|
|
|
|
|
|
|
In 1996 and 1998 Congress amended the Employee Retirement Income Security
Act (ERISA) with new provisions governing health care benefits. This
presented a new challenge for the Department of Labor’s Pension and
Welfare Benefits Administration (EBSA), which is charged with administration
of ERISA. To implement these health care provisions and to provide
broad-based compliance assistance to the regulated community, EBSA developed
comprehensive interpretive guidance at the earliest stages of
implementation. In addition, EBSA did extensive compliance assistance
outreach to group health plan sponsors, health insurance issuers, and other
affected parties.
|
 |
On
This Page |
 |
|
|
|
|
In fiscal years (FY)(1)
1997 and 1998, EBSA published regulations implementing the health care
provisions, initiated an education outreach campaign, and developed
compliance assistance publications.
|
|
Compliance assistance outreach continued through FY
1999 with the development of a pilot program, under which more than 200
health plans were reviewed for compliance with the new health care
provisions. In FY 2000, EBSA assessed the results of the pilot
program and made adjustments to expand its existing outreach and
compliance assistance efforts, as well as to develop internal quality
control for completing health plan reviews. Then, in FY 2001, EBSA
undertook its Health Disclosure and Claims Issues (HDCI) FY 2001
Compliance project (project), during which the Agency reviewed a large
number of plans to assess the level of compliance with the new health care
provisions. It was anticipated that this project would give the Agency a
baseline for assessing compliance on a specific provision-by-provision
basis.
|
|
The project was undertaken very early in the
implementation period of the new health care laws; compliance reviews were
begun only 2 years after the new health laws became applicable. However,
early reviews were important to enable the plan community and the Agency
to identify areas of misunderstanding and to enable the Agency to focus
its efforts on clarifying those requirements. Specifically, based on the
results of the project (which are presented in detail in this report),
EBSA is announcing its HIPAA Compliance Assistance Program (H-CAP), which
is comprised of three strategies, each with an action plan. After
identifying problem areas through the project and introducing H-CAP to
target these problems, EBSA anticipates that compliance rates will rise.
|
|
H-CAP’s first strategy is to develop and distribute
additional publications and other educational materials. EBSA is
publishing three new publications to assist group health plans and health
insurance issuers in complying with the new health laws. These materials
will be distributed through the Agency’s toll-free publications line, at
all workshops and compliance assistance activities, through industry
groups and industry newsletters, through the trade press and other
interested media, and via the Agency’s Web site.
|
|
The first is a Self-Audit Checklist. This checklist,
similar to the HIPAA checksheet used by EBSA investigators to determine
compliance, will be a useful tool for plans and issuers to assess their
compliance line-by-line with the health laws. In addition, Compliance
Assistance for Group Health Plans, EBSA’s current publication
highlighting the top 10 most common errors made by health plans, has been
updated with 5 additional tips for group health plans, based on common
mistakes found in the project. It also includes advice on how to avoid
these mistakes. Finally, a New Health Laws Notice Guide has been developed
summarizing all of the new health law notice requirements, including
sample language that can be used by plans.
|
|
H-CAP’s second strategy is to dedicate a section of
the compliance assistance page on EBSA’s Web site to the new health care
laws, making it easier for plans, issuers, and other service providers to
find, in one location, all of the regulations, publications, frequently
asked questions, and other guidance. The new, dedicated section will
supplement compliance assistance efforts EBSA has already made, including
making its benefits advisors available through EBSA's Toll-Free Employee
& Employer Hotline number, 1.866.444.3272, and electronically at
www.askpwba.dol.gov to answer questions about the new health law
requirements.
|
|
The third strategy will be to participate in new, live
workshops around the country where trained staff will meet with plan
administrators, plan sponsors, attorneys, consultants, and other service
providers to apply the Self-Audit Checklist to various sample plan
provisions and documents. These live workshops will supplement the Health
Benefits Education Campaign Compliance Assistance Seminars already
conducted by the Agency, which address a wider variety of health plan
topics, including the new health laws.
|
|

|
|
|
|
In October 2000, EBSA initiated the project, during
which 1,267 investigations were conducted of group health plans and their
compliance with the new health care laws in Part 7 of Title I of ERISA.
The new health laws are the Health Insurance Portability and
Accountability Act of 1996 (HIPAA), the Mental Health Parity Act of 1996 (MHPA),
the Newborns’ and Mothers’ Health Protection Act of 1996 (Newborns’
Act), and the Women’s Health and Cancer Rights Act of 1998 (WHCRA). Each
law provides new Federal protections to individuals in employment-based
group health plans.
|
|
Because these laws generally became effective only
about 2 years before the project began, implementation by group health
plans seems to have progressed steadily. Most group health plans made
changes to comply with the new health care laws. However, some plans
experienced start-up, implementation issues, particularly with respect to
certain notice provisions and certain discrete substantive provisions that
are technical in nature. In such cases, correction of these problems was
obtained through voluntary compliance by the plans and their service
providers.
|
|
The FY 2001 Compliance project was a review of group
health plans for compliance with 42 specific requirements of the new laws.
Generally, EBSA found that group health plans are in compliance with the
substantive provisions of the new health care laws—that is, the
provisions other than the notice requirements. However, implementation
problems exist, particularly with respect to certain notice provisions, as
well as regarding certain discrete substantive provisions that are
technical in nature. To address these problems, EBSA has developed the
HIPAA Compliance Assistance Program (H-CAP). H-CAP, which is discussed in
more detail below, should improve compliance by partnering with the
regulated community to address problem areas identified in the project.
|
|
Data from the project revealed that only 8 percent of
plans were cited with a violation of MHPA.(2)
This rate shows a sustained improvement from the 14 percent noncompliance
rate found by the General Accounting Office (GAO) using survey data
reported as of December 1999. (See Mental Health Parity Act: Despite New
Federal Standards, Mental Health Benefits Remain Limited (GAO/HEHS-00-95,
May 10, 2000.)
|
|
With respect to WHCRA, only 4.5 percent of plans were
cited with a violation of WHCRA’s substantive provisions (that is, the
provisions other than the notice requirements). This number increased,
however, when taking into account WHCRA’s notice requirements; the
investigations resulted in 21.8 percent of plans being cited with a
violation of WHCRA. Some of the WHCRA violations may have resulted from a
lack of formal guidance or a communication gap with health insurance
issuers about the required elements and timing for notices.
|
|
Similarly, regarding the Newborns’ Act, only 5.2
percent of plans were cited with a violation of the substantive
provisions. Again, the number increased, however, when taking into account
the notice requirements; 35.0 percent of plans were cited with a
violation. In this regard, there may have been some confusion among plan
administrators and health insurance issuers regarding the applicability of
the Newborns’ Act notice requirements, which may account for the high
rate of noncompliance.
|
|
Data from the project also revealed that 28.1 percent
of plans were cited with at least one violation of HIPAA’s substantive
portability (including the certificate of creditable coverage
requirements) or nondiscrimination provisions. Many of the violations
involved discrete plan provisions, such as “hidden” preexisting
condition exclusions or non-confinement clauses. In these instances, EBSA
found that one plan provision caused multiple HIPAA violations. Moreover,
notice problems played a role again; 35.9 percent of plans in the sample
were cited with at least one violation of HIPAA when taking into account
the notice provisions.
|
|
After reviewing all of the data, EBSA also observed
certain trends. Plans were reviewed for compliance with 42 health care
provisions, 6 of which were notice provisions. Most of the violations
cited involved these notice requirements. In addition, small and large
single-employer plans had the lowest noncompliance rates (as opposed to
mid-sized, single-employer plans). Among multiemployer plans, violation
rates, which were generally higher than among single-employer plans, also
peaked in the mid-sized range.
|
|
Combining the data, 30.7 percent of plans were not in
compliance with at least one of the 36 substantive provisions of the four
health care laws. After factoring in noncompliance rates with the six
notice provisions, the data reveal that 45.3 percent of group health plans
were cited with a violation of at least one provision of the four laws. In
many cases, noncompliance may have been the result of a mistake in
understanding and complying with the laws. Given the fact that the project
was initiated in the very early stages of the laws’ implementation
process, and taking into account the size of the ERISA health plan
universe (approximately 2.5 million plans), this confusion in
implementation is not unexpected. To address these implementation issues,
EBSA is initiating H-CAP to launch a partnership effort with the regulated
community to provide targeted compliance assistance and to rapidly improve
compliance rates.
|
|

|
|
|
|
Because, traditionally, Federal law did not regulate the provision of
specific health benefits, the enactment of these new health care laws presented
a challenge for EBSA. As mentioned earlier, before it undertook the broader FY
2001 Compliance project, EBSA launched a 1999 pilot project. This pilot project
involved the review of approximately 225 group health plans to determine initial
levels of compliance with these newly enacted laws. The Office of Enforcement (OE)
and investigators from regional offices worked with group health plans, group
health insurance issuers (issuers),(3) and other service providers regarding their
responsibilities under the new health care provisions. To assist investigators
with their reviews of plans and to establish uniform standards for review, the
Office of Health Plan Standards and Compliance Assistance (OHPSCA) developed a
HIPAA checksheet. This checksheet summarized the various requirements of each
law line by line and established standardized questions for group health plan
reviews. An updated, self-audit version of this checksheet is being made
publicly available simultaneously with the publication of this report.
|
|
The FY 1999 pilot project succeeded in introducing investigators to Part 7
compliance work and informed EBSA as to what additional measures would be needed
before investigations could be conducted by regional investigators on a broader
scale. Accordingly, in FY 2000, EBSA expanded its internal education program and
developed a variety of quality control measures to make health plan
investigations more efficient and effective. These efforts included making new
use of technology to develop printed and electronic materials as well as new,
faster methods of communication, as described below. Also in FY 2000, and
drawing from its growing experience with health plan investigations, EBSA
implemented HDCI, a national project reflecting the Agency’s increased
commitment to reviewing health plans. Later, in March 2000, EBSA published its
Strategic Enforcement Plan that identified health plan issues as one of the
Agency’s national priorities. EBSA’s primary focus in this area is to ensure
that health plans with trusts are financially sound and plan operators run the
health plan prudently and in the participants’ sole interests. Regional
offices were directed to perform a detailed Part 7 review in cases opened under
the project.
|
|
Although historically EBSA had a presence in civil and criminal health care
enforcement, prior efforts targeted issues such as delinquent participant
contributions to health plans, fraudulent multiple employer welfare
arrangements, and the failure to transmit to plans fee reductions and discounts
received from doctors and hospitals negotiated by administrative service
providers. HDCI represented a major shift in emphasis in enforcing all the
provisions of ERISA affecting group health plans, including Part 1 (relating to
reporting and disclosure), Part 4 (relating to fiduciary responsibility), Part 6
(relating to continuation health coverage under the Consolidated Omnibus Budget
Reconciliation Act of 1985 (COBRA)), and Part 7.
|
|
OE also recognized the need for specialized training for investigators and,
thus, prepared and presented to each region during its annual field training
session modules on the health care industry, health care contracts, health plan
criminal investigations, claims processing, remedies, and the COBRA health
coverage continuation provisions.
|
|
The project evolved as an outgrowth of HDCI and was designed specifically to
ascertain the level of compliance with the new Part 7 health care laws
throughout the employee health benefit plan universe. Data derived from the
project and presented in this report reflect, among other outcomes, a baseline
of overall compliance by group health plans with the Part 7 statutes and
regulations. The report includes an overview of the statutory and regulatory
provisions of Part 7; a discussion of regional office investigator training; an
explanation of the sampling methodology and field implementation of the project;
a presentation and interpretation of data; and a discussion of the impact the
investigations had on issuers and third-party administrators (TPAs).
|
|
The data presented in this report illustrate compliance with Part 7 overall
and with each of the individual laws that are the framework of Part 7.
Additionally, the data show violation rates by plan size (large or small) and
plan type (single or multiemployer). Analysis of these results assisted EBSA in
the development of H-CAP, and will influence how EBSA will implement additional,
future interpretive and compliance assistance activities.
|
|

