Updated 11/05
Facts About Charcot-Marie-Tooth Disease and Dejerine-Sottas Disease
|
For the Spanish version of this publication, click here: En Español
|
Dear Friends:
I've lived with Charcot-Marie-Tooth disease since my early 20s — more than half my life. The disease has progressed slowly
over the years, mostly affecting my lower legs and hands, so that now I use a
manual wheelchair part-time. In those years, I've continued a career in
computer technology, started a small business, pursued my interests in art and
photography, married, and contributed my knowledge and experience to others
with disabilities.
This pamphlet has been prepared to give you the basic knowledge about
CMT and Dejerine-Sottas disease that you'll
need, in order to help you prepare for changes that may occur in your future.
You'll learn that CMT is usually quite slow in progression and that, while it
presents challenges in daily life, there are many techniques and devices to
help you adapt to those challenges.
You'll read that many different genetic causes of CMT have been
found, and cases vary greatly. But CMT is almost never life-threatening, and it
seldom affects the heart and breathing functions.
And it doesn't affect intelligence or the spirit. I know of many
productive, successful people with CMT — doctors and scientists, artists and
singers, athletes and teachers, active teens and students. I know children with
CMT who have bright futures. We've all learned to strike a balance between
adapting to our limitations and surroundings, and living a fulfilling life
despite them.
I have the wonderful support of my family and great friends. I'm
involved in volunteer projects that help young people with disabilities,
advising them on independence and entrepreneurship, and raising public
awareness about disability wherever I go. What I've learned — and what I try to
teach — is that people with disabilities are — like everyone else — full of
possibilities and gifts. These, not our limitations, are what matter.
Another important extended family in my life is the Muscular
Dystrophy Association, which offers a great program of services, leads the
world in CMT research and keeps us well informed about the disease. See "MDA
Is Here to Help You," for details of the Association's program.
While MDA's research program continues making strides toward better
treatments and a cure, it's good to know that people with disabilities have
more opportunities than ever before to develop and use their abilities, and
that the laws entitle us to equal employment opportunities and access to public
places.
As you face the challenges ahead, remember, MDA and all its resources
are there to help you and your family. You're not alone.
George J. Donahue
Watertown, Mass.
top 
What Is Charcot-Marie-Tooth Disease?
 |
CMT causes degeneration of the peripheral nerves, leading to
muscle weakness in the body’s extremities.
1. Brain
2. Spinal cord
3. Arm muscle
4. Peripheral nerves
5. Foot muscle
6. Leg (peroneus) muscle
7. Hand muscle |
Charcot-Marie-Tooth disease (CMT)
is a neurological disorder, named after the three physicians who first
described it in 1886 — Jean-Martin Charcot and Pierre Marie of France, and
Howard Henry Tooth of the United Kingdom. Although most people have never heard
of CMT, it affects some 115,000 Americans.
Unlike other neurological disorders, CMT usually isn't
life-threatening, and it almost never affects the brain. It causes damage to
the peripheral nerves — tracts of nerve cell fibers that connect the
brain and spinal cord to muscles and sensory organs.
Peripheral nerves control movement by relaying impulses from the
spinal cord to muscles. They convey sensation by carrying feelings like pain
and temperature from the hands and feet to the spinal cord. They also help
control balance, by carrying information about the position of the body in
space. They transmit information about the feet and hands to the spinal cord
and then the brain, so that the brain knows where to place the feet when
walking and where the hands should be placed to reach for something.
Nerve damage, or neuropathy, causes muscle weakness and
wasting, and some loss of sensation, in the extremities of the body: the feet,
the lower legs, the hands and the forearms.
Although CMT can look very similar to acquired neuropathy — a
type of nerve damage caused by overexposure to certain chemicals — it isn't
caused by anything a person does, and it isn't contagious. It's hereditary,
meaning that it can be passed down through a family from one generation to the
next. (See "Does It Run in the Family?")
Because of these features, CMT is sometimes called hereditary and
motor sensory neuropathy (HMSN). Some doctors also use the
old-fashioned name peroneal muscular atrophy, which refers to wasting of
the peroneal muscle in the lower leg.
