While most people would do anything to protect their children from environmental hazards, many parents would be shocked to learn that children's exposure to toxicants can be much higher than their own. Far from being "little adults," children are very different both behaviorally and physiologically. For instance, children's habit of putting things in their mouths can increase their relative exposure to environmental toxicants such as lead. Moreover, children are particularly vulnerable to toxicants and other environmental hazards because many organ systems, including the gastrointestinal, central nervous, immune, and reproductive systems, are still developing after birth. In general, the younger the child, the greater any potential health effects.
Despite differences in behavior and physiology between children and adults, few studies have focused on the effects of these differences on risks to children's health of environmental exposures. "Children are not routinely included in risk assessment processes, and most environmental regulations are based on exposure data of adult males," write Joy Carlson and Katie Sokoloff of the Children's Environmental Health Network in the 1995 Environmental Health Perspectives Supplement on child health.
The lack of studies notwithstanding, there are indicators that children's environmental health may be declining. Asthma in children has increased by more than a third over the past 15 years, afflicting an estimated 4.2 million children under the age of 18 nationwide, according to the American Lung Association (ALA). "Asthma is now the leading cause of admissions to hospitals in children. It's reached epidemic proportions," says Philip Landrigan, professor of community medicine at the Mount Sinai Medical Center in New York, who authored the 1994 book Raising Children Toxic Free with Herbert Needleman, professor of child psychiatry and pediatrics at the University of Pittsburgh School of Medicine. Similarly, the rates of the two most common childhood cancers have increased significantly over the past 15 years: acute lymphocytic leukemia is up more than 10% and brain tumors are up more than 30%. While these increases may in part reflect better diagnoses, environmental hazards such as air pollution, pesticides, and industrial chemicals are also likely to play a role.

Lead
Lead is considered by many to be the greatest environmental health threat to children in the United States, especially along the eastern seaboard and in the midwest. While adults absorb about 10% of the lead they ingest, children's less mature digestive systems can absorb as much as 50% because lead resembles calcium and children's gastrointestinal tracts take up calcium at greater rates than adults'. Young children's nervous systems are particularly susceptible to detrimental effects of lead because the "blood-brain barrier" (which protects the brain from many substances) is not completely functional until three years of age, a period when neurons are still migrating and synapses are still forming.
While high levels of lead can cause mental retardation and even death, most of the lead poisoning in U.S. children is at levels so low that it goes undetected because there are no overt symptoms. "The effects typically don't manifest until school age. [Lead-poisoned] children have attention deficits, decreased hearing, and increased impulsivity, all of which can lead to difficulty in learning," says Janet Phoenix, manager of public health programs at the National Lead Information Center in Washington D.C.
These neurological effects are seen at blood lead levels near 10 micrograms per deciliter (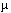 g/dl), which the Centers for Disease Control classifies as a "level of concern." Moreover, decreases in IQ and growth can occur even below 10
g/dl), which the Centers for Disease Control classifies as a "level of concern." Moreover, decreases in IQ and growth can occur even below 10 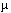 g/dl, according to the 1992 report Lead Toxicity by the Agency for Toxic Substances and Disease Registry (ATSDR) in Atlanta. In fact, no minimum level for lead toxicity has been identified, according to the 1993 American Academy of Pediatrics report Lead Poisoning: From Screening to Primary Prevention.
g/dl, according to the 1992 report Lead Toxicity by the Agency for Toxic Substances and Disease Registry (ATSDR) in Atlanta. In fact, no minimum level for lead toxicity has been identified, according to the 1993 American Academy of Pediatrics report Lead Poisoning: From Screening to Primary Prevention.
 |
| Source: Adapted from ATSDR, Toxicological Profile for Lead 1989 |
Three to four million U.S. children (17% of all children) had blood lead levels above 15 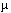 g/dl in 1989, according to the ATSDR report. "Most parents are not aware that lead is still a problem," says Maurci Jackson of United Parents Against Lead. "Our children are used as the lead detectors. We've got to reverse that and put the emphasis on prevention just as we do with immunizations. Lead testing needs to be standard for all children across the country."
g/dl in 1989, according to the ATSDR report. "Most parents are not aware that lead is still a problem," says Maurci Jackson of United Parents Against Lead. "Our children are used as the lead detectors. We've got to reverse that and put the emphasis on prevention just as we do with immunizations. Lead testing needs to be standard for all children across the country."
The main source of lead poisoning in children is old lead-based paint. Prior to 1955, much of the white interior paint in the country was half lead and half linseed oil--a durable but toxic combination. While lead-based paint was banned in the United States in 1971, the EPA estimates that more than three quarters of the homes in the United States still contain some. Children can be exposed to lead by eating chips that fall off the walls as the paint ages, by chewing on painted cribs, or by breathing dust when paint is sanded off walls during renovation.
Other sources of this toxicant include drinking water from lead-soldered plumbing and soil that contains lead residues from motor vehicle exhaust. Cultural practices can also expose children to lead. For example, the traditional pottery made by Hispanic people in the southwest United States, as well as much imported pottery, is fired at temperatures too low to fix the lead in the pigments, and kohl, a southeast Asian folk remedy that is applied around the eye, can be 80% lead.

