|
Although MHC proteins are required for T cell responses against foreign invaders, they can pose
difficulty during transplantation. Every cell in the body is covered with MHC
self-markers, and each person bears a slightly unique set. If a T lymphocyte
recognizes a non-self MHC scaffold, it will rally immune cells to destroy the cell
that bears it. For successful organ or blood stem cell transplantations, doctors must
pair organ recipients with donors whose MHC sets match as closely as possible.
Otherwise, the recipient's T cells will likely attack the transplant, leading to graft rejection.
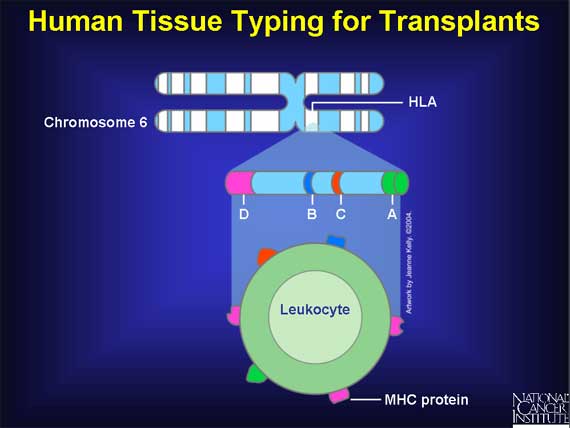
To find good matches, tissue typing is usually done on white blood cells, or leukocytes. In
this case, the MHC-self-markers are called human leukocyte antigens, or HLA. Each cell has a
double set of six major HLA markers, HLA-A, B, and C, and three types of HLA-D. Since each of
these antigens exists, in different individuals, in as many as 20 varieties, the number of
possible HLA types is about 10,000. The genes that encode the HLA antigens are located on chromosome 6.
< Previous | Index | Next Slide > |