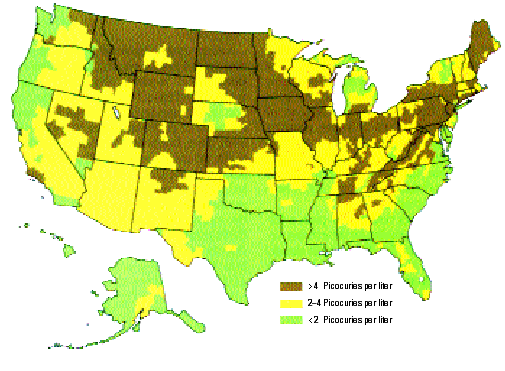
Regional radon. EPA has mapped out average U.S. indoor radon levels by county to determine which areas are most in need of remediation.
Who would expect an odorless, invisible gas that occurs nearly everywhere on earth to cause such trouble? Yet radon, the gas emitted by decay of uranium in the earth's crust, is one of America's most significant environmental risks, according to the EPA, which estimates that residential radon levels lead to approximately 13,600 lung cancer deaths each year. A new National Cancer Institute analysis of multiple studies of miners confirms early estimates, putting the number at 15,000. No other risk comes close, not even environmental tobacco smoke, which is estimated to cause some 3,000 deaths each year.
Hot debate surrounds the assessment of risk from radon exposure to Americans via indoor air and water supplies. The primary culprit is not radon gas itself, but its decay products, including polonium-214 and polonium-218, which have long half-lives and emit alpha particles--positively charged particles--and lung cancer when inhaled. Radon seeps into homes from the ground or is present in water supplies. Waterborne radon may be inhaled as radon or its progeny during household use--cooking or showering--or it may be ingested. But the EPA estimates that water sources contribute only about 5% of total airborne radon exposure, leaving indoor air as the worst offender. While the EPA estimates that approximately 200 cancer cases per year result from exposure to radon from public groundwater systems, estimates of annual lung cancer deaths from indoor air radon range from 7,000 to 30,000.
Radon Risk
The radon dilemma demonstrates the problems inherent in risk assessment and the science that forms its basis. Neither epidemiological nor biological studies to date have produced a definitive answer on radon risk, but ongoing studies and pooled analyses have begun to hone in.
Risk assessments are needed to establish exposure guidelines. There are currently no federal regulations on radon in indoor air. The Indoor Radon Abatement Act of 1988 does not direct the EPA to issue regulations on radon in indoor air. It does, however, establish as a national goal that indoor radon levels equal outdoor radon levels. Although this goal is not currently feasible, the EPA has established a 4 picocuries per liter (pCi/l) action guideline based on the capabilities of measurement and mitigation technologies. (A picocurie is a trillionth of a curie; 1 gram of uranium emits 1 curie of radiation.) In contrast, the Federal Safe Drinking Water Act requires the EPA to regulate the amount of radon in public drinking water supplies. Moreover, there is no known human threshold for this kind of radiation exposure. And smoking, the greatest single cause of lung cancer, must somehow be separated from radon exposure to arrive at excess risk. How radon and smoking act together to increase lung cancer risk is another enigma.
This spring, the National Cancer Institute released an analysis of 11 studies of male miners which evaluated the risk of exposure to radon in far greater detail than was previously possible. The studies included more than 2,700 lung cancer deaths among 68,000 miners in the United States, Canada, Europe, Scandinavia, Australia and China. The NCI found that 73% of the lung cancer in miners who never smoked and 39% of the lung cancer in miners who smoke may be due to radon progeny exposure. The analysis estimated that about 10% of all lung cancers in the United States may be attributable to indoor radon exposures--amounting to 10,000 U.S. lung cancer deaths a year among smokers and 5,000 among those who never smoked. Based on a 95% confidence interval, the analysis drove the range of attributable annual U.S. lung cancer deaths from 6,000 to 36,000.
Because of its size and precision, NCI's analysis is recognized as a key advance in radon research. But there is still widespread concern about using mine studies to estimate residential risk. "Studies of lung cancer risks from indoor radon exposures are inconclusive," the NCI said in announcing the new analysis. "Thus it is only possible to estimate residential risks from miner studies."
