doi: 10.1161/CIRCULATIONAHA.105.566737
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
(Circulation. 2006;113:e51-e52.)
© 2006 American Heart Association, Inc.
Cardiology Patient Page |
On-Pump and Off-Pump Coronary Artery Bypass Grafting
From the Division of Cardiac Surgery, Brigham and Women’s Hospital, Boston, Mass.
Correspondence to Dr P.S. Shekar, MD, Division of Cardiac Surgery, Brigham and Women’s Hospital, 75 Francis St, Boston MA 02115. E-mail pshekar{at}partners.org
Surgery for coronary artery disease is known as coronary artery bypass grafting (CABG). It was one of the landmark operations in the history of cardiac surgery that rescued millions of people afflicted by coronary artery disease. It was first performed by Kolesov,1 was popularized by Favaloro,2 and is still the leading heart operation performed today.
Current reasons for performing CABG are the presence of 3-vessel disease (all the 3 major arteries to the heart are blocked), left main coronary artery disease (the main artery itself is critically narrowed), and 3-vessel disease in diabetics. It also is used for patients with severely depressed heart function and for patients who need surgery for heart conditions in addition to coronary artery disease (such as replacement of valves or reconstruction of the heart muscle).
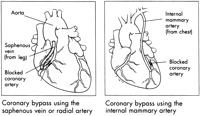
Similar to a detour on a highway in the setting of a roadblock, CABG involves the strategic placement of bypass grafts that will provide an alternative route for the blood to flow around the blockage (Figure). These bypass grafts are composed of other arteries and veins from the body of the patient that are harvested only when they are numerous in their location or their function in their primary location can be safely and effectively taken over by another vein or artery alongside it. These grafts are sewn onto a source of blood supply, most commonly the aorta (the large vessel that arises from the heart), and then in turn onto the coronary artery in a location beyond the blockage. The exact location of the graft attachment on the coronary artery does not have to be precise because blood will flow in both directions. Most bypass grafts are sewn by hand using fine sutures on fine needles and magnification.
|
There are 2 different methods of doing CABG: the traditional way, which is called the on-pump CABG, and the newer way, which is called the off-pump CABG. Opinion is still divided on which is the better way. Although a variety of new access options exist, most CABGs are performed via the midline sternotomy approach (down the middle through the breast bone).
On-pump CABG is a time-honored procedure that is performed while the heart is stopped. The blood supply must be provided to the rest of the body when the heart is stopped. Therefore, surgeons use the cardiopulmonary bypass machine (also known as the heart-lung machine or the pump), an artificial circulation system that does the work of the heart and the lungs. Pipes (cannulas) are placed in the heart to drain impure blood to the pump, where it is purified and pumped back into the patient. Thus, the heart can be safely stopped with specialized medications that not only keep it stopped but also nourish it when it is still. The bypass grafts are then constructed. At the end of the procedure, the heart is restarted. When it resumes adequate function, the cardiopulmonary bypass machine is disconnected after the pipes are withdrawn from the heart. On-pump CABG today is a safe procedure that has a small risk of death and/or complications. The average risk of this procedure to a low-risk patient is 1% to 2%. The patient’s other health-threatening conditions increase these risks. Some of the important complications that can occur with this technique are stroke, kidney or liver failure, decrease in higher mental function, and bleeding. These complications have been ascribed to the use of the pump and the need to manipulate both the heart and the large arteries to place the patient on the system. Development of new technology has made the heart-lung machine very safe. Surgeons have understood the various reasons for complications and have learned to identify them and to take necessary precautions.3 The bypass grafts constructed on a heart that has been temporarily stopped with the on-pump CABG technique are known to be complete4 and superior to alternative techniques.
Off-pump CABG is considered the newer method of performing CABG. The complications of on-pump CABG, especially stroke and decrease in higher mental function, spurred the development of this technique. This procedure is performed with the heart beating and without the use of the heart-lung machine. While definitely eliminating the placement of special pipes for the machine, use of artificial circulation, and excessive manipulation of the aorta, this technique introduces a new complexity of attaching grafts to the heart while it is constantly moving and filled with blood, a situation similar to threading a needle on a rocking boat. Special devices can mechanically stabilize the relevant part of the heart so that the suturing can be performed on a relatively immobile platform.5 There have been concerns that poor grafting technique could result from constant motion that can jeopardize the quality of these grafts. However, surgeons who have adapted and perfected this technique have excellent results.6,7 Even in experienced hands, the risk of death and/or complications from off-pump CABG is also about 1% to 2% in a low-risk patient. Nevertheless, this is a highly specialized procedure currently performed by some experienced surgeons with good results. The proposed benefits of this procedure such as a lower risk of stroke, neurocognitive dysfunction, organ dysfunction, and atrial fibrillation have not been confirmed by large clinical trials.8
Of the 2 techniques, on-pump CABG is the oldest and time-honored method. Advances in technology allow on-pump CABG to be performed with very low mortality and morbidity and with excellent results. It is still the most widely used technique. Off-pump CABG is a newer technique with the proposed benefit of lower complication rates. It is a highly specialized technique that has good results in the hands of surgeons who perform this surgery regularly. The choice of procedure should depend on the comfort level of the surgeon performing the procedure on a particular patient because the 2 procedures seem equally effective.
| Disclosures |
|---|
|
|
|---|
None.
