Protecting Against Unintended Pregnancy:
A Guide to Contraceptive Choices
by Tamar Nordenberg
I am 20 and have never gone to see a doctor about birth control. My boyfriend and I have been going together for a couple of years and have been using condoms. So far, everything is fine.
Are condoms alone safe enough, or is something else safe besides the Pill?
--Letter to the Kinsey Institute for Research in Sex, Gender, and Reproduction
This young woman is not alone in her uncertainty about contraceptive options. A 1995 report by the National Academy of Sciences' Institute of Medicine, The Best Intentions: Unintended Pregnancy and the Well-being of Children and Families, attributed the high rate of unintended pregnancies in the United States, in part, to Americans' lack of knowledge about contraception. About six of every 10 pregnancies in the United States are unplanned, according to the report.
Being informed about the pros and cons of various contraceptives is important not only for preventing unintended pregnancies but also for reducing the risk of illness or death from sexually transmitted diseases (STDs), including AIDS. (See "Preventing HIV and Other STDs.")
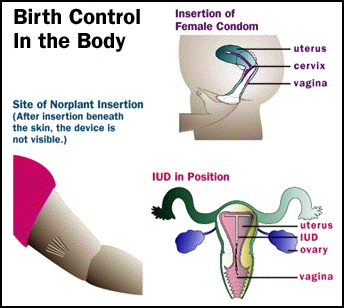 The Food and Drug Administration has approved a number of birth control methods, ranging from over-the-counter male and female condoms and vaginal spermicides to doctor-prescribed birth control pills, diaphragms, intrauterine devices (IUDs), injectable hormones, and hormonal implants. Other contraceptive options include fertility awareness and voluntary surgical sterilization.
The Food and Drug Administration has approved a number of birth control methods, ranging from over-the-counter male and female condoms and vaginal spermicides to doctor-prescribed birth control pills, diaphragms, intrauterine devices (IUDs), injectable hormones, and hormonal implants. Other contraceptive options include fertility awareness and voluntary surgical sterilization.
"On the whole, the contraceptive choices that Americans have are very safe and effective," says Dennis Barbour, former president of the Association of Reproductive Health Professionals, "but a method that is very good for one woman may be lousy for another."
The choice of birth control depends on factors such as a person's health, frequency of sexual activity, number of partners, and desire to have children in the future. Effectiveness rates, based on statistical estimates, are another key consideration. (See "Birth Control Guide.") FDA has developed a consumer-friendly table of pregnancy rates, which the agency encourages all contraceptives marketers to add to their products' labeling. Single copies of the table may be ordered from FDA, HFZ-210, 1350 Piccard Drive, Rockville, MD 20850.
Barrier Methods
Male Condom.
The male condom is a sheath placed over the erect penis before penetration, preventing pregnancy by blocking the passage of sperm.
A condom can be used only once. Some have a chemical added to kill sperm The addition of this spermicide, usually nonoxynol-9 in the United States, has
not been scientifically shown to provide additional contraceptive protection over the condom alone. Because it acts as a mechanical barrier, a condom prevents direct contact with semen, infectious genital secretions, and genital lesions and discharges.
Most condoms are made from latex rubber, while a small percentage are made from lamb intestines (sometimes called "lambskin" condoms). Condoms made from a type of plastic called polyurethane have been marketed in the United States since 1994.
Except for abstinence, latex condoms are the most effective method for reducing the risk of infection from the viruses that cause AIDS, other HIV-related illnesses, and other STDs. For people who are sensitive to latex, polyurethane condoms are a good alternative.
Some condoms are prelubricated. These lubricants do not increase birth control or STD protection. Non-oil-based lubricants, such as water or K-Y jelly, can be used with latex or lambskin condoms, but oil-based lubricants, such as petroleum jelly (Vaseline), lotions, or massage or baby oil, should not be used because they can weaken the condom and cause it to break.
Female condom.