The EPA, under fire about radon, responds that miner studies offer the best data available. "Next to actual residential radon data, the best data you can have is occupational human data," says Stephen Page, director of the EPA's radon division. "Most of your environmental issues actually extrapolate from animal studies, or human studies if you're lucky. We have human data from mines, and the National Academy of Sciences has also looked at the proper adjustments [to the data] that should be made." The academy has recommended reducing the measure of the effect of radon in mine exposures by 30% for estimates of the effect of radon in homes.
The NCI analysis also addresses what Page calls "a huge confounder": the criticism that most of the miners in the old study were smokers. "The point is," said Page, "you have human data that nonsmoking miners are at increased risk comparable to what the EPA and the National Academy has predicted for the general population of nonsmokers. That's significant."
The analysis also found that prolonged exposure at low doses is associated with more risk than shorter exposure at higher doses, although this relationship probably does not hold for the low radon levels found in homes.
 |
| Jonathan Samet--Radon risk assessment is controversial because the number of lung cancer deaths is so big. |
NCI's analysis serves as a new focus for the decade-old controversy over radon risk assessment and the problems of studying human exposures. "What are the problems we get into?" asks epidemiologist Jonathan Samet, chair of the epidemiology department at Johns Hopkins University School of Hygiene and Public Health and chair of the National Research Council's Committee on Health Risks of Exposure to Radon. "First, you have to extrapolate from miners, and they've been exposed only at one point of their lives. They work in dusty environments, and there may be other factors. Probably most important is that you have to extrapolate from exposure levels and rates higher than those typically experienced."
In mines, radon is measured according to the alpha energy emitted by radon progeny in a liter of air, called a working level (WL). A working level month (WLM) consists of 170 hours at an exposure rate of 1 WL. "The typical lifetime estimated average exposure from radon from indoor exposures is in the range of 14 to 20 working level months," explains Samet. "The miners have typically been exposed at levels in the 50 to 100 [WLM] range and far higher. So there's the exposure difference and an exposure rate difference, because most of the miners received the exposure over an interval of three or four years. And again, because of a possible repair process, for example, perhaps exposures received at a very low rate might have different biological effects. This is where some of these uncertainties begin to come in."
Why is radon risk assessment so controversial? "Because the number comes out so big," Samet says. "Those kinds of numbers [of lung cancer deaths] are disturbing." The complexities of extrapolating from miner studies and the connection between smoking and radon exposure make it difficult to identify actual risk. The number of lung cancer deaths attributable to radon is greater in smokers than nonsmokers, "indicating that the two carcinogenic exposures interact in a fashion that produces more lung cancers than would be expected by simply adding together their individual risks," said Samet.
One problem is that it is difficult to measure indoor air exposures that are relatively low. The EPA estimates that the average U.S. indoor radon level is around 1.3 pCi/l. The EPA recommends restructuring a home when levels are above 4 pCi/l, a number set in 1986 because it could be achieved with affordable technology. From its 1991 National Residential Radon Survey of 6,000 homes, the EPA estimated that 6% of U.S. homes have average exposures above the 4 pCi/l action level. The EPA then created a national map that identified about a third of all counties in the United States as high-radon hot spots. Critics continue to discount the EPA figures as exaggerations, particularly questioning earlier radon measurements of air in unventilated basements, where levels typically would be higher than in living areas. Another complication for epidemiologists is estimating radon exposure over time, since people change houses during their lifetime, and radon levels in homes may be altered by new heating systems and room additions, for example.
The EPA's radon program, which recommends that all 100 million American homes be tested, estimating that 6 million homes will have high radon levels that should be corrected, has been surrounded by controversy. "People who don't like the risk management approach have said we don't know enough to move into risk management," Samet observes. "I think the risk management approach makes the science, in a sense, a target." Samet notes that if radon were a man-made carcinogen with risk estimates this high, the regulatory paths would be more clearly defined.
Comparing the Air
A number of new studies seek to address the gaps in knowledge about radon exposures and cancer risks. A collaborative case-control study by the NIEHS is the largest study of its kind in the United States, involving some 1,494 lung cancer cases and 1,839 controls in Connecticut, Utah, and Idaho, including smokers and nonsmokers and women as well as men. The study measures radon in all homes where a person lived from age 25 to diagnosis of lung cancer. The study will cover the lifetime exposure of 70% of the people involved, according to study director Dale Sandler, chief of the Environmental and Molecular Epidemiology Section of the NIEHS. The study, which began in 1989, is expected to be completed in 1995.
