Traditionally a disease associated mostly with aging, cancer is even more devastating when it strikes the young. Families of children with cancer are often bewildered, asking difficult questions about what caused the disease and whether they are somehow responsible for what has happened to their child. Unfortunately, the science of epidemiology has not provided definitive answers to these wrenching questions, and while childhood cancer is by and large rare--accounting for only about 2% of all cancers diagnosed among all age groups--it is still the leading cause of disease-related death among children in the United States, afflicting approximately 8,000 children under the age of 15 annually. And despite the efforts of researchers to find a cure, childhood cancer rates also appear to be increasing at a rate of approximately 1% each year.
The rising trends appear to be most pronounced in the childhood cancers that are also most often diagnosed in the United States--leukemia and tumors of the central nervous system (CNS)--which, combined, account for roughly 50% of all cases. Both diseases are diagnosed most often among young children--leukemia in children under the age of two, and CNS cancers in children younger than five. These are also the age groups among which the trends of rising rates seem to be most pronounced. Data used to calculate national estimates of cancer incidence are drawn from the Surveillance, Epidemiology, and End Results (SEER) Program of the National Cancer Institute (NCI). Established in 1973, the SEER Program collects data on incidence, mortality, and patient survival from designated population-based registries in nine geographic locations. These locations include the states of Connecticut, Iowa, New Mexico, Utah, and Hawaii, and the metropolitan areas of Detroit, San Francisco, Seattle-Puget Sound, and Atlanta--areas that, all totaled, represent approximately 14% of the U.S. population. The SEER database contains information on two million cancers diagnosed between 1973 and 1994. Approximately 120,000 new cases are added annually.
Attempting to identify general trends in childhood incidence rates is a complex and difficult process. The rates vary widely by sex, age, race, nationality, and socioeconomic status. Also, because childhood cancer is so rare, statistical measures of incidence trends tend to fluctuate dramatically in response to small changes in yearly rates. Nevertheless, some major trends can be identified. For example, male children are generally diagnosed with cancer more often than females (although female rates are often higher than male rates among children under the age of 5), and incidence rates for blacks are, for the most part, lower than those for whites.
Of the childhood leukemias, by far the most common is acute lymphoblastic leukemia (ALL), which accounts for roughly 80% of all leukemias diagnosed in the United States. Based upon the most recent SEER data set (1973-1994), the incidence of ALL has been rising approximately 1.0% per year for all sexes and races combined. There is considerable racial variation in incidence rates for ALL, and rates among whites are almost twice those of blacks. According to Shelia Hoar Zahm, deputy chief of the occupational epidemiology branch at the NCI, rates of ALL in both sexes rose somewhat steadily until they peaked in 1989, but have since begun to decline, especially for males. Nonetheless, the recorded rate of increase among females was so dramatic in the 1970s and 1980s that, even with the recent decline, the number of cases in that sex since 1973 has increased by an estimated 32%.
 Second behind ALL, tumors of the CNS are the most commonly diagnosed childhood cancers. Most of these are brain tumors, particularly astroglial tumors that form on the interstitial cells and fibers of the nervous system. Analysis of SEER data from the period 1973-1994 indicates that the incidence of brain tumors in children of both sexes has been increasing at a fairly constant rate of approximately 2.0% per year, with an estimated overall increase since 1973 of 40.0%. Rates for white children are around 22% higher than those for blacks.
Second behind ALL, tumors of the CNS are the most commonly diagnosed childhood cancers. Most of these are brain tumors, particularly astroglial tumors that form on the interstitial cells and fibers of the nervous system. Analysis of SEER data from the period 1973-1994 indicates that the incidence of brain tumors in children of both sexes has been increasing at a fairly constant rate of approximately 2.0% per year, with an estimated overall increase since 1973 of 40.0%. Rates for white children are around 22% higher than those for blacks.
