
|
 |
 "Infection
Control for Viral Haemorrhagic Fevers "Infection
Control for Viral Haemorrhagic Fevers
In the African Health Care Setting"
Section 5. Disinfect Reusable Supplies and Equipment
This
section describes how to:
- Clean and disinfect
used gloves before reuse.
- Clean and disinfect
used medical instruments and supplies.
- Disinfect patient
waste and spills of infectious body fluids.
- Disinfect and
discard infectious waste and non-reusable supplies.
- Clean and disinfect
protective clothing, boots, and patients' sheets.
- Give first aid
for accidental exposures.
What to Disinfect:
Disinfection kills almost all bacteria, fungi, viruses, and protozoa.
It reduces the number of microorganisms to make equipment and surfaces
safer for use. When VHF is suspected in the health facility, all medical,
nursing, laboratory and cleaning staff should disinfect:
- *Hands and skin
after contact with a VHF patient or infectious body fluids
- Gloved hands after
contact with each VHF patient or after contact with infectious body
fluids (when gloves cannot be changed)
- Thermometers,
stethoscopes and other medical instruments after use with each VHF patient
- Spills of infectious
body fluids on the walls and floors
- Patient excreta
and containers contaminated by patient excreta
- Reusable supplies
such as protective clothing and patient bedding
- Used needles and
syringes.
*Note: All health
facility staff - including cleaning, waste disposal, and laundry staff
- who handle, disinfect, or clean VHF-contaminated supplies and equipment
should wear the same protective clothing as health care workers who provide
direct patient care. Wear thick gloves for the second pair of gloves.
Follow the steps in Section 4 for putting on
and taking off protective clothing.
| 5.1
Prepare Bleach Solutions |
 |
In a
central place in the health facility, prepare two solutions of ordinary
household bleach. Normally, ordinary household bleach has a 5.0% chlorine
concentration 7.
- 1:10 bleach solution
8 is a strong solution used to disinfect excreta and bodies. It
is also used to prepare the 1:100 bleach solution.
- 1:100 bleach solution
is used to disinfect 9: surfaces, medical equipment, patient
bedding, reusable protective clothing before it is laundered
- It is also recommended
for: rinsing gloves between contact with each patient, rinsing gloves,
apron, and boots before leaving the patient's room, and disinfecting
contaminated waste for disposal
Bleach
solutions must be prepared daily. They lose their strength after 24
hours. Anytime the odour of chlorine is not present, discard the solution.
Note:
1:10 bleach solution is caustic. Avoid direct contact with skin and eyes.
Prepare the bleach solutions in a well-ventilated area.
To
prepare bleach solutions:
- Gather the necessary
supplies:
- 1 container that
holds 10 measures (for example, 10 litres) to make the base 1:10 bleach
solution
- 1 large or several
smaller containers (1 for each station) with covers or lids to hold
the 1:100 bleach solutions. These containers should be a different colour
than the container holding the 1:10 bleach solution, or they should
be clearly labeled"1:100."
- Chlorine bleach
(for example, 1 litre of Javel)
- Clean water
- A measuring cup
or other container (for example, a bottle that holds 1 litre).
 |
Fig. 45. Marking
container for
mixing 1:10
bleach solutions |
- To prepare the
containers for mixing the bleach solutions, determine where to mark
the measurements for "9 parts" and "1 part" on each
container.
- Pour 9 measures
of water into the container. Mark a line where "9 parts" has
filled the container. For example, use a nail to scratch a line on a
metal or plastic bucket.
- Add 1 measure
of water to the first 9 parts. Using a nail, mark a line at the point
where the total volume has filled the container.
- To prepare 1:10
bleach solution:
- Fill the marked
container with water up to the mark for 9 parts.
- Then pour the
ordinary household bleach into the container up to the top mark.
 |
| Fig. 46. Preparing
bleach solutions |
- To prepare 1:100
bleach solution:
- Measure and pour
9 parts of water into the large container. Then measure and pour 1 part
of 1:10 bleach solution into the water to make 1:100 bleach solution.
- Distribute a container
to each station.
- Fill the container
at each station in the isolation area with the 1:100 bleach solution
as shown in Section 3.2.
- Place the remaining
1:10 bleach solution in the isolation area to disinfect spills and excreta.
|
|
Fig. 47.
Preparing bleach
solutions during an outbreak |
When there is
a large outbreak, make larger quantities of bleach solutions. Prepare
the disinfectants daily and distribute them as described in Section
3.