There are even more names for CMT because the disease exists in many
different forms, each unique in its severity, age of onset, progression and
exact symptoms. For example, Dejerine-Sottas disease (DS) is a
severe form of CMT that manifests during infancy or early childhood.
 |
Peripheral nerves control movement by relaying impulses from
the spinal cord (not shown) to our muscles (shown in the forearm).
A single peripheral
nerve is composed of many long nerve cell branches - or axons
- that extend from the spinal cord and connect to muscle fibers.
Each axon is surrounded by myelin made from the wrappings of Schwann
cells. |
Although there's no cure for CMT, there are treatments that can be
used to effectively manage its symptoms. Those treatments, described here along
with a general overview of CMT, have allowed many people with the disease to
lead active, productive lives.
top 
What Causes CMT?
CMT is caused by defects in genes, which are segments of DNA
contained in the chromosomes of the body’s cells. Genes are recipes
for making the proteins that serve essential functions in our bodies. Each form
of CMT is linked to a specific gene, and all of those genes make proteins found
within the peripheral nerves.
Peripheral nerves provide an essential relay between your brain and
the rest of your body. When you decide to move your leg, your brain sends an
electrical signal to muscle-controlling nerve cells in your spinal cord, which
then use the peripheral nerves to pass the signal on to your leg muscles.
And if you hurt your leg, you feel it because pain-sensitive nerve
cells there have sent an electrical signal through your peripheral nerves to
your brain.
The peripheral nerves are made up of fibers, or axons, that
extend from sensory nerve cells and muscle-controlling nerve cells, and carry
electrical signals to and from the spinal cord.
In order for you to move and react with precision and speed, axons
have to transmit their signals within a fraction of a second. This is a real
challenge for axons that have to stretch over long distances, like the ones
connected to muscles in your fingers and toes.
To give axons a performance boost, each one is surrounded by a
coating called myelin. Similar to the way plastic coating is used to
insulate electrical wiring, myelin insulates the electrical signals in axons.
It also provides essential nourishment to the axons.
Some 20 genes have been implicated in CMT, each one linked to a
specific type (and in many cases, more than one type) of the disease. (See "What
Are the Different Types of CMT?") Some of those genes make proteins
needed in axons, and others make proteins needed in myelin.
Defective myelin genes can cause a breakdown of myelin (called demyelination)
while defective axon genes can cause an impairment of axon function (axonopathy).
In either case, the end result is the same: Defects in the axon or
the myelin cause progressive damage to the axons.
The longest axons in the body are especially sensitive to damage,
which explains why CMT mostly causes motor and sensory problems in the body's
extremities.
Nerves other than those that go to and from the extremities can be
affected at the severe end of the CMT spectrum. If the nerves that go to and
from the diaphragm or intercostal (between the ribs) muscles are affected,
respiratory impairment can result.
top 
What Happens to Someone With CMT, and How Is It
Treated?
Partly because there are different types of CMT, the exact symptoms
vary greatly from person to person. This section provides a general picture of
CMT, and the next section describes different types of the disease.
Muscle Weakness
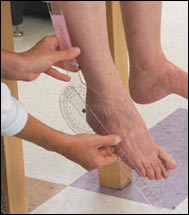 A doctor examines a patient with foot drop. A doctor examines a patient with foot drop. |
In general, people with CMT experience slowly progressive weakness
and wasting in the distal muscles, which control the extremities.
These muscles control foot and hand movements. More proximal muscles,
those closer to the trunk, such as the leg and arm muscles, are rarely
affected.
Usually, weakness begins in the feet and ankles, and manifests itself
as foot drop — difficulty lifting the foot at the ankle, so that the
toes point downward during walking. Foot drop causes frequent tripping, and
with increasing weakness and attempts at compensation, the affected person
develops an abnormal gait.
Many people with CMT make their first visits to a neurologist after
they notice frequent trips and falls, ankle sprains, or ankle fractures, caused
by foot drop.
When these problems occur, some people find they can overcome them
just by wearing boots or high-top shoes to support the ankles.
Others might require leg braces, such as an ankle-foot orthosis (AFO), a removable cast that fits snuggly around the foot and ankle.
