What Is Carotid Artery Disease?
Carotid (ka-ROT-id) artery disease is a condition in
which a fatty material called plaque (plak) builds up inside the carotid
arteries. You have two common carotid arteries—one on each side of your
neck—that divide into internal and external carotid arteries.
The internal carotid arteries supply oxygen-rich
blood to your brain. The external carotid arteries supply oxygen-rich blood to
your face, scalp, and neck.
Carotid Arteries
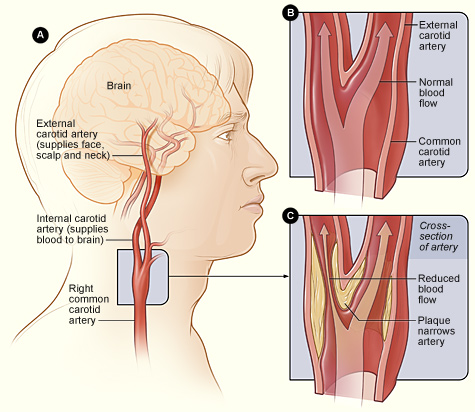
Figure A shows the location of the
right carotid artery in the head and neck. Figure B is a cross-section of a
normal carotid artery that has normal blood flow. Figure C show a carotid
artery that has plaque buildup and reduced blood flow.
Carotid artery disease can be very serious because
it can cause a
stroke, or “brain attack.” A stroke occurs when
blood flow to your brain is cut off.
If blood flow is cut off for more than a few
minutes, the cells in your brain start to die. This impairs the parts of the
body that the brain cells control. A stroke can cause lasting brain damage,
long-term disability, paralysis (an inability to move), or death.
Overview
When plaque builds up in arteries, the condition is
called
atherosclerosis
(ATH-er-o-skler-O-sis). Over time, plaque hardens and narrows the arteries.
This limits the flow of oxygen-rich blood to your organs and other parts of
your body.
Atherosclerosis can affect any artery in the body.
For example, when plaque builds up in the coronary (heart) arteries, a
heart
attack can occur. When plaque builds up in the carotid arteries, a stroke
can occur.
A stroke also can occur if blood clots form in the
carotid arteries. This can happen if, over time, the plaque in an artery cracks
or ruptures. Blood cells called platelets (PLATE-lets) stick to the site of the
injury and may clump together to form blood clots. Blood clots can partly or
fully block a carotid artery.
Also, a piece of plaque or a blood clot can break
away from the wall of the carotid artery. It can travel through the bloodstream
and get stuck in one of the brain’s smaller arteries. This can block
blood flow in the artery and cause a stroke.
Carotid artery disease may not cause signs or
symptoms until the carotid arteries are severely narrowed or blocked. For some
people, a stroke is the first sign of the disease.
Outlook
Carotid artery disease causes more than half of the
strokes that occur in the United States. Other conditions, such as certain
heart problems and bleeding in brain, also can cause strokes.
Lifestyle changes, medicines, and/or medical
procedures can help prevent or treat carotid artery disease and may reduce the
risk for stroke.
If you think you’re having a stroke, you need
urgent treatment. Call 9–1–1 right away if you have
symptoms of a stroke (don’t drive
yourself to the hospital). Getting care within 1 hour of having symptoms is
important.
You have the best chance for full recovery if
treatment to open a blocked artery is given within 6 hours of symptom onset.
Ideally, treatment should be given within 3 hours of symptom onset.
What Causes Carotid Artery Disease?
Carotid artery disease appears to start when damage
occurs to the inner layers of the carotid arteries. Major factors that
contribute to damage include:
When damage occurs, your body starts a healing
process. The healing may cause plaque to build up where the arteries are
damaged.
Over time, the plaque may crack. Blood cells called
platelets stick to the injured lining of the artery and may clump together to
form blood clots.
The buildup of plaque or blood clots can severely
narrow or block the carotid arteries. This limits the flow of oxygen-rich blood
to your brain and can cause a
stroke.
Who Is At Risk for Carotid Artery Disease?
Certain traits, conditions, or habits may raise your
risk for carotid artery disease. These conditions are known as risk factors.
The more risk factors you have, the more likely you are to get the disease. You
can control some, but not all, risk factors.
The major risk factors for carotid artery disease,
listed below, also are the major risk factors for
coronary
artery disease (CAD) and heart disease.
-
Unhealthy blood cholesterol levels. This includes high LDL cholesterol
(sometimes called bad cholesterol) and low HDL cholesterol (sometimes called
good cholesterol).