Additional Resources
- The Society of Thoracic Surgeons. CABG information. Available at: http://www.sts.org/sections/patientinformation/adultcardiacsurgery/cabg/index.html. Accessed January 5, 2006.
- MedicineNet, Inc. Coronary artery bypass graft center. Available at: http://www.medicinenet.com/coronary_artery_bypass_graft/index.htm. Accessed January 5, 2006.
- National Library of Medicine. Heart bypass surgery. Available at: http://www.nlm.nih.gov/medlineplus/heartbypasssurgery.html. Accessed January 5, 2006.
- MedicineNet, Inc. Coronary artery bypass graft center. Available at: http://www.medicinenet.com/coronary_artery_bypass_graft/index.htm. Accessed January 5, 2006.
| Footnotes |
|---|
The information contained in this Circulation Cardiology Patient Page is not a substitute for medical advice, and the American Heart Association recommends consultation with your doctor or healthcare professional.
| References |
|---|
|
|
|---|
- Kolesov VI. Mammary artery-coronary artery anastomosis as a method of treatment of angina pectoris. J Thorac Cardiovasc Surg. 1967; 54: 535–544.[Medline]
[Order article via Infotrieve]
- Favaloro RG. Saphenous vein autograft replacement of severe segmental coronary artery occlusion: operative technique. Ann Thorac Surg. 1968; 5: 334–339.[Medline]
[Order article via Infotrieve]
- Schachner T, Zimmer A, Nagele G, Laufer G, Bonatti J. Risk factors for late stroke after coronary artery bypass grafting. J Thorac Cardiovasc Surg. 2005; 130: 485–490.
[Abstract/Free Full Text] - Czerny M, Baumer H, Kilo J, Zuckermann A, Grubhofer G, Chevtchik O, Wolner E, Grimm M. Complete revascularization in coronary artery bypass grafting with and without cardiopulmonary bypass. Ann Thorac Surg. 2001; 71: 165–169.
[Abstract/Free Full Text] - Detter C, Deuse T, Christ F, Boehm DH, Reichenspurner H, Reichart B. Comparison of two stabilizer concepts for off-pump coronary artery bypass grafting. Ann Thorac Surg. 2002; 74: 497–501.
[Abstract/Free Full Text] - Puskas JD, Williams WH, Mahoney EM, Huber PR, Block PC, Duke PG, Staples JR, Glas KE, Marshall JJ, Leimbach ME, McCall SA, Petersen RJ, Bailey DE, Weintraub WS, Guyton RA. Off-pump vs. conventional coronary artery bypass grafting: early and 1-year graft patency, cost, and quality-of-life outcomes: a randomized trial. JAMA. 2004; 291: 1841–1849.
[Abstract/Free Full Text] - Puskas JD, Williams WH, Duke PG, Staples JR, Glas KE, Marshall JJ, Leimbach M, Huber P, Garas S, Sammons BH, McCall SA, Petersen RJ, Bailey DE, Chu H, Mahoney EM, Weintraub WS, Guyton RA. Off-pump coronary artery bypass grafting provides complete revascularization with reduced myocardial injury, transfusion requirements, and length of stay: a prospective randomized comparison of two hundred unselected patients undergoing off-pump versus conventional coronary artery bypass grafting. J Thorac Cardiovasc Surg. 2003; 125: 797–808.
[Abstract/Free Full Text] - Ehsan A, Shekar P, Aranki S. Innovative surgical strategies: minimally invasive CABG and off-pump CABG. Curr Treat Options Cardiovasc Med. 2004; 6: 43–51.[Medline]
[Order article via Infotrieve]
Related Article:
-
Issue Highlights
Circulation 2006 113: 463.[Extract] [Full Text]
This article has been cited by other articles:
 |
A. F. Marple, E. M. Antman, and M. M. Hand Modern Treatment for Heart Attacks: Opening Blocked Arteries Quickly Circulation, November 14, 2006; 114(20): e578 - e580. [Full Text] [PDF] |
||||
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||