Jan A.J. Stolwijk, professor of epidemiology and public health at Yale University, is conducting a portion of the study in Connecticut with 960 cases and an equal number of controls, using radon detectors placed in the living areas of homes. Researchers are calculating each subject's total radon exposure based on the data collected. The home registering the highest amount of radon had 30 pCi/l, while the home registering the least amount of radon had 0.1 pCi/l, according to Stolwijk. "We have put these [detectors] where people actually are, and we are now calculating their total exposure based on what actually happens. . . . they're exposed to a median level of 0.4 picocuries per liter, instead of the median level of about 1.5--about one-third to one-fourth what the EPA normally suggests," he says.
Analysis of the data is scheduled to begin in the fall of 1994, with results anticipated in late 1995. Study investigators are now focusing on reconstructing lifetime exposure histories and dealing with the inevitable problems of missing data on radon levels. A strength of this study, according to Sandler, is the emphasis on identifying the joint effects of smoking and radon. Says Stolwijk, "We are now constructing for each individual a record of how many cigarettes per day that individual smoked over a whole lifetime, based on detailed reports of smoking habits at different ages. We are going to have situations where you have people who did not have any radon in their younger years, but smoked. And who then later on lived in a house with radon in it, but didn't smoke. The effect of that can be compared with another small group of people having radon exposures but not smoking early on, who then switched over into no radon but smoking. We don't know how these combinations are going to work out."
The difficulty in running such a study is that not many houses have very high levels of radon. Stolwijk hopes to work with Connecticut's Department of Natural Resources, matching the homes his study has measured with geologic and soil characteristics, to identify areas where houses may have more radon.
Another NIEHS-supported study involves a five-year, case-control investigation of residential radon exposure in New Jersey's six northernmost counties, mountainous areas known to be high in radon. That study, which includes 780 lung cancer cases and about 850 controls, is a collaborative effort by researchers at Mount Sinai Medical Center in New York and the New Jersey Department of Health. The study found, according to Philip Landrigan, director of Mount Sinai's Environmental Health Sciences Center, that "the risk is present and visible at levels of exposure which are below the current federal guideline for radon in homes. . . . We can see it down as low as 2 picocuries per liter."
 |
| Michael Alavanja--Exposure to high levels of radon may present excess risk of adenocarcinoma to women. |
Two NCI studies of Missouri women also seek to pin down the smoking and radon link. The first study includes 2,000 nonsmoking women--600 lung cancer cases and 1,400 population-based controls. Of the 600 cases, 70% have never smoked, and 30% stopped smoking an average of 26 years ago. The subjects were queried about their diet, occupation, family history and personal health history, as well as residence, and year-long, radon measurements were made in the bedrooms and kitchens of every home the women occupied for the past 30 years. "It turns out Missouri is almost identical to the average radon concentration in the country," says Michael Alavanja, a senior scientist at the NCI who is conducting the study. "Seven percent of our population had over four picocuries per liter, which is the national average."
According to Alavanja, overall results show that among these women, there was no statistically significant excess risk from indoor exposure to radon. But there are intriguing findings among several subgroups, Alavanja says. To look at the distribution of radon exposure, the study assigned women to five subgroups according to levels of exposure. In the subgroup of women who experienced the highest exposure levels--a median of 4 pCi/l--the study found an excess risk of lung cancer of 20%, though that risk is not statistically significant. Other results showed, however, a significant excess risk among these women for adenocarcinoma, the most frequently occurring cancer cell type among nonsmoking women. Alavanja notes that in the study, only 40% of the subjects were living when interviews were conducted, so many interviews were done with the next-of-kin. In the subgroup of women who were interviewed in person, he reports, there was a statistically significant increase in excess risk. Detailed results of the study are to be published by the NCI.
Alavanja observed that the 20% excess risk found in the highest exposed group in Missouri corresponds to a Swedish study's next-to-highest group. That study, by researchers at the Karolinska Institute in Stockholm, reported in the New England Journal of Medicine in January 1994, was the largest epidemiological study completed to date, involving 1,360 men and women with lung cancer and 2,847 healthy people. It found that people exposed to radon levels of 3.8-10.8 pCi/l had a lung cancer risk 30% higher than people whose exposure averaged below 1.4. For those radon levels above 10.8 pCi/l, the lung cancer risk was 80% higher. "It may be that we're first seeing in our highest group [in Missouri] in effect what the Swedes are also seeing," Alavanja observes.