- High
blood pressure. Blood pressure is considered high if it stays at or above
140/90 mmHg over time.
- Smoking. This can damage and tighten blood
vessels, raise cholesterol levels, and raise blood pressure. Smoking also can
limit how much oxygen reaches the body's tissues.
- Older age. As you get older, your risk for
carotid artery disease goes up. About 1 percent of adults aged 50 to 59
have major plaque buildup in the carotid arteries. In contrast, 10 percent
of adults aged 80 to 89 have this problem. Before age 75, the risk is greater
in men than women. However, after age 75, the risk is higher in women.
- Insulin resistance. This condition occurs when
the body can't use its own insulin properly. Insulin is a hormone that helps
move blood sugar into cells where it's used. Insulin resistance may lead to
diabetes.
- Diabetes. With this disease, the body's blood sugar level is
high because the body doesn't make enough insulin or doesn't use its insulin
properly. People who have diabetes are four times more likely to have carotid
artery disease than people who don’t have diabetes.
-
Overweight or obesity. The most useful measure of overweight and obesity is
the body mass index (BMI). BMI measures your weight in relation to your height
and gives an estimate of your total body fat. A BMI between 25 and 29 is
considered overweight. A BMI of 30 or more is considered obese. You can check
your BMI using the National Heart, Lung, and Blood Institute’s
online BMI calculator, or your
doctor can check your BMI.
-
Metabolic syndrome. Metabolic syndrome is the name for a group of risk
factors that raise your risk for stroke and other health problems, such as
diabetes and heart disease.
- Lack of physical activity. Lack of activity can
worsen other risk factors for carotid artery disease.
- Family history of
atherosclerosis.
Having any of these risk factors doesn't mean that
you will get carotid artery disease. However, if you have one or more risk
factors, you can take steps to help prevent the disease.
Steps include following a healthy lifestyle and
taking any medicines your doctor prescribes. (For more information, see
“How Can Carotid Artery Disease Be
Prevented?”)
The amount of plaque buildup in the carotid arteries
also may suggest plaque buildup in other arteries. Doctors can predict the
degree of atherosclerosis in other arteries based on the thickness of the
carotid arteries. Thus, people who have carotid artery disease also are more
likely to have CAD.
What Are the Signs and Symptoms of Carotid Artery
Disease?
Carotid artery disease may not cause signs or
symptoms until it severely narrows or blocks the carotid arteries. Signs and
symptoms may include a bruit (broo-E), a transient ischemic attack (TIA), or a
stroke.
Bruit
During a physical exam, your doctor may listen to
your carotid arteries with a stethoscope. He or she may hear a whooshing sound
called a bruit. This sound may suggest changed or reduced blood flow due to
plaque. To find out more, your doctor may order tests.
Not all people who have carotid artery disease have
bruits.
Transient Ischemic Attack
For some people, having a TIA, or
“mini-stroke,” is the first sign of carotid artery disease. During
a mini-stroke, you may have some or all of the symptoms of a stroke. However,
the symptoms usually go away on their own within 24 hours.
The symptoms may include:
- Sudden weakness or numbness in the face or limbs,
often on just one side of the body
- The inability to move one or more of your limbs
- Trouble speaking and understanding
- Sudden trouble seeing in one or both eyes
- Dizziness or loss of balance
- A sudden, severe headache with no known cause
Even if the symptoms stop quickly, you should see a
doctor right away. Call 9–1–1 (don’t drive yourself
to the hospital). It’s important to get checked and to get treatment
started within 1 hour of having symptoms.
A mini-stroke is a warning sign that you’re at
high risk of having a stroke. You shouldn’t ignore these symptoms. About
one-third of people who have mini-strokes will have strokes if they don’t
get treatment.
Although a mini-stroke may warn of a stroke, it
doesn’t predict when a stroke will happen. A stroke may occur days,
weeks, or even months after a mini-stroke. In about half of the cases of
strokes that follow a TIA, the stroke occurs within 1 year.
Stroke
Most people who have carotid artery disease
don’t have mini-strokes before they have strokes. The symptoms of stroke
are the same as those of mini-stroke, but the results are not. A stroke can
cause lasting brain damage, long-term disability, paralysis (an inability to
move), or even death.
Getting treatment for a stroke right away is very
important. You have the best chance for full recovery if treatment to open a
blocked artery is given within 6 hours of symptom onset. Ideally, treatment
should be given within 3 hours of symptom onset.
