|
This study marks the first research effort
that utilized a survey of verified employers
i-n all 50 States to draw a profile of
the community health workers (CHWs) workforce.
Also, for this study, it was possible
to use recent refinements in occupational
and industry data,[1]
new reviews of the relevant literature,
and collaborations with four concurrent,
independently funded initiatives in CHW
support,[2]
education,[3]
and research promotion.[4]
Extent and Nature
of Current Research
An indicator of the degree of involvement
of the research community in any one topic
is the number of published journal articles
addressing that topic. Figure 6.1 compares
journal publications since 1965 in five-year
intervals.[5]
The increase in volume is significant:
from 62 articles in the 1970s to nearly
400 in the 1990s.
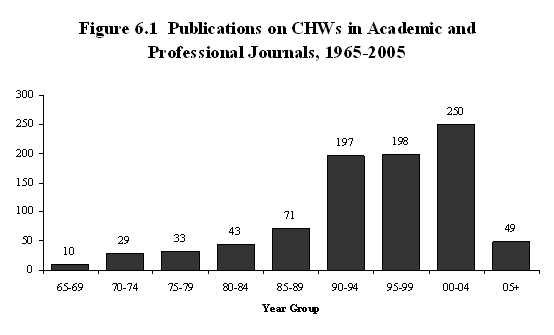 [D] [D]
Source: CHW National Workforce Study
(CHW/NWS) (2006).
The quality and the scope of research
within this pool of sources varied from
few rigorous evaluations of specific medical
interventions utilizing CHWs to many descriptive
reports of CHW programs. Many studies
suffered from small sample sizes, poor
research designs, and lack of control
groups. Rigorous longitudinal studies
were needed to clearly isolate the CHW
interventions and measure outcomes and
cost effectiveness.
Findings From Literature
Reviews
Nine literature reviews were published
between 2002 and 2006 to evaluate the
use of community health workers in specific
primary care and medical specialty interventions.
These reviews represent the best available
assessments of findings from research
on health interventions that included
the use of CHWs. No peer-reviewed journal
exists with a specific focus on CHW practice.
All of the articles reviewed represent
contributions to other fields such as
pediatrics and health education. Most
reported findings were statistically significant,
but not all of them had clinical significance.
Due to the variety of topics, methodologies,
and results, the collective research did
not provide a systematic evaluation of
CHW effectiveness and best practices.
It did present, however, valid-if fragmented-evidence
of CHW contributions to the delivery of
health care, prevention, and health education
for underserved communities. Also, these
literature reviews could provide a useful
framework on which to base future research.
No well-documented differences were found
between outcomes from programs involving
paid CHWs and volunteers. And, there were
no reports on the utilization of CHWs
in the private sector, as competitive
considerations kept the evaluation of
proprietary projects from being made public.
Table 6.1 displays the number and dates
of the studies examined, topics addressed,
and populations served by the interventions
reviewed.[6]
Then, each review is briefly described
and followed by a summary of findings
on cost effectiveness (Table 6.2).
Three of the nine reviews were limited
to the involvement of CHWs in interventions
addressing diabetes, heart disease/stroke,
and pregnancy in minority women. They
covered a total of 98 studies, of which
23 were included in more than one review.
Two reviews included only randomized controlled
trials (RCTs), and one excluded studies
measuring only changes in knowledge or
attitudes.