The Reality Female Condom, approved by FDA in April 1993, consists of a lubricated polyurethane sheath shaped similarly to the male condom. The closed end, which has a flexible ring, is inserted into the vagina, while the open end remains outside, partially covering the labia.
The female condom, like the male condom, is available without a prescription and is intended for one-time use. It should not be used together with a male condom because they may slip out of place.
Diaphragm.
Available by prescription only and sized by a health professional to achieve a proper fit, the diaphragm is a dome-shaped rubber disk with a flexible rim that works in two ways to prevent pregnancy. It covers the cervix so sperm can't reach the uterus, while a spermicide cream or jelly applied to the diaphragm before insertion kills sperm.
The diaphragm protects for six hours after it is inserted. For intercourse after the six-hour period, or for repeated intercourse within this period, fresh spermicide should be placed in the vagina with the diaphragm still in place. The diaphragm should be left in place for at least six hours after the last intercourse but not for longer than a total of 24 hours because of the risk of toxic shock syndrome (TSS), a rare but potentially fatal infection. Signs and symptoms of TSS include sudden fever, stomach upset, sunburn-like rash, and a drop in blood pressure.
Cervical cap.
The cervical cap is a soft rubber cup with a round rim, sized by a health professional to fit snugly around the cervix. It is available by prescription only and, like the diaphragm, is used with spermicide cream or jelly.
It protects for 48 hours and for multiple acts of intercourse within this time. Wearing it for more than 48 hours is not recommended because of the risk, though low, of TSS. Also, with prolonged use of two or more days, the cap may cause an unpleasant vaginal odor or discharge in some women.
Sponge.
The sponge, a disk-shaped polyurethane device containing the spermicide nonoxynol-9, is not currently marketed but may be sold again in the future. Inserted into the vagina to cover the cervix, the sponge is attached to a woven polyester loop for easier removal.
The sponge protects for up to 24 hours and for multiple acts of intercourse within this time. It should be left in place for at least six hours after intercourse but should be removed no more than 30 hours after insertion because of the risk, though low, of TSS.
Vaginal Spermicides Alone
Vaginal spermicides are available in foam, cream, jelly, film, suppository, or tablet forms. All types contain a sperm-killing chemical.
Studies have not produced definitive data on how well spermicides alone prevent pregnancy, but according to the authors of Contraceptive Technology, a leading resource for contraceptive information, the failure rate for typical users may be 26 percent per year.
Package instructions must be carefully followed because some spermicide products require the couple to wait 10 minutes or more after inserting the spermicide before having sex. One dose of spermicide is usually effective for one hour. For repeated intercourse, additional spermicide must be applied. And after intercourse, the spermicide has to remain in place for at least six to eight hours to ensure that all sperm are killed. The woman should not douche or rinse the vagina during this time.
Hormonal Methods
Combined oral contraceptives.
Typically called "the pill," combined oral contraceptives have been on the market for 40 years and are the most popular form of reversible birth control in the United States. This form of birth control suppresses ovulation (the monthly release of an egg from the ovaries) by the combined actions of the hormones estrogen and progestin.
If a woman remembers to take the pill every day at the same time of day as directed, she has an extremely low chance of becoming pregnant. But the pill's effectiveness may be reduced if the woman is taking some medications, such as certain antibiotics.
Besides preventing pregnancy, the pill offers additional benefits. As stated in the labeling, the pill can make periods more regular and lighter. It also has a protective effect against pelvic inflammatory disease, an infection of the fallopian tubes or uterus that is a major cause of infertility in women, and against ovarian and endometrial cancers.
The decision whether to take the pill should be made in consultation with a health professional. Birth control pills are safe for most women--safer even than delivering a baby--but they carry some risks.
Current low-dose pills have fewer risks associated with them than earlier versions. But women over age 35 who smoke and women with certain medical conditions, such as a history of blood clots or breast or endometrial cancer, may be advised against taking the pill. The pill may contribute to cardiovascular disease, including high blood pressure, blood clots, and blockage of the arteries.
