|
Here is some general information about the human papilloma
virus (HPV) and the HPV vaccine.
What are viruses?
Viruses are very small organisms -- most cannot even be seen
with a regular microscope. They cannot reproduce on their own. They
must enter a living cell, which becomes the host cell, and
"hijack" the cell's machinery to make more viruses.
Viruses can enter the body through the mucous membranes, such
as the nose, mouth, the lining of the eyes, or the genitals. They can
also enter through breaks in the skin. Once inside, they find their
specific type of host cell to infect. For example, cold and flu viruses
find and invade cells that line the respiratory tract (nose, sinuses,
breathing tubes, and lungs). The human immunodeficiency virus (HIV)
infects the T-cells and macrophages of the immune system. HPV infects squamous epithelial cells
in the body -- the flat cells that line the surface of the skin and
mucous membranes.
What is HPV?
HPV is short for human
papilloma virus (pap-uh-LO-muh). HPVs are a group of over
100 related viruses. Each HPV virus in the group is given a number,
which is called an HPV type. HPVs are called papilloma viruses because
some of the HPV types cause warts or papillomas, which
are non-cancerous tumors. The papilloma viruses are attracted to and
are able to live only in squamous epithelial cells in the body.
Squamous epithelial cells are thin, flat cells that are found on the
surface of the skin, cervix, vagina, anus, vulva, head of the penis,
mouth, and throat. HPVs will not grow in other parts of the body.
Of the more than 100 strains of HPV, about 60 HPV types cause
warts on non-genital skin, such as on the hands and feet. These are the
common warts.
The other 40 HPV types are mucosal types of HPV. "Mucosal"
refers to the body's mucous membranes, or the moist skin-like layers
that line organs and cavities of the body that open to the outside. For
example, the vagina and anus have a moist skin-like layer. The mucosal
HPV types are also called the genital (or anogenital) type
HPVs because they typically affect the anal and genital area. The
mucosal HPVs prefer the moist squamous cells found in this area. They
do not grow in the skin of the hands and feet.
Low-risk HPV types
Some types of genital HPVs can cause cauliflower-shaped warts
on or around the genitals and anus of both men and women. In women,
warts may also appear on the cervix and vagina. This type of "genital
wart" is known as condyloma
acuminatum and is most often caused by HPV-6 or HPV-11.
Because these genital warts rarely grow into cancer, HPV-6 and HPV-11
are called "low-risk" viruses. These low-risk types can also cause low-grade changes
in the cells of the cervix that do not develop into cancer.
High-risk HPV types
Other genital type HPVs have been linked with genital or anal
cancers in both men and women. These types are called "high-risk"
because they can cause cancer. They also cause low-grade and high-grade
changes in the cells of the cervix and pre-cancers. Doctors worry more
about the high-grade changes and pre-cancers, because they are more
likely to grow into cancers. Common high-risk HPV types include:
- HPV-16
- HPV-18
- HPV-31
- HPV-35
- HPV-39
- HPV-45
- HPV-51
- HPV-52
- HPV-58
In 90% of cases, the body's immune system clears the HPV
infection within 2 years. This is true of both high-risk and low-risk
HPV types.
In summary, low-risk HPV types can cause genital warts and
low-grade changes in the cells of the cervix. High-risk HPV types can
cause low-grade changes, high-grade changes, pre-cancer, and cancer in
the cells of the cervix.
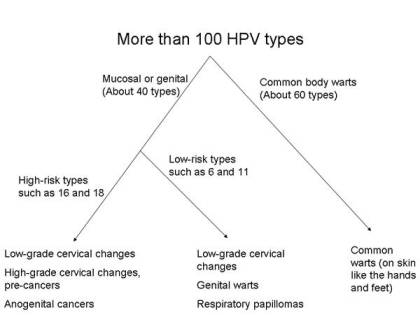
Here is a diagram showing the different groups of HPV types
and the problems each group can cause.
How do you get genital HPV?
