Rocking the Cradle
Phthalate Exposure in NICU Infants
|
Animal studies have linked di(2-ethylhexyl) phthalate (DEHP) with reproductive and developmental toxicity, and have demonstrated an especially pronounced effect on testicular development when administered postnatally. Previous research has shown that newborns treated at neonatal intensive care units (NICUs) may receive doses of DEHP at 2-3 times the average daily adult exposure, and that these infants have relatively high urinary levels of the DEHP metabolite mono(2-ethylhexyl) phthalate (MEHP). Now researchers, using urinary MEHP as a biomarker of DEHP exposure, demonstrate for the first time that the more DEHP-containing devices are used in treating an infant, the more DEHP makes its way into the infant's body [EHP 113:1222-1225].

|
Double jeopardy? Babies in neonatal intensive care units, already a high-risk group, are likely to have greater exposure to potentially harmful phthalates than other children.
image: Brand X |
Human DEHP exposure is widespread but generally much lower than the levels causing harm in animal studies. However, certain circumstances such as intensive medical treatment can result in higher-than-average exposure, which may be a particular risk for newborn males. DEHP is added to polyvinyl chloride (PVC) plastics for use in medical equipment including IV bags, blood bags, and various types of tubing, as well as many industrial and consumer PVC products. DEHP does not chemically link to PVC and leaches into fluids (such as blood and saline solution) that contact the plastic. The amount of leaching depends upon factors such as type of fluid, length of storage, and temperature.
The study involved 54 newborn girls and boys receiving treatment at two Boston-area NICUs between 1 March and 30 April 2003. The infants had been admitted for various reasons, and treatment included procedures such as mechanical ventilation, enteral feedings, and cardiac catheterization.
Prior to visiting the NICUs, the researchers defined low, medium, and high DEHP exposure categories based upon typical NICU procedures and equipment. Infants whose treatment consisted primarily of bottle and/or gavage feedings composed the low-exposure group. Infants in the medium-exposure group received more invasive therapies involving equipment such as an indwelling gavage tube or umbilical vein catheter. High-exposure infants experienced multiple and simultaneous invasive treatments, including endotracheal intubation and continuous umbilical vein catheterization.
One researcher visited the NICUs and observed each infant for 3-12 hours over the course of 1-3 days (more than one infant was observed at a time). During the observational visits, the researcher noted the equipment being used for each infant, then assigned the infant to an exposure group accordingly. At the end of each visit, urine samples were collected for MEHP measurement.
The researchers detected 10 phthalate metabolites in the samples, including 3 associated with DEHP, but focused on MEHP for data analysis since this metabolite is well studied and a proven biomarker of DEHP exposure. MEHP levels ranged from less than the level of detection to 758 nanograms per milliliter and did not vary substantially between multiple individual samples.
Between the two NICUs there were 13, 24, and 17 infants in the low-, medium-, and high-exposure groups, respectively. The researchers found that infants in the high-exposure group had MEHP levels five times higher than those in the low-exposure group. MEHP levels for medium-exposure infants were twice those of the low-exposure group.
The researchers indicate that the MEHP levels seen in this study are similar to those previously reported for NICU infants and higher than those reported for older children; no data are available for infants who did not need NICU care. The relevance of these exposures to health effects is unknown, and the researchers urge larger, more comprehensive studies with follow-up to determine consequences of DEHP exposure related to NICU treatment.
Julia R. Barrett
Arsenic and Prostate Cancer
Acquiring Androgen Independence
|
Scientists already suspect that prostate cancer, the second-leading cause of cancer death in U.S. men, is linked with chronic arsenic exposure. Now a team of researchers reports that human prostate cells that underwent chronic, low-level arsenic exposure not only exhibited aggressive carcinoma-like growth, but also showed an increased incidence of androgen independence, a state often linked to advanced or fatal prostate cancers, and one that makes these cancers more difficult to treat [EHP 113: 1134-1139].
Androgen, a sex hormone that stimulates and maintains masculine characteristics, is a necessary component in normal prostate function that can also encourage the survival and growth of prostate cancer. That is why some current treatments, such as pharmaceutical androgen blockers or removal of the testes, focus on making androgen less available to prostate cancer cells. However, some patients experience androgen independence, in which prostate cancer cells no longer need the male hormone to differentiate and grow out of control.
