- Home
- Search for Research Summaries, Reviews, and Reports
EHC Component
- EPC Project
Full Reports
- Research Review Dec. 15, 2009
- Appendixes Dec. 15, 2009
Related Products for this Topic
- Disposition of Comments Report Mar. 11, 2010
- Consumer Summary Apr. 14, 2010
- La Guías Sumaria de los Consumidores Aug. 24, 2010
- Executive Summary Dec. 15, 2009
Clinician Summary – Apr. 14, 2010
Core-Needle Biopsy for Breast Abnormalities: Clinician's Guide
Formats
- View PDF (PDF) 266 kB
- Download Audio (MP3) 10.3 MB
- Help with Viewers, Players, and Plug-ins
Table of Contents
- Introduction
- Clinical Bottom Line
- Core-Needle Breast Biopsy
- Accuracy of Core-Needle Breast Biopsy
- Misclassification of Biopsy Results
- Complications and Pain
- Resource for Patients
- For More Information
- Source
Introduction
This guide compares core-needle biopsy with open surgical biopsy for diagnosing breast lesions. It also summarizes the accuracy and possible harms of various core-needle biopsy methods. This guide does not discuss fine needle aspiration, another method for sampling breast tissue that provides a smaller tissue sample than core-needle biopsy.
Clinical Issue
Breast cancer is the second most common malignancy of women, with approximately 250,000 new cases diagnosed each year. More than 180,000 of these cases are invasive breast cancer. Early detection and treatment improves survival. Routine screening with physical examination and mammography is widely used in the United States. Suspicious findings on mammography may require a biopsy for diagnosis.
Over 1 million women have breast biopsies each year in the United States. Between 20 and 30 percent of these biopsies yield a diagnosis of breast cancer.
Open surgical biopsy removes suspicious tissue through a surgical incision. This procedure requires either a general or local anesthetic and closure of the incision with sutures. Because more than half of such procedures lead to a negative diagnosis, many women who undergo open surgical biopsies derive no direct benefit from this potentially disfiguring procedure.
Core-needle procedures, which remove a small tissue sample through a very small incision, have been widely adopted as a less invasive biopsy option. Currently, more than half of all breast biopsies use a core-needle technique. It is important to determine the accuracy and possible harms associated with the widespread use of core-needle methods
Clinical Bottom Line
Clinical Bottom Line
- Core-needle breast biopsies have a lower risk of any type of complication than open surgical biopsies.
Level of Confidence
- The sensitivity of core-needle biopsies performed using either stereotactic or ultrasound guidance is 97 – 99 percent.
Level of Confidence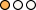
- Freehand core-needle breast biopsies have a lower sensitivity than biopsies performed using either stereotactic or ultrasound guidance.
Level of Confidence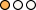
- More than 10 percent of core-needle breast biopsy specimens classified as atypical ductal hyperplasia or ductal carcinoma in situ are reclassified as invasive breast cancer on subsequent surgical biopsy.
Level of Confidence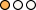
Confidence Scale
The confidence ratings in this guide are derived from a systematic review of the literature. The level of confidence is based on the overall quantity and quality of clinical evidence.
There are consistent results from good quality studies. Further research is very unlikely to change the conclusions.
Findings are supported, but further research could change the conclusions.
There are very few studies, or existing studies are flawed.
Core-Needle Breast Biopsy
Core-needle biopsy uses a hollow-core needle, ranging in size from 11 to 16 gauge, to remove one or more pieces of breast tissue. The operator either aims the needle directly to the area of a palpable lesion (freehand biopsy) or uses an imaging technique to localize the target lesion. The imaging techniques include stereotactic radiography, ultrasound, and magnetic resonance imaging (MRI). Techniques to extract the biopsy specimen include automated gun and vacuum assistance. There is no consensus on which of these techniques is preferable for attaining the highest accuracy and lowest rate of harm for core-needle breast biopsies.
Accuracy of Core-Needle Breast Biopsy
The goal of breast cancer screening programs is to detect cancers when they are small and can be most successfully treated. Early detection may require biopsy of suspicious abnormalities. Compared with open surgical biopsies, core-needle techniques may be less effectively targeted to the suspicious area of breast tissue. Therefore, they have the potential to miss an actual cancer (a false negative biopsy).
Sensitivity is an estimate of the proportion of all cases of cancer that are identified by a diagnostic test (in this case, core-needle biopsy). Research studies designed to measure sensitivity of core-needle biopsy generally use a second biopsy (with the open surgical method) or clinical followup over time to detect cancers that were missed.
