|
Cancer is a renegade system of growth inside the human body. The changes that must occur inside
for cancer to flourish are genetic changes, but factors outside the body also play a role.
Humans do not exist in contaminant-free surroundings. Over a lifetime, a person's internal genetic
makeup persistently interacts with external factors. Factors outside the body such as diet,
smoking, alcohol use, hormone levels, or exposures to certain viruses and cancer-linked chemicals
(carcinogens) over time may collectively conspire with internal genetic mutations to destabilize
normal checks and balances on growth and maturation. (Please see
Understanding Cancer for
more information.)

 |
When most people think of the word "environment," they think of forests, oceans, or mountains.
In cancer research, however, scientists define the environment as everything outside the body that
enters and interacts with it. This interaction is called an exposure. So, environmental exposures
can include such factors as sunshine, radiation, hormones, viruses, bacteria, and chemicals in the
air, water, food, and workplace, as well as lifestyle choices like cigarette smoking, excessive
alcohol consumption (more than 2 drinks/day), an unhealthful diet, lack of exercise, or sexual
behavior that increases one's exposure.
Researchers have estimated that as many as 2 in 3 cases of cancer (67 percent) are linked to some
type of environmental factor, including use--or abuse--of tobacco, alcohol, and food, as well as
exposures to radiation, infectious agents, and substances in the air, water, and soil.

The good news is that the major environmental factors that are linked to cancer deaths can be
modified, because most of them involve lifestyle choices. Almost one-third of all cancer deaths
could be prevented by eliminating the use of tobacco products, for example, and making better
dietary choices could prevent many more premature deaths from this disease. Our knowledge and
certainty about diet is much less firm than it is for tobacco. Diets are very complex and we need to
know what people ate in the past that impacted their cancer diagnoses today.

The environment influences cancer rates and risks. We can see this by comparing cancer rates in
different countries, and how rates change when people move from one country to another.
For example, U.S.-born Japanese men have twice the rate of colon cancer as native-born Japanese
men, and U.S.-born Japanese women have colon cancer rates 40 percent higher than their
counterparts born in Japan. So scientists study what exposures or characteristics differ between
Japanese immigrants and their descendants in the U.S. to better understand the environmental
factors that may be influencing their colon cancer rates and risks.

Certain types of exposures are linked to specific cancers. For example, exposure to asbestos is
linked to lung cancer, and exposure to benzidine (a chemical found in some dyes) is linked to
bladder cancer. Exposure to carcinogens from tobacco use is linked to several types of cancer,
including cancers of the lung, bladder, mouth, lip, throat, voice box, and esophagus.

 |
Of course, environmental exposures by themselves do not cause cancer. Cancer is complex and
involves many gene-gene interactions that occur inside you and are not well understood. For
example, certain randomly occurring gene changes may be accumulating in your body's cells right
now. And these same kinds of changes may not be occurring in your friends, your coworkers, or
even your family members, even though all of you remain in a similar environment most of the
time. Over your lifetime, random gene changes are passed along as your body cells grow and
divide, so they accumulate. The unique patterns that evolve over time may make some people more
likely than others to increase their risk for cancer after exposure to a particular chemical or after
choosing a particular behavior.

 |
You might wonder why some families are more cancer prone than others. In part, inheritance is involved in some of these cases. This is because, at birth, some offspring unknowingly inherit gene changes that can make them more susceptible to cancer. But this explains only a very small percent of new cancer cases, no more than 5 percent.
Others factors that may change your cancer risk include having stronger or weaker immune systems, variations in detoxifying enzymes or repair genes, or differences in hormone levels.

Rarely, several generations of the same family will develop the same type of cancer at rates much
higher than those that occur in the population overall. Often, the family members are passing on
mutated genes that impart a higher than average risk for developing this particular cancer. By
studying the genetic profiles of these affected families, researchers are learning which genes are
involved in cancer's development. Kidney cancer families are a good example of this. When
scientists discovered the gene changes involved in the inherited form of renal cancer, they were
able to use this information to better detect and diagnose sporadic or randomly occurring new
cases of this cancer type.
Only about 2 to 5 percent of cancers run in families this way.

Some families will exhibit higher than average rates of a particular cancer, yet when scientists
search their genomes, they are unable to find the usual genomic alterations suspected of increasing
cancer risk. These cases seem to point to gaps in our understanding of the full set of mutations
required for cancer's development. They also prompt researchers to probe deeper in search of
possible environmental exposures suffered by the clan collectively.