Remove the
disinfectants everyday or whenever the solutions become cloudy or
bloody. Replace the solution with a fresh supply. Safe disposal
of bleach solutions is described in Section
6.1.
If you cannot
smell chlorine in the bleach solution, the concentration is no longer
strong enough for disinfection. Replace the solution with a fresh
supply.
Make a schedule
for the cleaning staff so they know when to bring a fresh solution
into the isolation area, when to change them, and when to remove them.
7. The
recommendations in this section assume normal bleach solution has a 5%
chlorine concentration. Annex
8 contains a table describing quantities to use when preparing chlorine
solutions from other chlorine products.
8. This
is a solution with 0.5% chlorine concentration.
9. This
is a solution with 0.05% chlorine concentration.
| 5.2
Prepare Supply of Soapy Water |
 |
| |
|
 |
| Fig. 48. Small
piece of cake soap |
Prepare
a daily supply of soapy water.
- Gather the necessary
supplies:
- Ordinary cake
soap or powdered laundry detergent
- Supply of clean
water
- Large bucket
- Container for
measuring 1 litre
- Cut a small piece
of cake soap
- Mix one piece
of cake soap with 4 litres (1 gallon) of water.
- Make sure the
soap is well mixed with the water so there are suds. Pour into pan or
bucket for use in cleaning (see Section
3.3).
OR
- Mix powdered laundry
detergent according to instructions on packet
| 5.3
Disinfect Gloved Hands between Patients |
 |
Health
care workers should change outer gloves between each patient.
If there are not enough gloves to allow health care workers to change
to a new pair of outer gloves after examining or treating each patient,
disinfect gloved hands in 1:100 bleach solution after working with each
patient.
To
disinfect gloved hands:
- Place a bucket
of 1:100 bleach solution in the isolation room.
- If gloved hands
are visibly soiled, wash them first in soap and water.
- Dip the gloved
hands into the 1:100 bleach solution for 1 minute.
- Dry the gloved
hands with a one-use (or paper) towel, or let the gloved hands air-dry.
- If a bleach solution
is not available, wash gloved hands with soap and water.
- After several
rinses in bleach solution, the gloves may become sticky and will need
to be changed.
- If gloves will
be reused, place gloves in a bucket of soapy water. See Section
5.4 for instructions about washing used gloves. If gloves are not
going to be reused, discard them in the container for disposable infectious
waste.
| 5.4
Disinfect Used Gloves before Reuse |
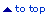 |
| |
|
 |
Fig. 49. Checking
gloves for holes |
Reusing gloves is
not recommended. If it is necessary to reuse gloves because the supply
in the health facility is limited, clean and disinfect them. Also check
them for holes. When cleaning staff handle contaminated supplies, make
sure they wear the same protective clothing as health care workers. They
should wear thick gloves as the second pair of gloves.
To clean and disinfect
gloves for reuse:
- Take the bucket
with soaking gloves to the VHF laundry area. Carefully move the gloves
to a bucket with fresh soapy water.
- Gently rub the
gloves to remove visible soiling and cover with water.
- Soak them overnight.
- Wearing at least
an apron and thick gloves, rinse the gloves in clean water. To check
for holes, fill each glove with rinse water. If any water squirts out,
there is a hole in the glove. Discard any gloves with holes.
- Air-dry the remaining
gloves.
- If available,
put talcum powder in dry gloves.
- Return clean gloves
to the storage shelf in the entry to the isolation area.
| 5.5
Disinfect Reusable Medical Instruments |
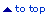 |
In the
isolation room, each time health care workers wash their hands between
patients, they should also disinfect thermometers and stethoscopes they
have used to examine the patient.
To
disinfect thermometers and stethoscopes with alcohol:
- 1. Use rubbing
alcohol (70% isopropyl).
- Place the alcohol
in a covered container and put it in the patient's room. Change the
alcohol at least once a week.
- Use a clean cloth
or paper towel and dip it in the alcohol solution.
- Carefully wipe
the thermometer with the alcohol solution and hold the cloth around
it for 30 seconds. Discard the cloth. Let the thermometer air-dry.
- Use another clean
cloth and dip it in the alcohol solution.
- Carefully wipe
the metal part of the stethoscope and hold the cloth against the surface
for 30 seconds. Let it air-dry.
- Discard the cloth
in the laundry container. Discard paper towels in the bucket for waste
to be burned.
