|
In the United States, the HIV/AIDS epidemic is a health crisis for African
Americans. At all stages of HIV/AIDS—from infection with HIV to death with
AIDS—blacks (including African Americans) are disproportionately affected
compared with members of other races and ethnicities [1,
2].
STATISTICS
HIV/AIDS in 2005
- According to the 2000 census, blacks make up approximately 13% of the US population. However, in 2005, blacks accounted for 18,121 (49%) of the estimated
37,331 new HIV/AIDS diagnoses in the United States in the 33 states with long-term, confidential name-based HIV reporting [2].*
- Of all black men living with HIV/AIDS, the primary transmission category
was sexual contact with other men, followed by injection drug use and
high-risk heterosexual contact [2].
- Of all black women living with HIV/AIDS, the primary transmission
category was high-risk heterosexual contact, followed by injection drug use [2].
- Of the estimated 141 infants perinatally infected with HIV, 91 (65%)
were black (CDC, HIV/AIDS Reporting System, unpublished data, December
2006).
- Of the estimated 18,849 people
under the age of 25 whose diagnosis of HIV/AIDS was made during 2001–2004 in
the 33 states with HIV reporting, 11,554 (61%) were black [3].
*See the
box (before the References section) labeled Understanding HIV and AIDS Data for a list of the 33 states.
Race/ethnicity of persons (including
children) with HIV/AIDS diagnosed
during 2005 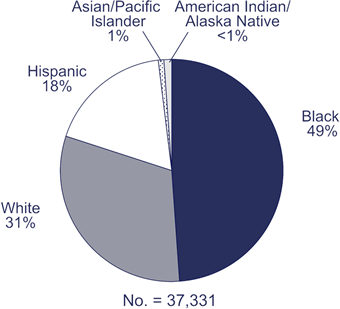
Note. Based on data from 33 states with long-term, confidential name-based HIV reporting.
Transmission categories for black adults and adolescents living with HIV/AIDS at the end of 2005

Note. Based on data from 33 states with long-term, confidential name-based HIV reporting.
AIDS in 2005
- Blacks accounted for 20,187 (50%) of
the estimated 40,608 AIDS cases
diagnosed in the 50 states and the
District of Columbia [2].
- The rate of AIDS diagnoses for black
adults and adolescents was 10 times the rate
for whites and nearly 3 times the rate for
Hispanics. The rate of AIDS diagnoses for
black women was nearly 23 times the rate for
white women. The rate of AIDS diagnoses for
black men was 8 times the rate for white men [2].
- The 185,988 blacks living with AIDS
in the 50 states and the District of
Columbia accounted for 44% of the
421,873 people in those areas living
with AIDS [2].
- Of the 68 US children (younger than 13
years of age) who had a new AIDS diagnosis,
46 were black [2].
- Since the beginning of the epidemic,
blacks have accounted for 397,548 (42%)
of the estimated 952,629 AIDS cases
diagnosed in the 50 states and the
District of Columbia [2].
- From the beginning of the epidemic
through December 2005, an estimated 211,559
blacks with AIDS died [2].
- Of persons whose diagnosis of AIDS had
been made during 1997–2004, a smaller
proportion of blacks (66%) were alive after
9 years compared with American Indians and
Alaska Natives (67%), Hispanics (74%),
whites (75%), and Asians and Pacific
Islanders (81%) [2].
Race/ethnicity of adults and adolescents living with HIV/AIDS, 2005
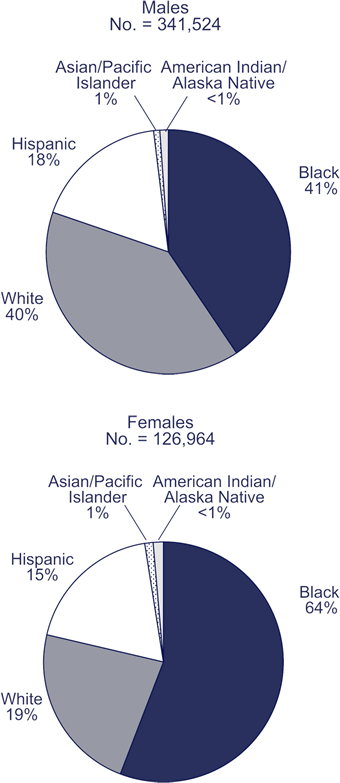
Note. Based on data from 33 states with long-term, confidential name-based HIV reporting.
RISK FACTORS AND BARRIERS TO PREVENTION
Race and ethnicity, by themselves, are not risk factors for HIV infection. Even
though HIV testing rates are higher for blacks than for members of other races
and ethnicities [4], rates of undetected or late
diagnosis of HIV infection are high for black men who have sex with men (MSM) [5].
