
Breathing is something that most people take for granted. Without giving it a thought, we pull an invisible stream of gases, aerosols, particles, microbes, pollen, and dust into our lungs with every breath. But not everyone breathes easily. For the more than 14 million Americans with asthma, breathing becomes difficult when sensitive airways are inflamed and constricted. The number of people with asthma increased by 42% in the last decade, according to a recent report by the Centers for Disease Control. Not only is asthma becoming more prevalent, but it is also more severe. According to the National Heart, Lung, and Blood Institute, the number of people who die of asthma jumped 58% between 1979 and 1992. Emergency room visits and hospital admissions for asthma are increasing. Children, ethnic minorities, and the urban poor are at the greatest risk. Researchers suspect that a variety of factors such as air contaminants and heightened exposure to aeroallergens in airtight homes trigger bouts of asthma or cause chronic airway inflammation that may lead to permanent lung dysfunction.
What could be making a respiratory disease, triggered by an allergic response and aggravated by a multitude of factors, more common, more acute, and potentially more fatal?
The rising number of asthmatics might be attributed to increased awareness among physicians, said Gale Weinman of the National Heart, Lung, and Blood Institute (NHLBI). "Physicians may now be recognizing ailments previously diagnosed as a cold or bronchitis as the long-term, chronic illness of asthma. However, increased diagnosis of asthma cannot [totally] explain the rise in its prevalence," she said.
"We're looking at a disproportionate rise in the incidence and mortality of asthma in ethnic minorities and those living in poverty," said Darryl Zeldin, a clinical investigator of asthma in the NIEHS Laboratory of Pulmonary Pathobiology. "Most researchers believe that there must be some environmental component to that. In the lower socioeconomic groups, individuals are being exposed very early in life to allergens. Once sensitized, repeated exposure to these allergens leads to chronic airway inflammation and asthma. But most likely there are multiple factors."
More Common, More Deadly
When people with asthma encounter allergens, environmental irritants, cold air, or viral infections, a complex cascade of events leads to airway inflammation and constriction. As air is forced past smaller and constricted openings, asthmatics develop an audible wheeze, shortness of breath, chest pain, and often coughing. Long-term exposure to irritants without medical intervention can lead to permanent reductions in lung function, damage to lung tissue, severe breathing discomfort, and lower resistance to infection, according to the American Lung Association (ALA).
For the 70-75% of asthmatics who have allergic asthma, their respiratory systems have developed a very specific response to a specific allergens. Nonallergic asthmatics, on the other hand, may wheeze after exercising or taking aspirin, and show little sensitivity to allergens. Asthma and allergies appear to be inherited separately, but they are mysteriously associated. Most asthmatics can name at least one person in their family who has asthma or allergies. At least half of the people with asthma have allergic rhinitis, or inflammation of the nasal membranes, and 35% have atopic dermatitis, known as eczema.
Asthma is a more manageable disease than it was three decades ago. "The philosophy of asthma management has changed," said Peter Gergen, director of the Office of Epidemiology and Clinical Trials at the National Institute of Allergy and Infectious Diseases. "The role of inflammation in asthma became more accepted. The use of anti-inflammatory drugs and the monitoring of peak flow [a measure of the ability to exhale air from the lungs] has been increasing through the 1980s." Rather than focusing on asthma attacks already in progress, physicians emphasize prevention of wheezing and maintenance of optimal lung function, said Gergen. The National Asthma Education Program, sponsored by the NHLBI, has provided physicians and patients with guidelines for treating asthma and helped change their understanding and management of the disease.
Still, during the last three decades, asthma prevalence and morbidity in the United States has been rising. "The paradox of asthma is that we've had good treatment and quite adequate medications, and yet we're still having this problem," said Gergen. From 1982 to 1992, the number of people 5-34 years old who were afflicted with asthma increased by 52%, according to a recent CDC report. This seems to follow an earlier trend found by Gergen and associates in the 1970s, when asthma prevalence among 6-11 year olds increased by 58%.
Trends in Asthma Prevalence, 1982-1993

The increase in asthma is not unique to the United States. Asthma appears to be growing worse in other economically developed countries as well. In Great Britain, deaths and hospital admissions due to asthma doubled between 1979 and 1985. In Finland, the proportion of military recruits with asthma increased 20-fold between 1961 and 1989. Sweden and Denmark also saw increasing death rates from asthma through the 1970s.
