What Is Peripheral Arterial Disease?
Peripheral arterial disease (P.A.D.) occurs when
plaque (plak) builds up in the arteries that carry blood to your head, organs,
and limbs. Plaque is made up of fat, cholesterol, calcium, fibrous tissue, and
other substances in the blood.
When plaque builds up in arteries, the condition is
called
atherosclerosis
(ATH-er-o-skler-O-sis). Over time, plaque can harden and narrow the arteries.
This limits the flow of oxygen-rich blood to your organs and other parts of
your body.
P.A.D. usually affects the legs, but also can affect
the arteries that carry blood from your heart to your head, arms, kidneys, and
stomach. This article focuses on P.A.D. that affects blood flow to the
legs.
Normal Artery and Artery With Plaque
Buildup
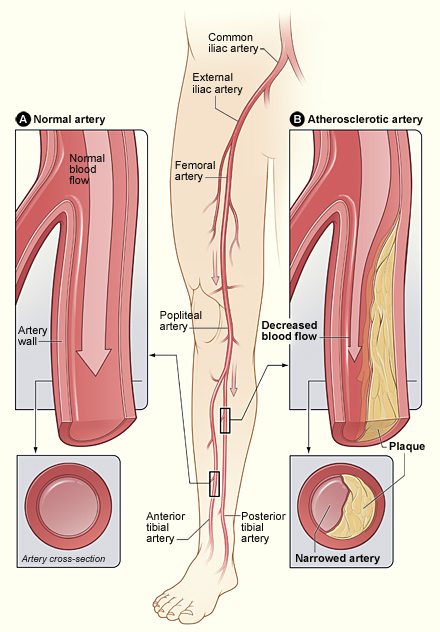
The illustration shows how P.A.D.
can affect arteries in the legs. Figure A shows a normal artery with normal
blood flow. The inset image shows a cross-section of the normal artery. Figure
B shows an artery with plaque buildup that’s partially blocking blood
flow. The inset image shows a cross-section of the narrowed artery.
Overview
Blocked blood flow to your legs can cause pain and
numbness. It also can raise your risk of getting an infection in the affected
limbs. It may be hard for your body to fight the infection.
If severe enough, blocked blood flow can cause
tissue death (gangrene). In very serious cases, this can lead to leg
amputation.
If you have leg pain when you walk or climb stairs,
talk to your doctor. Sometimes older people think that leg pain is just a
symptom of aging. However, the cause for the pain could be P.A.D. Tell your
doctor if you’re feeling pain in your legs and discuss whether you should
be tested for P.A.D.
Smoking is the main risk factor for P.A.D. If you
smoke or have a history of smoking, your risk for P.A.D. increases four times.
Other factors, such as age and having certain diseases or conditions, also
increase your risk.
Outlook
If you have P.A.D., your risk for
coronary
artery disease,
heart
attack,
stroke, and
transient ischemic attack (“mini-stroke”) is six
to seven times greater than the risk for people who don’t have P.A.D. If
you have heart disease, you have a 1 in 3 chance of having blocked leg
arteries.
Although P.A.D. is serious, it’s treatable. If
you have the disease, it’s important to see your doctor regularly and
treat the underlying atherosclerosis.
P.A.D. treatment may slow or stop disease progress
and reduce the risk of complications. Treatments include lifestyle changes,
medicines, and surgery or procedures. Researchers continue to explore new
therapies for P.A.D.
Other Names for Peripheral Arterial Disease
- Atherosclerotic peripheral arterial disease
- Peripheral vascular disease
- Vascular disease
- Hardening of the arteries
- Claudication
- Poor circulation
- Leg cramps from poor circulation
What Causes Peripheral Arterial Disease?
The most common cause of peripheral arterial disease
(P.A.D.) is
atherosclerosis.
The exact cause of atherosclerosis isn’t known.
The disease may start when certain factors damage
the inner layers of the arteries. These factors include:
When damage occurs, your body starts a healing
process. The healing may cause plaque to build up where the arteries are
damaged.
Over time, the plaque may crack. Blood cell
fragments called platelets stick to the injured lining of the artery and may
clump together to form blood clots.