Blacks are also more likely to face challenges associated with risk factors for
HIV infection, including the following.
Sexual Risk Factors
Black women are most likely to be infected with HIV as a result of sex with men
who are infected with HIV [2]. They may not be
aware of their male partners’ possible risk factors for HIV infection, such as
unprotected sex with multiple partners, bisexuality, or injection drug use [6,
7]. Sexual contact is also the main risk factor
for black men. Male-to-male sexual contact was the primary risk factor for 48%
of black men with HIV/AIDS at the end of 2005, and high-risk heterosexual
contact was the primary risk factor for 22% [2].
Substance Use
Injection drug use is the second leading cause of HIV infection both for black
men and women [2]. In addition to being at risk
from sharing needles, casual and chronic substance users are more likely to
engage in high-risk behaviors, such as unprotected sex, when they are under the
influence of drugs or alcohol [8]. Drug use can
also affect treatment success. A recent study of HIV-infected women found that
women who used drugs, compared with women who did not, were less likely to take
their antiretroviral medicines exactly as prescribed [9].
Lack of Awareness of HIV Serostatus
Not knowing one’s HIV serostatus is risky for black men and women. In a recent
study of MSM in 5 cities participating in CDC’s National HIV Behavioral
Surveillance System, 46% of the black MSM were HIV-positive, compared with 21%
of the white MSM and 17% of the Hispanic MSM. The study also showed that of
participating black MSM who tested positive for HIV, 67% were unaware of their
infection; of participating Hispanic MSM who tested positive for HIV, 48% were
unaware of their infection; of participating white MSM who tested positive for
HIV, 18% were unaware of their infection; and of participating multiracial/other
MSM who tested positive for HIV, 50% were unaware of their infection [10].
Persons who are infected with HIV but don’t know it cannot benefit from
life-saving therapies or protect their partners from becoming infected with HIV.
Sexually Transmitted Diseases
The highest rates of sexually transmitted diseases (STDs) are those for blacks.
In 2005, blacks were about 18 times as likely as whites to have gonorrhea and
about 5 times as likely to have syphilis [11].
Partly because of physical changes caused by STDs, including genital lesions
that can serve as an entry point for HIV, the presence of certain STDs can
increase one’s chances of contracting HIV infection 3- to 5-fold. Similarly, a
person who has both HIV infection and certain STDs has a greater chance of
spreading HIV to others [12]. A recent CDC
literature review showed that high rates of HIV infection for black MSM may be
partly attributable to a high prevalence of STDs that facilitate HIV
transmission [5].
Homophobia and Concealment of Homosexual Behavior
Homophobia and stigma can cause some black MSM to identify themselves as
heterosexual or not to disclose their sexual orientation [13,
14]. Indeed, black MSM are more likely than
other MSM not to identify themselves as gay [5].
The absence of self-identification or the absence of disclosure presents
challenges to prevention programs. However, data suggest that these men are not
at greater risk for HIV infection than are black MSM who identify themselves as
gay [14,
15]. The findings of these studies do not mean
that black MSM who do not identify themselves as gay or who do not disclose
their sexual orientation do not engage in risky behaviors, but the findings do
suggest that these men are not engaging in higher levels of risky behavior than
are other black MSM.
Socioeconomic Issues
Socioeconomic issues and other social and structural influences affect the rates
of HIV infection among blacks [16]. In 1999,
nearly 1 in 4 blacks were living in poverty [17].
Studies have found an association between higher AIDS incidence and lower income [18].
The socioeconomic problems associated with poverty, including limited access to
high-quality health care, housing, and HIV prevention education, may directly or
indirectly increase the risk factors for HIV infection.
PREVENTION
CDC estimates that
56,300 new HIV infections occurred in the United States in 2006 [19]. Populations of minority races and ethnicities are
disproportionately affected by the HIV epidemic. To reduce further the incidence
of HIV, CDC announced the
Advancing HIV Prevention (AHP)
initiative in 2003. This initiative comprises 4 strategies: making HIV testing a
routine part of medical care, implementing new models for diagnosing HIV
infections outside medical settings, preventing new infections by working with
HIV-infected persons and their partners, and further decreasing perinatal HIV
transmission.
CDC has also established the African American HIV/AIDS Work Group to focus on
the urgent issue of HIV/AIDS in African Americans. The work group developed a
comprehensive response to guide CDC’s efforts to increase and strengthen
HIV/AIDS prevention and intervention activities directed toward African
Americans. Already, CDC is engaged in a wide range of activities to involve
community leaders in the African American community and to decrease the
incidence of HIV/AIDS in blacks.