One of the biggest questions has been whether the pill increases the risk of breast cancer in past and current pill users. An international study published in the September 1996 journal Contraception concluded that women's risk of breast cancer 10 years after going off birth control pills was no higher than that of women who had never used the pill. During pill use and for the first 10 years after stopping the pill, women's risk of breast cancer was only slightly higher in pill users than non-pill users Women who have or have had breast cancer should not use the pill because the estrogen in the pill may worse their medical condition.
Side effects of the pill, which often subside after a few months' use, include nausea, headache, breast tenderness, weight gain, irregular bleeding, and depression.
Minipills.
Although taken daily like combined oral contraceptives, minipills contain only the hormone progestin and no estrogen. They work by reducing and thickening cervical mucus to prevent sperm from reaching the egg. They also keep the uterine lining from thickening, which prevents a fertilized egg from implanting in the uterus. These pills are slightly less effective than combined oral contraceptives.
Minipills, like combined oral contraceptives, can decrease menstrual bleeding and cramps and lower the risk of endometrial and ovarian cancer and pelvic inflammatory disease. Because they contain no estrogen, minipills don't present the risk of blood clots associated with estrogen in combined pills. They are a good option for new mothers who are breast-feeding, because combined oral contraceptives may decrease the quantity and quality of breast milk. They are also a good option for those who get severe headaches or high blood pressure from estrogen-containing products.
Side effects of minipills include menstrual cycle changes, weight gain, and breast tenderness.
Emergency Contraceptive ("Morning After Pill")
Two emergency contraceptive pill products have been approved by FDA for use in preventing pregnancy after intercourse when standard contraceptives have failed or when no contraceptives were used at all. One product contains the hormones progestin and estrogen; the other contains just progestin.
Available by prescription only, both products are believed to work by delaying or inhibiting ovulation, or by keeping a fertilized egg from implanting in the uterine wall. These pills are not effective once the fertilized egg has implanted.
Emergency contraceptives are about 75 percent effective, which means the number of women who would be expected to become pregnant after unprotected sex drops from eight without the "morning after pill" to two when it is used.
Side effects include nausea and vomiting, both of which were reported less frequently in women taking the progestin-only pills.
Injectable progestins.
Depo-Provera, approved by FDA in 1992, is injected by a health professional into the buttocks or arm muscle every three months. Depo-Provera prevents pregnancy in three ways: It inhibits ovulation, changes the cervical mucus to help prevent sperm from reaching the egg, and changes the uterine lining to prevent the fertilized egg from implanting in the uterus. The progestin injection is extremely effective in preventing pregnancy, in large part because it requires little effort for the woman to comply: She simply has to get an injection by a doctor once every three months.
The benefits are similar to those of the minipill and another progestin-only contraceptive, Norplant. Side effects are also similar and can include irregular or missed periods (which is not harmful and does not mean that the method isn't working), weight gain, and breast tenderness.
Implantable progestins.
Norplant, approved by FDA in 1990, and the newer Norplant 2, approved in 1996, are the third type of progestin-only contraceptive. Made up of matchstick-sized rubber rods, this contraceptive is surgically implanted under the skin of the upper arm, where it steadily releases the contraceptive steroid levonorgestrel.
The six-rod Norplant provides protection for up to five years (or until it is removed), while the two-rod Norplant 2 protects for up to three years. Norplant failures are rare, but are higher with increased body weight.
Some women may experience inflammation or infection at the site of the implant. Other side effects include menstrual cycle changes, weight gain, and breast tenderness.
Intrauterine Devices
An IUD is a mechanical device inserted into the uterus by a health-care professional. Two types of IUDs are available in the United States: the Paragard CopperT 380A and the Progestasert Progesterone T. The Paragard IUD can remain in place for 10 years, while the Progestasert IUD must be replaced every year.