The buildup of plaque or blood clots can severely
narrow or block the arteries and limit the flow of oxygen-rich blood to your
body.
Who Is At Risk for Peripheral Arterial
Disease?
Peripheral arterial disease (P.A.D.) affects 8 to 12
million people in the United States. African Americans are more than twice as
likely as Caucasians to have P.A.D.
The major risk factors for P.A.D. are smoking, age,
and having certain diseases or conditions.
Smoking
Smoking is more closely related to getting P.A.D.
than any other risk factor. Your risk for P.A.D. increases four times if you
smoke or have a history of smoking. On average, smokers who develop P.A.D. have
symptoms 10 years earlier than nonsmokers who develop P.A.D.
Quitting smoking slows the progress of P.A.D.
Smoking even one or two cigarettes a day can interfere with P.A.D. treatments.
Smokers and people who have
diabetes are at highest risk for P.A.D. complications,
including gangrene (tissue death) in the leg from decreased blood flow.
Age
As you get older, your risk for P.A.D. increases.
Genetic or lifestyle factors cause plaque to build in your arteries as you age.
About 5 percent of U.S. adults who are older than 50
have P.A.D. Among adults aged 65 and older, 12 to 20 percent may have
P.A.D. Older age combined with other risk factors, such as smoking or diabetes,
also puts you at higher risk.
Diseases and Conditions
A number of diseases and conditions can raise your
risk for P.A.D. These include:
What Are the Signs and Symptoms of Peripheral
Arterial Disease?
At least half of the people who have peripheral
arterial disease (P.A.D.) don't have any signs or symptoms of it. Others may
have a number of signs and symptoms.
Even if you don’t have signs or symptoms,
discuss with your doctor whether you should get checked for P.A.D. if
you’re:
Intermittent Claudication
People who have P.A.D. may have symptoms when
walking or climbing stairs. These may include pain, numbness, aching, or
heaviness in the leg muscles. Symptoms also may include cramping in the
affected leg(s) and in the buttocks, thighs, calves, and feet. Symptoms may
ease after resting.
These symptoms are called intermittent claudication
(klaw-de-KA-shen). During physical activity, your muscles need increased blood
flow. If your blood vessels are narrowed or blocked, your muscles won’t
get enough blood. When resting, the muscles need less blood flow, so the pain
goes away.
About 10 percent of people who have P.A.D. have
claudication. This symptom is more likely in people who also have
atherosclerosis
in other arteries.
Other Signs and Symptoms
Other signs and symptoms of P.A.D. include:
- Weak or absent pulses in the legs or feet
- Sores or wounds on the toes, feet, or legs that
heal slowly, poorly, or not at all
- A pale or bluish color to the skin
- A lower temperature in one leg compared to the
other leg
- Poor nail growth on the toes and decreased hair
growth on the legs
- Erectile dysfunction, especially among men who
have diabetes
How Is Peripheral Arterial Disease Diagnosed?
Peripheral arterial disease (P.A.D.) is diagnosed
based on your medical and family histories, a physical exam, and results from
tests.
P.A.D. often is diagnosed after symptoms are
reported. An accurate diagnosis is important, because people who have P.A.D.
are at increased risk for
coronary
artery disease (CAD),
heart
attack,
stroke, and
transient ischemic attack (“mini-stroke”). If you
have P.A.D., your doctor also may want to look for signs of these
conditions.
Specialists Involved
Primary care doctors, such as internists and family
practitioners, may treat people who have mild P.A.D. For more advanced P.A.D.,
a vascular specialist may be involved. This is a doctor who specializes in
treating blood vessel problems.
A cardiologist also may be involved in treating
people who have P.A.D. Cardiologists treat heart problems, such as CAD and
heart attack, which often affect people who have P.A.D.
Medical and Family Histories
To learn about your medical and family histories,
your doctor may ask:
- Whether you have any
risk
factors for P.A.D.
- About your symptoms, including any symptoms that
occur when walking, exercising, sitting, standing, or climbing
- About your diet
- About any medicines you take, including
prescription and over-the-counter medicines
- Whether anyone in your family has a history of
cardiovascular disease
Physical Exam
During the physical exam, your doctor will look for
signs and symptoms of P.A.D. He or she may check the blood flow in your legs or
feet to see whether you have weak or absent pulses.
