy options and solutions
that have worked in these five States
and others to expand the nursing pipeline
and, ultimately, to achieve the goal of
increasing the nursing supply to meet
future demand. What works in one State
may not be the best approach in another.
In California, for example, where schools
of nursing across the State are turning
away qualified applicants, expanding program
capacity may better meet short- and long-term
needs than recruiting more potential students.
Moreover, each State faces specific shortfalls:
while California policymakers may identify
a need to increase the numbers of baccalaureate
trained nurses, policymakers in Texas,
for example, may focus resources on increasing
enrollment in master’s and doctoral-level
programs leading to a teaching career.
[1].
Carolyn Gunning, “The Gulf Coast Healthcare
Collaborative” (presentation made at the
NCSL annual meeting, July 2004).
[2]. Texas Higher Education
Coordinating Board, “State Funding for
Professional Nurse Education” (Austin,
Texas: Texas Higher Education Board, January
11, 2005, e-mailed spreadsheet).
[3]. American Association
of State Colleges and Universities, State
Fiscal Conditions: Options Narrow, Pressures
Mount as Budget Crunch Drags On (Washington,
D.C.: AASCU, 2003), 4.
[4]. Deborah Greene,
Janet Allen and Tim Henderson, The
Role of States in Financing Nursing Education
(Washington, D.C.: NCSL, 2003).
[5]. Steve Boilard, California
Legislative Analyst’s Office, e-mail message
to author, February 5, 2005.
[6]. California Legislative
Analyst’s Office, An Assessment of
Differential Funding, (Sacramento,
Calif.: LAO, September 2004), http://www.lao.ca.gov/2004/diff_funding/Differential_Funding_Report_091504.pdf.
[7]. Boilard, e-mail
message.
[8]. Kathy Reeves Bracco,
State Structures: Georgia Case Study:
Work Processes (N.p.: The California
Higher Education Policy Center, 1997),
http://www.capolicycenter.org/georgia/georgia4.html.
[9]. The University System
of Georgia, Why We Are Where We Are,
(Atlanta.: USG, September 2004), http://www.usg.edu/pubs/budgetdocs/whywhere.pdf.
[10]. University System
of Georgia, “Legislative Update: Governor
Recommends Full Formula Funding, 2% Pay
Raises” (Atlanta: USG, January 18, 2005,
press release), http://www.usg.edu/pubs/lu/2005/01.18.05.pdf.
[11]. The University
System of Georgia, “Regents Recognize
‘Best Practices’ Within University System”
(Atlanta: USG, November 17, 2004, press
release), http://www.usg.edu/news/2004/111704.phtml.
[12]. Michael Baumgartner,
Indiana Commission for Higher Education,
e-mail message to author, February 3,
2005.
[13]. Kathy Reeves Bracco,
State Structures: The Texas Case Study:
Coordinating Processes for Texas Higher
Education (N.p.: The California Higher
Education Policy Center, Spring 1997).
[14]. National Conference
of State Legislatures, Medicaid Direct
and Indirect Graduate Medical Education
Payments: A 50-State Survey (Washington
D.C.: NCSL, December 2003).
[15]. California Department
of Finance, Budget Summary 2005-2006,
http://govbud.dof.ca.gov/BudgetSummary/BUDGETSUMMARYOVERVIEW/section1_1.html.
[16]. Georgia Student
Finance Commission, Education Loans
with Service Cancelable Benefits (Tucker,
Ga.: GSFC, 2004) http://www.gsfc.org/Main/publishing/pdf/2004/scl_brochure.pdf
[17]. The University
System of Georgia, “USG Distributes $2.05
Million to Keep Tackling Health-Care Shortage,”
(Atlanta: USG, August 8, 2004, press release).
[18]. The University
System of Georgia, “10-Year USG Admissions
Analysis Shows Good Progress in Attracting
Strong Students” (Atlanta: USG, January
11, 2005, press release).
[19]. Georgia Department
of Community Health, Healthcare Workforce
Policy Advisory Committee, Condition
Guarded, Fiscal Year 2003 Annual Report
(Atlanta: GDCH, August 2003).
[20]. Georgia Department
of Community Health, Healthcare Workforce
Policy Advisory Committee, What’s Ailing
Georgia’s Health Care Workforce? Serious
Symptoms. Complex Cures (Atlanta:
GDCH, August 2002).
[21]. Alexia Green et
al., “Addressing the Nursing Shortage:
A Legislative Approach to Bolstering the
Nursing Education Pipeline,” Policy,
Politics & Nursing Practice 5,
no. 1 (February 2004): 41-48.