Health statistics are only one measure of asthma's high cost. Health care expenses for asthma reach $6.2 billion per year, or nearly 1% of all U.S. health care expenses in 1985, according to a 1992 study by Kevin Weiss, director of research at the Rush Presbyterian St. Luke's Medical Center in Chicago, published in the New England Journal of Medicine. Of that amount, $1.6 billion was spent for inpatient hospital costs.
Asthma exacts an equally significant personal cost. Asthma is the number one cause of absenteeism for schoolchildren and a common reason for adult absenteeism from work. In 1985, adults with asthma lost nearly 3 million work days, at a cost of $285 million, according to an analysis by Weiss.
Though death from asthma is relatively rare, it is becoming more frequent. Asthma mortality in the United States declined by nearly 8% per year during the 1970s, but by 1977, the trend reversed, and the number of deaths due to asthma began to climb steadily, increasing about 6% per year. Asthma killed 1,674 Americans in 1977, but by 1991 the death rate had risen to 5,106 (from 0.8 to 2.0 per 100,000 people). Although most asthmatics who die of the disease are over 50 years old, rates of asthma death have increased in almost all age groups, according to Michael Sly, chairman of Allergy and Immunology at the Children's National Medical Center in Washington, DC.
Most asthma deaths occur in urban areas. In 1985, 21% of asthma deaths among 5-34 year olds occurred in New York City and Cook County, Illinois (which includes Chicago), where only 6.8% of the U.S. population in this age group resided, according to Weiss. David Lang and Marcia Polansky of the Hahnemann University Hospital reported in a 1994 study in the New England Journal of Medicine that a disproportionate number of the asthma deaths in Pennsylvania occurred in Philadelphia, where mortality was clustered in poorer neighborhoods.
Although some evidence suggests that asthma's death toll could be leveling off, the rising rate of hospital admissions and emergency room and doctor's office visits for asthma suggests that the disease is becoming more severe. Between 1965 and 1983, hospitalization rates for asthma increased by 50% in adults and over 200% in children. Approximately 4.5% more children were hospitalized for asthma each year from 1979 to 1987, Gergen and Weiss found.
Disproportionate Risk
Blacks, Hispanics, and people living in urban environments seem to be at the greatest risk for asthma. Using data on the U.S. population between 1976 and 1908 from the National Health and Nutrition Examination Survey, Gergen and co-workers found that asthma occurs more frequently in black children than in white, and more often in urban areas than rural ones. The prevalence of asthmas in these groups was not associated with gross family income, education level of the head of household, poverty index ratio, or crowding, the researchers found. In the 1980s, three times as many black children as white children under four were hospitalized because of asthma. Blacks 5-34 years of age are five times more likely to die of asthma than whites.
As depicted in a recent New York Times article about inhaler use in the South Bronx, Puerto Ricans in the United States suffer from asthma far more frequently than other ethnic groups. One in every five (20.1%) Puerto Rican children (6 months to 11 years) in the United States had asthma in 1982-1984, compared to 4.5% of Mexican-American, 8.8% of Cuban, 9.1% of black, and 6.5% of white children. Researchers have proposed that the high prevalence of asthma among Puerto Ricans could result from a possible genetic predisposition, or from the high rate of smoking among Puerto Rican women of childbearing age.
Blacks and Hispanics in Philadelphia had higher rates of death from asthma, but only in areas with higher poverty rates, according to Lang and Polansky. A study by Lawrence Wissow and colleagues at the Johns Hopkins University Hospital suggests that black children in Maryland are more likely to be hospitalized for asthma, but this tendency may be more strongly related to poverty than to race. The hospitalization rate for asthma in Maryland increased three times faster for blacks than for whites during the 1979-1982 period, but when poverty was considered as a factor, many of the racial differences in hospitalization rates disappeared. A higher proportion of children on Medicaid, or with no health insurance, were hospitalized for asthma than children with private health insurance.
Age-adjusted Death Rates for Asthma by Race, 1979-1992

These findings raise important questions about why the economically disadvantaged are at greatest risk of dying from asthma. "Poverty is associated with all sorts of diseases," said Gergen. "Poor people in the United States die more than the rich of all causes, and the gap is widening. General health is poorer, as well as access to medical care. Exposure, environmental quality of life, stress, and social factors all play a role," said Gergen.