|
|
|
|
Health Insurance Portability and Accountability Act of 1996
(HIPAA)
|
|
Legislative History
- HIPAA was enacted on August 21, 1996, to provide for, among other things,
improved portability and continuity of health care coverage.(4)
First, HIPAA
places limitations on a plan’s or issuer’s ability to impose a preexisting
condition exclusion. Specifically, a preexisting condition exclusion must relate
to a condition for which medical advice, diagnosis, care, or treatment was
recommended or received within the 6-month period ending on an individual’s
enrollment date. The exclusion period cannot extend for more than a maximum of
12 months (18 months for late enrollees) after the enrollment date, offset by
the days of an individual’s prior health coverage. The primary way that
individuals provide evidence of their prior health coverage is through a
certificate of creditable coverage provided to them by their prior health plan
or issuer when coverage ends. Accordingly, HIPAA also sets forth a process for
transmitting certificates and other health coverage information to a new group
health plan or issuer. In addition, HIPAA creates special enrollment rights,
which allow an individual to enroll in a group health plan for which he or she
is otherwise eligible when he or she loses eligibility for other health coverage
or has a new dependent. HIPAA also prohibits discrimination based on health
factors against individuals and their dependents in enrollment and premiums.
Finally, HIPAA preserves, through narrow preemption provisions, the States’
traditional role in regulating health insurance, including State flexibility to
provide greater protections.
|
|
Regulatory History
- After inviting comments from the regulated community and other interested
parties,(5) interim final regulations implementing HIPAA were published on April
8, 1997 (62 Fed. Reg. 16894). The regulations clarify the statutory provisions
and provide protections for individuals seeking health coverage while minimizing
burdens on plans and issuers. The regulations reduce burdens by providing model
language for HIPAA disclosures (including a model certificate of creditable
coverage), reducing unnecessary duplication in the issuance of certificates,
including flexible rules for dependents to receive the coverage information they
need, and allowing coverage information to be provided by telephone if all
parties agree. The regulations protect and assist participants and their
dependents by ensuring that individuals are notified of the length of time that
a preexisting condition exclusion clause in any new health plan may apply to
them after taking into account their prior creditable coverage, ensuring that
individuals are notified of their rights to special enrollment under a plan,
permitting individuals to obtain a certificate before coverage under a plan
ceases, and creating practical ways for individuals to demonstrate creditable
coverage to a new plan (if, for example, the individual does not receive a
certificate for the individual’s prior health coverage). Additional
regulations implementing HIPAA’s nondiscrimination provisions were published
on January 8, 2001 (66 Fed. Reg. 1378). The Departments of Labor, the Treasury,
and Health and Human Services (HHS) are presently drafting final rules on HIPAA’s
portability provisions. These rules will reflect further comments received from
interested parties representing the experience they have had with the interim
regulations.(6)
|
|
Effective Dates
- The HIPAA provisions first became applicable to group health plans and
issuers under two separate time lines. One was a general time line for the
majority of the provisions, which were generally effective for plan years
beginning on or after July 1, 1997, representing a staggered effective date for
the provisions. For collectively bargained plans, there is a special effective
date under HIPAA. For plans maintained pursuant to collective bargaining
agreements (CBAs) ratified before August 21, 1996, the majority of the
provisions apply to plan years beginning on the later of July 1, 1997, or the
date on which the last of the CBAs relating to the plan terminates (determined
without regard to any extension agreed to after August 21, 1996). The effective
date for HIPAA’s certification provisions for all group health plans and
health insurance issuers is July 1, 1996, to give individuals evidence of
creditable coverage prior to the July 1, 1997, effective date for the other
provisions.
|
|
The effective dates for the 1997 interim regulations regarding HIPAA’s
portability and nondiscrimination provisions mirror the statutory effective
dates. The 2001 regulations on HIPAA’s nondiscrimination provisions are
generally effective for plan years beginning on or after July 1, 2001, and
therefore were generally not considered when determining group health plan
compliance during the project.
|
|

|
|
Newborns’ and Mothers’ Health Protection Act of 1996 (Newborns’ Act)
|
|
Legislative History
- The Newborns’ Act was enacted on September 26, 1996.(7)
The law provides new
protection for mothers and their newborn children with regard to the length of
hospital stays following the birth of a child. Specifically, the Newborns’ Act
provides a general rule under which a group health plan and an issuer may not
restrict a mother’s or newborn’s benefits for a hospital stay in connection
with childbirth to less than 48 hours following a vaginal delivery or 96 hours
following a cesarean section. The Newborns’ Act permits an exception to the
48-hour (or 96-hour) general rule if the attending provider decides, in
consultation with the mother, to discharge the mother or her newborn earlier.
|
|
Regulatory History
- On October 27, 1998, the Departments of Labor, the Treasury, and HHS
published interim final regulations for group health plans and issuers under the
Newborns’ Act, after inviting comments from the regulated community and other
interested parties.(8) Among other things, the regulations clarify when the
48-hour (or 96-hour) period begins, provide that the determination as to whether
a hospital admission is in connection with childbirth is a medical decision to
be made by the attending provider, define who may be an attending provider, and
clarify the applicability of State law to insured arrangements.
|
|
Effective Dates
- The statutory provisions apply to group health plans and issuers for plan
years beginning on or after January 1, 1998. Clarifications contained in the
interim final rules apply for plan years beginning on or after January 1, 1999.
|
|

|
|
Mental Health Parity Act of 1996 (MHPA)
|
|
Legislative History
- MHPA was enacted on September 26, 1996.(9)
MHPA provides for parity in the
application of aggregate lifetime dollar limits, and annual dollar limits,
between mental health benefits and medical/surgical benefits. MHPA’s
requirements apply regardless of whether the mental health benefits are
administered separately under the plan. Nevertheless, MHPA does not require a
group health plan or health insurance coverage offered in connection with a
group health plan to provide mental health benefits.
|
|
Regulatory History
- The Departments of Labor, the Treasury, and HHS published interim final
regulations implementing the MHPA provisions on December 22, 1997, after
inviting comments from the regulated community and other interested parties.(10)
Among other things, the regulations clarify the application of the MHPA
provisions to group health plans with varying types of dollar limitations
(including inpatient/outpatient limits and in-network/out-of-network limits) and
the procedures a plan would undertake to elect the 1 percent increased cost
exception permitted under the statute.
|
|
Effective Date
- In general, MHPA and the interim final rules apply to group health plans and
issuers for plan years beginning on or after January 1, 1998.(11)
|
|

|
|
Women’s Health and Cancer Rights Act of 1998 (WHCRA)
|
|
Legislative History
- WHCRA was enacted on October 21, 1998.(12)
WHCRA requires group health plans
and issuers that offer medical and surgical benefits with respect to a
mastectomy to provide reconstructive breast surgery if a participant or
beneficiary is receiving benefits in connection with a mastectomy, elects
reconstruction, and the reconstruction is in connection with such mastectomy. In
particular, WHCRA requires coverage of the following reconstructive surgery
benefits: 1) all stages of reconstruction of the breast on which the mastectomy
was performed; 2) surgery and reconstruction of the other breast to produce a
symmetrical appearance; and 3) prostheses and physical complications of the
mastectomy, including lymphedemas.
|
|
The Departments published a Solicitation of Comments on issues arising under
WHCRA on May 28, 1999 (64 Fed. Reg. 29186). Question-and-answer guidance
(Q&As), including model language that may be used to satisfy WHCRA’s
disclosure requirements, was issued in May 1999 and updated in October 1999.
Additional guidance is currently under development.
|
|
Effective Date
- WHCRA applies to group health plans and issuers for plan years beginning on
or after October 21, 1998.
|
|