For example, CDC
- Funds demonstration projects
evaluating rapid HIV testing in
historically black colleges and
universities as well as projects to
improve the effectiveness of HIV testing
among black women and MSM.
- Conducts epidemiologic research focused on
blacks, including
- Brothers y Hermanos, a study of black and Latino MSM conducted in Los Angeles, New York, and Philadelphia that aims to identify and understand risk-promoting and risk-reducing sexual behaviors.
- Women’s Study, a study of black and Hispanic women in the southeastern United States that examines relationship dynamics, and
the cultural, psychosocial, and behavior factors associated with HIV infection.
- Addresses, through the
Minority AIDS Initiative, the health disparities experienced in the communities of minority races and ethnicities at high risk for HIV infection. Funds are used to address the high-priority HIV prevention needs in such communities, including funding community-based organizations (CBOs) to provide services to African Americans. Examples of the programs that CBOs carry out are
- A program in Washington, DC, that provides information to, and conducts HIV prevention activities for, MSM who do not identify themselves as homosexual. The activities include a telephone help line; Internet resources; and a program in barbershops that includes risk-reduction workshops, condom distribution, and training barbers to be peer educators.
- A program in Chicago that provides social support to help difficult-to-reach African American men reduce high-risk behaviors. This program also provides women at high risk for HIV infection with culturally appropriate, gender-specific prevention and risk-reduction messages.
- A program in South Carolina that is focused on changing the behaviors of adolescents to reduce their risk of contracting HIV infection and other STDs.
- Creates social marketing
campaigns, including those focused
on HIV testing, perinatal HIV
transmission, and the reduction of
HIV transmission to partners.
- Disseminates scientifically based interventions, including
- SISTA (Sisters Informing Sisters
About Topics on AIDS), a
social-skills training intervention
in which peer facilitators help African American women at highest risk reduce their risky sexual behaviors.
- Many Men, Many Voices (3MV), an STD/HIV prevention intervention for gay men of color that addresses cultural and social norms, sexual relationship dynamics, and the social influences of racism and homophobia.
- POL (Popular Opinion Leader), which identifies, enlists, and trains key opinion leaders to encourage safer sexual norms and behaviors within their social networks. POL has been adapted for African American MSM and shown to be effective in that population.
- Healthy Relationships, a small-group intervention for men and women living with HIV/AIDS.
- WILLOW (Women Involved in Life Learning from Other Women), to be disseminated in 2007, is a small-group, skills-training intervention for women living with HIV.
WILLOW enhances awareness of the risky behaviors associated with HIV transmission, discredits myths regarding HIV prevention for people living with HIV, teaches communication skills in negotiating safer sex, and reinforces the benefits of consistent condom use. WILLOW also teaches women how to recognize healthy and unhealthy relationships, discusses the effect of abusive partners on safer sex, and provides information about local shelters for women in abusive relationships.
CDC also supports research to create new
interventions for African Americans and to
test interventions that have proven
successful with other populations for use
with African Americans. Additionally, CDC
funds agencies through ADAPT (Adopting and
Demonstrating the Adaptation of Prevention
Techniques) to adapt and evaluate effective
interventions for use in communities of
color.
In addition, CDC
- Provides intramural training for researchers
who are members of minority races and ethnicities through a program called Research Fellowships on HIV Prevention in Communities of Color.
- Established the extramural Minority HIV/AIDS Research Initiative (MARI) in 2002 to create partnerships between CDC epidemiologists and researchers who are members of minority races and ethnicities and who work in communities of color. MARI funds epidemiologic and preventive studies of HIV in communities of color and encourages the career development of young investigators. CDC invests $2 million per year in the program and since 2003 has funded 13 junior investigators at 12 sites across the country [20].
Understanding HIV and AIDS Data
AIDS
surveillance: Through a uniform system, CDC receives
reports of AIDS cases from all US states and territories. Since the
beginning of the epidemic, these data have been used to monitor trends
because they are representative of all areas. The data are statistically
adjusted for reporting delays and for the redistribution of cases
initially reported without risk factors. As treatment has become more
available, trends in new AIDS diagnoses no longer accurately represent
trends in new HIV infections; these data now represent persons who are
tested late in the course of HIV infection, who have limited access to
care, or in whom treatment has failed.