Once made of clunky metal struts that required special shoes, AFOs are now made
of lightweight plastic that's custom-molded to fit the wearer's legs, and can
be worn underneath pants and tennis shoes.
For people with more proximal weakness, there’s the knee-ankle-foot
orthosis (KAFO), which extends up the leg, just above the knee. They
usually can be worn under trousers. Some orthoses allow movement of the ankle
or knee, while others prevent movement to add more support.
Most people with CMT won’t need a wheelchair or motorized scooter,
but an older person with advanced CMT or someone with a severe type might
require one of these to get around, especially when traversing long distances.
Like AFOs, wheelchairs aren’t what they used to be. There are wheelchairs that
can be used on almost any terrain — from shopping mall to hiking trail — many
of them powered by the flip of a switch.
MDA assists with purchase and repair of AFOs and wheelchairs.
Late in the course of CMT, many people experience weakness in the
hands and forearms, and have difficulty with gripping and fine finger
movements, such as turning doorknobs, and buttoning and zippering clothes.
Often, these problems can be overcome with occupational therapy, which
helps people accomplish the "job" of daily living through the use of assistive
devices.
For example, an occupational therapist might recommend that you put
special rubber grips on your home's doors, or buy clothes that fasten with
Velcro or snaps. Your MDA clinic can refer you to an occupational therapist.
Weakness of the respiratory muscles is rare in people with CMT, but
when it occurs it can be life-threatening. If you regularly experience
shortness of breath, you should have your breathing checked by a specialist,
who might recommend occasional or nighttime use of a device that delivers air
under pressure into the lungs.
Although it's usually too slight to cause disability or discomfort,
some people with CMT experience tremor (involuntary shaking). CMT with
obvious tremor is sometimes called Roussy-Levy syndrome.
Contractures and Bone Deformities
Many people with CMT eventually develop contractures (stiffened
joints because of abnormal tightening of muscles and associated tissues) that result in deformities of the feet and hands.
The contractures occur because as some muscles around a joint weaken,
others remain strong, contracting and pulling on the joint. Over time,
the bones around the joint shift into abnormal positions.
For example, as muscles that lift the foot at the ankle become weak,
muscles that lower and curl the foot downward contract and tighten, causing the
most common type of foot deformity — a shortened foot with a high arch (pes
cavus). As the contracture gets worse, the toes can become locked in a
flexed position.
 Foot contractures resulting in high-arched feet often occur
in CMT. Foot contractures resulting in high-arched feet often occur
in CMT. |
A small fraction of people with CMT develop "flat feet" (pes planus),
presumably because of a different pattern of muscle weakness.
During walking, these deformities can cause unusual friction against
the toes, heel and ball of the foot, leading to painful abrasions, blisters and
calluses. If left untreated, the contractures and secondary abrasions tend to
worsen over time, making it increasingly difficult to walk.
As CMT progresses, contractures in the hand can lock the fingers in a
flexed position, and in rare cases severe proximal weakness can lead to scoliosis (side-to-side curvature of the spine) or kyphosis (front-to-back spine
curvature).
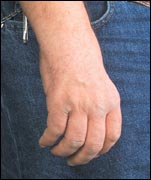 Hand contractures can occur late in the course of CMT. Hand contractures can occur late in the course of CMT. |
A small fraction of people with severe CMT also experience hip
displacement at an early age.
One of the most effective ways to keep muscles from tightening up and
forming contractures is to begin a regular program of physical therapy,
which usually consists of low-impact exercises and stretching.
Your MDA clinic can help get you started on an individualized
physical therapy program.
Foot contractures can also be delayed by using AFOs, which force the
feet into a normal position and decrease stress on the ankles. Similarly,
splints can be used to prevent unintended flexing of the toes and fingers.
If these methods fail and severe contractures occur, surgery can be
used to loosen up tight muscles and tendons, or to correct bone deformities.
Surgery is often necessary for advanced scoliosis.
Sensory Loss and Associated Symptoms
Because CMT causes damage to sensory axons, most people with CMT have
a decreased sensitivity to heat, touch and pain in the feet and lower
legs.