|
|
|
|
Collection and Coordination of Data
|
|
Identification of Plans to Review
- The project involved 1,267 investigations of large and small single-employer
group health plans and multiemployer plans. (See Table 1 and Chart 1.) The
Office of Policy and Research (OPR) prepared a Sample Design, which describes in
depth the sampling methodology. (See Appendix.) The project encompassed three
distinct samples: multiemployer, small single-employer (<100 employees), and
large single-employer (≥100 employees) plans. The multiemployer and
single-employer samples were selected from distinct data sources because no
central source identifies whether a given private-sector single employer offers
a group health plan covered by Title I of ERISA. However, EBSA already possessed
enough information from Annual Report Form 5500 filings to select the multiemployer
sample.
|
|
 The referrals to regional offices involved three distinct steps: (1) randomly
selecting a pool of entities suitable for investigation, (2) transmitting
referrals and opening cases, and (3) replacing entities found to be out-of-scope
with more entities. These steps were intended to preserve a minimum of 399 multiemployer
plans, 444 large-employer plans, and 448 small-employer plans. The referrals to regional offices involved three distinct steps: (1) randomly
selecting a pool of entities suitable for investigation, (2) transmitting
referrals and opening cases, and (3) replacing entities found to be out-of-scope
with more entities. These steps were intended to preserve a minimum of 399 multiemployer
plans, 444 large-employer plans, and 448 small-employer plans.
Referral of Multiemployer Plans
- The Office of Information Management had available certain data on multiemployer
plans, such as the plan sponsor and the plan administrator,
address and telephone number of both parties, total plan assets, and plan
sponsor’s Employer Identification Number (EIN). These plan data are derived
from Annual Report Form 5500 filings.
|
|
As an initial step, OPR provided OE with the basic information described
above for 398 multiemployer plans. OE referred these plans to EBSA regional
offices in August 2000 with instructions to open cases on or after October 1,
2000. Regional offices determined some plans to be out-of-scope or otherwise
ineligible for case opening. The most common reason was that the selected multiemployer
plan had merged with another plan, effectively terminating the
plan selected for investigation. Plans that were already under investigation or
had been investigated within the preceding 12 months were also withdrawn because ERISA
section 504(b) prohibits a EBSA investigation under these circumstances
absent “reasonable cause.” Plans offering only excepted benefits such as
certain dental and vision benefit plans, as defined in regulation 29 CFR § 2590.732(b), were also considered out-of-scope and were withdrawn
from the potential referrals.
|
|
Replacement of out-of-scope multiemployer plans occurred in two batches. OE
made the first set of replacements on March 30, 2001, and the second set was
disseminated on June 26, 2001. These replacements restored the number of
in-scope multiemployer plans to 409.
|
|
Referral of Single-Employer Plans - The task of assembling enough single-employer firms with group health plans
to maintain the goals of 444 (large firms) and 448 (small firms) was much more
complicated and resource intensive. EBSA obtained from Dun and Bradstreet (D
& B) basic information on 2,226 randomly selected large and small firms in
the 50 States and the District of Columbia. The information included the name of
the company, address, EIN, telephone number, number of employees, and whether
the company was a subsidiary. EBSA requested that certain known church or
government organizations be excluded from the records because Title I of ERISA
does not cover plans sponsored by such entities.(13)
OPR divided the large and
small samples by EBSA region and provided individual contact sheets for the
single employers. National office staff (primarily OE coordinators and OHPSCA
staff) then attempted to contact each firm directly by telephone to verify
coverage. In a few instances – particularly for large firms – staff could
verify through an Internet search that a firm offered a group health plan. When
staff determined that a firm was unreachable or out of scope, the next firm in
sequence was contacted so that each contact had a disposition. Staff entered
each disposition, along with other information gleaned from the contact, on the
standard contact sheet. OE then consolidated the dispositions on a master
spreadsheet. Once a sufficient number of referrals was amassed, they were
batched together by region and referred to regional offices on spreadsheets. The
spreadsheets (tracking files) were used throughout the project to match project
referrals with the corresponding cases in the Enforcement Management System
(EMS) in order to link with data on Part 7 violations. (See Table 10 for the
list of EMS codes used.) Ultimately, each of the firms and multiemployer plans
had a case number in the tracking file or a coded disposition (e.g.,
U-unreachable, C-church plan) entered on a master tracking file.
|
|
After OE made each set of referrals, regional coordinators typically
distributed the potential cases throughout their region. Regional managers
determined which investigators were assigned project investigations. The
regional coordinators reported back to the national coordinator when specific
referrals could not be investigated, for tracking and replacement purposes. The
regional coordinators also raised interpretive and procedural issues encountered
during the investigations.
|
|
OE made the initial assignment of 476 large-firm referrals to the field on
October 25, 2000. Along with the referrals, OE issued a guidance memorandum.
Among other items, the guidance provided a dedicated EMS National project code
to be used exclusively for these and subsequent project referrals. OE referred a
set of large-firm replacements on September 4, 2001. The entire allotment of
large-firm records selected by D & B was exhausted by this date.
|
|
OE made the initial batched referral of 151 small firms with plans on January
26, 2001. Staff attempting to contact companies had found many small firms
either did not offer a covered plan, or were unreachable.(14)
It was not possible
at that date to refer a greater number, because more time and resources were
needed to reach the target of 448 small firms with plans. By January 26, 2001,
485 contacts had identified 151 small firms with plans. The second batch of 310
referrals was made on March 27, 2001. Staff had contacted over 1,300 small firms
by this date. OE sent small-firm replacements to regional offices on November 1,
2001. By this date, staff had attempted to contact 1,604 small firms.
|
|
OE directed regional offices to enter Part 7 violations data in EMS by the
end of calendar year 2001. After January 1, 2002, OPR and OE verified the
accuracy of tracking files and EMS data fields. OPR then produced statistical
tables for comment and analysis.
|
|

|
|
Investigative Procedures
|
|
The project was part of the Program Operating Plan (POP) Guidance for 2001.
The POP Guidance instructed regional offices to use the HIPAA checksheet and
other compliance materials created by OHPSCA. The guidance also requested that
in these project cases regions should take the opportunity to undertake any
other reasonable investigative steps to ensure that no other problems exist in
the plan regarding claims payments, financial soundness, reporting, disclosure,
or fidelity bond issues.
|
|
To reinforce these points, the October 25, 2000, transmittal of the partial
large-firm sample included an “Investigative Guidance” section. This section
reiterated that the primary goal of the project was to gauge Part 7 compliance,
but it also stated the need to perform a sufficient review of compliance with
Parts 1, 4, and 6 of ERISA.
|
|
To increase efficiency, some regions developed standard opening letters for
multiemployer and single-employer plans. Generally, these document request
letters evolved from those used for general health plan investigations. Another
efficiency strategy was to group referrals by geographic location or by
third-party administrator.
|
|
Regions used the HIPAA checksheet in the project as a guide in
investigations. The checksheet also served as a training tool and as a means for
managers to monitor progress. Certain regions also created their own
investigative guides tailored to the project. For example, one region’s guide
prompted the investigator to address parent/subsidiary relationships, EMS
reporting requirements, and contact information.
|
|
Once the investigations were underway, investigators could draw from various
sources of expertise. Some regions held periodic meetings to discuss compliance
issues. Regional offices raised novel voluntary compliance issues with OE and
OHPSCA. OE presented a module on the project to all regional office staff during
its summer 2001 training. This module addressed technical and procedural issues
such as remedies, subpoenas, and coordination with State insurance commissions.
National office and regional managers continuously discussed the project in
routine conference calls and meetings. OE and OHPSCA also held several organized
teleconferences with all regional coordinators, in addition to informal
teleconferences with individual regions. These discussions covered technical and
procedural issues and offered the opportunity for regional office staff to raise
questions.
|
|

|
|
Education Program and Quality Control
|
|
Internal Education and Support Regarding Group Health Plan Compliance Assistance
|
|
New Training Tools - The national office worked closely with the regions to modify the HIPAA
checksheet and to develop additional materials to assist the regional offices
with investigations. EBSA’s benefit advisors, who receive public inquiries and
participate in compliance assistance outreach regarding the provisions of Part 7
of ERISA, would also use these tools. Examples of the various materials
developed include:
-
HIPAA Checksheet — OHPSCA retooled the HIPAA
checksheet, which was
designed for investigators to determine whether health plans are in compliance
with the law. Updates were made and modifications were added in accordance with
suggestions made by the regional offices following the FY 1999 pilot project.
-
The HIPAA Binder — This binder contains: (a) Q&As on recent changes
in health care law, (b) outlines explaining each new statute that was enacted,
(c) the Federal regulations, (d) information regarding comparable State laws,
(e) EBSA health publications, and (f) EBSA regional office and State insurance
department contacts. OHPSCA regularly updates this binder to include new
developments and publications related to health care law.
-
Lessons Learned Charts — These charts, generated by OHPSCA, contain
dozens of examples of commonly used plan provisions and practices that
investigators should be aware of when conducting compliance reviews of health
plans.
|
|
New Delivery Mechanisms - EBSA also made effective use of computer technology to provide the regional
offices with the most up-to-date materials in real time and to communicate
quickly with investigators on specific cases. Examples of the information
delivery mechanisms used by EBSA include:
-
Easy-access Intranet — This EBSA internal-only Web site was created to
provide investigators and benefit advisors with direct access in real time to
the most recent Part 7 compliance materials, such as: (a) the HIPAA Binder
materials (including the regulations and outlines), (b) the Lessons Learned
Charts, (c) HHS and Treasury Department publications, and (d) additional State
law and contact information.
-
Rapid Response Phone and Email Team — Through creation of a HIPAA
contact network, staff from OHPSCA and OE are available to provide immediate
technical assistance to investigators and benefit advisors with respect to
compliance-related inquiries.
-
Training Seminars and Teleconferences — Throughout the year, staff from
OHPSCA and OE travel to regional offices to provide training seminars for
investigators and benefit advisors. In addition, OHPSCA and OE conduct periodic
teleconferences to discuss their experiences and any substantive and procedural
issues that may arise.
-
Data Codes — To facilitate the tracking of Part 7 violations, EBSA
created new data codes (each representing a particular Part 7 violation) for
EMS. Four new codes allowed plans to be identified as not subject to each of the
Part 7 statutes.
|
|