Call 9–1–1 as soon as symptoms occur
(don’t drive yourself to the hospital). It’s very important to get
checked and to get treatment started within 1 hour of having symptoms.
Make those close to you aware of stroke symptoms and
the need for urgent action. Learning the signs and symptoms of a stroke will
allow you to help yourself or someone close to you lower the risk for damage or
death from a stroke.
How Is Carotid Artery Disease Diagnosed?
Your doctor will diagnose carotid artery disease
based on your medical history and the results from a physical exam and tests.
Medical History
Your doctor will find out whether you have any of
the major risk factors for carotid artery
disease. He or she also will ask whether you’ve had any
signs or symptoms of a
mini-stroke or
stroke.
Physical Exam
To check your carotid arteries, your doctor will
listen to them with a stethoscope. He or she will listen for a whooshing sound
called a bruit. This sound may indicate changed or reduced blood flow due to
plaque. To find out more, your doctor may order tests.
Diagnostic Tests
The following tests are common for diagnosing
carotid artery disease. If you have symptoms of a mini-stroke or stroke, your
doctor may use other tests as well.
Carotid Ultrasound
Carotid
ultrasound (also called sonography) is the most common test for diagnosing
carotid artery disease. It’s a painless, harmless test that uses sound
waves to create pictures of the insides of your carotid arteries. This test can
show whether plaque has narrowed your carotid arteries and how narrow they are.
A standard carotid ultrasound shows the structure of
your carotid arteries. A Doppler carotid ultrasound shows how blood moves
through your blood vessels.
Carotid Angiography
Carotid angiography (an-jee-OG-ra-fee) is a special type of x
ray. This test may be used if the ultrasound results are unclear or don’t
give your doctor enough information.
For this test, your doctor will inject a special
substance (called contrast dye) into a vein, most often in your leg. The dye
travels to your carotid arteries and highlights them on x-ray pictures.
Magnetic Resonance Angiography
Magnetic resonance angiography (MRA) uses a large magnet and
radio waves to take pictures of your carotid arteries. Your doctor can see
these pictures on a computer screen.
For this test, your doctor may give you contrast dye
to highlight your carotid arteries on the pictures.
Computed Tomography Angiography
Computed tomography (to-MOG-rah-fee), or CT, angiography takes
x-ray pictures of the body from many angles. A computer combines the pictures
into two- and three-dimensional images.
For this test, your doctor may give you contrast dye
to highlight your carotid arteries on the pictures.
How Is Carotid Artery Disease Treated?
Treatments for carotid artery disease may include
lifestyle changes, medicines, and medical procedures. The goals of treatment
are to stop the disease from getting worse and to prevent a
stroke.
Your treatment will depend on your symptoms, how
severe the disease is, and your age and overall health.
Lifestyle Changes
Making lifestyle changes often can help prevent
carotid artery disease or keep it from getting worse. For some people, these
changes may be the only treatment needed:
- Follow a healthy eating plan to prevent or lower
high
blood pressure and
high
blood cholesterol and to maintain a healthy weight.
- Increase your physical activity. Check with your
doctor first to find out how much and what kinds of activity are safe for you.
- If you're overweight or obese, lose weight.
- If you smoke, quit. Avoid exposure to secondhand
smoke.
Follow a Healthy Eating Plan
To help keep carotid artery disease from getting
worse, follow an eating plan that’s low in saturated and trans
fats, sodium (salt), and cholesterol. Therapeutic Lifestyle
Changes (TLC) and Dietary Approaches to Stop Hypertension (DASH) are two
examples of healthy eating plans.
TLC. Your doctor may recommend TLC
if you have high cholesterol. TLC is a three-part program that includes a
healthy diet, physical activity, and weight management.
With the TLC diet, less than 7 percent of your daily
calories should come from saturated fat. This kind of fat is mainly found in
meat and poultry, including dairy products. No more than 25 to 35 percent of
your daily calories should come from all fats, including saturated,
trans, monounsaturated, and polyunsaturated fats.
You also should have less than 200 mg a day of
cholesterol. The amounts of cholesterol and the different kinds of fat in
prepared foods can be found on the Nutrition Facts label.
Foods high in soluble fiber also are part of a
healthy eating plan. They help block the digestive tract from absorbing
cholesterol. These foods include:
- Whole grain cereals such as oatmeal and oat bran
- Fruits such as apples, bananas, oranges, pears,
and prunes
- Legumes such as kidney beans, lentils, chick
peas, black-eyed peas, and lima beans
A diet high in fruits and vegetables can increase
important cholesterol-lowering compounds in your diet. These compounds, called
plant stanols or sterols, work like soluble fiber.