Your doctor also may check the pulses in your leg
arteries for an abnormal whooshing sound called a bruit (broo-E). He or she can
hear this sound with a stethoscope. A bruit may be a warning sign of a narrowed
or blocked section of artery.
During the physical exam, your doctor may compare
blood pressure between your limbs to see whether the pressure is lower in the
affected limb.
He or she also may check for poor wound healing or
any changes in your hair, skin, or nails that may be signs of P.A.D.
Diagnostic Tests
Ankle-Brachial Index
A simple test called an ankle-brachial index (ABI)
is often used to diagnose P.A.D. The ABI compares blood pressure in your ankle
to blood pressure in your arm. This test shows how well blood is flowing in
your limbs. ABI can show whether P.A.D. is affecting your limbs, but it
won’t show which blood vessels are narrowed or blocked.
A normal ABI result is 1.0 or greater (with a range
of 0.90 to 1.30). The test takes about 10 to 15 minutes to measure both arms
and both ankles. This test may be done yearly to see whether P.A.D. is getting
worse.
Ankle-Brachial Index
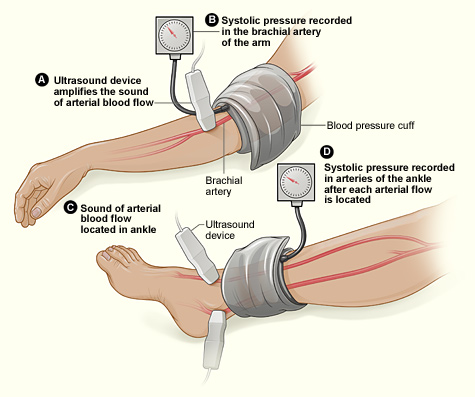
The illustration shows the ABI test.
The ABI compares blood pressure in the ankle to blood pressure in the arm. As
the cuff deflates, the blood pressure in the arteries is recorded.
Doppler Ultrasound
A Doppler ultrasound is a test that uses sound waves
to show whether a blood vessel is blocked. This test uses a blood pressure cuff
and special device to measure blood flow in the veins and arteries of the
limbs. A Doppler ultrasound can help find out how severe P.A.D. is.
Treadmill Test
A treadmill test can show how severe your symptoms
are and what level of exercise brings them on. For this test, you walk on a
treadmill. This shows whether you have any problems during normal walking.
You may have an ABI test done before and after the
treadmill test. This will help compare blood flow in your arms and legs before
and after exercise.
Magnetic Resonance Angiogram
A magnetic resonance angiogram (MRA) uses magnetic
and radio wave energy to take pictures of blood vessels inside your body. An
MRA is a type of
magnetic resonance imaging (MRI).
An MRA can find the location of a blocked blood
vessel and show how severe the blockage is.
If you have a
pacemaker,
man-made joint,
stent,
surgical clips, mechanical heart valve, or other metallic devices in your body,
you might not be able to have an MRA. Ask your doctor whether an MRA is an
option for you.
Arteriogram
An arteriogram provides a "road map" of the
arteries. It’s used to find the exact location of a blocked artery.
For this test, dye is injected through a needle or
catheter (tube) into an artery. This may make you feel mildly flushed. After
the dye is injected, an x ray is taken. The pictures from the x ray can show
the location, type, and extent of the blockage in the artery.
Some hospitals use a newer method of arteriogram
that uses tiny ultrasound cameras that take pictures of the insides of the
blood vessels. This method is called intravascular ultrasound.
Blood Tests
Your doctor may recommend
blood
tests to check for P.A.D. risk factors. For example, you may get a blood
test to check for
diabetes. You may also get a blood test to check your
cholesterol levels.
How Is Peripheral Arterial Disease Treated?
Treatments for peripheral arterial disease (P.A.D.)
include lifestyle changes, medicines, and surgery or procedures.
The overall goals of treating P.A.D. are to reduce
symptoms, improve quality of life, and prevent complications. Treatment is
based on your signs and symptoms, risk factors, and results from a physical
exam and tests.