To disinfect thermometers
and stethoscopes with bleach solution:
- 1. Place a covered
container of 1:100 bleach solution in the isolation room. Change the
bleach solution each day.
- Use a clean cloth
or paper towel and dip it in the bleach solution. Never dip a soiled
cloth back into the bleach solution. Use a cup or dipper to pour the
bleach solution on a soiled cloth.
- Wipe the thermometer
with the cloth soaked in bleach solution. Or, soak the thermometer for
10 minutes in the bleach solution. Let the thermometer air-dry.
- Use a clean cloth
or new paper towel and dip it in the bleach solution.
- Wipe the metal
part of the stethoscope with 1:100 bleach solution. Let it air-dry.
- Discard the cloth
in the laundry container. Discard paper towels in the bucket for waste
to be burned.
How to disinfect
and dispose of used needles and syringes is described in Sections
1.4 through 1.6.
| 5.6
Disinfect Bedpan or Waste Bucket |
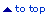 |
- Cover the contents
with 1:10 bleach. Empty the bedpan contents directly into the isolated
toilet or latrine.
- Clean the bedpan
with soap and water to remove solid waste. Pour into toilet or latrine.
Rinse the bedpan in 1:100 bleach solution and return it to patient's
room.
If a family member
is responsible for carrying out this task, make sure the family member
wears protective clothing.
| 5.7
Disinfect Patient's Utensils |
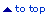 |
If families will
assist with patient care, provide 1:100 bleach solution and soap and water
so the family member can wash the patient's eating utensils. After washing
the utensils, rinse them in 1:100 bleach solution, and let them air-dry.
| 5.8
Disinfect Spills of Infectious Body Fluids |
 |
| |
|
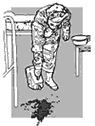 |
Fig. 50. Disinfecting
a spill on the floor |
Place a bucket containing
1:100 bleach solution in the isolation area.
To disinfect spills
of infectious body fluids:
- Use a cup or dipper
to pour bleach solution on spills. Cover the spill completely with 1:100
bleach solution. If the spill is heavy or dense, cover with 1:10 bleach
solution. Take care to prevent drops or splashes of the contaminated
body fluid from reaching anyone when pouring bleach solution on the
spill.
- Soak the spill
for at least 15 minutes.
- Remove the disinfected
blood or spilled material with a cloth soaked with 1:100 bleach solution.
- Discard any waste
in the container for collecting disposable infectious waste or in the
isolated latrine or toilet.
- Wash area as usual
with soap and clean water.
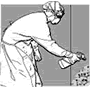 |
Fig. 51. Disinfecting
a spill on the wall |
To clean the walls
or other surfaces:
Surfaces such as
tabletops, sinks, walls and floors are not generally involved in disease
transmission. However, in a VHF patient's room, if walls are visibly soiled
with blood or other body fluids, clean them as follows 10:
- Use a sprayer
or mop to wash the walls with 1:100 bleach solution. Rinse the mop in
a fresh supply of 1:100 bleach solution. (If using a sprayer, apply
the spray close to the surface to minimize splashing and aerosols.)
- Wash the wall
as usual with soap and clean water to remove visible soil.
- Discard any waste
in container for collecting infectious waste or in the isolated latrine
or toilet.
10. Favero, MS, and
Bond, WW. Sterilization, disinfection, and antisepsis in the hospital.
In: Murray PR ed. Manual of Clinical Microbiology. Washington, D.C.: American
Society for Microbiology. pp. 183-200, 1991.
| 5.9
Disinfect Infectious Waste and Non-Reusable Supplies for Burning |
 |
Place a bucket or
other container containing 1:100 bleach solution in the patient's room.
Use it to collect infectious waste, contaminated items, and non-reusable
supplies that will be burned.
How to carry out safe waste disposal is described in Section
6.
| 5.10
Clean and Disinfect Protective Clothing |
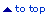 |
-
 |
Fig.
52. Transferring
laundry to the
cleaning area |
Set aside a special
part of the laundry or cleaning area for laundry from suspected VHF
patients. Make sure health facility staff who handle contaminated laundry
wear protective clothing, including thick gloves as the second pair
of gloves.
- Transfer laundry
as soon as possible to area set aside for VHF laundry.
- Carefully move
the laundry to a bucket with fresh 1:100 bleach solution.
- Soak laundry in
1:100 bleach solution for 30 minutes. Be sure that all items are completely
soaked.