Environmental Culprits
Spurred by the alarming statistics, researchers are focusing on direct exposures to allergens indoors where people are spending more of their time. Allergen levels are thought to be higher in less well-ventilated homes, where moisture accumulates, allowing mildew and molds to grow. Research shows that cumulative exposure to dust mites, which live in bedding, upholstery, and carpets, causes some people to develop allergic sensitivity, including asthma and airway hyperresponsiveness. The levels of cockroach antigen generally found in suburban homes are too low to sensitize individuals, but the 10-fold higher levels found in inner-city dwellings are enough to cause sensitization and appear to be associated with asthma.
"We're also concerned about second-hand tobacco smoke," said Alfred Munzer, pulmonary specialist at Washington Adventist Hospital and former president of the ALA. "There is increasing evidence that childhood exposure to environmental smoke can be a predisposing factor to developing asthma." The Harvard Six Cities Air Pollution Health Study demonstrated that in families where parents smoke, the frequency of coughing and wheezing in their children is increased by up to 30%. A 1986 study reported in the American Review of Respiratory Diseases that was conducted in Tecumseh, Michigan, showed parental smoking was associated with increased prevalence and risk of asthma in children.
Infants of women who smoke have higher levels of the antibody immunoglobin E (IgE) in umbilical cord blood compared to infants of nonsmokers, indicating an immune reaction. Whether children born to smoking mothers develop asthma pre- or postnatally is an unanswered question. The increase in asthma prevalence in western countries is correlated with more women of childbearing age smoking, according to a 1990 British study in the British Medical Journal.
Increasing asthma incidence cannot totally be explained by smoking in the United States, however. Between 1965 and 1990, cigarette smoking in the United States declined by 40%. Though the greatest number of smokers are 25-44 years of age, poorly educated, and live below the poverty level, according to statistics from the CDC's Office on Smoking and Health, the proportion of smokers in this group is also following a downward trend.


Young victims. Asthma is the number one cause of absenteeism among schoolchildren.
Photo Credit: National Collaborative Inner-City Asthma Study
The National Inner City Asthma Study (NICAS), underway in seven U.S. cities, sponsored by the National Institute of Allergy and Infectious Diseases (NIAID), may soon add to our understanding of the disease. During the first phase of NICAS, begun in 1991, health researchers surveyed people with asthma in selected cities to identify factors in their lives most strongly associated with asthma. These included access to medical care, the patient's understanding of the disease and its potential severity, and factors in the home that exacerbate asthma. Results are still being analyzed, but initial conclusions indicate that cockroach antigen is a more prevalent allergen in inner-city households than dust mite antigen.
In the second phase of NICAS, co-sponsored by the NIEHS, researchers will intervene to reduce allergen exposure inside inner-city residences. George Malindzak of the NIEHS is an administrator for the second phase, scheduled to begin this winter. "We know that some components of indoor air have a definite provocative effect on asthma," Malindzak said. "We're now looking into things that people with asthma can do for themselves to alleviate asthma episodes."
The NIEHS is involved in recommending ways to reduce dust mites and cockroaches and evaluating allergy symptoms and lung function in children who are susceptible to recurrent wheezing. NICAS data should provide some insight into the soaring asthma rates among the poor and minorities in inner cities.
Other studies are exploring the influence of a child's surroundings during the vulnerable first weeks and months of life. It is precisely during this period, scientists believe, that the environment of a child with a genetic predisposition can tip the scales toward developing a full-fledged allergy.
"Sensitization is the critical point," said Harvard School of Public Health researcher Douglas Dockery, who is working on another study funded by NIAID. "You have to have a combination of genetic factors which puts you at risk but also a challenge via environmental exposure that sensitizes you," said Dockery. Indeed, evidence suggests that increased exposure to dust mites in early life is associated with increased allergic responses and asthma.
Using a sample of newborn children whose parents have a history of asthma and allergies, Dockery and co-workers will follow the infants' health while monitoring their home exposure to dust mites, cockroaches, and other antigens. "Asthma is clearly a multifactorial process," said Dockery. "A lot of things could be contributing. I believe nutritional factors are important. There is also the whole maintenance issue and the need for empowerment of these people who have asthma and need appropriate clinical support."
