|
|
|||||
|
|
On
This Page:
OverviewMalaria must be recognized promptly in order to treat the patient in time and to prevent further spread of infection in the community.
Malaria can be suspected based on the patient's symptoms and the physical findings at examination. However, for a definitive diagnosis to be made, laboratory tests must demonstrate the malaria parasites or their components. Diagnosis of malaria can be difficult:
Clinical DiagnosisClinical diagnosis is based on the patient's symptoms and on physical findings at examination. The first symptoms of malaria (most often fever, chills, sweats, headaches, muscle pains, nausea and vomiting) are often not specific and are also found in other diseases (such as the "flu" and common viral infections). Likewise, the physical findings are often not specific (elevated temperature, perspiration, tiredness). In severe malaria (caused by Plasmodium falciparum), clinical findings (confusion, coma, neurologic focal signs, severe anemia, respiratory difficulties) are more striking and may increase the suspicion index for malaria. Thus, in most cases the early clinical findings in malaria are not typical and need to be confirmed by a laboratory test.
Microscopic Diagnosis
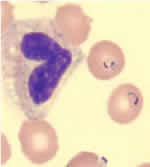
Malaria parasites can be identified by examining under the microscope a drop of the patient's blood, spread out as a "blood smear" on a microscope slide. Prior to examination, the specimen is stained (most often with the Giemsa stain) to give to the parasites a distinctive appearance. This technique remains the gold standard for laboratory confirmation of malaria. However, it depends on the quality of the reagents, of the microscope, and on the experience of the laboratorian. Alternate methods for laboratory diagnosis include: Antigen DetectionVarious test kits are available to detect antigens derived from malaria parasites. Such immunologic ("immunochromatographic") tests most often use a dipstick or cassette format, and provide results in 2-15 minutes. These "Rapid Diagnostic Tests" (RDTs) offer a useful alternative to microscopy in situations where reliable microscopic diagnosis is not available. Malaria RDTs are currently used in some clinical settings and programs. However, before malaria RDTs can be widely adopted, several issues remain to be addressed, including improving their accuracy; lowering their cost; and ensuring their adequate performance under adverse field conditions. The World Health Organization's Regional Office for the Western Pacific (WHO/WPRO) provides technical information, including a list of commercially available malaria RDTs, at http://www.wpro.who.int/rdt/. On June 13, 2007, the U.S. Food and Drug Administration (FDA) approved the first RDT for use in the United States. This RDT is approved for use by hospital and commercial laboratories, not by individual clinicians or by patients themselves. It is recommended that all RDTs are followed-up with microscopy to confirm the results and if positive, to quantify the proportion of red blood cells that are infected. The use of this RDT may decrease the amount of time that it takes to determine that a patient is infected with malaria.
Molecular DiagnosisParasite nucleic acids are detected using polymerase chain reaction (PCR). This technique is more accurate than microscopy. However, it is expensive, and requires a specialized laboratory (even though technical advances will likely result in field-operated PCR machines). Related Source: Molecular Diagnosis of Malaria and Babesiosis Other techniques related to malaria diagnosis are: SerologySerology detects antibodies against malaria parasites, using either indirect immunofluorescence (IFA) or enzyme-linked immunosorbent assay (ELISA). Serology does not detect current infection but rather measures past experience. Drug Resistance TestsDrug resistance tests are performed in specialized laboratories to assess the susceptibility to antimalarial compounds of parasites collected from a specific patient. Two main laboratory methods are available:
Page last modified : June 27, 2007 Content source: Division of Parasitic Diseases National Center for Zoonotic, Vector-Borne, and Enteric Diseases (ZVED)
|
|
||||||||||||||||||||||||||
| Home | Policies and Regulations | Disclaimer | e-Government | FOIA | Contact Us | ||||||
|