Normally, if environmental exposures cause an unwanted molecule to bind to a gene, excision
repair proteins rapidly remove that damaged area of the gene. Because the genes in the body that
produce these repair proteins can themselves have mutations, people can differ from one to
another in their gene repair activities. Unfortunately, genetic variations can make a person's gene
repair activities less efficient or more error-prone than normal, and this faulty condition can be
passed from generation to generation.

 |
Other genes in the body produce detoxifying proteins that prepare toxic molecules for quick
removal. Again, genetic variation in genes for detoxifying proteins can result in differences from
one person to another in the ability to eliminate cancer-causing compounds. On the other hand,
some genetic variation may actually produce hyperactive detoxifying gene activity. Then a person
who possesses hyperactive detoxifying proteins may have some protection from harmful
environmental exposures. Scientists believe, for example, that some persons inherit genes for
hyperactive detoxifier proteins in lung tissues. This inheritance may partly explain why some
smokers who refuse to give up the habit can still remain free of cancer. (For more information,
please see Genetic Variation.)

 |
We know that some exposures increase the risk of cancer, but we don't know which specific
combinations of environmental factors on the outside of the body combine with gene changes on
the inside to lead to cancer. We don't know why two persons can have very similar environmental
exposures, yet one gets cancer and the other does not. A number of individual factors are involved
and there are complex relationships among them.
The individual chance that someone will develop cancer in response to a particular, single
environmental exposure depends on how long and how often that person was exposed. It also
depends on the person's:
- exposures to certain environmental factors (including diet, hormones)
- genetic makeup
- age and gender

Every two years, the Federal Government publishes a report on environmental exposures that
have been linked to cancer. The most recent report included more than 220 substances. It helps to
understand which of these exposures have the most impact on the general public.
As you consider these factors one at a time, it is important to remember that an individual
accumulates a unique set of responses to his or her unique environment over a lifetime. Lengths
and strengths of exposures will vary, and the person's genome itself will change.

Cigarette, cigar, and pipe smoking have been linked to more than a dozen types of cancer,
including lung, mouth, bladder, colon, and kidney cancers. Chewing tobacco and snuff increase
the risk of oral cancer, and second-hand smoke increases the risk of lung cancer.

Smoking is the single most common cause of cancer, and exposure to cancer-causing substances
in tobacco products accounts for about 30 percent of cancer deaths in the United States. To reduce
your cancer risk, don't smoke or use tobacco products. Avoid smoke-filled rooms if possible.

Alcohol is another risk factor. Heavy drinkers have an increased risk of cancers of the mouth,
throat, liver, voice box, and esophagus. There is also some evidence for an increased risk of breast
cancer. Drinkers who also smoke may have an even higher risk of some oral and throat cancers.
Drink in moderation, if at all: no more than one or two drinks per day.

Being overweight is an important lifestyle factor related to cancer risk. There are links between
obesity and the risks of breast cancer (in older women), endometrial cancer, and cancers of the
kidney, colon, and esophagus. Not being physically active increases the risk of colorectal and
breast cancers.
Together, obesity and physical inactivity are linked to about 30 percent of the cases of colon,
endometrial, kidney, and esophageal cancers, as well as 30 percent of breast cancers in older
women.
Losing weight and exercising can help reduce your risk. Exercise at least 30 minutes a day, most
days of the week. Exercise alone can decrease the risk of colon cancer and breast cancer. The goal
should be for adults age 20 or older to keep their Body Mass Index (BMI) below 25. The BMI is
a number that shows your body weight adjusted for your height.

The federal report on carcinogens doesn't discuss specific foods and cancer risk. However,
studies show that consuming large quantities of red meat, preserved meats, salt-preserved meats,
and salt probably increases the risk of stomach and colorectal cancers. Research also shows that a
diet high in fruits and vegetables may decrease the risks of these cancers. And calorie restriction
has been shown to reduce cancer risk for several cancer types.
Eat a healthy calorie-restricted diet rich in whole grains, fruits, and vegetables. Avoid consuming
large amounts of fatty foods, red meats, salt, or salt-preserved food.

Some viruses are risk factors for cancer.
Human Papillomavirus
Certain strains of human papillomavirus (HPV), which are sexually transmitted, are the primary
causes of cervical and anal cancer. Women who begin having sexual intercourse before age 17, or
who have multiple sexual partners, are at greatest risk of HPV infection.
HPV may also be responsible for some cancers of the head and neck.
It's important to note that most people infected with HPV will not get cancer. Also, a vaccine is
now available that can prevent infection with the strains of HPV that cause cervical cancer.
Hepatitis B and C
The hepatitis B and hepatitis C viruses are major causes of liver cancer worldwide. The viruses are
transmitted through blood transfusions, injectable drug use, and unprotected sex. Vaccinations can
protect against hepatitis B, but there is not yet a vaccine for hepatitis C.