Table 6.1 Literature
Reviews of CHW Research Studies, 2002-2006
| Author,
Year |
Search
limited to |
Years
covered |
Number
of studies reviewed |
Number
of studies with reported results in
terms of: |
Location
and Population Served: Number of Studies
Specifying Each Characteristic†
|
| Health
care behaviors |
Awareness/
knowledge, attitudes |
Health-related
behavior |
Clinical
outcomes |
Urban
|
Rural
|
Men
|
Women
|
African-American
|
Hispanic/
Latino(a) |
Asian
|
Native
American |
| Andrews
2004 |
Minority
women |
1974,
1989-2002 |
24
|
15
|
7
|
11
|
2
|
17
|
7
|
0
|
24
|
15
|
5
|
1
|
4
|
| Brownstein
2005 |
Heart
Disease and Stroke |
1989-2003
|
6
|
4
|
0
|
0
|
4
|
6
|
0
|
3
|
0
|
6
|
1
|
0
|
0
|
| HRSA
2002 |
All
|
1991-1999
|
19*
|
18
|
6
|
5
|
2
|
12
|
7
|
1
|
7
|
9
|
10
|
1
|
0
|
| Lewin
2005 |
All
|
1972-2001
|
21*
|
9
|
1
|
7
|
13
|
20
|
1
|
1
|
13
|
4
|
1
|
0
|
0
|
| NFME**
2006 |
All
|
2002-2005
|
7
|
2
|
0
|
2
|
5
|
5
|
0
|
1
|
1
|
3
|
3
|
0
|
0
|
| Nemcek
2003 |
All
|
1974-1999
|
18***
|
9
|
2
|
2
|
5
|
13
|
5
|
2
|
4
|
6
|
8
|
0
|
0
|
| Norris
2006 |
Diabetes
|
1987-2003
|
15*
|
4
|
6
|
9
|
11
|
7
|
5
|
0
|
6
|
3
|
7
|
0
|
2
|
| Persily
2003 |
Prenatal
home visiting |
1987-2000
|
12*
|
9
|
3
|
1
|
5
|
3
|
1
|
0
|
12
|
0
|
2
|
0
|
0
|
| Swider
2002 |
All
|
1981-1999
|
19
|
14
|
2
|
8
|
3
|
15
|
0
|
1
|
9
|
3
|
4
|
1
|
0
|
Source: CHW/NWS (2006).
† A study was not counted
if the characteristic shown was not specifically
mentioned in the review.
* HRSA (2002): 19 of 20 studies reviewed
were in the U.S.; Lewin (2005): Of 24
U.S. studies, 21 were included and three
were excluded because they primarily referred
to the provision of paraprofessional clinical
care; Norris (2006): 15 of 18 articles
reviewed were in the U.S.; Persily (2003):
12 of 14 studies reviewed were in the
U.S.
** National Fund for Medical Education.
*** Nine of the 18 studies included were
program profiles in one report.[7]
Andrews 2004[8]
The evaluation, limited to research studies
involving ethnic minority women, found
that "[CHWs] are effective in increasing
access to health services, increasing
knowledge and promoting behavior change...."[9]
Only two of the cited studies described
clinical outcomes (reduction in low birth
weight (LBW) deliveries and weight loss).
The remaining 12 lacked a clear reference
to the theoretical framework supporting
the methods employed; 10 were descriptive;
6 were quasi-experimental; seven were
experimental; and one was a cross-sectional
pre-post design.
Andrews found that most of the studies
reported significant results for increasing
access to services, but that the investigators
differed in the definition of CHW roles
and responsibilities and in the retention
of participants, whose attrition ranged
from 16 to 60 percent. Andrews concluded
that CHW involvement in case management
was more successful for retention than
the more limited outreach role. Five of
the seven studies on increasing knowledge
on health behavior showed significant
results; the validity of findings in the
remaining two was limited by "high
attrition rates, small sample size and
lack of standardized instruments."
Two of the reviewed studies had positive
results in breastfeeding behavior, and
favorable reviews were given to single
studies on weight loss, drug use, high-risk
sexual behavior, and physical activity.
A study on diabetes self-care did not
show a measurable impact from the CHW
intervention. Two studies showed both
improved outcomes and reduced costs.
Brownstein 2005[10]
Brownstein's review of six studies related
to heart disease and stroke concluded
that CHW interventions were associated
with "significant improvements in
participants' blood pressure care and
control."[11]
Home visits by outreach workers "to
mobilize the patient's support system"
were more effective in hypertension control
than group education sessions.[12]
CHWs providing blood pressure (BP) monitoring,
education and follow-up (working with
nurse practitioners) produced significant
increases in appointment keeping and continuity
of care.[13]
CHWs teaming with a nurse and a physician
increased entry to care and reduced blood
pressure;[14]
a follow-up RCT combining hypertension
(HTN) care and medications with CHW visits
for education and for mobilizing family
support led, over a 3-year period, to
better care and better BP control than
a "usual-care" control group.[15]
A related Community-Based Participatory
Research (CBPR) project provided further
levels of training to CHWs, and compared
more- and less-intensive CHW interventions.
Both groups experienced significant increase
in BP control with no significant differences
in degree of improvement between the two
intervention groups.[16]
In a Medicaid population with diabetes
and hypertension, CHW care management
produced significant reductions in ER
visits, hospital admissions, and total
patient costs to the Medicaid program.[17]
HRSA 2002[18]
This review was developed for the Maternal
and Child Health Bureau (MCHB) as an exploratory
exercise in preparation for a national
cost-effectiveness study on the use of
CHWs in MCH programs. The evaluation studies
reviewed were selected for their relevance
to the design of the study, and the coverage
was not meant to be comprehensive.[19]
The principal relevance of this review
rests in identifying key considerations
for research on CHWs.