Genital HPV is spread mainly by direct genital contact during
vaginal, oral, or anal sex. It is not spread through blood or body
fluids. HPV is passed from one person to another during skin-to-skin
contact.
Infection is very common soon after a woman becomes sexually
active. In one study, more than 50% of college-aged women were found to
have gotten an HPV infection within 4 years of first having sex.
Transmission by genital contact without sexual intercourse is
not common, but infection has been reported in women who have never had
sexual intercourse. Oral-genital and hand-genital transmission of some
genital HPV types is possible and has been reported. Transmission from
mother to newborn during delivery is rare. When it occurs, it can cause
warts in the infant's throat called respiratory papillomatosis.
How common is HPV? Who gets it?
Genital HPV is a very common virus. Some doctors think it is
almost as common as the common cold virus. In the United States, over 6
million people (men and women) get an HPV infection every year. Almost
half of the infections are in people between 15 and 25 years of age.
About one-half to three-fourths of the people who have ever had sex
will have HPV at some time in their life.
What are the symptoms of HPV?
Genital HPV usually has no symptoms, unless it is a type that
causes genital warts. Genital warts may appear within weeks or months
after contact with a partner who has HPV. More rarely, genital warts
may show up years after exposure.
Most people will never know they have HPV because they have no
symptoms and the body's immune system causes the virus to become
inactive. A small number of people with HPV will have the virus for a
longer time. These people can develop cell changes that over many years
may lead to cervical or other genital or anal cancers.
How is HPV related to cervical cancer?
Almost all (more than 99%) cervical cancers are related to
HPV. Of these, about 70% are caused by HPV types 16 or 18. About
500,000 pre-cancerous cell changes of the cervix, vagina, and vulva are
diagnosed each year in the United States, and over half are related to
HPV 16 and 18. Low-grade changes in the cells of the cervix are caused
by a variety of HPV types, including 16, 18, 6, or 11. Low-grade
changes most often go away without treatment, although if they grow
into warts doctors may remove them. But low-grade changes may be caused
by some high-risk HPV types (as well as low-risk ones), and doctors who
find low-grade changes often do more testing.
Nearly all cervical cancers are related to HPV, but most
genital HPV infections do not cause cervical cancer. In research
studies, most people who test positive for genital HPV DNA test
negative later on, often within 6 to 12 months. Scientists are still
not sure whether this means that a person's immune system has
completely destroyed all of the HPV or has only suppressed the
infection to an extremely low level (too low to be detected by the
tests). If even a few cells of the cervix still contain HPV, it's
possible that the virus may start to become active again if your immune
system becomes very weak.
Changes in the cells of the cervix may suddenly happen many
years after being exposed to HPV. These changes may be low-grade or
high-grade. This delay could help explain how a woman could have these
changes after many years of normal Pap tests and no new sex partner.
If cells stay infected with HPV, the virus may cause the cells
of the cervix to change and become pre-cancer cells. True pre-cancer
cell changes are called high-grade SIL (squamous intraepithelial
lesions), sometimes abbreviated as HSIL. Another term for HSIL is CIN 2
and CIN 3. CIN is an abbreviation for cervical intraepithelial
neoplasia.
Pre-cancer cells are not cancer. Some pre-cancer changes may
return to normal on their own. But most cases of CIN 3 that are not
found and treated are likely to progress to cervical cancer over about
10 years. Still, very few HPV infections lead to cervical cancer.
Pre-cancer cells are found before they have a chance to grow into
cancer by having regular Pap tests.
For more information on cervical cancer, please see our
document, Cervical Cancer.
What about other cancers and HPV?
Many anal cancers are caused by the same types of genital HPV
that cause cervical cancer. A little less than half of cancers of the
vulva are HPV-related. Some other genital cancers (cancers of the
penis, vagina, vulva, and urethra) and some head and neck cancers
(mostly the tongue and tonsils) may be related to the high-risk types
of HPV. Also, many of the skin cancers in people with weak immune
systems might be related to this virus.
What about other HPV-related diseases?