Some researchers suggest that rates for a number of other childhood cancers, such as Wilms' tumor and non-Hodgkin's lymphoma, may also be rising. However, it is difficult to quantify trends for these diseases because they are characterized by very small sample sizes that are statistically unstable and that yield estimates that vary widely from year to year. For example, the estimated increase in cancers of the kidney and renal pelvis since 1973 (of which the majority are Wilms' tumor) published by SEER in 1990, 1992, 1993, and 1994, are 27.5%, 13.3%, 16.8%, and 45.6%, respectively. "With the small number of cases upon which these percentages are based, all it takes is random variation in the rate to translate to a difference in incidence trends," says Leslie Robison, professor of pediatrics at the University of Michigan in Ann Arbor and holder of the Children's Cancer Research Fund chair in pediatric cancer at the University of Minnesota Cancer Center in Minneapolis.
Investigating Childhood
Cancer Clusters
While certainly no one wants an increase in the number of cancer cases, small sample sizes are the bane of those attempting to conduct epidemiological studies on some of the dozens of childhood cancer "clusters" reported every year. A cluster is a statistical term used to describe a population with an elevated incidence rate of a given disease occurring either at a particular point in time (temporal clustering) or place (spatial clustering). Usually, childhood cancer clusters exhibit both temporal and spatial clustering, meaning that there is a simultaneous and conspicuous rise in the number of cases in a specific location. Because childhood cancer is so rare, these apparent elevations beyond the expected number of cases are often statistically significant and often garner substantial media coverage, striking fear into the heart of the community and giving rise to speculation about potential environmental causes. Unfortunately, even though the public may rightfully insist upon immediate answers from public health officials, the small sample sizes and generally insufficient information on environmental exposures make it difficult for researchers to link a cluster with a specific hypothesized cause. Whether or not the cases in a cancer cluster are even related to the same exposure is a point of dispute among researchers. For example, Kenneth Rothman, editor of the journal Epidemiology , suggests in a paper published in the July 1990 issue of the American Journal of Epidemiology that cancer clusters may merely represent aggregates of "causally unrelated diseases . . . that for a number of reasons have been captured within similar time-space coordinates." This hypothesis is occasionally referred to as the "Texas sharpshooter" phenomenon, referring to a gunman who fires a shot at a barn and then paints a bull's-eye around the hole.
Nonetheless, clusters do point researchers in directions that they might not have previously considered; realistically, they may also provide the necessary political motivation to fund larger-scale studies. "The clusters give us direction and help us to form hypotheses," says Peggy Reynolds, chief of the environmental epidemiology and geographical information section of the California department of health services in Emeryville. "Based upon these hypotheses, we can then take a broader and more comprehensive look, using the best epidemiological tools that are available to us, to see if the exposures people are worried about might be implicated in these diseases."
To illustrate, Reynolds points to a large study of childhood cancer in farming versus nonfarming communities that was recently completed by her agency. This study was initially prompted by a reported cluster of mixed childhood cancers in McFarland, a predominantly rural community in California's Kern County, where it was thought that elevated rates of cancers might have been linked to exposure to agricultural pesticides. "The elevated cancer rates in McFarland were statistically significant, but it was hard to evaluate the small numbers, and it was unlikely that by any measurement we could bring together the causal agents," says Reynolds. "To pin down the association, we decided to take a broader look, and examined 400 cases from four counties in central California [Fresno, Kern, Kings, and Tulare counties] over an 8-year period." The study didn't identify a statistically significant difference in cancer incidence between children in farming versus nonfarming communities (in fact, slightly higher rates were observed among the more urban areas), but it did illustrate how cancer clusters can lead directly to additional research opportunities. James Blumenstock, assistant commissioner at the New Jersey department of health and senior services in Trenton, whose department is currently investigating a cluster of leukemia and brain tumor cases in Dover County, New Jersey, adds that the existence of a cluster frequently results in accelerated cleanup and closer monitoring of drinking water supplies. "Even though we may never be able to identify a cause, we are identifying problems and fixing them," he says. "The difficulty is in helping the community frame a reasonable expectation. We have to help them understand the limits of the science--that we may never be able to provide a 'yes' or 'no' answer [regarding the cause of the cluster]."