Lifestyle Changes
Treatment often includes making long-lasting
lifestyle changes, such as:
- Quitting smoking. Your risk for P.A.D. increases
four times if you smoke. Smoking also raises your risk for other diseases, such
as coronary
artery disease (CAD). Talk to your doctor about programs and products that
can help you quit smoking.
- Lowering blood pressure. This lifestyle change
can help you avoid the risk of
stroke,
heart
attack,
heart
failure, and
kidney disease.
- Lowering
high
blood cholesterol levels. Lowering cholesterol can delay or even reverse
the buildup of plaque in the arteries.
- Lowering blood glucose levels if you have
diabetes. A hemoglobin A1C test can show how well you have
controlled your blood sugar level over the past 3 months.
- Getting regular physical activity. Talk with your
doctor about taking part in a supervised exercise program. This type of program
has been shown to reduce P.A.D. symptoms.
Follow a healthy eating plan that’s low in
total fat, saturated fat, trans fat, cholesterol, and sodium (salt).
Eat more fruits, vegetables, and low-fat dairy products. If you’re
overweight
or obese, work with your doctor to create a reasonable weight-loss plan.
The National Heart, Lung, and Blood
Institute’s
Therapeutic
Lifestyle Changes (TLC) and
Dietary
Approaches to Stop Hypertension (DASH) are two examples of healthy eating
plans.
Medicines
Your doctor may prescribe medicines to:
- Lower high blood cholesterol levels and
high
blood pressure
- Thin the blood to prevent clots from forming due
to low blood flow
- Help ease leg pain that occurs when you walk or
climb stairs
Surgery or Procedures
Bypass Grafting
Your doctor may recommend bypass grafting surgery if
blood flow in your limb is blocked or nearly blocked. For this surgery, your
doctor uses a blood vessel from another part of your body or a man-made tube to
make a graft.
This graft bypasses (goes around) the blocked part
of the artery, which allows blood to flow around the blockage. This surgery
doesn’t cure P.A.D., but it may increase blood flow to the affected
limb.
Angioplasty
Your doctor may recommend
angioplasty
(AN-jee-oh-plas-tee) to restore blood flow through a narrowed or blocked
artery.
During this procedure, a catheter with a balloon or
other device on the end is inserted into a blocked artery. The balloon is then
inflated, which pushes the plaque outward against the wall of the artery. This
widens the artery and restores blood flow.
A
stent
(a small mesh tube) may be placed in the artery during angioplasty. A stent
helps keep the artery open after angioplasty is done. Some stents are coated
with medicine to help prevent blockages in the artery.
Other Types of Treatment
Researchers are studying cell and gene therapies to
treat P.A.D. However, these treatments aren’t yet available outside of
clinical trials. For more information about clinical trials, see
"Links
to Other Information About Peripheral Arterial Disease."
How Can Peripheral Arterial Disease Be
Prevented?
Taking action to control your
risk factors can help prevent or delay peripheral
arterial disease (P.A.D.) and its complications.
Know your family history of health problems related
to P.A.D. If you or someone in your family has this disease, be sure to tell
your doctor.
If you smoke, quit. Smoking is more closely related
to getting P.A.D. than any other risk factor. Your risk for P.A.D. increases
four times if you smoke or have a history of smoking. Talk to your doctor about
programs and products that can help you quit smoking.
Follow a healthy eating plan that’s low in
total fat, saturated fat, trans fat, cholesterol, and sodium (salt).
Eat more fruits, vegetables, and low-fat dairy products. If you’re
overweight
or obese, work with your doctor to create a reasonable weight-loss
plan.
The National Heart, Lung, and Blood
Institute’s
Therapeutic
Lifestyle Changes (TLC) and
Dietary
Approaches to Stop Hypertension (DASH) are two examples of healthy eating
plans.
Get regular physical activity. Physical activity can
improve your fitness level and your health. Talk to your doctor about what
types of activity are safe for you. See the NHLBI's
"Your
Guide to Physical Activity and Your Heart." Although this guide focuses on
heart health, it also applies to general health and well-being.