Over 500,000 new cases of anal and genital warts are diagnosed
yearly in the United States. About 9 out of 10 of these cases are
caused by HPV-6 or HPV-11).
Do men have the kinds of cancers that are
related to HPV?
HPV is probably as common in men as in women. But HPV is not
as easily diagnosed in men as in women. Genital HPV is mostly passed to
men through vaginal and anal sex -- the same way it is in women. Some
types of HPV have been linked to cancer of the penis and anus in men.
Although cancer of the penis is rare, anal cancer is now almost as
common in men and women who have anal sex as cervical cancer was in
women before the Pap test was introduced. But keep in mind that even
though anal sex greatly raises a person's risk of anal cancer, anal sex
is not the only way to get anal HPV or anal cancer.
Like women, men do not have symptoms with HPV unless it is the
type that causes genital warts. In men, genital warts can appear around
the anus or on the penis, scrotum, groin, or thighs.
There is no test approved by the US Food and Drug
Administration (FDA) to detect HPV in men. But genital warts can be
found and treated. While women have the Pap test, there are no tests
approved to detect early HPV-related cancers in men. In gay, bisexual,
and HIV-positive men, some doctors use anal Pap tests to detect and
treat pre-cancerous changes of the anus. Since anal testing is in the
early stages of development and use, its effect on anal cancer rates
will not be seen for many years.
For more information on sexually transmitted illnesses in men,
please contact the American Social Health Organization (ASHA) at http://www.ashastd.org.
You can get information on teen sexual health in English at http://www.iwannaknow.org
or in Spanish at http://www.quierosaber.org.
Can HPV be treated?
No. Treatments cannot cure HPV. But most genital HPV
infections go away with the help of the body’s immune system.
About 70% of HPV infections appear to go away within a year and 90%
within 2 years. HPV itself cannot be treated, but the cell changes that
come from an HPV infection can be treated. For example, genital warts
can be treated. Pre-cancer cell changes caused by HPV can be found by
Pap tests and treated. And cervical, anal, and genital cancers can be
treated, too.
Can HPV be prevented?
Getting the HPV vaccine before being exposed to HPV will
prevent some HPV. Limiting the number of sex partners and avoiding sex
with people who have had many other sex partners decreases a person's
risk of exposure to HPV. HPV infection is so very common, though, that
even these measures are no guarantee that a person will not get HPV.
Still, these measures may help reduce the number of times a person is
exposed to HPV.
Condoms provide some, but not total, protection against HPV.
The virus can spread during direct skin-to-skin contact before the
condom is put on, and male condoms do not cover the entire genital
area, especially in women. The female condom covers more of the vulva
in women but has not been studied as carefully for its ability to
prevent HPV. Condoms are very helpful, though, in protecting from other
infections that can be spread through sexual activity.
What are the risk factors for genital HPV?
People with the following risk factors are more likely to have
genital HPV:
- having many sex partners
- being younger than 25 years of age
- starting to have sexual intercourse at age 16 or younger
- having a partner who has had several different sex partners
Still, a person who has had sex with only one partner can get
HPV if that partner already has the virus. HPV can also be picked up
from having sex with an infected person at any age.
Is there a vaccine to prevent HPV?
In 2006, the Food and Drug Administration (FDA) approved a
vaccine that prevents the 2 types of HPV (HPV 16 and 18) that cause 70%
of all cervical cancers. The vaccine also prevents 2 types of HPV (HPV
6 and 11) that cause 90% of all genital warts. This vaccine is named
Gardasil®.
There is another vaccine that is still being studied to see if
it safely prevents HPV 16 and 18. It is called Cervarix®,
and
it is not yet approved by the FDA for use in the United States. Unlike
Gardasil, it does not target the wart-causing HPV types.
Did the American Cancer Society play a role
in the development of the HPV vaccine?
Yes. Dr. Robert Rose at University of Rochester was a member
of 1 of 4 teams that contributed to the development of a vaccine
against HPV. The grant he received from the American Cancer Society in
the mid-1990s enabled him to continue and confirm his important work
studying the virus.