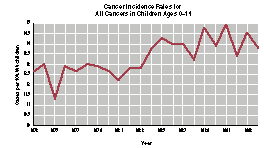
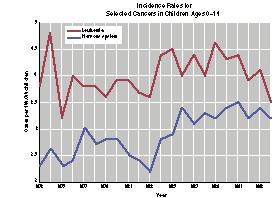
Source: Ries LAG, Kosary CL, Hankey BF, Miller BA, Harras A, Edwards BK (eds). SEER Cancer Statistics Review, 1973-1994, NIH Pub. No. 97-2789. Bethesda, MD: National Cancer Institute, 1997.
A name that has become synonymous with cancer clusters is Woburn, Massachusetts, where the rate of childhood leukemia mysteriously rose to four times the national average between 1966 and 1986. This cluster eventually led to a lawsuit and a subsequent trial that pitted the families of the young victims against W.R. Grace and Beatrice Foods, the two companies they accused of contaminating local wells with trichloroethylene (TCE), a chemical solvent that the families believe caused their children's illnesses. According to Robert Korr, deputy director for epidemiology at the bureau of environmental health assessment in Boston, Massachusetts, the most recent epidemiological investigations into the Woburn cluster identified a statistically significant association between the incidence of ALL and maternal consumption of water from two contaminated wells. There was no association between childhood consumption of the water and increased cancer risk, however. According to Korr, the wells were also contaminated with a variety of other solvents and heavy metals in addition to TCE.
Environmental Factors
The most frequently proposed causes of cancer in children are similar to those cited for adults: genetic abnormalities, ultraviolet and ionizing radiation, electromagnetic fields (EMFs), viral infections, certain medications, food additives, tobacco, alcohol, and a number of industrial and agricultural chemicals. The interplay between genetics and environmental exposures is thought to be a critical factor, and, according to Robison, genetically predisposed children may represent a unique subpopulation that is particularly sensitive to the cancer-causing properties of carcinogenic substances.
The best established environmental cause of childhood cancer is ionizing radiation, and both in utero and postnatal exposures have been linked to elevated childhood cancer rates. High-dose exposures such as those experienced by atomic bomb survivors and children receiving radiation therapy have been associated with elevated rates of ALL, acute myelogenous leukemia (AML), osteosarcoma, thyroid cancer, and soft-tissue sarcoma. However, the link to low-dose exposures is less clear and plagued by conflicting findings. The most compelling evidence for a link to low-dose exposures is an association between childhood cancer and prenatal exposures to diagnostic X rays. In a study published in the 28 February 1985 issue of the New England Journal of Medicine , E.B. Harvey and colleagues at the radiation branch of the NCI reported that the incidence of leukemia among twins X-rayed to determine fetal position was twice that of twins who were not X-rayed. Studies of other low-dose radiation exposures--exposure to low-level radioactive fallout, residing near a nuclear power plant, and having parents who work at a nuclear facility--have not been unequivocally linked to elevated cancer incidence in children.
Likewise, the highly controversial link between cancer and low-level EMFs has been increasingly discounted in the years since Nancy Wertheimer at the University of Colorado Health Science Center and physicist Ed Leeper, in an article published in the March 1979 issue of the American Journal of Epidemiology , first suggested that children residing in homes near certain "high current wiring configurations," or wire codes (the distribution patterns of residential power lines), were at increased risk of developing childhood leukemia. Dozens of subsequent studies demonstrated weak or equivocal associations between cancer incidence and proximity to high-voltage power lines, further fanning the public's fear that unseen electromagnetic waves were invading their homes and making them sick. But most of these studies had some serious limitations. For example, many simply used estimates of EMFs based on wire codes rather than direct measurements of EMFs in the home, and there was frequent significant recall bias with respect to exposure.
More recent studies appear to be downplaying the EMF connection. In the largest and most comprehensive study conducted to date on EMFs and leukemia, published in the 3 July 1997 issue of the New England Journal of Medicine , Martha Linet, an epidemiologist with the radiation branch of the NCI, and colleagues found little association between EMFs and elevated cancer incidence. This study, conducted as a joint research project between the NCI and the Children's Cancer Group (CCG), a multi-institutional research and treatment organization headquartered in Arcadia, California, had several strengths: it was large (629 children with leukemia and 619 controls), and it was based on direct measurements of EMFs in houses and schools taken by technicians who were blind to the disease status of the cases and controls. Additionally, the study also controlled for a wide range of potentially confounding variables, including maternal X ray exposure and socioeconomic status.