- Remove items from
the bleach solution and place in soapy water.
- Soak overnight
in soapy water.
- Scrub thoroughly
to remove stains. Rinse and line-dry.
- Use a needle and
thread to repair any holes or torn areas.
- The clean clothing
is now ready for use. It can be ironed although this is not necessary.
(It is not necessary to wear protective clothing when ironing cleaned
clothing.
Items that are very
worn out should be discarded or used as cleaning rags.
| 5.11
Clean and Disinfect Boots |
 |
Place a sprayer or
pan with 1:100 bleach solution at the exit of the patient's room. Change
the pan often. Steps for disinfecting boots are described in Section
4.4.
| 5.12
Clean and Disinfect Patient's Bedding |
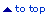 |
For plastic sheeting:
- If the plastic
sheeting becomes soiled during its use with the same patient, remove
liquid or solid waste with absorbent towels. Discard them in the container
for collecting infectious waste for burning. Then, wash the plastic
sheeting with 1:100 bleach solution.
- Change the plastic
sheeting between patients.
- If the plastic
sheeting cannot be changed between patients, wash it with 1:100 bleach
solution after each patient
 |
Fig.
53. Cleaning
patient's bedding |
For patient's
sheets:
- Remove sheets
from bed. Put them in a container (plastic bag or bucket) in the patient's
room.
- Take the container
directly to the laundry area.
- Soak in 1:100
bleach solution for 30 minutes. Be sure all items are completely soaked.
- Remove items from
the bleach solution and place them in soapy water. Soak overnight.
- Scrub thoroughly
to remove stains. Rinse and line-dry.
Mattresses:
If a mattress is
heavily soiled, remove it from the isolation area to the outdoors and
burn it. Make sure health facility staff wear protective clothing and
gloves when touching and carrying the soiled mattress.
If mattresses must
be reused:
- Pour 1:10 bleach
solution directly on the mattress. Let the solution soak through completely
to the other side.
- Flood the soiled
area with soapy water and rinse with clean water.
- Let the mattress
dry in the sun for several days.
- Turn the mattress
often so it dries on both sides.
| 5.13
Give First Aid for Accidental Exposures |
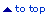 |
Accidental needlestick
injury: Assume any needlestick injury is a suspected contact for VHF
whether or not a break in the skin can be seen. If an accidental needlestick
injury occurs, treat the exposure site.
- Immerse the exposed
site in 70% alcohol for 20 to 30 seconds, and wash with soap and clean
water.
- Flush the site
in running water for 20 to 30 seconds.
- If needed, cover
with a dressing.
- Report the incident
to a supervisor or the physician-in-charge.
The purpose of notifying
the physician-in-charge is:
- To identify what
caused the problem
- To take corrective
action to solve the problem and prevent accidental transmission
- To provide appropriate
care for the possible case of VHF.
Remind the health
facility staff that accidents do happen even when every precaution to
prevent them has been taken. Reassure health facility staff that reporting
the accidental exposure will have no negative consequences. Explain that
reporting the accidental exposure is essential for protecting themselves,
their families, other health workers and patients.
Accidental contact
with infectious body fluids:
An accidental contact can occur if there is unprotected contact between
infectious body fluids and broken skin or the mouth, nose or eye. For
example, vomit may run under a glove, a patient might cough blood which
runs into the health care worker's eye, or coughed blood may run underneath
a health care worker's mask and get into the mouth. Treat any accidental
contact as a suspected contact with VHF. As soon as the contact occurs:
- Flush the area
in the most appropriate manner with soap and clean water. If a splash
occurs in the eye, flush it with clean water.
- Leave the isolation
area and remove the protective clothing as recommended.
- Take a shower
and put on street clothes.
- Report the exposure
to a supervisor or the physician-in-charge. Complete the necessary forms.
Follow up accidental
exposures:
- Monitor the condition
of the health facility staff. Take a measured temperature two times
per day.
- If a fever occurs
-- temperature is 38.5°C (101°F) or higher -- the health facility
staff should not do patient care activities. Treat as a suspected case
of VHF if the health facility staff's signs and symptoms meet the case
definition (Please see page 23 (section 2)and
Annex 4
|
 |
 |
 |
| Infection
Control For VHFs Manual |
|
|
 |
 |
|
| Sections
on this page |
|
|
 |
 |
|
|
 |

 "Infection
Control for Viral Haemorrhagic Fevers
"Infection
Control for Viral Haemorrhagic Fevers