Is the HPV vaccine safe?
Before it was approved, the HPV vaccine was tested in more
than 21,000 girls and women in many countries around the world. There
were no deaths due to the vaccine, and almost no serious side effects
reported during those trials. The most common side effect was brief
soreness at the injection site. The FDA has determined that the vaccine
is safe and effective for females aged 9 to 26 years.
By late 2008, more than 20 million doses of the vaccine had
been distributed in the United States. The Centers for Disease Control
and Prevention (CDC) and the FDA monitor the safety of all vaccines
used in the United States. As of August 31, 2008, the Vaccine Adverse
Event Reporting System (VAERS) had received a total of 10,326 reports
of potential side effects following HPV vaccination. (VAERS is a
national reporting system that monitors reports of potential side
effects following vaccination.) Less than 6% of those reports were
serious side effects, about half of the average for vaccines overall.
There have also been 27 cases of death after vaccination
reported to VAERS. Each death has been reviewed, and there was no
common pattern to the deaths that would suggest they were caused by the
vaccine. When there was an autopsy, death certificate, or medical
record, the cause of death was explained by factors other than the
vaccine. Some causes of these deaths include drug abuse, diabetes,
viral illness, and heart failure.
There were also reports of Guillain-Barré Syndrome
(GBS) after Gardasil vaccination in the United States. But only some of
these have been confirmed as GBS. The CDC says the number of GBS cases
reported are well within the range that would be expected to happen
anyway (that is, the same number of cases would be expected in people
who did not get the vaccine).
CDC and FDA doctors and scientists continue to review all
reports of serious side effects reported to VAERS to watch for
potential new vaccine safety concerns that may need further study. We
will monitor those reviews and report any concerns about the safety of
the vaccine.
What are the less serious side effects from
the vaccine?
Most reports of problems after the HPV vaccine have been
minor. Common events include pain at the injection site, headache,
nausea, and fever. There have also been reports of people fainting.
Fainting is common after injections, even more so in pre-teens
and teens. Falls that happen when someone faints can cause serious
injuries, such as head trauma. To help prevent injuries, CDC and FDA
recommend that people getting any vaccine should sit or lie down for 15
minutes after they get it.
Who should be vaccinated and when?
To be most effective, the HPV vaccine should be given before a
female has any type of sexual contact with another person. It is given
in a series of 3 doses within 6 months. Here are the recommendations
for each age group:
- girls ages 11
to 12
The vaccine should be given to girls ages 11 to 12 and as early as age
9.
- girls ages 13
to 18
Girls ages 13 to 18 who have not yet started the vaccine series or who
have started but have not completed the series should be vaccinated.
- young women
ages 19 to 26
Some authorities recommend vaccination of women ages 19 to 26, but the
American Cancer Society experts believed that there was not enough
evidence of the benefit to recommend vaccinating all women in this age
group. We do recommend that women ages 19 to 26 talk to their doctors
or nurses about whether to get the vaccine based on their risk of
previous HPV exposure and potential benefit from the vaccine.
What about women over 26 years of age?
Should they get the vaccine?
Women over 26 years of age were not included in the studies
that were done to test the vaccine. That means the FDA could not
approve the vaccine for this age group. Studies are now being done in
women ages 27 to 55. When those study results are known, a decision can
be made about whether to vaccinate women in this age group.
Keep in mind that the risk of HPV exposure is highest soon
after women become sexually active. So it is likely that women over 26
have already been exposed to HPV and would not benefit as much from the
vaccine.
Are there some girls or women who should not
get the HPV vaccine or who should wait?
Yes. Anyone who has ever had a life-threatening allergic
reaction to yeast or anything else in the HPV vaccine, or anyone who
has had a reaction to an earlier dose of HPV vaccine should not get the
vaccine. Tell the doctor if the girl getting the vaccine has any severe
allergies.
Pregnant women should not get the vaccine. Even though it
appears to be safe for both mother and the unborn baby, it is still
being studied. If a woman who is pregnant does get the vaccine, this is
not a reason to consider ending the pregnancy.