|
|
Compliance Assistance Activities for the Regulated Community
|
|
Compliance Assistance Materials - In addition to the quality control materials created for EBSA staff,
compliance materials were also developed to increase the public’s awareness
and understanding of HIPAA, the Newborns’ Act, MHPA, and WHCRA. The following
are examples of such materials:
-
Q&As Regarding Changes in Health Care Laws — EBSA published
Q&As: Recent Changes in Health Care Laws, which provides employers and
employees with information regarding their rights and obligations under the
health care laws. The information in this booklet is currently being updated and
converted into two new publications — one for employers and one for employees.
-
Frequently Asked Questions/Tips — Drawing from its experience in the FY
1999 pilot project, EBSA published Compliance Assistance for Group Health
Plans,
which provides 10 key compliance considerations for group health plans and tips
on how to bring plans into compliance with Part 7 of ERISA. Simultaneously with
the release of this report, this publication was also updated to a list of 15
key compliance considerations.
-
Posters and Information Cards — EBSA developed several posters and
information cards to increase the public’s awareness of health care laws. One
poster, which provided information on the Newborns’ Act, was distributed in FY
2001 to doctors’ offices (particularly obstetricians’ offices), drug stores,
and hospitals. Another poster provided information to help workers and their
families when their health benefits claims were denied. A card was also
developed to explain key protections under MHPA.
-
Form M-1 Worksheets — Worksheets were included with the Form M-1 Annual
Report for multiple employer welfare arrangements for administrators to use as a
self-audit tool for the provisions of Part 7 of ERISA. The worksheets were
updated in 2001 to include compliance tips.
|
|
Compliance Assistance Outreach Programs - EBSA also expanded its outreach programs to deliver these materials to the
public efficiently. These programs include:
-
Internet — All of EBSA’s publications and regulations are available
on its Internet site at www.dol.gov/pwba.
-
Public Outreach — Throughout the year, representatives from the Agency’s
national office and regional offices participate in seminars and presentations
to educate and familiarize employees, employers, plan administrators, issuers,
third-party administrators (TPAs), and State insurance department staff with
Part 7 of ERISA.
-
Expanded Participant and Compliance Assistance Program — EBSA increased
the number of benefit advisors in response to the significant rise in health
care inquiries. These benefit advisors handle written and telephone inquiries
from the public and conduct public outreach. They also participate in rapid
response programs following events such as plant closings and employer
bankruptcies to inform dislocated workers and their families about their rights
to private-sector health care.
-
Health Benefits Education Campaign — This campaign, which was launched
in FY 1999, is comprised of over 70 partners, representing a wide range of
interests from employees to employers to health care providers. Through the
campaign, EBSA distributes information on Federal health care laws to employees,
employers, plan administrators, issuers, TPAs, and State insurance department
staff. EBSA also participates in the campaign’s compliance assistance seminars
that take place across the country to help increase awareness regarding Part 7’s
provisions and to answer questions from the regulated community on its
requirements.
|
|

|
|
|
|
The following summary addresses noncompliance with the new health care laws
individually and overall. It also examines noncompliance with these laws by
sample (small single-employer plans, large single-employer plans, and multiemployer
plans). In doing this, it is important to realize that the goal of
the project was to measure the presence, rather than the extent, of violations
in sample plans. Therefore, if a plan is cited with any violation, the plan is
treated as being out of compliance. Thus, the weighted violation rates(15) found
in the tables include plans that may have been cited with one or numerous
violations. Moreover, the rates do not take into account the number of
participants and beneficiaries affected by a violation, which varies by
individual provision and individual plan.
|
|