Linet cautions that it may be premature to draw any definitive conclusions from the results of this study. "We're still waiting on the results of two large nationwide studies evaluating EMFs and childhood cancer," she says, "one in the United Kingdom headed by Sir Richard Doll, a professor emeritus at Oxford University, and another in Canada being led by Mary McBride and others from the Cancer Control Agency of British Columbia. The results of these studies should be available next year."
David Savitz, an epidemiologist at the University of North Carolina at Chapel Hill School of Public Health, is also reluctant to completely dismiss the association with EMFs. "The studies have gotten better and better, and it appears that the associations [with childhood leukemia and EMFs], especially those based upon wire coding schemes, are nonexistent," he says. "However, for measured fields, the picture is not so clear. Either there is no association or we just can't see what is going on yet."
A remarkable aspect of the epidemiology of ALL is that it is considered by many to be a disease of affluence, in which elevated rates of the disease correlate with increasing socioeconomic status. This observation is borne out by the substantially higher rates of ALL in developed versus underdeveloped nations, and the fact that whites have dramatically higher incidence rates for the disease than do blacks. The most striking increases have been seen following periods during which populations from different geographic regions have mixed (such as urban migrations), providing the basis for a hypothesis that ALL may constitute a rare response to an as-yet unknown viral infection. This idea has a long history; the theory was discarded when it was discovered that leukemia is not contagious, and more recently was resurrected when it was found that spontaneous leukemia in domesticated animals such as cats, chickens, and cattle is viral in nature. In an article published in the 1 February 1997 issue of The Lancet , Mel Greaves, a professor at the Institute of Cancer Research in London, proposes that children in developed countries are less able to ward off common infections because they have been denied some of the "early first exposures" to viruses and bacteria that prime the infant immune system. On the other hand, children in underdeveloped countries have increased resistance conferred upon them by breast-feeding (which occurs more often in underdeveloped nations and is the source of some of the infants' first exposure to infectious agents), multiple social contacts, and an overall considerably less hygienic environment. Thus, leukemia could paradoxically be included in a group of viral illnesses linked to improved hygiene, a group that also includes polio and infectious mononucleosis, among other diseases. In more affluent societies, the mother may also have reduced immunity to certain viruses, which she may contract and then pass on to the infant during pregnancy.
Foremost in the minds of many is the idea that childhood cancer may be related to exposures to environmental chemicals. Addressing the conspicuous absence of information on chemical exposures and toxicity relating to children has become a priority at the EPA. An executive order issued by the Clinton administration in April 1997 directed the EPA and other federal agencies to explicitly consider children's health when setting standards for pesticide residues in food and for contaminants in water and air. This executive order came on the heels of the 1996 Food Quality Protection Act, under which tolerances for over 9,000 pesticides and other chemicals are being reevaluated so as to ensure that childhood exposures are addressed in the standard-setting process.
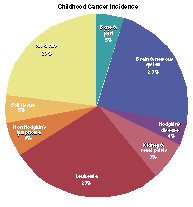 |
| Source: Ries LAG, Kosary CL, Hankey BF, Miller BA, Harras A, Edwards BK (eds). SEER Cancer Statistics Review, 1973-1994, NIH Pub. No. 97-2789. Bethesda, MD: National Cancer Institute, 1997. |
Children may potentially be exposed to carcinogenic compounds via maternal transfer in the womb, and also by drinking contaminated water and ingesting pesticide residues on fruits and vegetables. "Pound for pound, children breathe more air, drink more water, and eat more food than adults," says Philip Landrigan, scientific advisor to the administrator at the EPA's Office of Children's Health Protection (OCHP), and chair of the Mount Sinai Medical Center department of community medicine in New York City. "Thus, they are more heavily exposed to toxins present in those media. Children's exposures are further enhanced by their playing close to the ground and their normal hand-to-mouth activity," he says. Landrigan was chair of a committee that drafted a 1993 National Research Council report, Pesticides in the Diets of Infants and Children , which has had considerable influence on the Clinton administration's environmental policies.