These lifestyle changes can reduce your risk for
P.A.D. and help prevent and control conditions that can lead to P.A.D., such as
diabetes,
high
blood pressure,
high
blood cholesterol, heart disease, and
stroke.
Living With Peripheral Arterial Disease
If you have peripheral arterial disease (P.A.D.),
you’re also more likely to have
coronary
artery disease (CAD),
heart
attack,
stroke, and
transient ischemic attack (TIA, or "mini-stroke"). However,
you can take steps to treat and control P.A.D. and lower your risk for these
other conditions.
Living With Peripheral Arterial Disease
Symptoms
If you have P.A.D., you may feel pain in your calf
or thigh muscles after walking. Try to take a break and allow the pain to ease
before walking again. Over time, this may increase the distance that you can
walk without pain.
Talk with your doctor about taking part in a
supervised exercise program. This type of program has been shown to reduce
P.A.D. symptoms.
Check your feet and toes regularly for sores or
possible infections. Wear comfortable shoes that fit well. Maintain good foot
hygiene and have professional medical treatment for corns, bunions, or
calluses.
Ongoing Health Care Needs and Lifestyle
Changes
See your doctor for checkups as he or she advises.
If you have P.A.D., but don’t have symptoms, you should still see your
doctor regularly. Take all medicines as your doctor prescribes.
Lifestyle changes can help prevent or delay P.A.D.
and other related problems, such as CAD, heart attack, stroke, and TIA.
Lifestyle changes include quitting smoking, controlling risk factors, getting
regular physical activity, and following a healthy eating plan. For more
information on lifestyle changes, see "How Can
Peripheral Arterial Disease Be Prevented?"
Key Points
- Peripheral arterial disease (P.A.D.) occurs when
plaque builds up in the arteries that carry blood to the head, organs, and
limbs. When plaque builds up in arteries, the condition is called
atherosclerosis.
- Over time, plaque can harden and narrow the
arteries. This limits the flow of oxygen-rich blood to your organs and other
parts of your body.
- P.A.D. usually affects the legs, but also can
affect the arteries that carry blood from your heart to your head, arms,
kidneys, and stomach.
- Blocked blood flow to your legs can cause pain
and numbness. It also can raise your risk of getting an infection in the
affected limbs. It may be hard for your body to fight the infection. If severe
enough, blocked blood flow can cause tissue death (gangrene). In very severe
cases, this can lead to leg amputation.
- The most common cause of P.A.D. is
atherosclerosis. The exact cause of atherosclerosis isn’t known. The
disease may start when certain factors damage the inner layers of the
arteries.
- The major risk factors for P.A.D. are smoking,
age, and having certain medical conditions. Smoking is more closely related to
getting P.A.D. than any other risk factor. Your risk for P.A.D. increases four
times if you smoke.
- At least half of the people who have P.A.D.
don’t have any signs or symptoms of it. Some people who have P.A.D. may
have symptoms when walking or climbing stairs. These may include pain,
numbness, aching, or heaviness in the leg muscles. Symptoms also may include
cramping in the legs, buttocks, thighs, calves, and feet.
- P.A.D. is diagnosed based on your medial and
family histories, a physical exam, and results from various tests. An accurate
diagnosis is important, because people who have P.A.D. are at increased risk
for coronary
artery disease,
heart
attack,
stroke, and
transient ischemic attack. If you have P.A.D., your doctor
also may want to look for signs of these conditions.
- Treatments for P.A.D. include lifestyle changes,
medicines, and surgery or procedures. Treatment is based on your signs and
symptoms, risk factors, and results from a physical exam and tests.
- Taking action to control your risk factors can
help prevent or delay P.A.D. and its complications.
- You can take steps to treat and control P.A.D.
and lower your risk for complications. Talk to your doctor about taking part in
a supervised exercise program. This type of program has been shown to reduce
P.A.D. symptoms. Take good care of your feet and legs. See your doctor for
checkups as he or she advises, and take all medicines as your doctor
prescribes.
Links to Other Information About Peripheral
Arterial Disease
NHLBI Resources
Non-NHLBI Resources
Clinical Trials
|