Epstein-Barr virus causes mononucleosis. In people with weakened immune systems, it can also
lead to some types of lymphoma.
People with weakened immune systems may also be at risk for a cancer called Kaposi's sarcoma
if they are infected with human herpesvirus 8 (also known as Kaposi's sarcoma-associated
herpesvirus, or KSHV). In the United States, KSHV infection is most common in homosexual
men.

A bacterium called Helicobacter pylori (H. pylori) is the primary cause of stomach ulcers and
inflammation of the stomach. H. pylori can contribute to the development of stomach cancer, but
most infections lead to neither symptoms nor cancer.

Ultraviolet radiation--which comes from natural sunlight, sunlamps, or tanning beds--can lead to
melanoma and other forms of skin cancer. While some sun exposure is good for health, excessive
exposure during childhood seems a particularly important factor that increases skin cancer risk,
and repeated exposure as an adult can increase risk as well.
If possible, avoid sun exposure between 10 am and 4 pm. Wear protective clothing and use
sunscreen. Do not use tanning beds or other types of artificial UV exposure.

Invisible high-energy rays called ionizing radiation can damage the body's DNA and genes,
possibly enabling cancer-related mutations. There are several sources of ionizing radiation,
including cosmic rays, radon, fallout from atomic bombs or above-ground nuclear testing, and
screening or diagnostic X-rays.
We are all exposed to the ionizing radiation from the cosmic rays that enter earth's atmosphere
from outer space. This radiation may account for a very small percentage (about 1 percent) of our
total cancer risk.

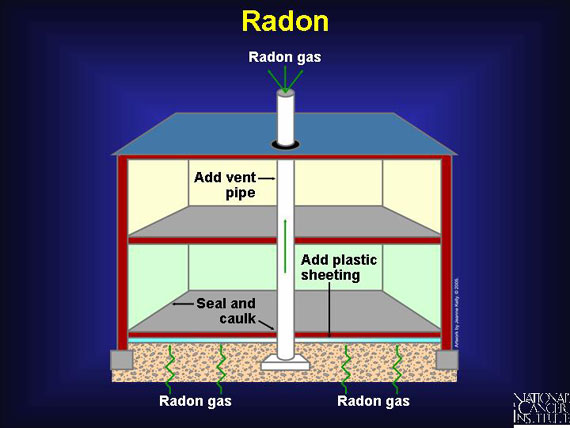
Radon, a naturally occurring radioactive gas found at low levels in most soil, is produced in the
soil when the element uranium starts to break down. The health effects of high radon levels were
first seen in the increased cases of lung cancer found in underground uranium miners in the
United States and around the world. Radon gas seeps into cracks in the foundation of homes from
surrounding soil; about 1 in 20 homes has elevated radon levels. Research estimates that about
20,000 lung cancer deaths every year may be linked to radon exposures in homes.
Check the radon levels in your home regularly. A ventilation system in your basement can
dramatically reduce radon levels.
Atomic bombs and above-ground atomic bomb testing releases ionizing radiation that can increase
cancer risk. People affected by the atomic bombs in Japan at the end of World War II, those living
near nuclear testing sites in Nevada in the late 1950s and early 1960s, and those near the site of the
Chernobyl nuclear power plant accident in the former Soviet Union in 1986 were all exposed to
ionizing radiation.
Japanese atomic bomb survivors had increased rates of cancers of the breast, thyroid, lung,
stomach, and other organs. People, especially children, exposed to iodine-131 (one form of
radioactive iodine) both from the above-ground nuclear testing that has occurred in the United
States and from the Chernobyl accident, have an increased risk of thyroid cancer.

X-rays, mammograms, and radiation therapy all involve exposure to ionizing radiation. An X-ray
of the chest exposes a patient to only a small amount of radiation--about the same as one gets from
two airplane flights across the United States.
Studies have not shown an elevated cancer risk associated with X-rays taken to diagnose a disease
or condition. One exception to this is in children whose mothers received X-rays while pregnant:
the children were found to have increased risks of leukemia and other types of cancers. Because of
this finding, X-rays to diagnose a condition in pregnant women are no longer recommended.
Talk with your doctor about the need for each X-ray that he or she suggests. Ask about shields to
protect other parts of your body during an X-ray.