Alavanja is curious to see if the second Missouri case-control study of women smokers and nonsmokers mirrors the Swedish study, which saw the greatest effect among smokers. Results are expected in early 1995.
Studies Under Glass
A continuing problem with lifetime residential studies is accounting for exposures that occurred years ago. Some homes no longer exist, and there is also concern that contemporary measurements may not reflect past radon levels. The second Missouri study employs a new technique that measures lead-210 molecules and polonium-210 left on glass when radon emits alpha particles. "We locate glass objects in the home that were around at least 30 years ago," Alavanja explains. Among them: mirrors that came with a bedroom suite or the glass on a framed picture that always hung in the person's bedroom.
An EPA pilot study being conducted by the NIEHS will evaluate the use of this technology. Because there appears to be some error introduced by the presence of cigarette smoke, the study will compare measurements under different smoking conditions.
A new residential study in China will measure homes built largely underground in an area where radon levels are relatively high. Jay Lubin, a biostatistician in NCI's Division of Cancer Etiology, is principal investigator. Lubin, who led the analysis of the 11 miner studies, said, "We anticipate looking at 800 to 900 lung cancer cases and an equal number of controls. We're hoping that the study population will bridge the exposure range between lower-exposure residential studies and the higher-exposure miner studies. We're hoping to have a better opportunity to detect excess risk due to radon."
Will epidemiological studies eventually release radon's secrets? "You may never be able to design a study that definitively does it," says Page of the EPA, speculating that such a study might cost several hundred million dollars. "All the mainstream scientific organizations say that you need to look at your residential epidemiological studies in combination with all the other information that's out there: the miner studies, the animal studies and now, most recently, molecular research. What everybody agrees on is that not any one of those studies by themselves is going to tell you with any kind of precision such things as a threshold."
Samet says that expectations for case- control studies may be too high. He is especially concerned about sample sizes, which must be large. "We would anticipate, if a lot of studies are done that are not quite big enough, that some would be construed as showing carcinogenicity and others would not, although the findings may be quite mutually compatible."
 |
| Naomi Harley--Long-term tests should be required before remediation. |
Beyond epidemiological studies, new biological research into how radiation causes lung cancer holds promise. Among advocates of a biological model is Naomi Harley, a radiation physicist in the Department of Environmental Medicine at New York University's School of Medicine. Harley, whose work is funded by the Department of Energy, began studying radon as a health issue in the 1950s for the Atomic Energy Commission. In the 1970s she began work on radon decay dosimetry in the lung.
The dose-response relationship is the key to understanding risks. Harley notes that radon itself, with a half-life of 3.8 days, does not give a person much of a dose. The dose comes from the radon decay products which attach to aerosols, are inhaled, and then are deposited on airway surfaces. Some of these decay products have short half-lives with long clearance times. The alpha particles they emit irradiate adjacent tissue, causing mutations or sterilizing or killing cells.
Exposure to decay products is lower in homes than in mines, Harley explained, but dosimetrically, for each unit of exposure, a person receives the same kind of alpha particle energy whether at home or in a mine. Researchers are continuing to investigate these mechanisms, Harley said, including the sizes of particles in mines and homes, and how an inhaled aerosol is deposited in the lung.
Harley says that the NCI analysis does not offer a good biological model, especially concerning the smoking-radon link, which is neither additive nor multiplicative, she says. "I'm trying to work up a more biological model with a colleague. What is the cell turnover rate? Why does the risk reduce when you get away from exposure? Even for smokers, why is the risk reduced when you stop smoking? The biological model remains to be done."
Radon Repairs
One distinction that typically isn't made, Lubin observes, is the difference between lung-cancer deaths attributable to radon and the number of lives that may be influenced if every home over 4 pCi/l were remediated. ". . . About 2,000 to 4,000 lung cancer deaths [would be avoided]," he says. "It has to be clear that one cannot eliminate radon from the environment of homes. You can only reduce it."

The EPA estimates the cost per life saved would be around $700,000. That figure includes the cost of testing 100 million homes at about $25 each and mitigating all 6 million high-radon homes at $500 to $2,000 each. Such costs inflame yet another debate over measuring radon levels. The EPA has long been criticized for what appear to be exaggerations, although Page insists the early numbers were never intended to be used for health risk assessment.