The mechanisms behind androgen independence are not completely understood, but scientists do know that this phenomenon sometimes occurs when androgen receptors go functionally awry. In some cases, the androgen receptors are "overexpressed," greatly increasing in number. In other cases, the receptors mutate, which can result in hyperresponsiveness to androgens. Still other receptor mutations allow nonandrogens (such as the estrogens) and even androgen inhibitors to stimulate cancer growth. Sometimes androgen receptors are bypassed completely, and cell growth is activated by other naturally occurring compounds including insulin-like growth factor-1, epidermal growth factor, and others.
In the current study, researchers examined the growth of normal and arsenic-transformed human prostate epithelial cells. The arsenic-transformed cells had been exposed continuously to sodium arsenite and, after 29 weeks of exposure, produced malignant tumors when inoculated into nude mice. Both cell lines were observed in two different media. One medium included the complete range of steroids, including ample amounts of androgen and growth factors. The other lacked normal amounts of sex hormones and growth factors.
The experiment showed that, consistent with malignant cell growth, prostate cells chronically exposed to arsenic grew more rapidly than control cells in both media. In the steroid-rich medium, the arsenic-transformed cells proliferated approximately twice as fast as the unexposed control cells. In the steroid-depleted medium, the arsenic-transformed cells proliferated about 2.5 times faster than control cells.
Arsenic exposure therefore appeared to be associated with the acquisition of androgen independence in prostate cells. However, the observed arsenic-induced androgen independence did not occur by any previously studied mechanism; it was not linked to overexpression of androgen receptors or receptor mutations that facilitate cell growth via nonandrogens.
A clue may lie in earlier experiments, in which the same researchers observed a marked increase in production of K-ras (an oncogene associated with prostate cancers) in arsenic-transformed cells. K-ras is a key part of a growth-stimulating pathway in the prostate that is stimulated by androgens. K-ras was clearly correlated with arsenic-induced carcinoma-like growth and androgen independence. The authors speculate here that arsenic may bypass the androgen receptor and directly cause aberrant K-ras activation.
John Tibbetts
Air Pollution in Space and Time
Birth Outcomes Are Complicated by Exposure Variations
|
The association between air pollution and adverse effects on human birth outcomes is drawing increasing attention worldwide. In one of the latest developments, two epidemiologists at the University of California, Los Angeles, have found that the typical use of air pollution data from fixed monitoring stations may be inadequate for accurately pinpointing the links between air pollution and birth outcomes [EHP 113:1212-1221]. They also corroborate earlier findings that timing of pollution exposures is significant and that studying different pollutant combinations substantially complicates analysis.

|
Born of necessity. A study of Los Angeles mothers shows that more detailed exposure information is critical for accurately drawing links between air pollution and adverse birth outcomes.
image: Photodisc |
Using new data in a follow-up on previous work, the researchers discovered that carbon monoxide (CO) and particulate matter (PM10) had significant adverse effects--and at concentrations well below U.S. federal standards--on preterm and low-birth-weight (LBW) births for women living within one mile of an air pollution monitoring station. However, they measured substantially less or no effect for women living just two to four miles away. They also found the effects were most pronounced in association with exposure during early and late gestation, but less apparent for the full pregnancy.
The researchers used state and county databases documenting births to mothers living in the Los Angeles area from 1994 to 2000. To analyze LBW at full term, they studied a zip code cohort of 136,134 births, of which 2,778 were LBW. To analyze preterm births, they used 106,483 of the same births (minus births by cesarean section), of which 9,268 were preterm. Data from 18 government air pollution monitors documented CO, PM10, nitrogen dioxide, and ozone levels. There were two years of data for fine particulate matter (PM2.5), but the researchers found that wasn't a long enough period to provide significant findings (although many other studies have found that PM2.5 is more of a health concern than PM10).