Although people with CMT often complain that their feet get cold
(caused as much by a loss of insulating muscle as by damage to sensory axons),
most of these sensory losses are undetectable except by a neurological exam —
but it's important to recognize that they occur.
Combined with the regular abrasions caused by foot
deformities, the lack of pain sensitivity makes people with CMT at risk
for developing ulcerations — wounds that have gone unnoticed and become
severely infected. If you have CMT, and especially if you have any foot
deformities, you should check your feet regularly for injuries.
Paradoxically, some people with CMT experience more pain — a
combination of painful muscle cramps and neuropathic pain. This pain
isn't caused by an external trigger, but by defective signals in sensory axons.
Both types of pain can usually be alleviated with medication.
In many people with CMT, sensory loss is associated with dry skin and
hair loss in the affected area.
In rare cases, sensory loss can include gradual hearing impairment
and sometimes deafness. Watching out for these potential problems will enable
you to seek appropriate treatment if necessary.
Drug Warning
The use of certain prescription drugs or excess alcohol can lead to
acquired neuropathy, and thus might exacerbate CMT. Case studies have shown
that the chemotherapy drug vincristine can cause rapid deterioration in people
with CMT.
When taking a prescription drug for the first time, it's a good idea
to consult your doctor about its possible effects on CMT. Or, enter the
specific name of the drug into an Internet search engine, along with the words
“prescribing information,” to receive a full explanation of what the drug does
and what its side effects may be.
You’re unlikely to see anything specific about CMT. However, if the
medication’s side effect description mentions words like neuropathy, paresthesias, neuropathic pain or peripheral nerve damage, you may want to
consult your physician about its use in CMT and possible alternatives.
Lists of contraindicated (forbidden) drugs for people with CMT are
often composed mostly of medications used to treat serious conditions, such as
cancer. In these cases, there may be no alternative to taking the drug, with
the awareness that CMT symptoms may worsen.
top 
What Are the Different Types of CMT?
The many different types of CMT are distinguished by age of onset,
inheritance pattern, severity, and whether they're linked to defects in axon or
myelin.
While those distinctions are useful, it's important to realize that,
because of the vast number of genetic defects that can lead to CMT, some people
fall on the borders between different types of CMT, and many have specific
"subtypes" not detailed here.
(For more information about the genetics and inheritance of CMT, see
"Does It Run in the Family?")
CMT1 and CMT2
Onset: usually
childhood or adolescence
Inheritance: type 1, autosomal dominant; type
2, autosomal dominant or recessive
Features: These are the two most common forms
of CMT. (In fact, a subtype of CMT1 called CMT1A, caused by a defect in the PMP22 gene on chromosome 17, accounts for around 60 percent of all CMT cases.)
CMT1 is caused by demyelination and CMT2 is caused by axonopathy, but
both produce the classic symptoms described above.
CMT2 is sometimes associated with a treatable condition called restless
legs syndrome, an irresistible urge to move the legs while sitting or
lying down.
CMTX
Onset: childhood or
adolescence
Inheritance: X-linked
Features: CMTX has symptoms similar to those
of CMT1 and CMT2. Because of its linkage to the X chromosome, it often affects
males more severely than females.
CMT4
Onset: infancy,
childhood or adolescence
Inheritance: autosomal recessive
Features: CMT4, a demyelinating form of CMT,
causes weakness, usually mostly distal, but sometimes involving proximal
muscles. Sensory dysfunction can also occur. When CMT4 begins in infancy, it’s
characterized by low muscle tone. Young children with CMT4 generally have
delayed motor (movement-related) development.
Dejerine-Sottas Disease
Onset: early
childhood (generally before 3 years)
Inheritance: autosomal dominant or
recessive
Features: DS is sometimes classed
as a subgroup of CMT4 and is also sometimes called HMSN3. It’s a severe
neuropathy, with generalized weakness sometimes progressing to severe
disability, loss of sensation, curvature of the spine and sometimes mild
hearing loss.
Several of the genes that, when flawed, cause Dejerine-Sottas
disease, are the same genes that, when flawed in a different way, lead to
various forms of CMT.