Today the EPA continues to support short-term measurements made over a few days to identify radon problems. This is not long enough, says Harley, especially when measurements are very near the 4 pCi/l guideline. "The guideline should be that you need a long-term test before you remediate," she says. EPA's Citizen's Guide to Radon does advise that long-term measurements are best.
Harley also is concerned about inaccurate analysis by radon test vendors. This can be particularly problematic when the reading is just above or just below the federal guideline. Other factors may affect these measurements. Said Harley, "We've observed that about 20% of the radon in a house on average each year comes from little peaks due to barometric pressure drops. Temperature and barometric pressure are the two major variables that control radon in the house."
One hour-by-hour study by Harley of existing homes included a new and tightly sealed energy-efficient home and a leaky frame house built 80 years ago. The new home had radon levels of 20-30 pCi/l when the heat exchanger was off, but averaged about 3-4 pCi/l with the heat exchanger on. Barometric peaks were still observable. A sub-slab fan that sucks air from beneath the house--the standard mitigation recommended by the EPA--reduced the radon level to about 1.0 pCi/l. The older home, which was located 50 miles away and had the same weather, had a consistently lower radon level. Says Harley, "You never see a 20 [pCi/l] in this house. Old homes are just leaky."
Harley's research has shown that blowing air beneath a house, rather than sucking it out from underneath, reduces the barometric pressure peaks. "You still see them, but they're not nearly as high." Another year of study, she says, will confirm these results.
High Water Marks
Although radon in water poses only an estimated 5% of the nation's radon risk, the federal Drinking Water Act requires the EPA to regulate the amount of radon in public drinking water supplies. The EPA has proposed a maximum contaminant level of 300 pCi/l equivalent to 0.03 pCi/l in air.
At least 27,000 water systems would be affected by the proposed standard, according to geologist Tim Gill of the EPA's Drinking Water Standards Division. The annual cost to fix the problem including installing, maintaining, and operating packed-tower aeration systems would total $283 million, according to the EPA. "It breaks down to $9,000 to $11,000 per system," says Gill. Others say the cost will be many times higher. Still others argue that putting this cost into perspective by comparing it to the cost of a single case of cancer makes the cost per public water system very small.
The cost would be borne mostly by small systems. Of the 27,000 systems affected, 24,000 are "small to very small systems that are serving no more than 1,000 people each," Gill said. The reason so many small systems would be affected by the proposed rule, Gill explains, is because most small systems use groundwater, whereas large municipal systems tap surface waters such as rivers and lakes.
Risks from waterborne radon exposure are considered minimal. "The rule of thumb is 10,000 picocuries per liter of radon in water contributes about 1 picocurie in air," says Lubin. Harley's 1994 DOE study comparing the concentration of radon in water to radon in air found this factor to be 40,000 to 1 rather than 10,000 to 1.
 |
| Irina Cech--There are no two houses alike. |
Irina Cech, professor of environmental health sciences and hydrology at the University of Texas, argues about the usefulness of such a conversion factor. Said Cech, "I'm more interested in the air being inhaled when you take a shower. This diffusion rate is irrelevant when radon is inhaled from water in an enclosed environment of a shower stall. We know very little about the impact of the inhalation of hot aerosol bearing radon on the body." In addition, she says, "There are no two houses alike. We don't inhale air on the average."
The bottom line on radon, say researchers, is wait and see. Samet and Lubin agree that until current case-control studies are complete, there is little need for new ones. "We already have a wealth of information from studies of miners and other lines of research on which to base our policy development," Samet said. "On the other hand, for an issue so sweeping as to touch every home, we would like to be very certain about our understanding of the risk. Right now, with radon, the more data we have, the more sophisticated questions we want to ask of it. In a sense, the answers may then become a little more uncertain."
Page believes that epidemiological studies must be looked at in combination with animal studies and molecular research. "There's still going to be such uncertainty that the best we're going to be able to do is try to quantify that uncertainty," he said. "It's important to remember that the information we now have is as strong as there is for most any environmental pollutant. . . . Meanwhile the challenge for EPA is to act on the currently available database and develop a policy that's responsible, based on what we know and what we don't know."
Laura Alderson
Laura Alderson is a freelance writer in Raleigh, North Carolina.
Last Update: June 20, 1998





