Mouse Model Points to Possible New Strategy
For Treating Rare Muscle Disease, Kidney Disorders
Researchers Surprised by Clues Uncovered in
Transgenic Mice
Based on clues provided by a study with transgenic mice, a research
group at the National Human Genome Research Institute (NHGRI),
part of the National Institutes of Health (NIH), has developed
a strategy that will be tested as the first treatment for people
with hereditary inclusion body myopathy (HIBM), a rare, degenerative
muscle disease. In an unexpected finding, the research indicates
that the approach also might benefit patients with certain kidney
disorders.
The scientists, led by Marjan Huizing, Ph.D., an associate investigator
in NHGRI’s Medical Genetics Branch, report their findings in the
June issue of the Journal of Clinical Investigation. The
study was supported by the NHGRI Division of Intramural Research
and was conducted in collaboration with researchers supported by
the Howard Hughes Medical Institute (HHMI), Bethesda, Md., and
the HIBM Research Group, Encino, Calif.
“It is gratifying to see how the tools and technologies generated
by the sequencing of the human genome are being used to uncover
new strategies for treating genetic human disease,” said NHGRI
Director Francis S. Collins, M.D., Ph.D. “This work also underscores
the value of animal models in learning more about the pathways
involved in human disease and how to target therapies that affect
those pathways.”
NHGRI Scientific Director Eric D. Green, M.D., Ph.D. said, “We
are excited by the possibility that this study may lead to new
treatments for those who suffer from either HIBM or kidney dysfunction.
This work is a solid example of translational research, where discoveries
in the laboratory provide a way forward to aid patients dealing
with a frustrating and debilitating inherited disorder.”
HIBM is a genetic disease with non life-threatening symptoms that
emerge in adulthood and lead to slowly progressive muscle weakness.
Most patients develop symptoms while in their early 20s and become
wheelchair-bound by the time they reach 40, as their arm, hand,
leg and core muscles progressively weaken. It is caused by a mutation
in the GNE gene, which codes for two enzymes that produce
sialic acid, a sugar important to muscle development and kidney
function.
The new research focused on a form of HIBM in Iranian-Jewish families,
which is caused by a specific mutation in the GNE gene
known as M712T. Numerous other GNE mutations can cause
HIBM and occur in populations worldwide. At this time, there is
no treatment available for any type of HIBM.
In their search for potential HIBM treatments, the researchers
drew upon previous evidence that impairment of the enzymes that
promote sialic acid production causes low sialic acid levels in
muscle proteins. They hypothesized that a compound called N-acetylmannosamine,
or ManNAc, a sugar that is naturally converted to sialic acid,
might have an impact on the muscle weakness caused by HIBM.
To help test that hypothesis, Dr. Huizing and her colleagues created
a transgenic mouse model in which M712T GNE gene mutation
was introduced into a strain of mice. However, the researchers
were surprised to find that, instead of developing adult-onset
muscle disease as expected, the transgenic mice developed a kidney
condition that caused them to die just a few days after birth.
When the researchers supplemented the diets of pregnant transgenic
mice with ManNAc, sialic acid production improved in the fetuses,
and they were born with markedly improved kidneys.
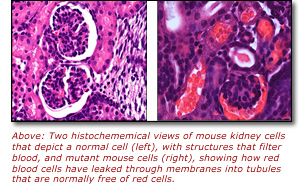 |
“We were surprised that the HIBM mutation had such a detrimental
impact on kidney function in the transgenic mice,” said Dr. Huizing. “Structural
elements in the kidney that are important for filtering waste from
the blood in these animals were severely impaired and we linked
this to sialic acid deficiency. This outcome demonstrates the significance
of the ability of the body to synthesize sialic acid for kidney
development and function.”
NHGRI Clinical Director William Gahl, M.D., Ph.D., who was a co-author
of the study, said, “With respect to the disease HIBM, we are hoping
that humans with the same genetic mutation as in our mouse model
will also respond to ManNAc. The availability of these transgenic
mice will assist us greatly in assessing the appropriate dosage
of the drug to test in HIBM patients.”
To date, none of the offspring born to transgenic mice who received
ManNAc supplementation have gone on to develop muscle weakness,
but the mutant mice remain smaller than their unaffected siblings.
Studies are currently ongoing in Dr. Huizing’s laboratory to study
the mutant mice until they reach an older age when researchers
can assess any onset of muscle weakness. In addition, NHGRI clinical
researchers recently observed a temporary, but significant, improvement
in muscle strength among HIBM patients who received intravenous
immune globulin G — an effect that researchers suspect was
mediated through the provision of sialic acid present in the immune
globulin.
NHGRI researchers expect the clinical trial of ManNAc for HIBM
to begin in late summer or early fall. Based on their findings,
the group is also exploring the possibility that ManNAc may benefit
people suffering from diseases that involve damage to the cell
layers of the kidney that are required for filtering the blood.
NHGRI is one of the 27 institutes and centers at the National
Institutes of Health, which is an agency of the Department of Health
and Human Services. The NHGRI Division of Intramural Research develops
and implements technology to understand, diagnose and treat genomic
and genetic diseases. Additional information about NHGRI can be
found at www.genome.gov.
The National Institutes of Health (NIH) — The Nation's
Medical Research Agency — includes 27 Institutes and
Centers and is a component of the U.S. Department of Health and
Human Services. It is the primary federal agency for conducting
and supporting basic, clinical and translational medical research,
and it investigates the causes, treatments, and cures for both
common and rare diseases. For more information about NIH and
its programs, visit www.nih.gov.
|