HIV surveillance: Monitoring trends in the HIV
epidemic today requires collecting information on HIV cases that have
not progressed to AIDS. Areas with confidential name-based HIV infection
reporting requirements use the same uniform system for data collection
on HIV cases as for AIDS cases. A total of 33 states (Alabama, Alaska,
Arizona, Arkansas, Colorado, Florida, Idaho, Indiana, Iowa, Kansas,
Louisiana, Michigan, Minnesota, Mississippi, Missouri, Nebraska, Nevada,
New Jersey, New Mexico, New York, North Carolina, North Dakota, Ohio,
Oklahoma, South Carolina, South Dakota, Tennessee, Texas, Utah,
Virginia, West Virginia, Wisconsin, and Wyoming) have collected these
data for at least 5 years, providing sufficient data to monitor HIV
trends and to estimate risk behaviors for HIV infection.
HIV/AIDS: This term is used to refer to 3
categories of diagnoses collectively: (1) a diagnosis of HIV infection
(not AIDS), (2) a diagnosis of HIV infection and a later diagnosis of
AIDS, and (3) concurrent diagnoses of HIV infection and AIDS. |
REFERENCES
- LCWK2.
Deaths, percent of total deaths, and death rates for the 15 leading causes of death in 10-year age groups, by race and sex: United States, 2003.
 Accessed January 29, 2007. Accessed January 29, 2007.
- CDC.
HIV/AIDS Surveillance Report, 2005. Vol. 17.
Rev ed. Atlanta: US Department of Health
and Human Services, CDC: 2007:1–46. Accessed June 28, 2007.
- CDC.
Racial/ethnic
disparities in diagnoses of HIV/AIDS—33
states, 2001–2004.
MMWR 2006;55:121–125.
- Anderson JE, Chandra A, Mosher WD.
HIV Testing in the United States, 2002. Hyattsville, Md: National Center for Health Statistics; 2005:1–32. Advance Data from Vital and Health Statistics, No. 363.
- Millett GA, Peterson JL, Wolitski, RJ, Stall R. Greater risk for HIV infection of black men who have sex with men: a critical literature review.
American Journal of Public Health 2006;96:1007–1019.
- Hader SL, Smith DK, Moore JS, Holmberg SD. HIV infection in women in the United States: status at the millennium.
JAMA 2001;285:1186–1192.
- Millett G, Malebranche D, Mason B, Spikes P. Focusing “down low”: bisexual black men, HIV risk and heterosexual transmission.
Journal of the National Medical Association 2005;97:52S–59S.
- Leigh BC, Stall R. Substance use and risky sexual behavior for exposure to HIV: issues in methodology, interpretation, and prevention.
American Psychologist 1993;48:1035–1045.
- Sharpe TT, Lee LM, Nakashima AK, Elam-Evans LD, Fleming P. Crack cocaine use and adherence to antiretroviral treatment among HIV-infected black women.
Journal of Community Health 2004;29:117–127.
- CDC.
HIV
prevalence, unrecognized infection, and HIV
testing among men who have sex with men—five U.S.
cities, June 2004–April 2005.
MMWR 2005;54:597–601.
- CDC.
Sexually Transmitted Disease Surveillance, 2005.
Atlanta: US Department of Health and
Human Services, CDC; November 2006. Accessed January 28, 2007.
- Fleming DT, Wasserheit JN. From epidemiological synergy to public health policy and practice: the contribution of other sexually transmitted diseases to sexual transmission of HIV infection.
Sexually Transmitted Infections 1999;75:3–17.
- CDC.
HIV/AIDS
among racial/ethnic minority men who have
sex with men—United States, 1989–1998.
MMWR 2000;49:4–11.
- CDC.
HIV/STD
risks in young men who have sex with men
who do not disclose their sexual orientation—six U.S.
cities, 1994–2000 .
MMWR 2003;52:81–85.
- Hart T, Peterson J. Predictors of risky sexual behavior among young African American men who have sex with men.
American Journal of Public Health
2004;94:1122–1123.
- National Minority AIDS Council. African Americans, health disparities and HIV/AIDS: recommendations for
confronting the epidemic in black America.
 November 2006. Accessed January 28, 2007.
November 2006. Accessed January 28, 2007.
- US Census Bureau. Poverty: 1999. Census 2000 Brief.
 May 2003. Accessed January 28, 2007. May 2003. Accessed January 28, 2007.
- Diaz T, Chu SY, Buehler JW, et al. Socioeconomic differences among people with AIDS: results from a multistate surveillance project.
American Journal of Preventive Medicine 1994;10:217–222.
- Hall HI, Ruiguang S, Rhodes P, et al. Estimation of HIV incidence in the United States.
JAMA. 2008;300:520-529.
- Trubo R. CDC initiative targets HIV research gaps in black and Hispanic communities.
JAMA 2004;292: 2563–2564.
|