Many studies have suggested a link between a number of childhood cancers-- including leukemia, lymphoma, neuroblastoma, and brain tumors--and exposure to pesticides. These studies have focused on a wide range of potential scenarios including prenatal exposures, postnatal exposures in the home, and parental occupations such as agriculture and pesticide application. Because these studies are typically constrained by limited sample sizes and exposure data, the link to pesticides is still considered by most cancer researchers to be hypothetical. Nonetheless, Zahm comments in the September 1995 issue of Environmental Health Perspectives Supplements , "It is striking that many of the reported increased risks are of greater magnitude than those observed in studies of pesticide exposed adults. These results suggest that children may be a particularly sensitive subpopulation with respect to possible carcinogenic effects of pesticides."
In a study published in the November 1997 issue of EHP , Janice M. Pogoda, a statistician with Statology, a consulting firm based in Truckee, California, and colleagues report a statistically significant association between elevated rates of brain tumors (particularly in children under the age of five) and home use of flea and tick foggers by their mothers while pregnant. A search of pesticides used in flea and tick products by the authors turned up a number of compounds that are common to most formulations: pyrethrins and pyrethroid insecticides (the most common), organophosphates, and carbaryl, a carbamate that is classified as noncarcinogenic by the EPA. Carbaryl is of particular interest because it reacts with nitrite at pH 1 (a level that can be reached in the stomach) to form nitrosocarbaryl, which is a known skin and forestomach carcinogen in mice. Nitrites are commonly found in cured meats such as hot dogs and sausages.
"The fetal animal in particular is exquisitely sensitive to N -nitroso compounds, particularly nitrosoamides and nitrosoureas," says Susan Preston-Martin, a professor of preventive medicine at the University of Southern California in Los Angeles. "[These compounds] can cause CNS tumors in a wide variety of species, including primates, and a much smaller dose is required if the exposure is transplacental. Even exposures to precursors like nitrite and sodium nitrite in food and water will cause tumors in offspring." Basing her hypothesis upon the overwhelming evidence for the association in animals, Preston-Martin initiated the largest study conducted to date of maternal consumption of cured meats and incidence of pediatric brain tumors, and found a statistically significant dose-response relationship. Her findings were published in the August 1996 issue of Cancer Epidemiology . Preston-Martin also found that women who consumed cured meats during pregnancy reduced the risk of pediatric brain tumors in their children if they took vitamins C, A, and E, which bind with nitrates and remove them from circulation.
Nitrosamines are among the many suspected human carcinogens found in tobacco smoke. The role of maternal tobacco use in the etiology of childhood cancer remains controversial, and the findings of many studies conflict. Most of these studies are plagued by a lack of quantitative information and the inability to control for exposure to secondary smoke during pregnancy. In a study published in the 3 January 1996 issue of the Journal of the National Cancer Institute, Xiao-Ou Shu and colleagues at the CCG report that children of women who smoked were actually at reduced risk of childhood leukemia after adjusting for confounding variables such as socioeconomic status and low birth weight, which is related to heavy maternal smoking. In the same report, the authors cite an increased risk of AML among children whose mothers consumed alcohol during pregnancy. According to the authors, "The risk of AML appeared to increase with the frequency of maternal drinking, was pronounced for the children whose mothers drank during the second or third trimester of pregnancy, and was associated with all types of alcohol." They also note that their findings are consistent with the results of two other studies--one completed by the CCG in 1993, and another conducted by the Dutch Childhood Leukemia Group in 1994--that identified a link between childhood cancer and maternal alcohol use.