Congenital Hypomyelinating Neuropathy (CHN)
Onset: congenital (at
or near birth)
Inheritance: autosomal recessive, spontaneous
Features: Unlike other types of CMT, CHN is
associated with reduced myelin formation (hypomyelination) from birth
rather than a breakdown of existing myelin. Both genetically and clinically,
it's similar to DS, but usually has an earlier onset and a nonprogressive or
slowly progressive course.
Many children with CHN grow up and experience gradual improvements in
strength.
Hereditary Neuropathy with Liability to Pressure Palsies (HNPP)
Onset: usually
adolescence.
Inheritance: autosomal dominant
Features: HNPP has an origin similar to that
of CMT1A (it's caused by a distinct defect in the PMP22 gene), but usually a
different manifestation.
Most people with HNPP have recurring attacks of palsy (paralysis)
or parasthesia (tingling) that are localized to a single limb and clear
up after several weeks. Often, these attacks are brought on by a compression
injury to the affected limb, but sometimes there's no obvious trigger. In other
people, HNPP is progressive and resembles CMT.
top 
How Is CMT Diagnosed?
A combination of lower leg weakness and foot deformities is a red
flag for CMT, but isn't sufficient for diagnosis. When a patient has those
symptoms, a well-trained neurologist will usually start with a physical exam to
look for further signs of distal weakness and sensory loss.
As a test for leg weakness, the neurologist might ask the patient to
walk on his heels, or to move part of his leg against an opposing force.
To look for sensory loss, the neurologist will usually test the
patient's deep tendon reflexes (like the knee-jerk reflex), which are
reduced or absent in most people with CMT.
During this initial evaluation, the neurologist will also ask about
the patient's family history. A family history of CMT-like symptoms, combined
with signs of nerve damage from the individual's physical exam, strongly point
to CMT or another hereditary neuropathy.
Lack of a family history doesn't rule out CMT, but might prompt the
neurologist to ask about diabetes, overexposure to certain drugs and other
potential causes of neuropathy.
Next, if the diagnosis is still consistent with CMT, the neurologist
may arrange for genetic testing. These tests, done by drawing a blood
sample, are designed to detect the most common genetic defects known to cause
CMT. Many, but certainly not all, of the genetic mutations underlying CMT can
be detected with a DNA blood test.
A positive genetic test result can provide a definite diagnosis and
useful information for family planning. But once again, a negative result
doesn't rule out CMT.
The neurologist may also perform a nerve conduction velocity test (NCV), which measures the strength and speed of electrical signals
transmitted through nerves.
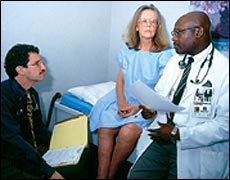 Doctors have
many tests for diagnosing CMT. Doctors have
many tests for diagnosing CMT. |
It's done by placing surface electrodes, similar to those used for
electrocardiograms, on the skin at various points over a nerve. One electrode
delivers a mild shock that stimulates an electrical response in the nerve, and
the others record this response as it travels through the nerve. (If necessary,
a topical anesthetic or sedative is used to ease discomfort caused by the
shocks.)
Delayed responses are a sign of demyelination and small responses are
a sign of axonopathy. Thus, NCV is often used to distinguish between CMT1 and
CMT2.
Other procedures sometimes used to diagnose CMT include electromyography (EMG), which measures the electrical signals in muscles, and less commonly, nerve
biopsy, which involves the removal and examination of a small piece of
nerve.
top 
Does It Run in the Family?
CMT can run in a family, even when there’s no obvious family history
of it. In part, this is because CMT can be inherited in three different ways
that aren’t always easy to trace through a family tree: X-linked, autosomal
dominant and autosomal recessive.
X-linked means that the genetic defect (or mutation) is
located on the X chromosome. In females, who have two X chromosomes, a normal
copy of the gene on one chromosome can often compensate (at least partially)
for the defective copy. Therefore, X-linked diseases usually affect males more
severely than females, because males only have one X chromosome. X-linked
diseases (like CMTX) cannot be passed from father to son.
Autosomal means the mutation occurs on a chromosome other than
the X or Y. Therefore, autosomal diseases affect males and females equally. Autosomal
recessive means that two copies of a defective gene are required for
the full-blown disease. One copy is inherited from each parent, neither of whom
would normally have the disease. Autosomal dominant means one copy of a
defective gene is enough to cause disease. In that case, a person who inherits
the defective gene from a parent will have the disease, as will the parent.