[22]. Karen Love, the
WorkSource, e-mail message to author,
January 2005.
[23]. Marshall Hill,
“Increasing Capacity and Efficiency in
Programs Leading to RN Licensure in Texas”
(presentation at the SHEEO Professional
Development Conference, August 14, 2004).
[24]. Ibid.
[25]. Texas Higher Education
Coordinating Board, Increasing Capacity
and Efficiency in Programs Leading to
Initial RN Licensure in Texas (Austin,
Texas.: THECB, July 2004), http://www.thecb.State.tx.us/UHRI/reports.cfm.
[26]. Andrew Kirk, “U
Nursing Initiative Gets What it Needs,”
The Daily Utah Chronicle, March
4, 2004, http://www.dailyutahchronicle.com/global_user_elements/printpage.cfm?storyid=626260.
[27]. Medical College
of Georgia School of Nursing, Nursing
Workforce Diversity Grant Web page, http://www.mcg.edu/son/diversity/index.htm.
[28]. University of
Utah, “Grant Boosts U College of Nursing’s
Diversity Efforts” (Salt Lake City: UU,
November 19, 2004, news release), http://www.utah.edu/unews/releases/04/nov/nursing.html.
[29]. Gordon and Betty
Moore Foundation, “Gordon and Betty Moore
Foundation to Fund Betty Irene Moore Nursing
Initiative” (San Francisco: November 2003,
news release), http://www.moore.org/news/2003/news_pr_111303nursing.asp.
[30]. Lisa Rapaport,
“Sutter Gives Funds for Nurse Education,”
The Sacramento Bee, November 17,
2004, http://www.sacbee.com/content/business/story/11449967p-12364137c.html.
[31]. Maureen Keefe,
University of Utah College of Nursing,
telephone interview by author, November
2004.
[32]. Janet Coffman,
“States’ Options for Addressing Nursing
Workforce Challenges” (presentation at
annual meeting of the National Conference
of State Legislatures, August 2001).
[33]. California Office
of Statewide Health Planning and Development,
Healthcare Workforce and Community Development
Division, “The Health Careers Training
Program,” Web page, http://www.oshpd.cahwnet.gov/HWCDD/professions/hctp.htm.
[34]. Indiana Health
Care Professional Development Commission,
2001 Annual Report (Indianapolis, Ind.:
ISDH, 2001), http://www.in.gov/isdh/publications/2001report/toc.htm.
[35]. Indiana Nursing
Workforce Development Steering Group,
The Nursing Workforce Shortage in Indiana:
Current Status and Future Trends (Indianapolis,
Ind.: INWD, 2002), www.indiananursingworkforce.org.
[36]. Georgia Perimeter
College Nursing Department, home Web page,
http://www.gpc.edu/~nursing/.
[37]. Indiana Nursing
Workforce Development Steering Group,
The Nursing Workforce Shortage in Indiana:
Current Status and Future Trends (Indianapolis,
Ind.: Indiana Nursing Workforce Development
Steering Group, 2002).
[38]. Texas Legislature,
Senate Subcommittee on Higher Education,
“Request for Information From March 29,
2004 Hearing” (Austin: Texas Legislature,
2004). http://www.thecb.State.tx.us/HealthRelated/NursingShortageHearing032904.pdf.
[39]. Valerie Hepburns,
“Nursing Education and State Policy: The
Georgia Experience” (presentation at the
National Conference of State Legislatures
State Nursing Education Summit, San Diego,
Calif., September 2003).
[40]. Janet Coffman,
Joanne Spetz, Jean Ann Seago, Emily Rosenoff
and Edward O’Neill, Nursing in California:
A Workforce Crisis (San Francisco,
Calif.: California Workforce Initiative
and the UCSF Center for Health Professions,
January 2001).
[41]. Ibid.
[42]. Georgia Department
of Community Health, Healthcare Workforce
Policy Advisory Committee, Condition
Guarded, Fiscal Year 2003 Annual Report
(Atlanta: GDCH, August 2003).
[43]. Georgia Hospital
Association, Economic Analysis of Hospital
Providers in the State of Georgia
(Marietta, Ga.: Deloitte Consulting, October
2004).
[44]. Indiana Nursing
Workforce Development Steering Group,
“The Nursing Workforce Shortage in Indiana:
Current Status and Future Trends” (Indianapolis,
Ind.: INWD, 2002), www.indiananursingworkforce.org
[45]. Marshall Hill,
“Increasing Capacity and Efficiency in
Programs Leading to RN Licensure in Texas”
(presentation at the SHEEO Professional
Development Conference, August 14, 2004).
[46]. Ibid. |