Lewin 2005[20]
This review of 43 RCTs excluded studies
measuring only changes in knowledge, attitudes,
or intentions, which "were not considered
useful indicators of the effectiveness
of [CHW] interventions."
The investigators concluded that CHWs
"show promising benefits" in
a limited range of health issues, including
childhood immunizations.
National Fund for Medical Education
2006[21]
This review was conducted to accompany
a study on financing and sustainability
of CHW services. It summarized findings
of earlier literature reviews and examined
seven RCTs published from 2002 to 2005.
Of these, one[22]
reported no positive effect in measuring
the role of CHWs in reduction of exposure
of children to tobacco smoke. Two suggested
positive effects but were included with
reservations over "shortcomings in
the design of the CHW role."[23]
The four remaining RCTs showed impact
on blood glucose in African-American men
with diabetes,[24]
on the participation by Hispanic women
in an annual comprehensive clinical exam,[25]
on smoking cessation by adult Latinos,[26]
and on blood pressure control in urban
African-Americans.[27]
Nemcek 2003[28]
Nemcek, writing from a nursing standpoint,
concluded that "the rationale is
strong for using CHWs to improve delivery
of community-based preventive care"
and that findings suggest roles for CHWs
in three domains: (1) developing a "therapeutic
alliance" between patient, provider,
and family/community support systems;
(2) risk reduction; and (3) improving
patterns of health care utilization.
Of 18 programs reported in 10 articles,
Nemcek found nine acceptable process and
outcome evaluations, two with only outcome
descriptions, and the remaining seven
with process evaluations only. Improved
utilization of services, including medical
appointment-keeping and less frequent
ER visits, were the most commonly reported
types of outcomes. Clinical outcomes included
reduction of low birth weight deliveries
and changes in blood pressure and sugar
levels. Changes in health-related knowledge,
treatment compliance, and lifestyles were
also included.
Nemcek found no useful information for
evaluating the structure of CHW programs
"because programs have lacked a standard
structure" and noted there was "a
dearth of CHW process and outcome evaluation
evidence in the literature... most reports
are not research studies and the use of
rigorous controls was not documented."
Norris 2006[29]
Norris et al. reviewed 18 articles evaluating
CHW interventions focusing on adults with
diabetes and showing client outcomes,
including eight RCTs. Multiple CHW roles
and activities were identified, and the
investigators concluded that there were
"some preliminary data demonstrating
improvements in participant knowledge
and behavior." Other research designs
included six before/after designs, three
non-randomized comparison studies, and
one with post-intervention measures only.
Persily 2003[30]
This review encompassed 14 studies, of
which one was not from the United States
and one was purely descriptive, limited
to programs intended to improve pregnancy
outcomes. Persily found that, although
"home visiting by lay workers may
be more accepted by pregnant women,"
published studies showed "mixed results."
Among the 14 studies on "lay home
visiting programs," eight showed
positive impact on use of prenatal care;
three of five, examining low birth weight
delivery, showed impact; and one study
showed impact on pre-term delivery. Three
studies reported impact on "social
support." Only one study (on child
abuse) showed no significant impact. However,
the review described weaknesses in the
studies such as the use of descriptive
or quasi-experimental designs, poorly
specified interventions, and lack of cost
analyses.
Swider 2002[31]
This review covered 19 CHW effectiveness
studies of various design from 1981 through
1999. Swider concluded that there was
some evidence for supporting CHWs in increasing
access to care, particularly for underserved
populations, but "inconclusive results"
regarding knowledge acquisition, clinical
outcomes, and behavioral changes. In most
of the studies reviewed, the CHWs' "primary
role expectations were not reported, nor
were details of the intervention they
provided." Therefore, only one of
four studies with a primary CHW role of
"outreach and case finding"
had positive outcomes.
Cost Effectiveness
Ten published studies[32]
were found that dealt with cost effectiveness
of, or return on investment (ROI) from,
CHW activities. In only two of these studies
did cost considerations constitute the
main topic of the published article.[33]
The limited number of studies and the
variety of measures used did not allow
meaningful conclusions overall.
In Table 6.2, the articles' health-related
objectives, outcome measures, and cost-effectiveness
results are displayed by author in alphabetical
order.
