|
The Effect of Outdoor Fungal Spore Concentrations on Daily Asthma Severity
Ralph J. Delfino,1,2 Robert S. Zeiger,3,4 James M. Seltzer,3,5 Donald H. Street,6 Reneé M Matteucci,1 Patrick R. Anderson,1 Petros Koutrakis7 1Graduate School of Public Health, San Diego State University, San Diego, CA 92120 USA; 2Epidemiology Division, Department of Medicine, University of California, Irvine, CA 92717 USA; 3Department of Pediatrics, University of California, San Diego, CA 92103 USA; 4Department of Allergy, Southern California Permanente Medical Group, San Diego, CA 92111 USA; 5Clinical Research Institute, San Diego, CA 92131 USA; 6Bayer Corp., Allergy Products, Independence, OR 97351 USA; 7Environmental Chemistry Laboratory, Department of Environmental Health, Harvard University School of Public Health, Boston, MA 02115 USA Abstract
The relationship between day-to-day changes in asthma severity and combined exposures to community air pollutants and aeroallergens remains to be clearly defined. We examined the effects of outdoor air pollutants, fungi, and pollen on asthma. Twenty-two asthmatics ages 9-46 years were followed for 8 weeks (9 May-3 July 1994) in a semirural Southern California community around the air inversion base elevation (1,200 ft) . Daily diary responses included asthma symptom severity (6 levels) , morning and evening peak expiratory flow rates (PEFR) , and as-needed ß-agonist inhaler use. Exposures included 24-hr outdoor concentrations of fungi, pollen, and particulate matter with a diameter <10 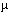 m (PM10 ; maximum = 51 m (PM10 ; maximum = 51 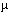 g/m3) and 12-hour daytime personal ozone (O3) measurements (90th percentile = 38 ppb) . Random effects longitudinal regression models controlled for autocorrelation and weather. Higher temperatures were strongly protective, probably due to air conditioning use and diminished indoor allergens during hot, dry periods. Controlling for weather, total fungal spore concentrations were associated with all outcomes: per minimum to 90th percentile increase of nearly 4,000 spores/m3, asthma symptom scores increased 0.36 (95% CI, 0.16-0.56) , inhaler use increased 0.33 puffs (95% CI, g/m3) and 12-hour daytime personal ozone (O3) measurements (90th percentile = 38 ppb) . Random effects longitudinal regression models controlled for autocorrelation and weather. Higher temperatures were strongly protective, probably due to air conditioning use and diminished indoor allergens during hot, dry periods. Controlling for weather, total fungal spore concentrations were associated with all outcomes: per minimum to 90th percentile increase of nearly 4,000 spores/m3, asthma symptom scores increased 0.36 (95% CI, 0.16-0.56) , inhaler use increased 0.33 puffs (95% CI,
-0.02-0.69) , and evening PEFR decreased 12.1 l/min (95% CI, -1.8-22.3) . These associations were greatly enhanced by examining certain fungal types (e.g., Alternaria, basidiospores, and hyphal fragments) and stratifying on 16 asthmatics allergic to tested deuteromycete fungi. There were no significant associations to low levels of pollen or O3, but inhaler use was associated with PM10 (0.15 inhaler puffs/10 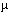 g/m3 ; p<0.02) . These findings suggest that exposure to fungal spores can adversely effect the daily respiratory status of some asthmatics. Key words: Alternaria, asthma, basidiomycete, epicutaneous allergen skin tests, epidemiology, longitudinal data analysis, ozone, panel study, particulate air pollution. Environ Health Perspect 105:622-635 (1997) g/m3 ; p<0.02) . These findings suggest that exposure to fungal spores can adversely effect the daily respiratory status of some asthmatics. Key words: Alternaria, asthma, basidiomycete, epicutaneous allergen skin tests, epidemiology, longitudinal data analysis, ozone, panel study, particulate air pollution. Environ Health Perspect 105:622-635 (1997) Address correspondence to R. J. Delfino, Epidemiology Division, Department of Medicine, College of Medicine, University of California, Irvine, CA 92697-7550 USA. The authors wish to thank M. Wolfson, P. Roberts, and C. Donoghue for the preparation and chemical analysis of ozone passive samplers and M. Hossain, D. White, and their staff for providing the stationary site O3 and weather data and for their assistance in siting the remaining stationary site monitors. We also thank F. Lurmann, P. Roberts, H. Margolis, and E. Avol for helping us obtain the PM10 data. We also appreciate the skilled efforts of our clinic coordinators K. Mostafa and L. Skific. Most of all we wish to thank our study participants for their diligent efforts. This project was supported by grant number ES06214 from the NIEHS. The contents of this paper are solely the responsibility of the authors and do not necessarily represent the official views of the NIEHS or the National Institutes of Health. Received 1 July 1996 ; accepted 19 February 1997.
The full version of this article is available for free in HTML format. |