When CMT is passed on in an autosomal dominant pattern, it can be
easy to recognize in the family tree. In contrast, X-linked or autosomal
recessive types of CMT might seem to occur "out of the blue." But in reality,
the mother or both parents might be carriers who silently harbor a
genetic mutation. Many parents have no idea they're carriers of a disease until
they have a child with the disease.
CMT also can occur when a new mutation occurs during the child’s
conception. These are called spontaneous mutations, and after they
occur, they can be passed on to the next generation.
Your risk of inheriting or passing on CMT depends largely on what
type of CMT you have (see "What Are the Different Types of CMT?").
A good way to find out more about this risk is to talk to your MDA clinic
physician or a genetic counselor at the MDA clinic. Also, see MDA's pamphlet "Genetics
and Neuromuscular Diseases." |
top 
MDA's Search for Treatment and Cures
| MDA's Web site is constantly updated with the latest information about the neuromuscular diseases in its program. See the latest research news. |
In 1991, the genetic causes of CMT were completely unknown.
But just 10 years later, MDA-funded scientists had helped to identify 10
CMT-linked genes and found evidence for several others. This accomplishment has
led to genetic testing for many types of CMT, which has greatly
improved diagnosis.
Of equal importance, the ongoing hunt for CMT genes has given
insights into treatments that might be used to stop or reverse the
disorder. As the CMT gene hunt nears completion, MDA-funded scientists are
beginning to investigate how and why specific genetic mutations lead to
different types of CMT. In the future, this knowledge could enable physicians
to more accurately predict the course of CMT in individual patients.
In addition to genetic advances, MDA-funded scientists have made
significant progress in understanding the biology of axons and Schwann cells —
the cells that make myelin in the peripheral nerves. The
formation and maintenance of myelin seems to require a finely tuned interaction
between axons and Schwann cells, and within axons, there's an intricate
railroad-like system for transporting nutrients from one end to the other. Some
scientists hope to treat CMT by finding ways to improve axon-Schwann cell
interaction or axonal transport.
Other scientists are investigating gene therapy for CMT. With MDA
support, one group is developing a method to supply damaged nerves with genes
that encode neurotrophic factors, naturally occurring proteins that
stimulate nerve cell growth. This approach could perhaps be used to treat all
types of CMT, regardless of the underlying defect.
Another group has treated a small group of people with CMT1A with
neurotrophin 3, a neurotrophic factor, and found it improved sensory function.
Other lab studies involve blocking the hormone progesterone, and
giving high doses of ascorbic acid (vitamin C).
Still other scientists hope to treat CMT with stem cells —
primitive cells capable of generating specific cell types in the body. In
recent laboratory experiments, scientists have found efficient ways to turn
stem cells into nerve cells and myelin-producing cells, which might one day be
used to repair the damaged nerves in people with CMT.
top 
MDA Is Here to Help You
The Muscular Dystrophy Association offers a vast array of services to help you and your family deal with CMT or DS. The staff at
your local MDA office is there to assist you in many ways. The Association's
services include:
- a nationwide network of 220 hospital-affiliated clinics staffed by top neuromuscular disease specialists
- professionally facilitated support groups for those affected,
spouses or other caregivers
- assistance with purchase and repair of wheelchairs and leg braces,
and with purchase of communication devices
- evaluations for physical, occupational and respiratory therapy
- flu shots to help protect the respiratory system
- equipment loan closets
MDA's public health education program helps you to stay abreast of research news, medical findings and disability information related to
CMT. MDA's Web site at www.mda.org offers more than 3,000
pages of valuable information, including news and online chats.MDA publishes many brochures and booklets about living
with neuromuscular diseases, available in Spanish and English. Everyone
registered with MDA also receives Quest, MDA's
bimonthly national magazine.
If you have any questions about CMT or DS, someone at MDA will help you find the
answer.
|
top 
Facts About Charcot-Marie-Tooth Disease and Dejerine-Sottas Disease
|

Back to Disease Booklets
|