Fish are an important part of a healthy diet.
They're a good source of omega-3 fatty acids, which help lower blood
cholesterol levels. Try to have about two fish meals every week. Fish high in
omega-3 fats are salmon, tuna (canned or fresh), and mackerel.
You also should try to limit the amount of sodium
that you eat. This means choosing low-sodium and "no added salt" foods and
seasonings at the table or when cooking. The Nutrition Facts label on food
packaging shows the amount of sodium in the item.
Try to limit drinks with alcohol. Too much alcohol
will raise your blood pressure and triglyceride level. (Triglycerides are a
type of fat found in the blood.) Alcohol also adds extra calories, which will
cause weight gain. Men should have no more than two drinks containing alcohol a
day. Women should have no more than one drink containing alcohol a day.
See the NHLBI’s
“Your
Guide to Lowering Your Cholesterol With TLC” for more information.
DASH. Your doctor may recommend the
DASH eating plan if you have high blood pressure. The DASH eating plan focuses
on fruits, vegetables, whole grains, and other foods that are healthy and lower
in salt/sodium.
This eating plan is low in fat and cholesterol. It
also focuses on fat-free or low-fat milk and dairy products, fish, poultry, and
nuts. The DASH eating plan is reduced in red meats (including lean red meat),
sweets, added sugars, and sugar-containing beverages. It's rich in nutrients,
protein, and fiber.
The DASH eating plan is a good healthy eating plan,
even for those who don’t have high blood pressure. See the NHLBI’s
"Your
Guide to Lowering Your Blood Pressure With DASH" for more information.
Increase Physical Activity
Regular physical activity can lower many carotid
artery disease risk factors, including LDL ("bad") cholesterol, high blood
pressure, and excess weight. Physical activity also can lower your risk for
diabetes and raise your levels of HDL cholesterol (the
“good” cholesterol that helps prevent plaque buildup).
Check with your doctor about how much and what kinds
of physical activity are safe for you. Unless your doctor tells you otherwise,
try to get at least 30 minutes of moderate-intensity activity on most or all
days of the week. You can do the activity all at once or break it up into
shorter periods of at least 10 minutes each.
Moderate-intensity activities include brisk walking,
dancing, bowling, bicycling, gardening, and housecleaning. More intense
activities, such as jogging, swimming, and various sports, also may be
appropriate for shorter periods.
See the NHLBI's
"Your
Guide to Physical Activity and Your Heart" for more information. Although
this guide focuses on heart health, it also applies to general health and
well-being.
Maintain a Healthy Weight
Maintaining a healthy weight can decrease risk
factors for carotid artery disease and stroke. Even a modest weight gain of a
few pounds a year can almost double your chances of having a stroke.
If you're overweight, aim to reduce your weight by 7
to 10 percent during your first year of treatment. This amount of weight loss
can lower your risk for carotid artery disease and other health problems.
After the first year, you may have to continue to
lose weight so you can lower your body mass index (BMI) to less than 25.
BMI measures your weight in relation to your height.
A BMI between 25 and 29 is considered overweight for adults. A BMI of 30 or
more is considered obese for adults. A BMI of less than 25 is the goal for
preventing and treating carotid artery disease.
You can find out your BMI using the NHLBI's
online calculator, or your
health care provider can measure your BMI.
For more information on losing weight and
maintaining your weight, see the Diseases and Conditions Index
Overweight
and Obesity article.
Quit Smoking
If you smoke or use tobacco, quit. Smoking can
damage your arteries and raise your risk for stroke and other health problems.
Talk to your doctor about programs and products that
can help you quit. The U.S. Department of Health and Human Services has
information on how to
quit smoking. Also, take steps to protect yourself from
secondhand smoke.
Medicines
You may need medicines to treat diseases and
conditions that damage the carotid arteries. High blood pressure, high blood
cholesterol, and diabetes can worsen carotid artery disease.
Some people can control these problems with
lifestyle changes. Others also need medicines to achieve and maintain control.
You may need antiplatelet (an-ty- PLATE-lit)
medicines to prevent blood clots from forming in your carotid arteries and
causing a stroke. Damage and plaque buildup make blood clots more likely.
Aspirin and clopidogrel are two common antiplatelet
medicines. They stop platelets from clumping together to form clots. These
medicines are a mainstay of treatment for people who have known carotid artery
disease.