|
|
Noncompliance Rates
|
|
Based on the data, it appears implementation of the requirements of Part 7 by
group health plans has progressed steadily. Only 8 percent of plans were cited
with a violation of MHPA. This low violation rate may have resulted from the
narrow scope of MHPA’s provisions and the relatively simple changes that plans
made in order to come into compliance.
|
|
The investigations showed that 4.5 percent and 5.2 percent of plans were
cited with a violation of the substantive provisions of WHCRA and the Newborns’
Act, respectively (that is, the provisions of these laws other than the notice
requirements). Most violations of these two laws involved problems with adequate
or timely notices. Specifically, after taking into account the notice
requirements, 35.0 percent and 21.8 percent of plans were cited with a violation
of the Newborns’ Act and WHCRA, respectively.
|
|
Regarding HIPAA, the data reveal that 28.1 percent of plans were cited with
at least one violation of HIPAA’s substantive portability or nondiscrimination
provisions. Many of the violations involved discrete plan provisions. In these
instances, EBSA found that a single plan provision could violate multiple HIPAA
requirements. After factoring in the notice requirements, 35.9 percent of plans
in the sample were cited with at least one violation.
|
|
Accordingly, after taking into account all of the violations cited, the data
reveal that 30.7 percent of plans were cited with at least one violation of the
36 substantive requirements under the four laws. After factoring in the six
additional notice provisions, 45.3 percent of group health plans were cited with
at least one violation. In many cases, noncompliance may have been the result of
a mistake in understanding and complying with the laws. Given the short
implementation period since the provisions of Part 7 and the regulations became
effective, and taking into account the size of the ERISA health plan universe
(approximately 2.5 million plans), this confusion in implementation is not
unexpected.
|
|
 MHPA Noncompliance Rates
- Among the four health care laws, MHPA was found to have the lowest
noncompliance rate, 8.0 percent. (See Table 6 and Chart 2.)(16)
One explanation of
the low violation rate could be that the GAO published its May 2000 report
involving MHPA compliance(17) before EBSA initiated the project, which may have
caused a decrease in the number of MHPA violations. Thus, GAO’s focus on MHPA
compliance may have contributed to additional MHPA compliance among other plan
sponsors and administrators throughout the country. This may also explain why
noncompliance rates fell from 14 percent when the GAO did its 1999 survey to 8 percent in this FY 2001 project. MHPA Noncompliance Rates
- Among the four health care laws, MHPA was found to have the lowest
noncompliance rate, 8.0 percent. (See Table 6 and Chart 2.)(16)
One explanation of
the low violation rate could be that the GAO published its May 2000 report
involving MHPA compliance(17) before EBSA initiated the project, which may have
caused a decrease in the number of MHPA violations. Thus, GAO’s focus on MHPA
compliance may have contributed to additional MHPA compliance among other plan
sponsors and administrators throughout the country. This may also explain why
noncompliance rates fell from 14 percent when the GAO did its 1999 survey to 8 percent in this FY 2001 project.
|
|
Further, because MHPA is very narrowly focused on annual and lifetime dollar
limits and some plans never included these limits, these plans were
automatically in compliance with the law. Finally, another reason for the high
compliance rate could be that compliance with MHPA is fairly easy and
inexpensive — plans can merely delete annual and lifetime dollar limits on
mental health benefits while retaining other restrictions such as visit and
network limits.
|
|
Nonetheless, annual dollar limits and constructive annual dollar limits
comprised the majority of the violations cited. Examining all of the plans cited
with MHPA violations, 58 percent included annual dollar limits and 53 percent
included constructive annual dollar limits that were out of compliance with MHPA.
(Derived from violation rates in Table 6.) This may be because annual limits are
more prevalent than lifetime limits and, therefore, are more likely to be out of
parity.
|
|
EBSA investigators cited constructive dollar limits when a plan had a
combination of a fixed limit on the number of visits per year and a fixed limit
on the payment per visit that effectively imposed a ceiling on annual mental
health benefits that was lower than for medical/surgical benefits. For example,
suppose a plan has no dollar limit or visit limit on medical/surgical benefits,
but has a 30-visit limit per year on mental health benefits coupled with a $100
maximum payment by the plan per visit. The plan, in effect, has a $3,000 annual
limit on mental health benefits while having no such limit on medical/surgical
benefits.(18) In situations such as these, violations of MHPA’s annual dollar
limit provisions were cited.
|
|
To help increase compliance with MHPA’s annual dollar limit provisions,
EBSA’s publication Compliance Assistance for Group Health Plans warns plans
and issuers about constructive dollar limits and provides tips on how to bring
plans into compliance.
|
|
 WHCRA Noncompliance Rates
- Regarding WHCRA, noncompliance with the substantive provisions (that is, the
provisions other than the notice requirements) was generally low; only 4.5
percent of plans were cited with a substantive violation. (See Table 7.)
However, taking into account the notice requirements, noncompliance was higher.
As Table 6 and Chart 3 show, EBSA cited 21.8 percent of plans for a violation of
WHCRA. The effect of the notice violations is more prominent when examining the
percentage of all plans that were cited with failing to provide WHCRA’s annual
and/or enrollment notice (17.7 percent). (See Table 6.)(19)
Moreover, 8.8 percent
of plans were cited for failing to provide WHCRA’s one-time, January 1999
notice.(20) Small plans were responsible for most of the violations. (With respect
to small plans, 18.0 percent were cited for failure to provide the annual and/or
enrollment notice and 8.9 percent were cited for failure to provide the one-time
notice.) WHCRA Noncompliance Rates
- Regarding WHCRA, noncompliance with the substantive provisions (that is, the
provisions other than the notice requirements) was generally low; only 4.5
percent of plans were cited with a substantive violation. (See Table 7.)
However, taking into account the notice requirements, noncompliance was higher.
As Table 6 and Chart 3 show, EBSA cited 21.8 percent of plans for a violation of
WHCRA. The effect of the notice violations is more prominent when examining the
percentage of all plans that were cited with failing to provide WHCRA’s annual
and/or enrollment notice (17.7 percent). (See Table 6.)(19)
Moreover, 8.8 percent
of plans were cited for failing to provide WHCRA’s one-time, January 1999
notice.(20) Small plans were responsible for most of the violations. (With respect
to small plans, 18.0 percent were cited for failure to provide the annual and/or
enrollment notice and 8.9 percent were cited for failure to provide the one-time
notice.)
|
|
The reason for this high rate of noncompliance may be that WHCRA regulations
are still under development. EBSA did publish guidance on the WHCRA notice
requirements and provided model notices in 1999. However, some plans may not
have found this guidance, which is available on EBSA’s Web site, but was not
published in the Federal Register because it is informal guidance rather than a
regulation. Issuers in particular may not be accustomed to contacting EBSA for
compliance assistance, which may have impacted the small plan noncompliance rate
especially because small plans are more likely to be insured. (21)
|
|
To coordinate more closely with issuers and to help them use EBSA as a
resource, the Agency began to sponsor compliance assistance seminars targeted
towards issuers, TPAs, and other service providers. EBSA held five of these
seminars in calendar year 2001 and held four seminars in calendar year 2002.
These seminars are jointly sponsored with State insurance departments and take
place across the country.
|
|
 Newborns’ Act Noncompliance Rates
- Noncompliance with the substantive provisions of the Newborns’ Act was also
low; only 5.2 percent of plans were cited with a substantive violation (See
Table 7.) However, similar to WHCRA, notice requirements were problematic. Among
all of the plans investigated, 32.5 percent were cited with a violation of the
notice requirements and, overall, 35 percent of plans were cited with a
violation. (See Table 6 and Chart 4.) Accordingly, of the plans that were cited
with Newborns’ Act violations, 93 percent involved notice violations.
Moreover, small plans were much more likely to have violated the Newborns’ Act
notice provisions than large or multiemployer plans. (As Table 6 and Chart 5
show, 34.2 percent of small plans were cited with Newborns’ Act notice
violations.) One reason for this high incidence of violations may be confusion
as to the applicability of the Newborns’ Act. Newborns’ Act Noncompliance Rates
- Noncompliance with the substantive provisions of the Newborns’ Act was also
low; only 5.2 percent of plans were cited with a substantive violation (See
Table 7.) However, similar to WHCRA, notice requirements were problematic. Among
all of the plans investigated, 32.5 percent were cited with a violation of the
notice requirements and, overall, 35 percent of plans were cited with a
violation. (See Table 6 and Chart 4.) Accordingly, of the plans that were cited
with Newborns’ Act violations, 93 percent involved notice violations.
Moreover, small plans were much more likely to have violated the Newborns’ Act
notice provisions than large or multiemployer plans. (As Table 6 and Chart 5
show, 34.2 percent of small plans were cited with Newborns’ Act notice
violations.) One reason for this high incidence of violations may be confusion
as to the applicability of the Newborns’ Act.
|
|
All self-insured plans are required to comply with the Newborns’ Act,
including its notice provisions. In contrast, insured plans in States that have
a State law applicable to insurance and that meets certain requirements are not
subject to the substantive provisions of the Newborns’ Act.(22)
Nonetheless,
these insured plans are still required to make certain disclosures with respect
to hospital stays in connection with childbirth.(23)
|
|
 Perhaps, because small plans are more likely to be insured and because there
may have been some confusion among the issuers as to whether ERISA requires
disclosures by insured plans regarding hospital stays in connection with
childbirth, a high number of these violations were cited. Even though the error
might have originated with the issuer, the plan administrator is ultimately
responsible for compliance with ERISA and, thus, was cited in these instances. Perhaps, because small plans are more likely to be insured and because there
may have been some confusion among the issuers as to whether ERISA requires
disclosures by insured plans regarding hospital stays in connection with
childbirth, a high number of these violations were cited. Even though the error
might have originated with the issuer, the plan administrator is ultimately
responsible for compliance with ERISA and, thus, was cited in these instances.
In addition, because the original regulation addressing the Newborns’ Act
notice required plans to describe the provisions of the Federal law and most
insured plans are subject to State law requirements rather than the Federal law,(24) there may have been some resistance by issuers for insured plans to make
such disclosures. In an attempt to address legitimate concerns by some issuers
and insured plans, EBSA worked with these entities to develop language that
could be used to meet their obligations under ERISA while also summarizing
accurately the rights of participants and beneficiaries to hospital stays in
connection with childbirth under State law. The Newborns’ Act notice
regulation was revised in November 2000 to decrease confusion and uncertainty
regarding this requirement.(25)
|
|
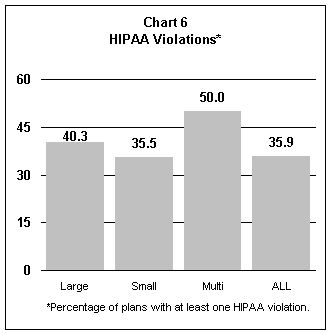 HIPAA Noncompliance Rates
- Among the four health care laws, HIPAA had the highest rate of noncompliance;
28.1 percent of plans were cited with a substantive violation. (See Table 7.)
After taking into account the effect of notice violations, the noncompliance
rate was 35.9 percent. (See Table 6 and Chart 6.) The HIPAA violations may be
divided into four categories: 1) impermissible preexisting condition exclusions;
2) nondiscrimination violations; 3) failure to provide complete certificates of
creditable coverage; and 4) special enrollment violations. With regard to
impermissible preexisting condition exclusions, 23.8 percent of plans were cited
with a violation. (See Table 6.) This relatively high rate of noncompliance may
be due to the presence of violations for three discrete issues. First, EBSA
investigators identified “hidden preexisting condition exclusions” in a
number of plans. Second, EBSA identified nonconfinement clauses in 4.9 percent
of plans, which resulted in violations of both the preexisting condition
exclusion provisions and the nondiscrimination provisions. (See Table 6.) Third,
some plans and issuers improperly calculated the beginning of the 12-month (or
18-month) look-forward period and the end of the 6-month look-back period. (EBSA
cited 9.5 percent of plans for violating the 12-month (or 18-month) look-forward
provision and 11.7 percent of plans for violating the 6-month look-back
provision, some of which is attributable to a miscalculation as to the start or
end of the period. (See Table 6.)) All of these problems are explained below. HIPAA Noncompliance Rates
- Among the four health care laws, HIPAA had the highest rate of noncompliance;
28.1 percent of plans were cited with a substantive violation. (See Table 7.)
After taking into account the effect of notice violations, the noncompliance
rate was 35.9 percent. (See Table 6 and Chart 6.) The HIPAA violations may be
divided into four categories: 1) impermissible preexisting condition exclusions;
2) nondiscrimination violations; 3) failure to provide complete certificates of
creditable coverage; and 4) special enrollment violations. With regard to
impermissible preexisting condition exclusions, 23.8 percent of plans were cited
with a violation. (See Table 6.) This relatively high rate of noncompliance may
be due to the presence of violations for three discrete issues. First, EBSA
investigators identified “hidden preexisting condition exclusions” in a
number of plans. Second, EBSA identified nonconfinement clauses in 4.9 percent
of plans, which resulted in violations of both the preexisting condition
exclusion provisions and the nondiscrimination provisions. (See Table 6.) Third,
some plans and issuers improperly calculated the beginning of the 12-month (or
18-month) look-forward period and the end of the 6-month look-back period. (EBSA
cited 9.5 percent of plans for violating the 12-month (or 18-month) look-forward
provision and 11.7 percent of plans for violating the 6-month look-back
provision, some of which is attributable to a miscalculation as to the start or
end of the period. (See Table 6.)) All of these problems are explained below.
|
|
Hidden preexisting condition exclusions may not have been apparent to some
plan administrators, issuers, and TPAs although EBSA investigators were
specifically trained to identify these types of violations. As explained
earlier, a plan seeking to impose a preexisting condition exclusion is required
to comply with HIPAA’s limitations on preexisting condition exclusions,
including the 6-month look-back limitation, 12-month look-forward limitation
offset by creditable coverage, general notice, and individual notice. Rather
than make all of these changes, some plan sponsors chose to eliminate their plan’s
overall preexisting condition exclusion. However, remaining plan exclusions may
have had some form of timing provision that made the exclusion preexisting in
nature. Because these plans may not have realized that these exclusions are
considered preexisting condition exclusions, they did not comply with HIPAA’s
limitations on such plan provisions and multiple violations of HIPAA were cited.
|
|
An example of a hidden preexisting condition exclusion is a plan provision
that covers treatment for injuries in connection with an accident only if the
accident occurred while the individual was covered under the plan. Another
example is a plan provision that excludes coverage for cosmetic surgery unless
it is required by reason of a congenital defect and the individual has been
continuously covered under the plan since birth.
|
|
When these hidden preexisting condition exclusions were detected, violations
of HIPAA’s 6-month look-back period, 12-month look-forward period, offset by
creditable coverage, general notice, and individual notice provisions were
cited. (See Table 9 regarding high correlations among these violations.)
Accordingly, a single mistake by a plan caused multiple citations for HIPAA
violations in these instances.
|
|
To raise awareness regarding hidden preexisting condition exclusions, EBSA
published Compliance Assistance for Group Health Plans, which sets forth ten key
compliance considerations and tips on how to bring the plan into compliance.
Hidden preexisting condition exclusions are highlighted as the number one
compliance consideration.
|
|
Another violation cited by some EBSA investigators involved a plan’s
imposition of a non-confinement clause. (See Table 6, which identifies 4.9
percent of plans being cited with non-confinement clause violations.) An example
of a non-confinement clause is a plan provision stating that if a dependent is in
a hospital or other health care facility on the date coverage is otherwise to
become effective, the effective date of coverage is delayed until the dependent
is released from the hospital or health care facility. Because these plan
provisions deny benefits for a condition based on the fact that the condition
was present before the effective date of coverage, they are preexisting
condition exclusions. As with hidden preexisting condition exclusions, when
non-confinement clauses were found, multiple violations of the preexisting
condition exclusion provisions were cited by EBSA investigators. In addition,
because these plan provisions deny eligibility based on a health factor, they
are also violations of HIPAA’s nondiscrimination provisions and were cited as
such.
|
|
To help raise awareness as to the impermissibility of non-confinement
provisions, EBSA collaborated with the Centers for Medicare & Medicaid
Services (formerly the Health Care Financing Administration) to publish
Insurance Standards Bulletins 00-01 and 00-04, which describe different types of
non-confinement provisions and explain the multiple HIPAA provisions they
violate.
|
|
The third reason some plans were cited with violations for an impermissible
preexisting condition exclusion is that the plan improperly calculated the
beginning of the 12-month (or 18-month) look-forward period and the end of the
6-month look-back period. Under HIPAA, these periods are measured from an
individual’s enrollment date. The enrollment date is defined as the first day
of coverage under the plan, or if there is a waiting period for coverage, the
first day of the waiting period.(26) Therefore, if an individual begins work on
January 15 and coverage does not begin until the first day of the next calendar
month (February 1), the individual has a 17-day waiting period for coverage.
Moreover, the individual’s enrollment date is January 15, the first day of the
waiting period, and the 12-month look-forward and 6-month look-back periods
should be measured from this date. EBSA found that some plans that included a
waiting period calculated these periods from the first day of coverage (February
1 in this example), rather than the first day of the waiting period. This was
apparent particularly when health coverage was offered through an issuer or
through a multiemployer plan, where these parties may be further removed from
the employer and less likely to know an individual’s date of hire.
|
|
Because these miscalculations result in longer preexisting condition
exclusions for individuals than is permissible and to increase awareness among
the regulated community regarding this issue, EBSA included in its publication
Compliance Assistance for Group Health Plans information on enrollment dates and
tips on how to bring the health plan into compliance. At seminars with issuers
and multiemployer plans, EBSA representatives also encouraged these entities to
coordinate with employers to get information on individuals’ dates of hire to
avoid this problem.
|
|
With respect to HIPAA’s certificate provisions, 7.3 percent of plans were
cited with a violation. (See Table 6.) This rate of noncompliance initially
caused concern because the certificate provisions are so important –
certificates provide individuals with evidence of their creditable coverage,
which may be used to reduce a future preexisting condition exclusion and to gain
guaranteed access to health coverage in the individual insurance market.(27)
However, after closer inspection, in many of the plans it was not that plans
were failing to issue certificates of creditable coverage. Rather, certificates
were being provided, but they were incomplete. Two pieces of information that
some plans were missing were waiting period information and dependent
information.
|
|
Specifically, under HIPAA, there are seven data elements required to be
included on a certificate of creditable coverage: the date of the certificate;
the name of the group health plan; the name of the participant (or dependent)
and his or her identification number; certain identifying information regarding
the plan administrator or issuer who is required to provide the certificate; the
telephone number to call for further information regarding the certificate; the
individual’s creditable coverage information (which includes, if the
individual has less than 18 months of creditable coverage, the date any waiting
period began and the date coverage began); and the date coverage ended (if it
ended). Participants and their dependents each have an independent right to
certificates of creditable coverage, although plans can combine creditable
coverage information for families on a single certificate, which may be copied,
if the information is the same.
|
|
Based on EBSA’s experience, it seems that some plans were neither providing
certificates to dependents, nor identifying dependents on the certificate of
creditable coverage provided to participants. In these cases, the certificates
were incomplete because they did not provide dependents with any evidence of
creditable coverage, as required by HIPAA, and were cited accordingly. Other
plans were not including waiting period information on certificates of
creditable coverage. This information is important because, under HIPAA, time
spent in a waiting period for coverage tolls any significant break in coverage
that might otherwise occur with respect to the individual.(28)
As such, it is
required to be reported on the certificate of creditable coverage for
individuals with less than 18 months of creditable coverage.
|
|
To increase compliance assistance and awareness as to the importance of
including this information on certificates of creditable coverage, EBSA’s
publication Compliance Assistance for Group Health Plans discusses the inclusion
of dependent and waiting period information on certificates of creditable
coverage.
|
|
Regarding special enrollment rights, 15.9 percent of plans were cited with a
violation, which occurred most often with respect to the notice of special
enrollment rights. (See Table 6, which shows that 12.1 percent of plans were
cited with a violation of the special enrollment notice provision while only 5.2
percent of plans were cited for failing to provide substantive special
enrollment rights to individuals upon loss of coverage and only 3.0 percent of
plans were cited for failing to provide special enrollment after gaining a new
dependent.) Of the plans cited for a special enrollment violation, 76 percent
involved a special enrollment notice violation.
|
|
EBSA was concerned that 12.1 percent of plans were cited for violations of
the special enrollment notice provisions, especially in light of the fact that
the regulations provide a model notice.(29)
(See Table 6.) Some of the
noncompliance may be attributed to the fact that a number of plans provided
special enrollment under their own terms before the passage of HIPAA. These
plans likely assumed that no additional changes were required in order to comply
with the special enrollment provisions – overlooking the special enrollment
notice requirement. For some violations, EBSA found that plans did provide the
special enrollment notice, but did not provide the notice within required time
frames. The special enrollment notice must be provided to an employee on or
before the time the employee is offered the opportunity to enroll in the plan.(30)
Some plans that were cited included the special enrollment notice in the plan’s
summary plan description (SPD), which is a permissible form of disclosure, but
which has separate timing requirements. If a plan provided employees with the
SPD after enrollment, a violation of the special enrollment notice provisions
was cited.
|
|
Overall Part 7 Noncompliance Rate - After taking into account all of the violations cited under the four health
care laws, the data reveal that 30.7 percent of group health plans were cited
with a violation of at least one substantive provision of the new health care
laws. After taking into account violations of notice requirements, 45.3 percent
of group health plans were cited with a violation of at least one provision of
Part 7. While this may initially seem relatively high to some, several
mitigating factors should be considered when interpreting this number. As
explained earlier, EBSA investigators were highly trained in identifying
violations of discrete and sometimes technical areas of the law. Their
expertise, combined with the large number of Part 7 requirements, may help
explain the relatively high rate of noncompliance found. Moreover, when
violations were detected, EBSA investigators were generally able to secure
voluntary compliance with the law.
|
|