In some urban areas, more than half of the children with asthma may receive all their medical care at the emergency room, and many are never diagnosed. "The fact that many inner-city asthmatics end up in the hospital shows that something is wrong with the treatment," said Gergen. The uninsured have poor access to long-range care programs that would provide help in managing the disease and preventing acute episodes.
Increasing awareness of asthma and improving treatment are the aims of the National Asthma Education Program, a major effort of the NHLBI since 1989. In addition to training professionals about asthma management, the program is working with communities and organizations to educate people about asthma, including school staff, teachers, and coaches.
Breathing Bad Air
"The consensus seems to be that the environment is playing a tremendous role in the increasing prevalence of asthma," said Munzer. In addition to the provocation of asthma by allergens, he says, "air pollution is a big factor."
The nation's air has improved dramatically in the past 25 years. Emissions of soot and smog-forming volatile organic compounds have decreased significantly in the United States since 1970 despite crowded highways where more vehicles are driven twice as many miles. Release of sulfur oxide has decreased by 30% since 1970. Between 1988 and 1993, overall industrial emissions of toxic compounds decreased by 39%.
The distribution of asthma in other countries also fails to implicate pollution as an aggravating factor. Some of the highest asthma mortality rates occur in Australia and New Zealand, which have excellent air quality. Asthma is more prevalent in rural areas of the Scottish highlands, which have some of the lowest ozone concentrations in the world, than in more urban and polluted parts of the United Kingdom, according to a recent report.
Several U.S. studies of air quality and respiratory disease have also come up empty-handed in linking asthma to air pollution. In a comparison of schoolchildren in the Six Cities Study, measurements of lung function and asthma prevalence did not differ significantly between cities in relation to air quality. Philadelphia's soaring numbers of asthma deaths from 1978 to 1991 were starkly contrasted with the city's declining average annual air pollutant levels in the study by Lang and Polansky.
In spite of overall improvements in air quality, many Americans are not breathing risk-free air, according to EPA Administrator Carol Browner. Almost 100 million people live in areas where the air does not meet national air quality standards. Eighty percent of Hispanics and 65% of blacks live in "nonattainment areas" for air standards. For more sensitive populations, like those with asthma, polluted air presents a daily challenge.
"It is clear that for people with asthma, episodes of air pollution will aggravate that preexisting condition, resulting in more symptoms, more use of medications, and more hospital visits," said Dockery. "We can show that it is related to day-to-day variations in air quality."
In the Six Cities Study, scientists found that the odds of having bronchitis increased with greater concentrations of fine particulates (particles less than 15 micrometers in diameter). Moreover, the 10% of children with asthma or persistent wheeze accounted for 42% of the bronchitis episodes.
Another study by Dockery and Harvard researcher C.A. Pope substantiated these findings. When fine particle concentrations reached the current air quality standard of 150 micrograms per cubic meter (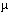 g/m3), schoolchildren experienced increased respiratory symptoms, and those with asthma doubled their use of asthma medications.
g/m3), schoolchildren experienced increased respiratory symptoms, and those with asthma doubled their use of asthma medications.
The question remains whether small particles in the atmosphere provoke asthma episodes. In Seattle, Washington, a study by Joel Schwartz of the Harvard School of Public Health and co-workers showed that the PM10 level (number of particles less than 10 micrometers in diameter) on the previous day was a significant predictor of the number of emergency room visits for asthma. At 30 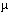 g/m3--the mean concentration of PM10 in Seattle during the study period--PM10 exposure appeared to be responsible for approximately 12% of the emergency visits for asthma, according to Schwartz.
g/m3--the mean concentration of PM10 in Seattle during the study period--PM10 exposure appeared to be responsible for approximately 12% of the emergency visits for asthma, according to Schwartz.
Higher PM10 levels in other communities also present a serious concern. In 1992, nearly one-fifth of Americans with asthma lived in areas where PM10 levels exceeded the national standard of 150 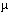 g/m3, and nearly one-half were exposed to levels exceeding 55
g/m3, and nearly one-half were exposed to levels exceeding 55 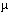 g/m3, according to the ALA.
g/m3, according to the ALA.