Radiation to treat a condition--such as cancer or ringworm--is more likely to increase cancer risk.
For example, people who receive radiation to treat conditions of the head and neck have an
increased risk of thyroid cancer and of tumors of the head and neck.

About 20 ingredients in pesticides have been found to cause cancer in animals. Studies of people
with high exposure to pesticides--farmers, crop duster pilots, pesticide manufacturers--have
shown higher rates of blood and lymphatic system cancers in these people, as well as melanoma
and cancers of the lip, stomach, brain, lung, and prostate.

Some chemotherapy drugs used to treat cancer may increase the risk of second cancers later in life.
Drugs that suppress the immune system--used to treat some cancers as well as to prepare patients
receiving organ transplants--also are associated with increased risk of cancer, particularly
lymphoma.
On the other hand, new estrogen-blocking drugs called aromatase inhibitors can decrease the
recurrence of breast cancer.
Any medication carries risks and benefits, so always check with a health professional before
starting a new drug.

Estrogen and progesterone are naturally occurring hormones. Given to women to treat the
symptoms of menopause, they have been linked to increased risk of breast cancer.
Estrogen may also increase the risk of endometrial cancer, but progesterone helps protect against
this increased risk. Estrogen and progestin (a synthetic form of progesterone) taken together are
associated with increased risks of breast cancer, heart disease, stroke, and blood clots. Women
who take oral contraceptives, which contain both estrogen and progesterone, may have increases
in early-onset breast cancers and liver cancer, but have substantially reduced risks of endometrial
and ovarian cancers.

The synthetic hormone tamoxifen is used in breast cancer therapies to prevent recurrence of
disease or to prevent onset in women at high risk for this cancer, but it may increase the risk of
endometrial cancer, strokes, and blood clots.
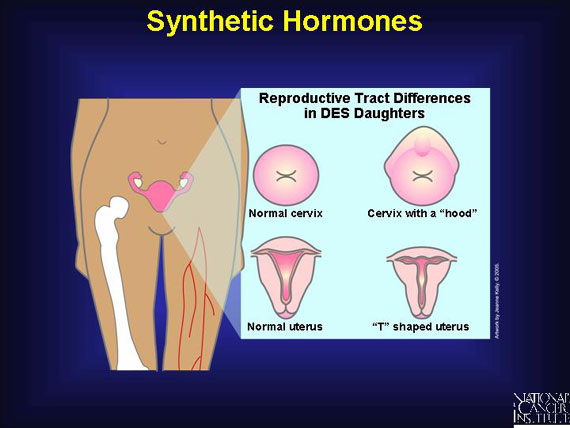
DES (diethylstilbestrol) is another synthetic hormone that was prescribed to pregnant women in
the 1940s, 1950s, and 1960s. DES use was discontinued after scientists discovered that women
taking it had an increased risk of breast cancer, and that girls born to women taking DES had an
increased risk of rare types of vaginal and cervical cancer. Most physical or structural differences
associated with exposure to DES are found in the reproductive tract, including a "hood" or collar
on the cervix and a T-shaped uterus.
Solvents are used in paint removers, grease removers, paint thinners, and dry cleaning. The
solvents benzene, carbon tetrachloride, chloroform, and methylene chloride have been linked to
human cancer.
The strongest evidence linking a solvent to cancer involves benzene, which is also found in
cigarette smoke and gasoline. It increases the risk of leukemia.
If you must work with solvents, work outside or make sure the area is well ventilated.

Some fibers and dusts can increase the risk of lung-related cancers.
Asbestos is linked to increased risks of lung cancer and mesothelioma, a rare cancer of the lining
of the lung and abdominal cavity. In the past, asbestos was widely used in construction, but its use
has been restricted. However, workers employed in construction, electrical work, or carpentry
may still be exposed through renovations or asbestos-removal projects.
Other fibers and dusts (including silica dust and wood dust) can increase the risks of cancers of
the lung, nasal cavities, and sinuses.
Wear a well-fitting mask if your job exposes you to fine particles, fibers, or dust.

Dioxins are byproducts of paper bleaching, smelting, and waste incineration. They are widespread
in the environment because they break down very slowly. They also accumulate in fat cells. Most
of our exposure to dioxins comes from eating dairy products, fish, and meat.

These compounds (known as PAHs) come from the burning of carbon-based material. They are
found in wood smoke, car exhaust, cigarette smoke, and charcoal-grilled foods. Sausages and
roasted coffees may also contain PAHs. These compounds have been linked to increased risks of
lung, skin, and urinary cancers.