|
|
Trends Within the Numbers
|
|
High Compliance Rates Observed for Certain Part 7 Provisions
- The attached tables show that a majority of group health plans are in
compliance with certain Part 7 provisions. One of HIPAA’s most important
provisions relates to group health plans providing certificates of creditable
coverage. As Table 6 shows, most plans (92.7 percent) complied with this
requirement. In addition, after excluding violations cited for non-confinement
clauses, compliance with HIPAA’s nondiscrimination requirements was also very
high (96 percent).(31) Compliance with MHPA (92 percent) and the substantive
provisions (excluding the notice requirements) of the Newborns’ Act (94.8
percent) and WHCRA (95.5 percent) was also high. (See Table 7.)
|
|
Many Violations Involved Part 7 Notice Requirements
- Many of the violations cited in the project involved noncompliance with one
or more of Part 7’s notice requirements. Excluding certificates of creditable
coverage, plans are required to make six disclosures under Part 7, many of which
are often made in the SPD. These six disclosures are: (a) a general notice of
preexisting condition exclusions (for plans imposing a preexisting condition
exclusion); (b) individual notices of preexisting condition exclusions (for
plans imposing a preexisting condition exclusion); (c) a notice of special
enrollment rights; (d) a Newborns’ Act notice; (e) WHCRA annual and enrollment
notices; and (f) a WHCRA one-time notice. Of those plans that were required to
provide these notices, 14.5 percent of plans were cited for failure to provide
an adequate general notice of preexisting condition exclusion (so that 40
percent of plans cited with a HIPAA violation failed to provide the general
notice) and 10.5 percent of plans were cited for failure to provide an adequate
individual notice of preexisting condition exclusion (so that 29 percent of
plans cited with a HIPAA violation failed to provide the individual notice).
With respect to the special enrollment notice, violations were cited in 12.1
percent of plans (so that 34 percent of plans cited with a HIPAA violation
failed to provide the special enrollment notice). As mentioned earlier,
violations of the notice requirements accounted for most of the overall
noncompliance rates for the Newborns’ Act (32.5 percent) (so that 93 percent
of plans cited with a Newborns’ Act violation failed to provide this notice)
and WHCRA (17.7 percent and 8.8 percent) (so that 81 percent of plans cited with
a WHCRA violation failed to provide the annual and/or enrollment notice and 40
percent of plans cited with a WHCRA violation failed to provide the one-time
notice). Interestingly, MHPA, which has no notice requirement, had the lowest
noncompliance rate of the four health care laws.
|
|
In some cases, noncompliance was cited because the plan failed to provide any
notice. In other cases, notice was provided but was found to be inadequate. In
either case, the development and distribution of model notices by EBSA should
lead to increased future compliance. EBSA intends to issue model language for
the two notices of preexisting condition exclusion when it publishes its final
HIPAA portability regulations. As described earlier, EBSA has made changes to
the Newborns’ Act notice requirement and is developing regulations for
distribution of the model language for WHCRA disclosures to a wider audience.
|
|
 As illustrated in Table 7 and Chart 7, by not taking into account violations
with respect to the Part 7 notices, the overall noncompliance rate decreases
from 45.3 percent to 30.7 percent. HIPAA noncompliance in particular decreases
from 35.9 percent to 28.1 percent and noncompliance with the Newborns’ Act and
WHCRA decrease dramatically from 35.0 percent and 21.8 percent to 5.2 percent
and 4.5 percent, respectively. As such, EBSA hopes that taking the relatively
simple steps outlined above regarding compliance assistance with the notice
provisions will lead to greatly increased overall Part 7 compliance rates in the
future. As illustrated in Table 7 and Chart 7, by not taking into account violations
with respect to the Part 7 notices, the overall noncompliance rate decreases
from 45.3 percent to 30.7 percent. HIPAA noncompliance in particular decreases
from 35.9 percent to 28.1 percent and noncompliance with the Newborns’ Act and
WHCRA decrease dramatically from 35.0 percent and 21.8 percent to 5.2 percent
and 4.5 percent, respectively. As such, EBSA hopes that taking the relatively
simple steps outlined above regarding compliance assistance with the notice
provisions will lead to greatly increased overall Part 7 compliance rates in the
future.
Effect of Issuers - As noted above, one survey found that most small companies do not self-insure
their health benefits.(32) Instead, most small firms obtain group health coverage
through a health insurance issuer. Among the findings in a recent GAO survey of
the small group health insurance market is that the median market share of each
State’s largest insurance carrier was approximately 33 percent in the States
surveyed.(33) Plan sponsors of any size may purchase coverage (including model
plan documents) from issuers and contract for provision of certificates and
notices by issuers. The tendency of small firms to contract with issuers and the
dominant market share of certain issuers in some markets suggests a potential
multiplier effect. For example, a fully compliant prototype plan document
benefits each group health plan that follows the provisions. Conversely,
confusion concerning one issuer’s notice and disclosure obligations would
generally affect multiple plans. For the reasons discussed in Section V below,
EBSA intends to explore this possible effect.
|
|
 Small and Large Plans Have Lowest Overall
Noncompliance Rates - The project was designed, in part, to measure compliance among large and
small single-employer plan sponsors, determined by taking into account the
number of employees reported. In contrast, Table 5A and Chart 8 indicate
violation rates by single-employer plans broken down by the number of
participants reported in the plan. This table shows that mid-sized plans
experienced higher noncompliance rates than small and large plans. Very small
plans (those with 2-9 participants) and small plans (those with 10-24
participants) had overall Part 7 noncompliance rates of 43.2 percent and 48.8
percent, respectively. Part 7 noncompliance peaked for mid-sized plans (those
with 25-99 participants) at 52.3 percent. Then, noncompliance fell again for
large plans (those with 100-500 participants) and very large plans (those with
500 participants or more), which had noncompliance rates of 46.0 percent and
37.0 percent, respectively. Small and Large Plans Have Lowest Overall
Noncompliance Rates - The project was designed, in part, to measure compliance among large and
small single-employer plan sponsors, determined by taking into account the
number of employees reported. In contrast, Table 5A and Chart 8 indicate
violation rates by single-employer plans broken down by the number of
participants reported in the plan. This table shows that mid-sized plans
experienced higher noncompliance rates than small and large plans. Very small
plans (those with 2-9 participants) and small plans (those with 10-24
participants) had overall Part 7 noncompliance rates of 43.2 percent and 48.8
percent, respectively. Part 7 noncompliance peaked for mid-sized plans (those
with 25-99 participants) at 52.3 percent. Then, noncompliance fell again for
large plans (those with 100-500 participants) and very large plans (those with
500 participants or more), which had noncompliance rates of 46.0 percent and
37.0 percent, respectively.
|
|
EBSA observed a similar trend among small and large multiemployer
plans. Very
small multiemployer plans (those with 2-99 participants) and small multiemployer
plans (those with 100-499 participants) had overall Part 7 noncompliance rates
of 50.0 percent and 52.3 percent, respectively. With respect to mid-sized multiemployer
plans (those with 500-999 participants), Part 7 noncompliance
peaked at 68.0 percent. For large multiemployer plans (those with 1,000-4,999
participants) and very large multiemployer plans (those with 5,000 or more
participants), the noncompliance rates were 67.9 percent and 51.3 percent,
respectively. (See Table 5B and Chart 8.)
|
|
One reason that compliance among very small and small plans may have been
higher is the effect of issuers in the small group health plan market.(34)
Issuers’
policies may be more likely to comply with Part 7 for several reasons. First,
many State insurance departments review insurance policies for compliance with
health care laws before they are approved for marketing to employers. Second,
many issuers tend to hire general counsel specializing in health care laws.
Moreover, large and very large plan sponsors may also have human resource
departments and general counsel specializing in health care laws.
|
|
Conversely, mid-sized plan sponsors may lack the expertise of an issuer and
the resources of larger plans. Some of these mid-sized employers, when deciding
the terms of the plans they sponsor, may mirror provisions in their stop-loss
insurance policies(35) without taking additional steps to comply with applicable
law. Because stop-loss insurers are not separately subject to Part 7, these
policies may contain provisions that violate Part 7. Therefore, unless the plan
sponsor takes steps to ensure compliance, violations may exist.
|
|
Multiemployer Plans Have Highest Overall Noncompliance Rate
- Multiemployer plans are established through collective bargaining between one
or more labor unions and two or more employers. In contrast to the
single-employer plans reviewed, multiemployer plans have a board of trustees
comprised of an equal number of representatives from labor and management. The
governance and service provider relationships unique to multiemployer plans may
account for the relatively high noncompliance rate of 60.1 percent. (See Table 2
and Chart 9.)
|
|
Experience has shown that some multiemployer plan documents were drafted
decades earlier and are rewritten over the years. Accordingly, piecemeal
compliance may result. In addition, the effective date for some multiemployer plans may have been more recent than the effective date for single-employer
plans. Some multiemployer plans may have had a shorter time frame within which
to understand and implement HIPAA’s provisions. Finally, EBSA found that a
multitude of plans could be impacted as a result of misunderstandings by TPAs
regarding the implementation of the new health care laws. As a result of these
misunderstandings, a multiplier effect could have occurred among plans in the
nation and the sample. To the extent that TPAs can have such a large impact on
compliance, EBSA may be able to work with these entities in the future and
leverage its enforcement resources to obtain broad-based compliance from many multiemployer
plans. (In this regard, see also the discussion of Supplemental
Benefits under Section V, below.)
|
|
 Other Correlations Between Violations
- Table 9 sets forth the highest correlations between violations that were
cited for all three samples pooled. Having a correlation coefficient(36) closer to
1.0 indicates that if one of the violations occurs, there is a very high
probability the other violation will also occur. As Table 9 shows, a plan that
was cited for a violation of one of the preexisting condition exclusion period
provisions was likely to have been cited for a violation of other preexisting
condition exclusion period provisions. Of the top 10 pairs of violations having
the highest correlations, 7 pairs involved correlations of HIPAA preexisting
condition exclusion periods. (EBSA found correlations ranging from 0.796 to
0.504 for these 7 pairs.)(37) These correlations are consistent with EBSA’s
finding of hidden preexisting condition exclusions and non-confinement clauses in
some plans, which resulted in citations for multiple preexisting condition
exclusion period violations by those plans. In addition, a plan that was cited
for a violation of one of the substantive special enrollment provisions was
likely to have been cited for a violation of the other substantive special
enrollment provisions. (EBSA found a 0.478 correlation between violations of
provisions governing special enrollment triggered by a new dependent and those
triggered by loss of other coverage.) Violations of MHPA’s annual and lifetime
provisions were also closely correlated. (EBSA found a 0.601 correlation between
these violations.) Other Correlations Between Violations
- Table 9 sets forth the highest correlations between violations that were
cited for all three samples pooled. Having a correlation coefficient(36) closer to
1.0 indicates that if one of the violations occurs, there is a very high
probability the other violation will also occur. As Table 9 shows, a plan that
was cited for a violation of one of the preexisting condition exclusion period
provisions was likely to have been cited for a violation of other preexisting
condition exclusion period provisions. Of the top 10 pairs of violations having
the highest correlations, 7 pairs involved correlations of HIPAA preexisting
condition exclusion periods. (EBSA found correlations ranging from 0.796 to
0.504 for these 7 pairs.)(37) These correlations are consistent with EBSA’s
finding of hidden preexisting condition exclusions and non-confinement clauses in
some plans, which resulted in citations for multiple preexisting condition
exclusion period violations by those plans. In addition, a plan that was cited
for a violation of one of the substantive special enrollment provisions was
likely to have been cited for a violation of the other substantive special
enrollment provisions. (EBSA found a 0.478 correlation between violations of
provisions governing special enrollment triggered by a new dependent and those
triggered by loss of other coverage.) Violations of MHPA’s annual and lifetime
provisions were also closely correlated. (EBSA found a 0.601 correlation between
these violations.)
|
|