Table 6.2 Studies
| Lead
author |
Year
|
Health
issue |
Outcome
measures |
Cost-effectiveness
results |
| Barnes-Boyd
|
2001
|
Infant
mortality reduction |
Mortality
rates, program retention, health problems
identified, immunization rates |
Implied
cost-saving potential in that outcomes
with nurse-CHW team were at least
equal to those of nurse-only team
(no computation of cost savings) |
| Beckham
|
2004
|
Asthma
management |
Reported
symptoms, doctor visits, emergency
department (ED) visits |
Total
per capita costs reduced from $310
to $129; ED costs reduced from $1,119
per participant to $188 |
| Black
|
1995
|
Non-Organic
Failure to Thrive (NOFTT) |
Child
development measures, parent-child
interaction scores |
Costs
of intervention "generally consistent
with" other home-visiting programs
($1,709 to $6,200 per year) |
| Fedder
|
2003
|
Diabetes
management |
ED
visits, hospital admissions, quality-of-life
indicators |
Cost
to Medicaid reduced an average of
$2,245 per patient per year |
| Krieger
|
2000
|
Older
adult flu and pneumonia prevention
|
Immunization
rates |
Marginal
cost per additional vaccine administered
= $117; options for lower cost discussed
|
| Krieger
|
2005
|
Asthma
(indoor triggers) |
Caregiver
quality of life; use of urgent health
services; symptom days |
Projected
four-year net savings $189 to $721
per participant |
| Sox
|
1999
|
Cancer
screenings for women |
Effectiveness
of trained Community Health Aides
performing clinical exams and Pap
smears (Alaska) |
Implied
cost saving in reduced travel of clinical
personnel to remote villages (no estimates)
|
| Weber
|
1997
|
Mammography
|
Rates
of mammography use |
Marginal
cost of CHW activity per additional
mammography performed = $375, equivalent
to $11,591 per year of life saved
|
| Whitley
|
2006
|
Primary
care utilization |
Utilization,
charges and reimbursements |
Cost
reduction of $14,244 per month, program
cost of $6,229 per month = ROI ratio
of 2.28:1 |
| Wolff
|
1997
|
Mental
illness |
Treatment
contact, psychiatric symptoms, satisfaction
with treatment |
Total
cost of treatment less with CHW but
not statistically significant: treatment
only, $49,510; treatment with CHW
team, $39,913; brokered case management,
$45,076 |
Source: CHW/NWS (2006).
[1] Appendix B.
[2] The CHW Programs
Inventory initiated by the Center for
Sustainable Health Outreach (CSHO) of
The University of Southern Mississippi
under a grant from the W. K. Kellogg Foundation
(WKKF) became the starting point for the
CHW National Employer Inventory (CHW/NEI)
through a partnership agreement with CSHO.
Also, the Albuquerque, Miami, Northern
Manhattan, Oakland, and FirstHealth (North
Carolina) Community Voices sites provided
feedback to develop contacts for the CHW/NEI
in their respective States.
[3] The Community Health
Worker National Education Collaborative
(CHW-NEC) initiative explored, under a
grant from the U.S. Department of Education's
Fund for the Improvement of Postsecondary
Education, best practices for CHW education
and training and provided a taxonomy of
key areas for developing employable CHWs
(discussed in Chapter 4).
[4] The preparatory work
for a forthcoming invitational conference
to set a National research agenda on CHWs,
supported by the California Endowment,
The Northwest Area Foundation, The California
Health Care Foundation, The Health Care
Education-Industry Partnership of Minnesota,
and The California Wellness Foundation,
enhanced the material used in this chapter.
[5] The list of journal
articles was obtained from the bibliographic
database of 1,068 entries compiled for
this study. The 2005+ year group in Figure
6.1 includes nine articles from 2006.
[6] Appendix F contains
a table that shows selected articles by
author, date of publication, and health
issue addressed, which were included in
the nine reviews.
[7] Health Resources
and Services Administration. Impact of
community health workers on access, use
of services, and patient knowledge and
behavior. Bureau of Primary Health Care,
Health Resources and Services Administration,
U.S. Department of Health and Human Services
1998.
[8] Andrews JO, Felton
G, Wewers ME et al. Use of community health
workers in research with ethnic minority
women. J Nurs Scholarsh 2004; 36 (4):358-65.
[9] Ibid. (p.358)
[10] Brownstein JN,
Bone LR, Dennison CR et al. Community
health workers as interventionists in
the prevention and control of heart disease
and stroke. Am J of Prev Med 2005; 29
(5S1):128-33.
[11] Ibid. (p.132).