Some metals--including arsenic, beryllium, cadmium, chromium, lead, and nickel--have been
associated with several types of cancer, including lung, kidney, brain, skin, and liver cancers.

Vinyl chloride is used in the plastics industry and has been associated with lung cancer and with
angiosarcomas (blood-vessel tumors) of the liver and brain. Most people are not routinely
exposed to vinyl chloride unless they work in plastics manufacturing plants. People who live close
to such plants also may be exposed through contaminated air.

Benzidine has been known to be associated with cancer since the 1920s. It is used in the
production of dyes for paper, textiles, and leather. Exposure to these dyed products is not
hazardous, however.

Aflatoxins are produced by certain types of fungi that grow on grains and peanuts. People can
also be exposed to aflatoxins by eating meat or dairy products from animals that ate contaminated
feed. Exposure to high levels of aflatoxins increases the risk of liver cancer. Peanuts are screened
for aflatoxins in most countries, including the United States.

Americans commonly use more than 100,000 chemicals, and this doesn't take into account
mixtures or combinations of chemicals. Plus, some chemicals are altered by the atmosphere, water,
or incineration.
Scientists have been working for several decades to identify substances that cause cancer. They
have three ways to do this: through human studies, animal studies, and laboratory experiments.

Human studies are the way to decide with the most certainty whether a substance causes cancer.
By following groups of people over time, researchers may be able to see whether certain
exposures lead to cancer. They also compare a group of people who have been diagnosed with a
type of cancer to another group of people without the disease. Sometimes the group with cancer
has patterns of exposures very different from the patterns in the group without cancer.
Many environmental causes of cancer have first been noticed in the workplace, because people in
certain occupations have higher exposures to some chemicals than do people in the general
population.

Rodents (mice and rats) are commonly used in studies of environmental causes of cancer. They
have a relatively short lifespan (2 to 3 years), and their bodies' responses to known cancer causing
chemicals are similar to a human response. Dietary studies in rodents are more difficult,
however, due to differences in the digestive systems of rodents and humans.
In animal studies, the chemical exposures are usually at much higher levels than would be seen
with human exposure. If an extremely high level of exposure does not lead to cancer, researchers
reason that the chemical most likely does not cause cancer at lower levels either.

Researchers study human cells in the laboratory to see whether certain chemicals might cause
changes that could lead to cancer.
These studies are often done to see if animal studies--which take longer and are more complex--
are actually needed. If a chemical does not cause cancer in laboratory cells, animal studies usually
aren't done.

How do scientists decide which exposures are high risk and which are low risk?
Risk assessment involves three factors:
1. Potency: The potential of a given amount of a substance to cause cancer. Benzene, for example,
is quite potent because even small amounts of it can increase cancer risk. Other compounds, such
as chloroform, are less potent; they require higher exposures to increase the risk by the same
degree.
2. Type of exposure: Whether the exposure is one-time (acute) or long-term (chronic), and
whether it is unavoidable (in the workplace, for example, or in the air we breathe).
3. Dose response: A dose-response trend describes what happens to cancer risk as the level of
exposure increases or decreases.

Certain occupations carry an increased cancer risk: these include painters; furniture makers;
workers in the iron, steel, coal, and rubber industries; and workers involved in shoe
manufacturing and repair.
Always use proper protective equipment when handling chemicals, and clean spills immediately.
Ask at your workplace about Material Safety Data Sheets, which contain information about
hazardous substances.
The National Institute for Occupational Safety and Health (http://www.cdc.gov/niosh/) can answer
many of your questions.

Cancer screening tests help detect cancer at an early stage, which allows treatment to occur before
the cancer spreads.
Get screened regularly for these cancers:
- Colon/rectum: Tests include the fecal occult blood test, sigmoidoscopy, and colonoscopy.
- Breast: The standard screening test is a mammogram, or X-ray of the breast tissue.
- Cervix: The standard screening test is the Pap smear.
Guidelines for when testing should begin and how often it should occur may be different for each
person, so talk with your doctor about what's right for you.
Also talk with your health care provider about exposures at work and at home, and discuss
whether your family or personal history may put you at risk for certain types of cancer. Your
doctor may recommend other cancer screening tests as well.

While it is always prudent to be aware of environmental exposures to carcinogens, one must also
remember that the major environmental factors linked to cancer deaths can be avoided, because
most of them involve behavior choices. More than half of all cancer deaths could be prevented by
eliminating the use of tobacco products, moderating the use of alcohol, and making better dietary
choices.

|