|
|
|
|
During the project, EBSA focused its investigative efforts primarily on
compliance with respect to specific group health plans. Although most of these
plans agreed to amend their plan documents to comply with Part 7, a more
global effect emerged as a result of the investigations. EBSA determined that
noncompliance for some plans originated with their service providers (that is,
their issuers or TPAs). Specifically, some plan provisions that were cited for
a violation of Part 7 were derived from policies or model plan documents
generated by issuers or TPAs with standard provisions. In these cases, the
simple amendment of an issuer’s policy or TPA’s document results in a
one-time correction for a much larger universe, particularly if the issuer or
TPA operates nationwide.
|
|
Some investigators pursued this broad-based compliance assistance effort in
the project and other cases by attempting to work with issuers and TPAs on
standard provisions that were in violation of a Part 7 provision. EBSA
determined that when the issuers and TPAs agreed to amend policy terms or
model documents, thousands of plans and millions of participants were affected
by the corrections. At the close of the first quarter of FY 2002, four
regional offices were able to estimate the number of participants and plans
affected by this type of compliance. Those estimates reflected that amendments
made to nine different standard insurance policies or model documents resulted
in corrections for over 2.7 million participants and nearly 14,000 insured
plans.(38)
|
|
The primary challenge to pursuing this type of blanket correction is that,
under ERISA, EBSA does not have direct enforcement authority over issuers for
the provisions of Part 7.(39) Therefore, these compliance gains were generally
the result of voluntary compliance work. In some cases, issuers and TPAs
agreed to correct standard provisions to ensure that all ERISA-covered group
health plans they serviced were in compliance with Part 7. In other cases,
EBSA worked with State insurance departments, who retain direct enforcement
authority against issuers, to raise Part 7 awareness and increase broad-based
compliance for standard policies and model documents. Using both compliance
methods, EBSA was able to help bring about additional, far-reaching compliance
assistance by working directly with issuers and TPAs.
|
|

|
|
|
|
The project was a review of group health plans for compliance with 42
specific requirements of the new laws. Generally, EBSA found that group health
plans are in compliance with the substantive provisions of the new health care
laws (that is the provisions other than the notice requirements). Given the
very large and complex universe of ERISA-covered health plans, it was not
unexpected that confusion would arise with respect to implementing the
various, sometimes technical requirements of the new health care laws. In this
regard, the project was initiated in the early stages of the implementation
process - generally only 2 years after the law became effective for most
plans.
|
|
However, implementation problems exist, particularly with respect to
certain notice provisions, as well as regarding certain discrete substantive
provisions that are technical in nature. To address these problems, EBSA is
initiating H-CAP, which is comprised of three strategies, each with an action
plan.
|
|
H-CAP’s first strategy is to develop and distribute additional
publications and other educational materials. EBSA will publish three new
publications to assist group health plans and health insurance issuers in
complying with new health laws. These materials will be distributed through
EBSA’s toll free publications line, at all workshops and compliance
assistance activities, through industry groups and industry newsletters,
through the trade press and other interested media, and via EBSA’s Web site.
|
|
Specifically, a Self-Audit Checklist has been developed. This checklist,
similar to the HIPAA checksheet used by EBSA investigators to determine
compliance, will be a useful tool for plans and issuers to assess their
compliance line-by-line with the health laws. In addition, Compliance
Assistance for Group Health Plans, EBSA’s current publication highlighting
the top ten most common errors made by health plans, has been updated with
five additional tips for group health plans, based on common mistakes found in
the project. It also includes advice on how to avoid these mistakes. Finally a
New Health Laws Notice Guide has been developed summarizing all of the new
health law notice requirements, including sample language that can be used by
plans.
|
|
H-CAP’s second strategy is to dedicate a section of EBSA’s compliance
assistance page on EBSA’s Web site to the new health care laws, making it
easier for plans, issuers, and other service providers to find in one location
all of the regulations, publications, frequently asked questions, and other
guidance. The new, dedicated section will supplement compliance assistance
efforts EBSA has already made, including making our Benefits Advisors
available, through EBSA's Toll-Free Employee & Employer Hotline number,
1.866.444.3272, and
electronically at www.askpwba.dol.gov to answer questions about the new health
law requirements.
|
|
The third strategy is to participate in new, live workshops around the
country where trained staff will meet with plan administrators, plan sponsors,
attorneys, consultants, and other service providers to apply the Self-Audit
Checklist to various sample plan provisions and documents. These live
workshops will supplement the Health Benefits Education Campaign Compliance
Assistance Seminars already conducted by the Agency, which address a wider
variety of health plan topics, including the new health laws.
|
|
In addition to H-CAP, EBSA intends to implement several changes to its
interpretive program. Specifically, EBSA would like to provide additional
clarity and model notices in future interpretive guidance. EBSA intends to
amend its regulations to include sample language that could be used by plans
and issuers providing the general and individual notices of preexisting
condition exclusions. In addition, EBSA intends to amend its regulations to
include model educational information about the HIPAA provisions to be
included in the certificate of creditable coverage. This model language was
suggested by the GAO(40) and EBSA hopes this type of education will increase
awareness about and compliance with HIPAA’s provisions. EBSA also intends to
provide additional regulatory guidance on issues such as hidden preexisting
condition exclusions.
|
|
EBSA is optimistic that these partnership efforts with plans, issuers, and
other service providers will lead to increased understanding about the new
health care laws and increased compliance rates as well.
|
|