No one understands why small particles may provoke asthma. "Larger particles get trapped by our defense mechanisms, but these fine particles behave almost like a gas, going very deep into the lungs," said Munzer.
"It is puzzling that we observed the same effects--mortality, hospital admissions, aggravation of asthma, and reduced pulmonary function--associated with particles in Los Angeles, Philadelphia, and Steubenville, Ohio," said Dockery. "Clearly, the particles in these cities have a different chemical makeup, but all of the particles in the different communities come from combustion--whether from automobile engines, as in Los Angeles, from industry and power plants in Philadelphia, or from steel mills in Steubenville," he said.
In 1993, the ALA sued the EPA for failing to follow the Clean Air Act requirement to review the PM10 standard five years after its establishment in 1987. The EPA, now performing a review under a court-ordered schedule, is required to make recommendations by the end of January 1997. "If EPA tightens the current particulate standards, as recent scientific evidence suggests it should, potentially tens of thousands of hospitalizations, respiratory problems, and premature deaths can be avoided each year," said Ronald H. White, ALA director of environmental health.
Mark Utell, of the University of Rochester Medical Center and a member of the EPA's Clean Air Scientific Advisory Committee, which reviews EPA staff recommendations and PM10 criteria documents, believes that the toxicity of particulates should be more completely understood before standards are lowered. "There is no real toxicological basis for understanding how PM10 is linked with the epidemiological results. We need a stronger framework for understanding associations that occur with PM10, at concentrations as low as 30 micrograms per cubic meter," said Utell.
The ALA also sued the EPA for failing to review the federal ozone standard. The ALA estimates that the health of 2 million children under age 18 who have asthma is potentially at risk because they live in high-smog areas (ozone is the main component of smog). EPA staff scientists concede that a more stringent standard is needed to protect public health. In the second staff paper of the review, the agency has recommended that the old standard of 0.12 ppm be lowered to an average concentration of 0.07-0.09 ppm over an 8-hour time period, with 1-5 exceedances allowed per year.
Ozone is a powerful oxidant and respiratory irritant. Studies in recent years have linked ozone levels well below current U.S. health standards to a decline in lung function, respiratory symptoms, and increased hospital admissions and emergency room visits for respiratory problems. Other pollutants, such as sulfur dioxide, the main component of acid aerosols, and nitrogen dioxide, an indoor pollutant from gas stoves, clearly exacerbate asthma. Results of the Six Cities Study associated acid aerosols with respiratory symptoms, changed pulmonary function, and mortality.
"An important question is whether pollutant gases can enhance a person's susceptibility to being sensitized [to allergens]," said Paul Nettesheim, chief of the Laboratory of Pulmonary Pathobiology at the NIEHS. Animal studies have shown that ozone, sulfur dioxide, and components of diesel exhaust fumes irritate cells lining the airways and increase an animal's sensitivity to inhaled allergens. Irritation of the bronchi by pollutants like ozone could make it easier for antigens to penetrate the airway lining and reach lymphocytes and other cells involved in the allergic response, Nettesheim said.
David Peden, an investigator at the Center for Environmental Medicine and Lung Biology of the University of North Carolina at Chapel Hill School of Medicine, has examined how ozone exposure might exacerbate the response of people who are allergic to dust mites when they are in contact with the allergen. His results suggest that ozone would worsen the asthmatic response. But whether ozone exposure increases the likelihood of developing allergies in general is still open to question.
One study showed people with asthma to be more sensitive to ragweed pollen when they were exposed to substantial amounts of ozone. "One could say . . . if not for ozone, these people with asthma could make it all the way through the ragweed season without trouble," said Jane Koenig of the University of Washington School of Public Health, a co-author of the paper with Schwartz. "Then you have to ask, how does one decide what your main stimulus is to control? Ragweed would be hard to control. Ozone might be a little easier."
While many factors that provoke asthma, such as air pollution and cigarette smoking, are decreasing, the disease is becoming more prevalent. Its increasing severity is concentrated in urban pockets where children live under poor conditions, are frequently exposed to allergens and air pollution episodes, and have sporadic medical care. Research suggests that education, controlling exposure to antigens in the indoor environment, and improving urban air quality could improve the quality of life for these children.
Elaine Friebele
[Table of Contents]
Last Update: May 1, 1997