Your health care team will help find a treatment
plan that’s right for you. Sticking to this plan will help avoid further
harm to your carotid arteries.
Procedures
You may need a medical procedure to treat carotid
artery disease. Doctors use one of two methods to open narrowed or blocked
carotid arteries.
Carotid Endarterectomy
This treatment is mainly for people whose carotid
arteries are blocked 50 percent or more.
For the procedure, a surgeon will make a cut in your
neck to reach the narrowed or blocked carotid artery. He or she will make a cut
in the artery and remove the plaque inside. The artery and your neck will then
be stitched up.
Carotid Endarterectomy
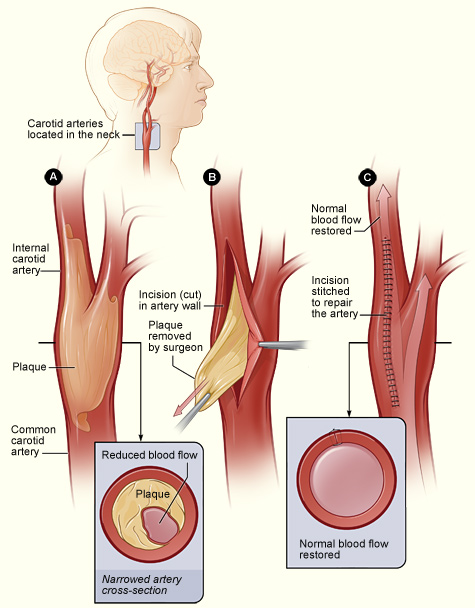
The illustration shows the process
of carotid endarterectomy. Figure A shows a carotid artery that has plaque
buildup. The inset image shows a cross-section of the narrowed carotid artery.
Figure B shows how the carotid artery is cut and the plaque removed. Figure C
shows the artery stitched up and normal blood flow restored. The inset image
shows a cross-section of the artery with plaque removed and normal blood flow
restored.
Carotid Artery Angioplasty and Stenting
Doctors use a procedure called
angioplasty (AN-jee-oh-plas-tee) to widen the carotid arteries
and restore blood flow to the brain.
A thin tube with a balloon on the end is threaded
through a blood vessel in your neck to the narrowed or blocked carotid artery.
Once in place, the balloon is inflated to push the plaque outward against the
wall of the artery.
A
stent
(a small mesh tube) is then put in the artery to hold the plaque back and keep
the artery open.
Carotid Artery Stenting
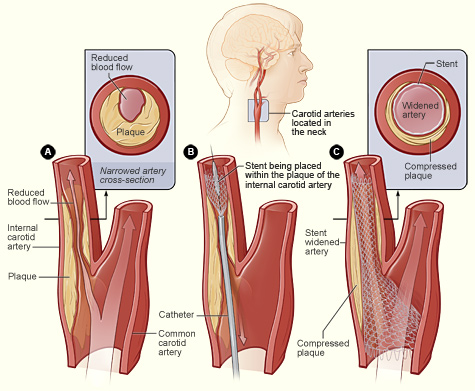
The illustration shows the process
of carotid artery stenting. Figure A shows an internal carotid artery that has
plaque buildup and reduced blood flow. The inset image shows a cross-section of
the narrowed carotid artery. Figure B shows a stent being placed in the carotid
artery to hold back plaque and keep the artery open. Figure C shows normal
blood flow restored in the stent-widened artery. The inset image shows a
cross-section of the stent-widened artery.
How Can Carotid Artery Disease Be Prevented?
Taking action to control your
risk factors can help prevent or delay
carotid artery disease and
stroke. The more risk factors you have, the more likely you
are to get carotid artery disease.
Making lifestyle changes and taking prescribed
medicines are important steps. For information on healthy eating plans,
physical activity, maintaining a healthy weight, and medicines, see
“How Is Carotid Artery Disease
Treated?”
Know your family history of health problems related
to carotid artery disease. If you or someone in your family has this disease,
be sure to tell your doctor. Also, let your doctor know if you smoke.
Living With Carotid Artery Disease
If you have carotid artery disease, you can take
steps to stop it from getting worse. Make lifestyle changes, follow your
treatment plan, and know the warning signs of
stroke.
Lifestyle Changes
For more information, see
“How Is Carotid Artery Disease
Treated?”
Treatment Plan
Following your treatment plan is important. It may
help prevent your carotid artery disease from getting worse. It also can lower
your risk for stroke and other health problems.