Improved Diagnosis Raises Questions
While continued research on each unique cause helps to shed light on how individual cancers may occur in the first place, it still tells little about why cancer incidence rates are rising overall. Improved diagnostics and better recording of cases by state and federal cancer registries are both assumed to play a role, but even taken together they cannot explain the magnitude of the increases that have been observed over the last several decades. Zahm asserts that part of the observed increase in ALL may be attributed to more accurate histological classification of the disease. Before specific treatments for ALL were developed, most leukemias were treated the same way, and so leukemias were often reported to state and federal cancer registries as "Leukemia-Not Otherwise Specified," a generalized category applied to all leukemias. However, once treatment regimes were developed that were specific to ALL, the physicians would record the disease as such. However, she cautions that it would be misleading to write off the increase simply to changes in classification, because the incidence rate for the category of "All Leukemias Combined" (including ALL) has also been rising slightly. "If increased reporting was all that happened, you would expect that the incidence for 'All Leukemias Combined' would remain level," Zahm says. "However, these numbers have also been increasing as well. This indicates that something else is going on that we are not currently aware of."
Gurney, an epidemiologist at the St. Louis University School of Public Health, says that some researchers attribute the apparent increase in CNS tumors in children to improved diagnosis of the disease, particularly with the advent of computerized axial tomography scans in the 1970s, and magnetic resonance imaging in the 1980s. However, he says that rather than explain the increases in children, it is more likely that the use of this technology explains increases in the elderly, who may in the past have been frequently misdiagnosed with degenerative diseases such as Alzheimer's disease, rather than correctly diagnosed with brain tumors. Says Gurney, "It's true that these kinds of diagnostic workups are now done much more often [on children], but even so you'd expect to see a gradual flattening in the yearly childhood incidence rates, and we're not seeing that." Gurney also notes that if improved diagnosis was a factor in increased reporting, one would expect to see an increase in other types of tumors that are also identified using the same types of imaging equipment. However, this is not always the case. For example, the incidence of primitive neuroectodermal tumors has not risen during the same time period.
Is the increase in cancer incidence therefore related to some as-yet unidentified environmental factors? Many researchers believe this to be the case. An important distinction between childhood and adult cancers is the short latency period that characterizes cancers in children. According to Gurney, this would seem to indicate that environmental factors likely interact with certain predisposed genetic traits at an early stage in a child's life.
Robison notes that in the future research on the causes of children's cancer may do well to focus on the role of parental occupation in increased cancer risk, looking at the types of work held by the parents both prior to the child's birth as well as after. "The literature is filled with observations of increased or decreased estimates of risk depending upon the occupation of the parents," he says. "However, it's difficult to focus on the exposures. One should look at biomarkers of susceptibility and exposure. It is also possible to identify subpopulations that are especially susceptible." Robison is currently conducting research on these areas through the CCG's epidemiology program. Steven Galson, scientific director of the OCHP, agrees that continued research on biomarkers is important. His office is encouraging research in this area, as well as enhanced surveillance of childhood cancers, particularly through the use of geographic information systems and the development of toxicological screening methods that focus on neonatal and juvenile animal models.
Fortunately, even though the incidence rates are increasing, the prognosis for children with cancer has never been better. Medical research has made great advances in the management and treatment of cancers over the last several decades, and afflicted families can take heart that a diagnosis of cancer in their child may no longer present the same bleak prospect that it did in the past. Thanks to new treatments such as growth factors that stimulate recovery of healthy bone-marrow cells during chemotherapy and improved techniques in bone-marrow transplantation, long-term survival rates (defined as being disease-free for five years or more) for ALL now range from 50% to 90%. The prognosis depends on a number of variables, most importantly whether the leukemic cells originate as T-cells, which have a worse prognosis, or B-cells. According to John Lazlo, national vice president of the American Cancer Society and author of the recent book The Cure of Childhood Cancer--Into the Age of Miracles , the best prognosis is for children under the age of 10 with no nervous system involvement, a white blood cell count of under 50,000 cells at the time of diagnosis, and elevated DNA content of the leukemic cells.
The long-term survival rate for children diagnosed with pediatric brain tumors has also improved, from approximately 54% in 1973 to a current range of 73-85%. Much of the improved diagnosis derives from improved delivery systems for radiation treatment and the use of antiangiogenic drugs that block the blood vessels that nourish brain tumors and allow them to grow.
