
September 2011
Adult Smoking in the US
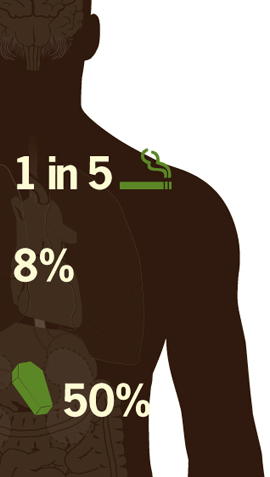
Tobacco use remains the single largest preventable cause of disease, disability, and death in the US. Some people who smoke every day are smoking fewer cigarettes; however, even occasional smoking causes harm. The percentage of American adults who smoke decreased from 20.9% in 2005 to 19.3% in 2010. That translates to 3 million fewer smokers than there would have been with no decline. But almost 1 in 5 adults still smoke. Reducing tobacco use is a winnable battle—a public health priority with known, effective actions for success. A combination of smoke-free laws, cigarette price increases, access to proven quitting treatments and services, and hard-hitting media campaigns reduces health care costs and saves lives.
Latest Findings
443,000 Americans die of smoking or exposure to secondhand smoke each year.
Millions of people still smoke.
- For every smoking-related death, another 20 people suffer with a smoking-related disease.
- In 2010, 19.3% of adults (or 45.3 million) smoked cigarettes, compared with 20.9% of adults in 2005.
- Smoking costs the US about $96 billion each year in direct medical costs and $97 billion from productivity losses due to premature death.
There is no safe level of smoking.
- Each cigarette you smoke damages your lungs, your blood vessels, and cells throughout your body.
- Even occasional smoking is harmful, and the best option for any smoker is to quit completely.
- The more years you smoke, the more you damage your body. Quitting at any age has benefits.
- A majority of Americans who have ever smoked have already quit; you can too.
Why is it so hard to quit smoking?
- Nicotine is a highly addictive drug. Addiction keeps people smoking even when they want to quit.
- Cigarettes deliver more nicotine more quickly now than ever before.
- The tobacco industry spends about $9.94 billion each year, or $27 million every day, on cigarette advertising and promotion—72% of these dollars are spent on discounts to offset tobacco taxation and other tobacco control policies.
What's the most effective way to quit smoking?
- Different ways work for different people. Many smokers have to try multiple times before they're able to quit for good. It is important to keep trying until you succeed; each time you learn something that will help you quit for good.
- While you're trying to quit, nicotine and non-nicotine containing medications can help lessen the urge to smoke. Talk to your health care provider for help.
- Individual, group, or telephone counseling can double your likelihood of success. A combination of medication and counseling is more effective than medication or counseling alone.
- Smokers can receive free resources and assistance to help them quit by calling 1-800-QUIT-NOW (1-800-784-8669) or visiting www.smokefree.gov.
The more states invest in comprehensive tobacco control programs, the greater the reductions in smoking—and the longer they invest, the greater and faster the impact.
- California's adult smoking rate has dropped nearly 50% and the number of cigarettes smoked per person has decreased by 67% since the state began the nation's longest-running tobacco control program in 1988.
- California saved $86 billion in health care costs by spending $1.8 billion on tobacco control, a 50:1 return on investment over its first 15 years of funding its tobacco control program.
Who's At Risk?
US Adult Smoking Statistics
SOURCE: National Health Interview Survey, 2010
Percent of adults who smoke by sex

Percent of adults who smoke by poverty level

Percent of adults who smoke by racial/ethnic group

Percent of adults who smoke by education level

Education estimates are among individuals ≥ 25 years of age.
U.S. State Info
Adult Smoking Prevalence by State

SOURCE: Behavioral Risk Factor Surveillance System, 2010
What Can Be Done
Here's What Works
Tobacco users can:
- Quit. The sooner you quit, the sooner your body can begin to heal, and the less likely you are to get sick from tobacco use.
- Ask a health care provider for help quitting and call 1-800-QUIT-NOW for free assistance.
- Find a step-by-step quit guide at www.smokefree.gov.
State and community leaders can:
- Fund comprehensive tobacco control programs at CDC-recommended levels.
- Enact 100% smoke-free indoor air policies that include workplaces, restaurants, and bars.
- Increase the price of all tobacco products.
- Implement hard-hitting media campaigns that raise public awareness of the dangers of tobacco use and secondhand smoke exposure.
- Use the World Health Organization's (WHO's)
MPOWER strategies to prevent and reduce tobacco use and to make tobacco products less accessible, affordable, attractive, and accepted.
M=Monitor tobacco use and prevention policies
P=Protect people from tobacco smoke
O=Offer help to quit
W=Warn about the dangers of tobacco use
E=Enforce restrictions on tobacco advertising
R= Raise taxes on tobacco
Parents and nonsmokers can:
- Make your home and vehicles smoke-free.
- Not start, if you aren't already using tobacco.
- Quit if you smoke; children of parents who smoke are twice as likely to become smokers.
- Teach children about the health risks of smoking and secondhand smoke.
- Encourage friends, family, and coworkers to quit.
Health care providers can:
- Ask their patients if they use tobacco; if they do, help them quit.
- Refer patients interested in quitting to 1-800-QUIT-NOW, www.smokefree.gov, or other resources.
- Advise all patients to make their homes and vehicles 100% smoke-free.
- Advise nonsmokers to avoid secondhand smoke exposure.
Employers can:
- Establish a policy banning the use of any tobacco product indoors or outdoors on company property by anyone at any time.
- Provide all employees and their dependents with health insurance that covers support for quitting with little or no co-payment.
Retailers can:
- Learn the new Food and Drug Administration (FDA) restrictions on youth access to tobacco products and tobacco marketing to youth, and closely follow them.
- Never sell any tobacco product to customers younger than 18 years of age (or 19 in states with a higher minimum age requirement).
- Check the photo ID of any customer trying to buy tobacco products who appears to be 26 years of age or younger.
Contact Us:
- Centers for Disease Control and Prevention
1600 Clifton Rd
Atlanta, GA 30333 - 800-CDC-INFO
(800-232-4636)
TTY: (888) 232-6348 - cdcinfo@cdc.gov