|
|
|
-
EBSA's fiscal year runs from October 1
through September 30.
-
For simplicity, this report references
the percentage of plans cited with a violation. However, these
percentages are actually weighted violation rates, which are explained
in footnote 15 of this report.
-
An issuer is generally an insurance company or health maintenance
organization that is required to be licensed and that is subject to State law
that regulates insurance. See 29 CFR § 2590.701-2.
-
HIPAA amended ERISA, the Internal Revenue Code (Code), and the Public
Health Service Act (PHS Act) with parallel provisions. Generally, ERISA covers
private-sector group health plans and health insurance issuers. However, the
Department of Labor does not enforce the provisions of Part 7 directly against
issuers, which are under the jurisdiction of the States or the Department of
Health and Human Services (HHS).
-
See Solicitation of Comments published on December 30, 1996 (61 Fed. Reg.
68697).
-
See Solicitation of Comments published on October 25, 1999 (64 Fed. Reg.
57520).
-
Initially, the Newborns’ Act amended only ERISA and the PHS Act. The
Taxpayer Relief Act of 1997 was enacted on August 5, 1997, and added provisions
substantially similar to those in the Newborns’ Act to the Code.
-
See Solicitation of Comments published on June 26, 1997 (62 Fed. Reg.
34604).
-
Initially, MHPA amended only ERISA and the PHS Act. The Taxpayer Relief Act
of 1997 was enacted on August 5, 1997, and added provisions substantially
similar to those in MHPA to the Code.
-
See Solicitation of Comments published on June 26, 1997 (62 Fed. Reg.
34604).
-
Initially, MHPA included a sunset provision under which the requirements
did not apply to benefits for services furnished on or after September 30, 2001.
Through a series of legislative enactments, the sunset date has been extended to
December 31, 2003. See Pub. L. 107-116, Pub. L. 107-147, and Pub. L. 107-313.
-
The statute amended ERISA and the PHS Act and is administered by the
Departments of Labor and HHS.
-
ERISA section 4(b).
-
See Table 1, which indicates that of 1,604 small firms, 1,045 such
companies were either unreachable (298) or did not offer a covered group health
plan (747).
-
Probabilities of selection vary widely between samples, being highest for
multiemployer plans, and lowest for plans of small firms. (See Appendix.)
Statistical weights correct for these intended differences in probabilities of
selection. Statistical weights also correct for the anticipated, but
unintentional, differences in probabilities of selection that arise from plans
that cover workers at multiple subsidiaries of the same firm. Such plans had
multiple chances of selection, because all subsidiaries are listed in the D
& B database used as the sampling frame. The same plan would have been
investigated if any of its subsidiaries had been selected, leading to a higher
probability of selection, and a lower weight for such plans. The very low
probability of selection for plans of small firms translates into a very high
statistical weight for these plans. As a result, violation rates from the small
firm sample dominate the overall weighted violation rates for all plans, which
are nudged only slightly in the direction of the large firm and multiemployer rates. In simple terms, the violation rate for all plans resembles the violation
rate for small plans, because most plans are small.
-
Because MHPA has no notice requirements, the noncompliance rate is the
same in Table 7, which excludes the effect of the notice provisions and cites
noncompliance with only the substantive provisions of the new health care laws.
-
See Mental Health Parity Act: Despite New Federal Standards, Mental Health
Benefits Remain Limited (GAO/HEHS-00-95, May 10, 2000).
-
For purposes of its enforcement, EBSA did not attempt to construct a
maximum payment in cases where a plan limited payments by a certain percentage
of usual, customary, and reasonable rates for providers in that area.
-
Under ERISA section 713(a), plans must deliver to the participant written
notice of the availability of WHCRA coverage upon enrollment and annually
thereafter. Under ERISA section 713(b), plans are required to provide a one-time
notice to each participant and beneficiary regarding the coverage required by
WHCRA. This notice is required to be transmitted — (1) in the next mailing to
the participant or beneficiary; (2) as part of any yearly informational packet
sent to the participant or beneficiary; or (3) not later than January 1, 1999;
whichever is earlier.
-
The data reflect that, with respect to the annual and/or enrollment
notices, 81 percent of the plans that were cited with a WHCRA violation failed
to provide one or both of these notices. In addition, 40 percent of the plans
that were cited with a WHCRA violation failed to provide the one-time notice.
-
See The Employee Benefits Research Institute fact sheet, “Employment-Based
Health Care Benefits and Self-Funded Employment-Based Plans: An Overview”
(April 2000) at p. 5 (citing 1997 Robert Wood Johnson Foundation Employer Health
Insurance Survey).
-
“(1) In general. — The requirements of this section shall not apply
with respect to health insurance coverage if there is a State law (as defined in
section 731(d)(1)) for a State that regulates such coverage that is described in
any of the following subparagraphs:
-
Such State law requires such coverage to provide for at least a 48-hour
hospital length of stay following a normal vaginal delivery and at least a
96-hour hospital length of stay following a cesarean section.
-
Such State law requires such coverage to provide for maternity and
pediatric care in accordance with guidelines established by the American College
of Obstetricians and Gynecologists, the American Academy of Pediatrics, or other
established professional medical associations.
-
Such State law requires, in connection with such coverage for maternity
care, that the hospital length of stay for such care is left to the decision of
(or required to be made by) the attending provider in consultation with the
mother.” ERISA section 711(f).
-
See ERISA section 711(d) and the applicable regulations at 29 CFR §
2520.102-3(u).
-
It appears that insured coverage in all States except Wisconsin, Puerto
Rico, the Virgin Islands, American Samoa, Wake Island, and the Northern Mariana
Islands is subject to State law requirements that meet the criteria in ERISA
section 711(f), rather than the Federal Newborns’ Act provisions.
-
A group health plan’s summary plan description (SPD) should include a
statement describing any requirements under Federal or State law applicable to
the plan, and any health insurance coverage offered under the plan, relating to
a hospital length of stay in connection with childbirth for the mother or
newborn child. If Federal law applies in some areas in which the plan operates
and State law applies in other areas, the statement should describe the
different areas and the Federal or State law requirements applicable in each.
See 29 CFR § 2520.102-3(u)(1).
-
26 See 29 CFR § 2590.701-3(a)(2).
-
Section 2741 of the PHS Act guarantees access to individual health
insurance coverage without a preexisting condition exclusion for eligible
individuals. Eligible individuals are individuals who have had coverage for at
least 18 months without a significant break in coverage where the most recent
period of coverage was under a group health plan; did not have their group
coverage terminated because of fraud or nonpayment of premiums; are ineligible
for Medicare, Medicaid, or a group health plan; do not have other insurance
coverage; and are ineligible for continuation coverage under COBRA or if
offered COBRA continuation coverage (or continuation coverage under a similar
state program) have both elected and exhausted their continuation coverage.
-
ERISA section 701(c)(2)(B).
-
See 29 CFR § 2590.701-6(c).
-
Id.
-
Although not reflected in the attached tables, after excluding
violations cited for non-confinement clauses, plans were found to have the
following HIPAA violation rates: 7.0 percent for large plans; 6.8 percent for multiemployer
plans; 3.8 percent for small plans; and 4.0 percent for all plans.
-
See supra, note 25. The survey indicated that
4 percent of participants in
plans sponsored by employers with fewer than 50 employees are in self-funded
plans. The percentage increased to 8 percent for participants in plans sponsored by
companies with 50-99 employees.
-
The GAO also found that “[t]he five largest carriers, when combined,
represented three-quarters or more of the market in 19 of the 34 states
supplying information, and they represented more than 90 percent in 7 of these
states.” March 25, 2002 letter from Kathryn G. Allen, Director, Health Care
- Medicaid and Private Health Insurance Issues to The Honorable Christopher
“Kit” Bond concerning Private Health Insurance: Number and Market Share of
Carriers in the Small Group Health Insurance Market.
-
See supra, note 25.
-
Stop-loss insurance is generally protection purchased by self-funded
plans or their plan sponsors against the risk of large losses or severe
adverse claims experience. In some cases, this type of coverage merely
indemnifies the plan or the plan sponsor if aggregate claims reach a certain
attachment point. In other cases, the insurance coverage may cover claims
under terms similar to that in a health insurance policy.
-
Technically, the correlations reported are Pearson correlation
coefficients. A correlation of 0 indicates statistical independence, that is,
the existence of one violation has no effect on the likelihood of the other.
All of the correlations discussed in this section or shown in Table 10 are
statistically significant at the 1 percent level.
-
There was a 0.796 correlation between violations of HIPAA’s
look-forward and look-back rules, a 0.689 correlation between violations of
HIPAA’s individual notice and general notice, a 0.648 correlation between
violations of HIPAA’s rules governing impermissible preexisting condition
exclusions on adopted children and newborns, a 0.639 correlation between
violations of HIPAA’s creditable coverage offset rule and its look-forward
rule, a 0.623 correlation between the violations of HIPAA’s creditable
coverage offset rule and its look-back rule, a 0.516 correlation between the
violations of HIPAA’s general notice provision and the look-back rule, and a
0.504 correlation between violations of HIPAA’s general notice provisions
and the look-forward rule.
-
In one region, amendments to the policy terms of a single nationwide
issuer affected 2.55 million participants and 5,000 plans.
-
See ERISA section 502(b)(3).
-
See Private Health Insurance: Progress and Challenges in Implementing
1996 Federal Standards (GAO/HEHS-99-100, May 12, 1999).
|
|

|
|
This publication has been developed by the U.S.
Department of Labor, Employee Benefits Security Administration. It
is available to sensory impaired individuals upon request by calling:
Voice phone: 202.693.8664
TTY: 202.501.3911
|
|
This booklet constitutes a small entity compliance guide
for purposes of the Small Business Regulatory Enforcement Act of 1996.
|
| |
|