Any woman who finds out that she was pregnant when she got the
vaccine is encouraged to call the HPV vaccine in pregnancy registry at
1-800-986-8999. Information from this registry will help us learn how
pregnant women respond to the vaccine. Pregnant women who have started
the vaccine series should complete the series after their baby is born.
Women who are breast-feeding may safely get the vaccine.
Why does the vaccine have to be given at
such a young age?
The vaccine will prevent HPV only if it is given before a girl
has been exposed to HPV. The vaccine is recommended for girls ages 11
to 12 because most girls at this age have not become sexually active.
This is also an age when girls will be seeing their doctor and getting
other vaccinations.
Can boys get this vaccine?
At this time boys cannot get the HPV vaccine. Boys were
included in some of the studies -- the vaccine was found to be safe and
the boys' immune systems did respond to it. It is not known at this
time if the vaccine will protect boys from genital warts or keep them
from passing HPV to their partners. Studies are being done to find out
if the vaccine will prevent HPV infection and genital warts in boys.
What are the benefits of the vaccine?
The vaccine will prevent the 2 types of HPV that cause most
cervical cancers (about 70%) and the 2 types of HPV that cause most
genital warts (about 90%), but only in women who have not already been
exposed to these types of HPV. It also helps prevent vulvar and vaginal
cancers related to these 2 types of HPV. The vaccine will not prevent
HPV in women who have already had these HPV types.
It is possible that the vaccine also could prevent some other
HPV-related cancers, including some cancers of the anus and penis, as
well as some head and neck cancers. It will be some years before
studies can prove whether it will prevent these cancers.
How long will the vaccine prevent HPV
infection?
How long a new vaccine protects people is never known when the
vaccine is first introduced. Research is being done to find out how
long protection against HPV will last, and if a booster vaccine will be
needed.
How much does the HPV vaccine cost? Is it
covered by health insurance plans?
The drug company price is $120 per dose. This cost does not
include the cost of giving the shots or the doctor's charge. So the
cost for the series (3 shots over 6 months) could be as much as $500 or
more. Insurance plans will likely cover the cost. But check with your
insurance plan to know for sure.
The vaccine is included in the federal Vaccine for Children
(VFC) program. This program covers vaccine costs for children and teens
that don't have insurance and for some children and teens that are
underinsured. The VFC program provides free vaccines to children and
adolescents younger than 19 years of age, who are either
Medicaid-eligible, American Indian or Alaska Native, or uninsured.
There are over 45,000 sites that provide VFC vaccines,
including hospitals and private and public clinics. The VFC program
also allows children and adolescents to get VFC vaccines through
federally qualified health centers or rural health centers if their
private health insurance does not cover vaccinations. For more
information about the VFC program, visit
www.cdc.gov/vaccines/programs/vfc/default.htm.
Or call 1-800-CDC-INFO
(1-800-232-4636).
Some states and US territories have programs that will cover
the vaccine costs, too. You can find the contact information for your
area at the CDC Web site given above.
Do you need to be tested for HPV before
getting the vaccine?
No. Testing is not needed and it is not recommended. A
positive HPV test result does not tell you which types of HPV are
present. Even after infection with one type of HPV, the vaccine could
still prevent the other types of HPV. A negative test does not tell you
if you have had HPV but no longer have it.
Will women and girls who have been
vaccinated still need Pap tests?
Yes. People who get vaccinated will still need Pap tests
because the vaccine will not prevent all types of HPV that can cause
cervical cancer. If your daughter or granddaughter gets the vaccine,
she will still need to have Pap tests at the usual times.
If girls who are vaccinated will still need
a Pap test, why should they get vaccinated?
The vaccine will actually prevent about 70% of cervical
cancers. And those who have had the HPV vaccine can avoid the cervix
cell changes caused by the HPV types the vaccine contains. The Pap test
does not keep the cells in the cervix from changing -- it can pick up
changes in the cervix after they happen, but before they can become
cervical cancer. This means that if a woman has an abnormal Pap test,
she will have other tests and then treatment to prevent the cells from
becoming cancer. Also, Pap tests are not perfect and can miss cervical
changes and cancers.