Air Pollution
While lead is the major environmental hazard to children in much of the United States, air pollution may pose an even greater threat to children in urban areas. Children are more vulnerable to air pollution in part because lungs continue to develop throughout childhood, adding new alveoli until about age 20. Damage from air pollution can impede lung development and may lead to chronic lung disease later in life, according to the ALA's 1995 report Danger Zones: Ozone Air Pollution and Our Children.
Children's exposures to air pollution are likely to be much greater than adults' for several reasons. Due to their higher metabolic rates, children need more oxygen and therefore breathe more air--twice as much air per pound of body weight compared to adults. In addition, children often play outside on warm, sunny afternoons, which is when ozone levels peak. Children also breathe air closer to the ground, where respirable particles settle, and can be so much more active that they breathe air pollutants deeper into their lungs than adults.
The ozone and particulate air pollution that children breathe comes primarily from motor vehicles. Ozone can damage the cells that line the respiratory tract, making airways narrower and causing wheezing, chest pain, bronchitis, and asthma. These effects are greater in children because their airways are narrower than those of adults. Ozone can also decrease resistance to respiratory infection, make airways more sensitive to airborne allergens, and act synergistically with airborne acidity to damage deep lung tissues, according to the 1993 American Academy of Pediatrics' report Ambient Air Pollution: Respiratory Hazards to Children. While the federal standard for ozone is 120 parts per billion averaged over an hour, wheezing and other symptoms can occur at exposures to lower levels over longer periods of time, according to the ALA.
Besides diesel vehicle and car exhaust, sources of particulate air pollution include wood fires and factory and utility smokestacks. Particulate air pollution comprises solid and liquid particles less than 10 microns in diameter. Particles this small can be inhaled deep into the lungs, causing wheezing and coughing, and triggering asthma attacks, and are also associated with pleurisy and pneumonia. Symptoms can occur below the federal standard of 150 micrograms per cubic meter, according to Landrigan.
While there have been no direct studies of the effects of air pollution on children, autopsies of 100 Los Angeles children who died for unrelated reasons in 1990 revealed that more than 80% had subclinical lung damage, says spokesman Jerry Martin of the California Air Resources Board. "We're pretty certain that the only thing they had in common was living in polluted air," he says. This pilot study led to an ongoing, long-term study to determine the effects on developing lung tissues of growing up in polluted air.

Pesticides on Food
Besides having greater exposures to lead and air pollution compared to adults living in the same environment, children can also be exposed to greater amounts of pesticides because they generally eat much more of certain foods than adults do.
For example, children eat up to seven times more apples, bananas, grapes, pears, and carrots in proportion to their body weight. Standards for food pesticide levels are inadequate for protecting children because they are based on adult exposures, says Landrigan, who chaired the National Academy of Sciences committee that authored the 1993 study Pesticides in the Diets of Infants and Children. The report called for new pesticide residue standards that reflect the critical differences in children's diet and physiology. "We agree with the general thrust of the [NAS] recommendations but the methods are not necessarily available," says John McCarthy, vice president for scientific and regulatory affairs of the Washington, D.C.-based American Crop Protection Association.
Children of farmworkers are probably exposed to the highest levels of pesticides used on food but there are no good studies showing this, says Valerie Wilk, a health specialist with the Farmworker Justice Fund in Washington, D.C. "Temporary housing is right on the fields and the concentration of pesticides inside them is high. And most often the whole family is out in the fields and the kids are crawling around in pesticide-contaminated soil," she says. A recent pilot study by the California Department of Health suggested that agricultural pesticide levels are indeed elevated in houses within a quarter mile of fields, according to Lawrie Mott of the Natural Resources Defense Council in San Francisco. McCarthy agrees that pesticide exposures of farmworkers is a problem. "We are champions of the 1992 EPA worker protection standards," he says. "For example, we are helping to train and educate farmworkers--those who plant and harvest the crops--and pesticide applicators."



