

Peyronie’s Disease
On this page:
Peyronie’s disease, a condition of uncertain cause, is characterized by a plaque, or hard lump, that forms on the penis. The plaque develops on the upper or lower side of the penis in layers containing erectile tissue. It begins as a localized inflammation and can develop into a hardened scar.
Cases of Peyronie’s disease range from mild to severe. Symptoms may develop slowly or appear overnight. In severe cases, the hardened plaque reduces flexibility, causing pain and forcing the penis to bend or arc during erection. In many cases, the pain decreases over time, but the bend in the penis may remain a problem, making sexual intercourse difficult. The sexual problems that result can disrupt a couple’s physical and emotional relationship and lead to lowered self-esteem in the man. In a small percentage of patients with the milder form of the disease, inflammation may resolve without causing significant pain or permanent bending.
The plaque itself is benign, or noncancerous. A plaque on the top of the shaft (most common) causes the penis to bend upward; a plaque on the underside causes it to bend downward. In some cases, the plaque develops on both top and bottom, leading to indentation and shortening of the penis. At times, pain, bending, and emotional distress prohibit sexual intercourse.
One study found Peyronie’s disease in 1 percent of men. Although the disease occurs mostly in middle age, younger and older men can develop it. About 30 percent of men with Peyronie’s disease develop fibrosis (hardened cells) in other elastic tissues of the body, such as on the hand or foot. A common example is a condition known as Dupuytren’s contracture of the hand. In some cases, men who are related by blood tend to develop Peyronie’s disease, which suggests that genetic factors might make a man vulnerable to the disease.
Men with Peyronie’s disease usually seek medical attention because of painful erections and difficulty with intercourse. Since the cause of the disease and its development are not well understood, doctors treat the disease empirically; that is, they prescribe and continue methods that seem to help. The goal of therapy is to keep the Peyronie’s patient sexually active. Providing education about the disease and its course often is all that is required. No strong evidence shows that any treatment other than surgery is effective. Experts usually recommend surgery only in long-term cases in which the disease is stabilized and the deformity prevents intercourse.
A French surgeon, François de la Peyronie, first described Peyronie’s disease in 1743. The problem was noted in print as early as 1687. Early writers classified it as a form of impotence, now called erectile dysfunction (ED). Peyronie’s disease can be associated with ED; however, experts now recognize ED as only one factor associated with the disease—a factor that is not always present.
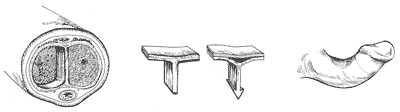
A cross-section of the penis (left) displays the internal cavity that runs the length of the penis and is divided into two chambers (corpora cavernosa) by a vertical connecting tissue known as a septum. It is believed that, during trauma such as bending, bleeding might occur at a point of attachment of the septum to tissue lining the chamber wall (center). The bleeding results in a hard scar, which is characteristic of Peyronie’s disease. The scar reduces flexiblility on one side of the penis during erection, leading to curvative (right).
[Top]
Course of the Disease
Many researchers believe the plaque of Peyronie’s disease develops following trauma (hitting or bending) that causes localized bleeding inside the penis. Two chambers known as the corpora cavernosa run the length of the penis. The inner-surface membrane of the chambers is a sheath of elastic fibers. A connecting tissue, called a septum, runs between the two chambers and attaches at the top and bottom.
If the penis is abnormally bumped or bent, an area where the septum attaches to the elastic fibers may stretch beyond a limit, injuring the lining of the erectile chamber and, for example, rupturing small blood vessels. As a result of aging, diminished elasticity near the point of attachment of the septum might increase the chances of injury.
The damaged area might heal slowly or abnormally for two reasons: repeated trauma and a minimal amount of blood flow in the sheath-like fibers. In cases that heal within about a year, the plaque does not advance beyond an initial inflammatory phase. In cases that persist for years, the plaque undergoes fibrosis, or formation of tough fibrous tissue, and even calcification, or formation of calcium deposits.
While trauma might explain acute cases of Peyronie’s disease, it does not explain why most cases develop slowly and with no apparent traumatic event. It also does not explain why some cases disappear quickly or why similar conditions such as Dupuytren’s contracture do not seem to result from severe trauma.
Some researchers theorize that Peyronie’s disease may be an autoimmune disorder.