You may need to take medicines to control certain
risk factors and to prevent blood clots that could cause a stroke. Taking
prescribed medicines and following a healthy lifestyle can help control carotid
artery disease. However, they can’t cure the disease. You will likely
have to stick with your treatment plan for life.
Ongoing Care
If you have carotid artery disease, having ongoing
medical care is important.
Most people who have the disease will need to have
their blood pressures and blood cholesterol levels tested one or more times a
year. If you have
diabetes, you’ll also need routine blood sugar tests and
other tests.
Testing shows whether these conditions are under
control, or whether your doctor needs to adjust your treatment for better
results.
If you’ve had a stroke or procedures to
restore blood flow in your carotid arteries, you will likely need a yearly
carotid
Doppler ultrasound test. This test shows how well blood flows through your
carotid arteries.
Repeating this test over time will show whether the
narrowing or blockage in your carotid arteries is getting worse. Results also
can show how well procedures to treat your arteries have worked.
Follow up with your doctor regularly. The sooner
your doctor spots problems, the sooner he or she can prescribe treatment.
Stroke Warning Signs
Know the warning signs of a stroke and what to do if
they occur. The signs and symptoms of stroke may include:
- Sudden weakness or numbness in the face or limbs,
often on only one side of the body
- The inability to move one or more of your limbs
- Trouble speaking and understanding
- Sudden trouble seeing in one or both eyes
- Dizziness or loss of balance
- A sudden, severe headache with no known cause
Call 9–1–1 as soon as symptoms occur
(don't drive yourself to the hospital). It's very important to get checked and
to get treatment started within 1 hour of having symptoms.
You have the best chance for full recovery if
treatment to open a blocked artery is given within 6 hours of symptom onset.
Ideally, treatment should be given within 3 hours of symptom onset.
Make those close to you aware of stroke symptoms and
the need for urgent action. Learning the signs and symptoms of a stroke will
allow you to help yourself or someone close to you lower the risk for damage or
death from a stroke.
Key Points
- Carotid artery disease is a condition in which a
fatty material called plaque builds up inside the carotid arteries. You have
two common carotid arteries—one on each side of your neck—that divide
into internal and external carotid arteries.
- Plaque narrows the carotid arteries and limits
blood flow to the brain. It also makes it more likely that blood clots will
form in the carotid arteries. Blood clots can partly or fully block a carotid
artery.
- Carotid artery disease can be very serious
because it can cause a
stroke, or “brain attack.” A stroke occurs when
blood flow to your brain is cut off. If blood flow is cut off for more than a
few minutes, the cells in your brain start to die. This can cause lasting brain
damage, long-term disability, paralysis (an inability to move), or death.
- Carotid artery disease appears to start when
damage occurs to the inner layers of the carotid arteries. This causes your
body starts a healing process. The healing causes plaque to build up where the
arteries are damaged. Over time, the plaque may crack and cause blood clots to
form in the arteries.
- The major risk factors for carotid artery disease
are unhealthy
blood cholesterol levels,
high
blood pressure, smoking, older age, insulin resistance,
diabetes,
overweight
or obesity,
metabolic
syndrome, lack of physical activity, and a family history of
atherosclerosis.
- Carotid artery disease may not cause signs or
symptoms until it severely narrows or blocks the carotid arteries. Signs and
symptoms may include a bruit, transient ischemic attack (TIA), or a stroke. A
bruit is a whooshing sound your doctor may hear while listening to your carotid
arteries with a stethoscope. A TIA is a “mini-stroke.” During a
mini-stroke, you have some or all of the symptoms of a stroke. However, they
usually go away on their own within 24 hours.
- If you think you're having a stroke or
mini-stroke, you need urgent treatment. Call 9–1–1 (don't drive
yourself to the hospital). It's important to get checked and to get treatment
started within 1 hour of having symptoms.
- Your doctor will diagnose carotid artery disease
based on your medical history and the results from a physical exam and tests.
- Treatment for carotid artery disease may include
lifestyle changes, medicines, and medical procedures. The goals of treatment
are to stop the disease from getting worse and to prevent a stroke.
- Taking action to control your risk factors can
help prevent or delay carotid artery disease and stroke. Making lifestyle
changes and taking prescribed medicines are important steps. Know your family
history of health problems related to carotid artery disease.
- If you already have carotid artery disease, you
can take steps to stop it from getting worse. Making lifestyle changes,
following your treatment plan, and knowing the warning signs of stroke are
important.
Links to Other Information About Carotid Artery
Disease
NHLBI Resources
Non-NHLBI Resources
|