Can cervical cancer be prevented without a
vaccine?
In some cases, yes, cervical cancer can be prevented without a
vaccine. Pap tests done according to American Cancer Society guidelines
and with proper follow up will prevent most but not all cases of
cervical cancer. Pap tests can find cervix cell changes early before
they become cervical cancer. These changed cervix cells can then be
killed or removed to prevent them from becoming cancer. The Pap test
will find most but not all cervical cancers at an early, curable stage.
Most cervical cancers in the United States are diagnosed in women who
have never had a Pap test, or who haven't had a Pap test in 5 or more
years.
If all women who have had sex had regular Pap tests, most
cervical cancers could be prevented. Pap tests are used to find changes
in the cells of the cervix early so they can be treated before they
become cervical cancer.
Is the American Cancer Society in favor of
vaccinating against HPV?
Yes, the Society is very much in favor of vaccinating against
HPV. The Society has been actively involved in providing credible and
unbiased information to the public and to health care providers. The
Society emphasizes the ongoing need to follow screening guidelines,
such as getting regular Pap tests, and the critical need to ensure that
the vaccine is available to the medically underserved.
What is the American Cancer Society doing to
promote the vaccine's use?
The Society is engaged in an active public education effort to
ensure broad public awareness and acceptance of the new vaccine. The
Society recognizes the importance of building and sustaining the
infrastructure to support successful implementation of the vaccine
program.
Do you want more information?
For more information on cervical cancer, HPV, HPV testing, and
the HPV vaccine,
please call us anytime, day or night, at 1-800-ACS-2345
(1-800-227-2345) or visit our Web site at www.cancer.org.
For more information on the HPV vaccine from the Centers for
Disease Control (CDC), visit
http://www.cdc.gov/vaccines/vpd-vac/hpv/default.htm
References
Anhang R, Goodman A, Goldie, SJ. HPV Communication: Review of
existing research and recommendations for patient education. CA Cancer
J Clin.2004;54:245-247.
Centers for Disease Control and Prevention. Genital HPV
infection: CDC fact sheet. Available at:
http://www.cdc.gov/std/HPV/STDFact-HPV.htm. Accessed December 1, 2008.
Centers for Disease Control and Prevention. Human
Papillomavirus Infection. Available at:
http://www.cdc.gov/Features/HPV. Accessed December 3, 2008.
Centers for Disease Control and Prevention. Questions and
answers about HPV vaccine safety. Available online at:
http://www.cdc.gov/vaccinesafety/concerns/hpv_faqs.htm. Accessed
December 4, 2008.
Centers for Disease Control and Prevention, Vaccine Adverse
Event Reporting System. Reports of health concerns following HPV
vaccinations. Available at:
http://www.cdc.gov/vaccinesafety/vaers/gardasil.htm. Accessed December
3, 2008.
Markowitz LE, Dunne EF, Saraiiya M,; et al. Quadrivalent human
papillomavirus vaccine: recommendations of the advisory committee on
immunization practices (ACIP). MMWR.2007;56:1-
23.
Moscicki AB, Hills NK, Shiboski S, Darragh TM, et al. Risk
factors for abnormal anal cytology in young heterosexual women. Cancer
Epidemiol Biomarkers Prev. 1999;8:173-8.
Nyitray A. Anal cancer and human papillomaviruses in
heterosexual men. Curr
Oncol. 2008; 15: 204–205.
Saslow D, Castle P, Cox T, et al. American Cancer Society
guidelines for human papillomavirus vaccine use to prevent cervical
cancer and its precursors. CA
Cancer J Clin. 2007;57:7-28.
Winer RL, Hughes JP, Feng Q, et al. Condom use and the risk of
genital human papillomavirus infection in young women. N Engl J Med.
2006;354:2645-54.
Last
Medical Review: 07/09/2009
Last Revised: 07/09/2009
|