Pesticides Used in the Home
For most children, however, pesticides used in the home and yard may pose a greater threat than pesticide residues on food. Compared to adults, children can be exposed to higher levels of pesticides in flea bombs, pest strips, herbicides, and other pesticides used at home because they are more likely to play on floors and lawns. For example, after flea bombs are used, concentrations of the insecticide Dursban (chlorpyrifos) are much higher one foot above the floor, where babies play, than six feet above the floor, where adults breathe. The EPA estimates that 84% of U.S. households use pesticides. Unfortunately, there are no regulations for home pesticide use, says Landrigan. For example, the highly toxic organophosphate pesticide diazinon (Spectocide) is allowed for use in homes and by commercial lawn care companies but is banned for use on golf courses, corn, and alfalfa fields, he says.
While several studies have suggested that home exposure to pesticides can cause brain cancer and leukemia in children, the results are not conclusive. "There are no data on children [and pesticides] period," says Sandra Schubert, program director of the National Coalition Against the Misuse of Pesticides in Washington, DC. "Until recently there has been no concerted effort to look at children's issues. Half of the problem is lack of education--people assume that if the EPA approved a product, then it's safe." Wendy Gordon, executive director of Mothers and Others for a Livable Planet, an advocacy group for children's health issues, agrees: "At the federal level, the laws are very protective. But when the laws are translated into regulations, they are designed to protect industry. Chemicals are innocent until proven guilty."

Endocrine Disrupters
There is rising concern that DDT and its metabolites, some PCBs, and a host of other compounds can disrupt the endocrine system and thus have disastrous effects on sexual development and reproduction. The DDT metabolite DDE, for instance, mimics the effects of estrogen by binding to the hormone's receptors. In wildlife from salmon to alligators and eagles to whales, endocrine disrupters are associated with reproductive effects such as decreased fertility, feminization of males, and masculinization of females. "The evidence is pretty good for wildlife but is less clear for people--it's all epidemiological," says Michael Fry of the Department of Avian Sciences at the University of California at Davis, who is a member of a National Academy of Sciences panel reviewing data on the effects of endocrine disrupters on wildlife and people. "People are exposed to such a wide range of toxins that it's hard to show a cause," says Schubert. "But endocrine disrupters are particularly scary because people have found parallels between wildlife and the human population."
While DDT and PCBs have been banned in the United States for about 20 years, they are still used extensively in developing countries and are widespread in the environment. In addition, the DDT analogues dicofol, kelthane, and methoxychlor, as well as many other endocrine-disrupting compounds, are currently used in the United States. In light of the effects of endocrine disrupters on wildlife, Theo Colborn of the World Wildlife Fund in Washington D.C. calls for reexamining the endocrinological effects of new and currently used pesticides. Colborn says that most tests assess only acute toxicity, carcinogenicity, or mutagenicity, and that we need to do, for example, in vitro assays for hormone receptor binding. "We respectfully disagree," says the American Crop Protection Association's McCarthy. "The current routine testing required for pesticides is good enough." Others suggest getting rid of endocrine-disrupting compounds entirely. "We think we know enough about many of these compounds to ban them," says Monica Moore, program director of the Pesticide Action Network's North American Regional Center in San Francisco.

Hazardous Waste
There are an estimated 30,000- 40,000 hazardous waste sites in the United States, according to Jeffrey Lybarger, director of health studies at the ATSDR. Nearly 1,300 of these are Superfund sites, 42% of which are landfills or waste storage/treatment facilities, 31% are abandoned manufacturing facilities, 8% are waste recycling facilities, 5% are mining sites, and 4% are government properties, according to a 1995 Chemosphere article by Assistant Surgeon General Barry Johnson. To date, more than 2,000 toxicants have been identified at Superfund sites, and 275 of these are ATSDR/EPA priority substances--those that pose the greatest health risks. Lead is ranked first on the list, PCBs are seventh, and DDT is twelfth.
Hazardous waste sites are largely uncharacterized. "We don't know the extent of the contamination so we can't assess the health risk," says Lybarger. But, he says, children's behavior makes them more at risk for increased exposure to hazardous waste because they play outside more, play in dirt, and are curious. "They may play in an abandoned drum," he says. "They may not have the wisdom to leave it alone."
The many epidemiological studies of the adverse health effects of hazardous waste sites have been inconclusive. But while the overall impact of hazardous waste is unknown, investigations at specific sites have documented symptoms ranging from headaches and neurobehavioral problems to cardiac anomalies and cancer, according to a 1993 NRC review Environmental Epidemiology: Public Health and Hazardous Wastes. The EPA ranks Superfund sites eighth on their list of the top 29 environmental causes of cancer. "Although the hazard posed by an individual site to public health and ecosystems remains somewhat controversial, the evidence is mounting that many sites do present a hazard to human health because of releases of contaminants into groundwater and other environmental media," writes Assistant Surgeon General Johnson.

