
U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES
The two key markers for chronic kidney disease (CKD) are urine albumin and estimated glomerular filtration rate (eGFR).
Assess urine albumin excretion yearly to diagnose and monitor kidney damage in patients with type 1 diabetes for five years or more or with type 2 diabetes.
UACR is a ratio between two measured substances. Unlike a dipstick test for albumin, UACR is unaffected by variation in urine concentration.
Albuminuria1 is present when UACR is greater than 30 mg/g and is a marker for CKD.
Albuminuria is used to diagnose and monitor kidney disease. Change in albuminuria may reflect response to therapy and risk for progression. A decrease in urine albumin may be associated with improved renal and cardiovascular outcomes.

In a large cohort of CKD patients, a higher UACR at time of diagnosis was associated with increased risk for renal events—loss of half of eGFR, dialysis, or death. (Chronic Renal Insufficiency Cohort study)
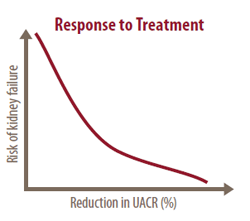
A randomized trial of diabetes patients with CKD found that the greater the reduction of UACR in response to treatment (with ARBs), the lower the risk of progression to kidney failure. (De Zeeuw D, et al. Kidney International, 2004:65:2309-2320)
1 Albuminuria is a term that describes all levels of urine albumin. Microalbuminuria is a term used to describe urine albumin levels not detected by a dipstick test, i.e., 30 mg/g–300 mg/g. Macroalbuminuria is sometimes used to describe albumin levels more than 300mg/g.
The two key markers for chronic kidney disease (CKD) are estimated glomerular filtration rate (eGFR) and urine albumin.
Calculate eGFR from stable serum creatinine levels at least once a year in all patients with diabetes.
See if your lab reports eGFR routinely. If it does not, ask your lab to do so. You can also calculate can eGFR yourself by using NKDEP's GFR calculators.

If kidney disease is detected, it should be addressed as part of a comprehensive approach to the treatment of diabetes.
PDF files require Adobe Acrobat
Page last updated: March 1, 2012