The researchers discovered that for the first trimester, the highest quartile of CO concentrations observed--never more than two-thirds of the U.S. Environmental Protection Agency (EPA) 8-hour standard--was associated with a 27% increase in risk of preterm birth for women living within one mile of a pollution monitoring station. Similar CO exposures and distances during the third trimester were associated with a 36% increase in LBW following a full-term pregnancy. Parallel effects were seen for PM10--which never exceeded two-thirds of the EPA 24-hour standard--early and late in pregnancy. This generally confirmed findings from an earlier study using data from 1989 to 1993. No significant relationships were seen for nitrogen dioxide or ozone.
The researchers were able to account for many potentially confounding factors, including maternal age, level of prenatal care, and infant's sex. However, they had no data for other factors known to influence birth outcomes, such as maternal occupation, height, weight, weight gain during pregnancy, and smoking status. Folding in such data could affect the outcome of this study, the team acknowledges. The team's finding that effect estimates diminished for women living farther than one mile from a station suggests that the air monitoring stations may not provide accurate measures of exposure for these women; development of ways to better capture spatial variability in pollutant concentrations is therefore an important goal.
The researchers concluded that improved air pollutant data reflecting both geographic variation and the specific substances in the ambient air mixture will lead to much better understanding of air pollutants on birth effects. Also important are the use of finer breakdowns of the pregnancy period and more detailed background information on the parents and child.
Bob Weinhold
When Lead Goes to Your Head
Genotype May Link Exposure and Meningioma
|
Scientists know very little about the causes of most brain tumors. A small percentage of cases can be explained by familial syndromes, or by exposure to ionizing radiation, but the precise roles of specific genes or other environmental factors, such as lead, remain largely unexplored. A research team now reports an association between a genetic variant for 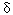 -aminolevulinic acid dehydratase (ALAD)--an enzyme involved in the synthesis of heme--and an increased risk of developing meningioma, a tumor that occurs in the membranes covering the brain and the spinal cord [EHP 113:1209-1211].
-aminolevulinic acid dehydratase (ALAD)--an enzyme involved in the synthesis of heme--and an increased risk of developing meningioma, a tumor that occurs in the membranes covering the brain and the spinal cord [EHP 113:1209-1211].

|
Chasing leads on brain tumors. Information on what causes brain tumors is fragmented; however, new data may tie together clues about lead exposure and a predisposition to develop meningioma.
image: Colorado Springs Imaging
|
Some previous studies suggested that people who carry an ALAD polymorphism known as ALAD2 tend to have higher concentrations of lead in their blood. Other research has indicated that occupational exposure to lead may increase the risk of meningioma. The findings of the current study suggest a possible link between these two results.
The team discovered a connection between ALAD2 and meningioma in a study of 573 patients with brain tumors from hospitals in Arizona, Massachusetts, and Pennsylvania. The patients were compared to 505 control subjects who were admitted to the same hospitals for conditions that did not involve tumors. Of the brain tumor patients, 151 had meningioma, 355 had glioma (a cancer that grows from glial cells in the brain), and 67 had acoustic neuroma (a tumor of the auditory nerve).
The ALAD genotype--based on the ALAD1 and ALAD2 alleles--was determined for each patient and each control subject. Possible links between the ALAD2 allele and the brain tumors were investigated using unconditional logistic regression.
The statistical analyses revealed that people who carried the ALAD2 allele (heterozygotes and homozygotes) were 1.6 times more likely than the ALAD1 homozygotes to develop meningioma. This modest but significant association was stronger in males, who were 3.5 times more likely to develop meningioma if they had the variant allele. However, the authors caution that their sample size may be too small to draw conclusions about gender-related effects. They saw no increased risk linked with the ALAD2 allele for glioma or acoustic neuroma.
These results raise the question of how the ALAD2 allele might increase the risk of meningioma. Previous work by the same team, based on the same study subjects, found an elevated risk of meningioma for occupational groups that may be exposed to lead, including auto body painters and industrial production supervisors. Certain other studies have shown that individuals who carry the ALAD2 allele have higher levels of lead in their blood. Together, these results suggest that lead may play a role in the link between the ALAD2 alleleand meningioma. The researchers recommend that future investigations should consider the combined effects of exposure to lead and the ALAD2 allele on the incidence of this cancer.
Michael Szpir