[Top]
Diagnosis and Evaluation
Doctors can usually diagnose Peyronie’s disease based on a physical examination. The plaque is visible and palpable whether the penis is flaccid or erect. Full evaluation, however, may require examination during erection to determine the severity of the curvature. The erection may be induced by injecting medicine into the penis or through self-stimulation. Some patients may eliminate the need to induce an erection in the doctor’s office by taking a digital or Polaroid picture in the home. The examination may include an ultrasound scan of the penis to pinpoint the location and extent of the plaque and evaluate blood flow throughout the penis.
[Top]
Treatment
Because the course of Peyronie’s disease is different in each patient and because some patients experience improvement without treatment, medical experts suggest waiting 1 to 2 years or longer before attempting to correct it surgically. During that wait, patients often are willing to undergo treatments whose effectiveness has not been proven.
Experimental Treatments
Some researchers have given vitamin E orally to men with Peyronie’s disease in small-scale studies and have reported improvements. Yet, no controlled studies have established the effectiveness of vitamin E therapy. Similar inconclusive success has been attributed to oral application of para-aminobenzoate, a substance belonging to the family of B-complex molecules.
Researchers have injected chemical agents such as verapamil, collagenase, steroids, calcium channel blockers, and interferon alpha-2b directly into the plaques. These interventions are still considered unproven because studies included small numbers of patients and lacked adequate control groups. Steroids, such as cortisone, have produced unwanted side effects, such as the atrophy or death of healthy tissues. Another intervention involves iontophoresis, the use of a painless current of electricity to deliver verapamil or some other agent under the skin into the plaque.
Radiation therapy, in which high-energy rays are aimed at the plaque, has also been used. Like some of the chemical treatments, radiation appears to reduce pain, but it has no effect at all on the plaque itself and can cause unwelcome side effects. Although the variety of agents and methods used points to the lack of a proven treatment, new insights into the wound healing process may one day yield more effective therapies.
Surgery
Peyronie’s disease has been treated surgically with some success. The two most common surgical procedures are removal or expansion of the plaque followed by placement of a patch of skin or artificial material, and removal or pinching of tissue from the side of the penis opposite the plaque, which cancels out the bending effect. The first method can involve partial loss of erectile function, especially rigidity. The second method, known as the Nesbit procedure, causes a shortening of the erect penis.
Some men choose to receive an implanted device that increases rigidity of the penis. In some cases, an implant alone will straighten the penis adequately. In other cases, implantation is combined with a technique of incisions and grafting or plication (pinching or folding the skin) if the implant alone does not straighten the penis.
Most types of surgery produce positive results. But because complications can occur, and because many of the phenomena associated with Peyronie’s disease (for example, shortening of the penis) are not corrected by surgery, most doctors prefer to perform surgery only on the small number of men with curvature so severe that it prevents sexual intercourse.
[Top]
For More Information
American Urological Association
1000 Corporate Boulevard
Linthicum, MD 21090
Phone: 1–866–RING–AUA (746–4282) or 410–689–3700
Fax: 410–689–3800
Email: aua@auanet.org
Internet: www.urologyhealth.org
National Organization for Rare Disorders
55 Kenosia Avenue
P.O. Box 1968
Danbury, CT 06813–1968
Phone: 1–800–999–6673 or 203–744–0100
Fax: 203–798–2291
Email: orphan@rarediseases.org
Internet: www.rarediseases.org
[Top]
National Kidney and Urologic Diseases Information Clearinghouse
3 Information Way
Bethesda, MD 20892–3580
Phone: 1–800–891–5390
TTY: 1–866–569–1162
Fax: 703–738–4929
Email: nkudic@info.niddk.nih.gov
Internet: www.kidney.niddk.nih.gov
The National Kidney and Urologic Diseases Information Clearinghouse (NKUDIC) is a service of the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). The NIDDK is part of the National Institutes of Health of the U.S. Department of Health and Human Services. Established in 1987, the Clearinghouse provides information about diseases of the kidneys and urologic system to people with kidney and urologic disorders and to their families, health care professionals, and the public. The NKUDIC answers inquiries, develops and distributes publications, and works closely with professional and patient organizations and Government agencies to coordinate resources about kidney and urologic diseases.
Publications produced by the Clearinghouse are carefully reviewed by both NIDDK scientists and outside experts.
This publication is not copyrighted. The Clearinghouse encourages users of this publication to duplicate and distribute as many copies as desired.
NIH Publication No. 07–3902
September 2005
[Top]
|