Radiation
Radiation can have devastating effects on children. While very high doses can cause blindness, intractable bloody diarrhea, and death, lower doses have more subtle effects such as genetic mutations, hematopoetic disorders, and cancer. A 1990 NAS report concluded that there are no safe levels of radiation. The younger the child and the greater the radiation dose, the greater the risk of cancer. Studies of atomic bomb survivors show that children who were under the age of 20 when exposed to the radiation were at greater risk of developing cancer. Similarly, atomic bomb survivors who had received heavier doses were more likely to develop leukemia. Repeated exposure to X-rays can cause a wide range of childhood cancers including brain cancer, leukemia, lung cancer, and thyroid cancer.
Historically, Department of Energy nuclear weapons manufacturing facilities released radioactive compounds into the environment, which may have affected children living nearby. For example, from the mid-1940s to the mid-1950s, the Hanford nuclear weapons manufacturing facility in eastern Washington released radioactive iodine into the air; the facility was closed in the late 1980s. "A lot of radiation was released--700,000 curies total--and native Americans were potentially affected by the radiation," says Michael Sage, deputy chief of radiation studies at the National Center for Environmental Health in Atlanta. The CDC is three years into a study of whether people in the Yakima and Umatilla Nations who lived near the site during the time of the releases have higher incidences of thyroid diseases such as hypothyroidism, hyperthyroidism, and cancer.
Commercial nuclear power plants are safer than DOE facilities on a day-to-day basis in part because the reactors are newer and do not produce nuclear material. "The big issue is potential accidents like Three Mile Island," says Sage. Landrigan adds that nuclear waste is the greatest long-term risk of nuclear power generation, pointing out that we have yet to find a safe disposal method.
Today some argue that the most significant source of radiation exposure in children is radon, a gas produced from uranium-rich soils. Radon seeps into houses through cracks in basements and gaps around pipes. Radon breaks down into radioactive particles that can be retained in the lungs. While there have been no studies in children, studies have shown that radon can cause lung cancer in miners. Residential exposure to radon may account for 13,000 lung cancer deaths per year, according to the 1989 American Academy of Pediatrics report Radon Exposure: a Hazard to Children. Children are at greater risk for radon exposure because they breathe more per body weight and are closer to the floor, where radon breakdown products accumulate. Compared to an adult, a six-month old baby will receive about twice the radon exposure per body weight.

EMFs
There is no consensus on the effects of electric and magnetic fields (EMFs) on children's health. Four out of 14 studies suggest that there is a link between proximity to power lines and childhood cancers such as leukemia, according to the 1995 NIEHS/DOE booklet Questions and Answers About EMF: Electric and Magnetic Fields Associated with the Use of Electric Power. One of the studies suggests that living within 130 feet of high-current power lines may increase children's risk of leukemia several fold. "Some studies have shown risks, some haven't. The studies that have [shown risk] are convincing enough that we can't say there's no risk--but it's probably not that great," says Anne Mellinger, medical epidemiologist at the National Center for Environmental Health's Radiation Studies Branch.

Poor and Minority Children
While all children are vulnerable to environmental hazards, poor and minority children are particularly at risk because they tend to live in less healthy environments. For example, poor and minority children are more likely to be exposed to pesticides used on crops because more than 70% of seasonal farmworkers are Hispanic, according to the EHP Supplement on child health. And the areas with three of the five largest hazardous waste sites nationwide have twice as many people of color as areas without such sites, says Jerry Poje, director of minority health programs at the NIEHS.
Although children's average blood lead levels are down nationwide, there has been no such decrease in minority populations, says Poje. Of the several million U.S. children with lead poisoning, 55% are poor and black while 26% are poor and white, according to the 1989 ATSDR report on lead toxicity. Poor and minority children are more likely to be exposed to higher levels of lead because low-income housing tends to be poorly maintained and more likely to have old, peeling paint. To make matters worse, poor children can absorb lead more readily because their diets can be deficient in protein, calcium, iron, and zinc.
Poor and minority children are also at greater risk for exposure to air pollution in part because ozone and particulates from motor vehicles are concentrated in inner cities. The ALA estimates that 69% of Hispanics, 67% of Asian-Americans, 61% of blacks, and 51% of whites live in areas where ozone levels exceed the EPA standard.
While there are many reasons to be concerned about children's environmental health, "environmental diseases are in part the result of personal and collective choices in the way we live, in the way we consume our resources, and dispose of our waste products, "write Landrigan and Needleman. "There is cause for optimism in this observation. If a disease is made by human beings, we should be able to prevent it." As a nation, preventing disease in our children is the only way to protect our future.

Robin Meadows
[
Table of Contents]
Last Update: May 7, 1997