The quality of the studies on the accuracy of core-needle breast biopsies generally has been low. The majority are retrospective chart reviews rather than prospective studies. Most provide poor details about the patient populations. The size, location, or imaging characteristics of a lesion may influence the choice of one breast biopsy technique over another. However, research studies have not included sufficient information about these characteristics to determine their impact on biopsy accuracy.
Although the quality of the evidence base is low, the studies have found that the clinical technique used to perform a core-needle breast biopsy does influence the sensitivity of the procedure (see Table 1). The freehand technique has substantially lower sensitivity than biopsies using either stereotactic radiography or ultrasound for guidance. Vacuum assistance provides a small additional increase in sensitivity. Evidence is insufficient to determine the accuracy of MRI-guided core-needle biopsies.
| Method | Automated Gun Core-Needle Biopsy | Vacuum-Assisted Core-Needle Biopsy | |||
|---|---|---|---|---|---|
| Freehand | Ultrasound-guided | Stereotactic-guided | Ultrasound-guided | Stereotactic-guided | |
| Sensitivity | 86% | 98% | 98% | 97% | 99% |
| Level of Confidence |
|||||
Are there false positive biopsies?
All open surgical biopsy specimens read as invasive breast cancer are considered true positive readings. In clinical practice, false positives are not considered to occur with core-needle biopsies. This is because a true breast cancer may have been small and completely removed by the core needle biopsy.
Misclassification of Biopsy Results
Some biopsies are read as noninvasive neoplastic lesions. These neoplastic lesions include lobular carcinoma in situ (LCIS), atypical lobular hyperplasia (ALH), ductal carcinoma in situ (DCIS), and atypical ductal hyperplasia (ADH). Core-needle breast biopsies may miss areas of invasive cancer in specimens in which the lesion is predominantly noninvasive.
The rates of invasive cancer reported in research studies support the widespread clinical practice of performing open surgical biopsy on all women whose core-needle biopsy is read as DCIS or ADH.
- About 13-36 percent of core-needle breast biopsy specimens diagnosed as DCIS will be found to have invasive breast cancer on subsequent surgical biopsy.
Level of Confidence: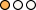
- About 22-44 percent of core-needle breast biopsy specimens diagnosed as ADH will be found to have in situ or invasive breast cancer on subsequent surgical biopsy.
Level of Confidence: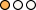
- The studies did not report misclassification rates for ALH or LCIS.
Complications and Pain
Clinically significant complications occur in a minority of women who undergo open surgical biopsies. The rate of hematomas is 2-10 percent, and the rate of infections is 4-6 percent. The rate of any complication is substantially lower with core-needle biopsies.
- Core-needle breast biopsies have a lower risk of hematomas and infection (less than 1 percent) than open surgical biopsies.
Level of Confidence:
- Vacuum-assisted core-needle breast biopsy procedures are associated with slightly more severe bleeding events than biopsies performed with an automated gun device.
Level of Confidence: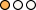
There is generally a low level of pain following a core-needle biopsy procedure. Less than 1 percent of women who have undergone a core-needle breast biopsy use narcotic pain medications following the procedure.
Resource for Patients
Having a Breast Biopsy: A Guide for Women and Their Families is a companion to this clinician guide. It can help women talk with their health care professional about breast biopsy options. It provides information about:
- Core-needle and open surgical biopsies.
- Accuracy of breast biopsies.
- Discomfort and complications of the procedure.
For More Information
For electronic copies of the consumer guide, this clinician guide, and the full systematic review, visit this Web site: www.effectivehealthcare.ahrq.gov
For free print copies, call:
The AHRQ Publications Clearinghouse
(800) 358-9295
Consumer’s Guide, AHRQ Pub. No. 10-EHC007-A
Clinician’s Guide, AHRQ Pub. No. 10-EHC007-3
AHRQ created the John M. Eisenberg Center at Oregon Health & Science University to make research useful for decisionmakers. This guide was written by David Hickman, M.D., Erin Davis, B.A., Seth Meyer, M.A., and Martha Schechtel, R.N., of the Eisenberg Center.
Source
The source material for this guide is a systematic review of 107 research studies. The review, Comparative Effectiveness of Core-Needle and Open Surgical Biopsy for the Diagnosis of Breast Lesions (2009), was prepared by the ECRI Institute Evidence-based Practice Center. The Agency for Healthcare Research and Quality (AHRQ) funded the systematic review and this guide. The guide was developed using feedback from clinicians who reviewed preliminary drafts. The full systematic review is available at www.effectivehealthcare.ahrq.gov.
Return to Top of Page

 E-mail Updates
E-mail Updates