Practically every child diagnosed in the United States is treated by members of either the CCG or the Pediatric Oncology Group, both of which are large, multidisciplinary organizations that provide care tailored specifically to children. This fact is critical, according to Denmond Hammond, president of the National Childhood Cancer Foundation and former head of the CCG, because the biology of cancer in children differs considerably from that of adults, and their treatment is best conducted by specialists trained in the management of childhood malignancies. However, the increase in incidence trends leaves many unanswered questions. "The truth is, we don't yet know what's behind the increases [in childhood cancer]," says Landrigan. "We need to agree on the facts and lay out a coordinated agenda for research." An EPA-sponsored conference on childhood cancer that was held in September 1997 in Washington, DC, drew close to 300 physicians, academic and government researchers, and public interest representatives, all assembled for the purpose of designing a multimillion-dollar research strategy that will begin early next year and hopefully start to reverse this devastating trend of illness in the nation's children.
Charles W. Schmidt
Children's Health Source List American Cancer Society , Internet: http://www.cancer.org
1599 Clifton Road NE, Atlanta GA, 30329, 1-800-227-2345 Case Western Reserve University , Internet: http://gcrc.meds.cwru.edu/stachy.htm
11100 Euclid Avenue, Cleveland, OH 44106, fax: (216) 844-5916, e-mail: stachy@po.cwru.edu , Center for Nutrition Policy and Promotion , Internet: http://www.usda.gov/fcs/cnpp.htm
U.S. Department of Agriculture, 1120 20th Street NW, Suite 200, North Lobby, Washington, DC 20036, (202) 418-2312, CureSearch , Internet: http://www.curesearch.org/
440 E. Huntington Drive, Suite 300, PO Box 60012, Arcadia, CA 91066-6012, 1-800-458-6223,
fax: 1-800-723-2822. Children's Environmental Health Network , Internet: http://www.cehn.org/
5900 Hollis Street, Suite E, Emeryville, CA 94608, (510) 450-3818, fax: (510) 450-3773, e-mail: cehn@aimnet.com Children's Health Environmental Coalition , Internet: http://checnet.org/
PO Box 846, Malibu, CA 90265, (310) 573-9608, fax: (310) 573-9688, e-mail: chec@checnet.org Children's Health Initiative, Agency for Toxic Substances and Disease Registry , Internet: http://atsdr1.atsdr.cdc.gov:8080/child/
1600 Clifton Road (E28), Atlanta, GA 30333, (404) 639-0700, fax: (404) 639-0744, e-mail: rwa1@cdc.gov National Center for Environmental Health, Centers for Disease Control and Prevention ,
Internet: http://www.cdc.gov/nceh/ncehhome.htm
Mail Stop F-29, 4770 Buford Highway NE, Atlanta, GA 30341-3724, (770) 488-7030, e-mail: ncehinfo@cdc.gov , National Childhood Cancer Foundation , Internet: http://www.nccf.org/
440 E. Huntington Drive, Suite 300, PO Box 60012, Arcadia, CA 91066-6012, 1-800-458-6223, fax: 1-800-723-2822 National Environmental Education and Training Foundation , 734 15th Street NW, Suite 420, Washington DC 20005, (202) 628-8200,
fax: (202) 628-8204 National Institute of Child Health and Human Development , Internet: http://www.nih.gov/nichd/
9000 Rockville Pike, Bethesda, MD 20892, (301) 496-4000 NIEHS Office of Communications , Internet: http://www.niehs.nih.gov/kids/kidsatoz.htm
MD EC-12, PO Box 12233, Research Triangle Park, NC 27709, Attention: John Peterson, (919) 541-7860, fax: (919) 541-2242,
e-mail: booklet@niehs.nih.gov Office of Children's Health Protection, U.S. Environmental Protection Agency , 401 M Street SW, Washington, DC, 20460, (202) 260-7778 Pediatric Oncology Group , Internet: http://www.pog.ufl.edu/
645 N. Michigan Avenue, Suite 910, Chicago, IL 60611, (312) 482-9944, fax: (312) 482-9460 |
Last Update: 2006 February 28