It's not entirely clear how IUDs prevent pregnancy. They seem to prevent sperm and eggs from meeting by either immobilizing the sperm on their way to the fallopian tubes or changing the uterine lining so the fertilized egg cannot implant in it.
IUDs have one of the lowest failure rates of any contraceptive method. "In the population for which the IUD is appropriate--for those in a mutually monogamous, stable relationship who aren't at a high risk of infection--the IUD is a very safe and very effective method of contraception," says Lisa Rarick, M.D., former director of FDA's division of reproductive and urologic drug products.
The IUD's image suffered when the Dalkon Shield IUD was taken off the market in 1975. This IUD was associated with a high incidence of pelvic infections and infertility, and some deaths. Today, serious complications from IUDs are rare. Side effects can include pelvic inflammatory disease (an infection of a woman's reproductive organs), ectopic pregnancy (in which a fertilized egg implants in the fallopian tube instead of the uterus), perforation of the uterus, heavier-than-normal bleeding, and cramps. Complications occur most often during and immediately after insertion.
Traditional Methods
Fertility awareness.
Also known as natural family planning or periodic abstinence, fertility awareness entails not having sexual intercourse or using a barrier method of birth control on the days of a woman's menstrual cycle when she is more likely to become pregnant.
Because a sperm may live in the female's reproductive tract for up to seven days and the egg may remain fertile for about 24 hours, a woman could get pregnant from intercourse that occurred from seven dkays before ovulation to 24 hours or more after. Methods to approximate when a woman is fertile are usually based on the menstrual cycle, changes in cervical mucus, or changes in body temperature.
"Natural family planning can work," Rarick says, "but it takes an extremely motivated couple to use the method effectively."
Withdrawal.
In this method, also called coitus interruptus, the man withdraws his penis from the vagina before ejaculation. Fertilization is prevented if the sperm don't enter the vagina.
Effectiveness depends on the male's ability to withdraw before ejaculation. Also, withdrawal doesn't provide protection from STDs, including HIV. Infectious diseases can be transmitted by direct contact with surface lesions and by pre-ejaculatory fluid.
Surgical Sterilization
Surgical sterilization is a contraceptive option intended for people who don't want children in the future. It is considered permanent because reversal requires major surgery that is often unsuccessful.
Female sterilization.
Female sterilization blocks the fallopian tubes so the egg can't travel to the uterus. Sterilization is done by various surgical techniques, usually under general anesthesia.
Complications from these operations are rare and can include infection, ectopic pregnancy, hemorrhage, and problems related to the use of general anesthesia.
Male sterilization.
This procedure, called a vasectomy, involves sealing, tying or cutting a man's vas deferens, which otherwise would carry the sperm from the testicle to the penis.
Vasectomy involves a quick operation, usually under 30 minutes, with possible minor postsurgical complications, such as bleeding or infection.
Research continues on effective contraceptives that minimize side effects. One important research focus, according to FDA's Rarick, is the development of birth control methods that are both spermicidal and microbicidal to prevent not only pregnancy but also transmission of HIV and other STDs.
Tamar Nordenberg is a staff writer for FDA Consumer.
Publication No. (FDA) 00-1277
Table
of Contents |
How to Subscribe
| Back
Issues | FDA
Home Page
FDA/Office
of Public Affairs
Web page last updated by clb
2000-JUN-00.
 The Food and Drug Administration has approved a number of birth control methods, ranging from over-the-counter male and female condoms and vaginal spermicides to doctor-prescribed birth control pills, diaphragms, intrauterine devices (IUDs), injectable hormones, and hormonal implants. Other contraceptive options include fertility awareness and voluntary surgical sterilization.
The Food and Drug Administration has approved a number of birth control methods, ranging from over-the-counter male and female condoms and vaginal spermicides to doctor-prescribed birth control pills, diaphragms, intrauterine devices (IUDs), injectable hormones, and hormonal implants. Other contraceptive options include fertility awareness and voluntary surgical sterilization.