[12] Morisky DE, Levine
DM, Green LW et al. Five-year blood pressure
control and mortality following health
education for hypertensive patients. Am
J Public Health 1983; 73 (2):153-62.
[13] Bone LR, Mamon
J, Levine DM et al. Emergency department
detection and follow-up of high blood
pressure: use and effectiveness of community
health workers. Am J Emerg Med 1989; 7
(1):16-20.
[14] Hill MN, Bone LR,
Kim MT et al. A clinical trial to improve
high blood pressure care in young urban
black men: recruitment, follow-up, and
outcomes. Am J Hypertens 1999; 12:548-54.
[15] Dennison CR, Hill
MN, Bone LR et al. Comprehensive hypertension
care in underserved urban black men: high
follow-up rates and blood pressure improvement
over 60 months. Circulation 2003; 108:381.
[16] Levine DM, Bone
LR, Hill MN et al. The effectiveness of
a community/academic health center partnership
in decreasing the level of blood pressure
in an urban African-American population.
Ethn Dis 2003; 13 (3):354-61.
[17] Fedder DO, Chang
RJ, Curry S et al. The effectiveness of
a community health worker outreach program
on healthcare utilization of West Baltimore
City Medicaid patients with diabetes,
with or without hypertension. Ethn Dis
2003; 13 (1):22-7.
[18] Health Resources
and Services Administration. A literature
review and discussion of research studies
and evaluations of the roles and responsibilities
of community health workers (CHWs). Maternal
and Child Health Bureau, Health Resources
and Services Administration, U.S. Department
of Health and Human Services July 5, 2002.
[19] Ibid. (p.19).
[20] Lewin SA, Dick
J, Pond P et al. Lay health workers in
primary and community health care. Cochrane
Database of Systematic Reviews, 2005.
[21] National Fund for
Medical Education. Advancing Community
Health Worker Practice and Utilization:
The Focus on Financing. San Francisco
(CA): Center for the Health Professions,
University of California at San Francisco,
2006.
[22] Conway TL, Woodruff
SI, Edwards CC et al. Intervention to
reduce environmental tobacco smoke exposure
in Latino children: null effects on hair
biomarkers and parent reports. Tob Control
2004; 13 (1):90-2.
[23] Krieger JW, Takaro
TK, Song L et al. The Seattle-King County
Healthy Homes Project: a randomized, controlled
trial of a community health worker intervention
to decrease exposure to indoor asthma
triggers. Am J Public Health 2005; 95
(4):652-9; Hill MN, Han H-R, Dennison
CR et al. Hypertension care and control
in underserved urban African American
men: behavioral and physiologic outcomes
at 36 months. Am J Hypertens 2003; 16
(11):906-13.
[24] Gary TL, Bone LR,
Hill MN et al. Randomized controlled trial
of the effects of nurse case manager and
community health worker interventions
on risk factors for diabetes-related complications
in urban African Americans. Prev Med 2003;
37 (1):23-32.
[25] Hunter JB, de Zapien
JG, Papenfuss M et al. The impact of a
promotora on increasing routine chronic
disease prevention among women aged 40
and older at the U.S.-Mexico border. Health
Educ Behav 2004; 31 (4 Suppl):18S-28S.
[26] Woodruff SI, Talavera
GA, Elder JP. Evaluation of a culturally
appropriate smoking cessation intervention
for Latinos. Tob Control 2002; 11 (4):361-7.
[27] Levine DM et al.
(2003).
[28] Nemcek MA, Sabatier
R. State of evaluation: community health
workers. Public Health Nurs 2003; 20 (4):260-70.
[29] Norris SL, Chowdhury
FM, Van Le K et al. Effectiveness of community
health workers in the care of persons
with diabetes. Diabet Med 2006; 23 (5):544-56.
[30] Persily CA. Lay
home visiting may improve pregnancy outcomes.
Holist Nurs Pract 2003; 17 (5):231-8.
[31] Swider S. Outcome
effectiveness of community health workers:
an integrative literature review. Public
Health Nurs 2002; 19 (1):11-20.
[32] Published studies
in Table 6.2 are referenced in Appendix
I.
[33] Whitley EM, Everhart
RM, Wright RA. Measuring return on investment
of outreach by community health workers.
J Health Care Poor Underserved 2006; 17
(1 Suppl):6-15; Wolff N, Helminiak TW,
Morse GA et al. Cost-effectiveness evaluation
of three approaches to case management
for homeless mentally ill clients. Am
J Psychiatry 1997; 154 (3):341-8.
|