ATP III At-A-Glance: Quick Desk Reference
Table of Contents
ATP III Classification of LDL, Total, and HDL Cholesterol (mg/dL)
- LDL Cholesterol - Primary Target of Therapy
| <100 | Optimal |
| 100-129 | Near Optimal/Above Optimal |
| 130-159 | Borderline High |
| 160-189 | High |
 190 190 | Very high |
- Total Cholesterol
| <200 | Desirable |
| 200-239 | Borderline High |
 240 240 | High |
- HDL Cholesterol
| <40 | Low |
 60 60 | High |
- Clinical CHD
- Symptomatic carotid artery disease
- Peripheral arterial disease
- Abdominal aortic aneurysm.
Major Risk Factors (Exclusive of LDL Cholesterol) That Modify LDL Goals
- Cigarette smoking
- Hypertension (BP
 140/90 mmHg or on antihypertensive medication)
140/90 mmHg or on antihypertensive medication)
- Low HDL cholesterol (<40 mg/dl)*
- Family history of premature CHD (CHD in male first degree relative <55 years; CHD in female first degree relative <65 years)
- Age (men
 45 years; women
45 years; women  55 years)
55 years)
* HDL cholesterol  60 mg/dL counts as a "negative" risk factor; its presence removes one risk factor from the total count.
60 mg/dL counts as a "negative" risk factor; its presence removes one risk factor from the total count.
Note: in ATP III, diabetes is regarded as a CHD risk equivalent.
Three levels of 10-year risk:
- >20% -- CHD risk equivalent
- 10-20%
- <10%
- Establish LDL goal of therapy
- Determine need for therapeutic lifestyle changes (TLC)
- Determine level for drug consideration
LDL Cholesterol Goals and Cutpoints for Therapeutic Lifestyle Changes (TLC) and Drug Therapy in Different Risk Categories.
| Risk Category |
LDL Goal |
LDL Level at Which to Initiate Therapeutic Lifestyle Changes (TLC) |
LDL Level at Which to Consider Drug Therapy |
| CHD or CHD Risk Equivalents (10-year risk >20%) |
<100 mg/dL |
 100 mg/dL 100 mg/dL |
 130 mg/dL (100-129 mg/dL: drug optional)* 130 mg/dL (100-129 mg/dL: drug optional)* |
2+ Risk Factors (10-year risk  20%) 20%) |
<130 mg/dL |
 130 mg/dL 130 mg/dL |
10-year risk 10-20%:  130 mg/dL 130 mg/dL
10-year risk <10%:  160 mg/dL 160 mg/dL |
| 0-1 Risk Factor** |
<160 mg/dL |
 160 mg/dL 160 mg/dL |
 190 mg/dL 190 mg/dL
(160-189 mg/dL: LDL-lowering drug optional) |
* Some authorities recommend use of LDL-lowering drugs in this category if an LDL cholesterol <100 mg/dL cannot be achieved by therapeutic lifestyle changes. Others prefer use of drugs that primarily modify triglycerides and HDL, e.g., nicotinic acid or fibrate. Clinical judgment also may call for deferring drug therapy in this subcategory.
** Almost all people with 0-1 risk factor have a 10-year risk <10%, thus 10-year risk assessment in people with 0-1 risk factor is not necessary.
TLC Features
- TLC Diet:
- Saturated fat <7% of calories, cholesterol <200 mg/day
- Consider increased viscous (soluble) fiber (10-25 g/day) and plant stanols/sterols (2g/day) as therapeutic options to enhance LDL lowering
- Weight management
- Increased physical activity
- Consider drug simultaneously with TLC for CHD and CHD equivalents
- Consider adding drug to TLC after 3 months for other risk categories.
Drugs Affecting Lipoprotein Metabolism
| Drug Class |
Agents and Daily Doses |
Lipid/Lipoprotein Effects |
Side Effects |
Contraindications |
| HMG CoA reductase inhibitors (statins) |
Lovastatin (20-80 mg), Pravastatin (20-40 mg), Simvastatin (20-80 mg), Fluvastatin (20-80 mg), Atorvastatin (10-80 mg), Cerivastatin (0.4-0.8 mg) |
LDL-C 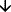 18-55% 18-55%
HDL-C 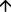 5-15% 5-15%
TG 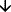 7-30% 7-30% |
Myopathy
Increased liver enzymes |
Absolute:
Active or chronic liver disease
Relative:
Concomitant use of certain drugs* |
| Bile acid Sequestrants |
Cholestyramine (4-16 g)
Colestipol (5-20 g)
Colesevelam (2.6-3.8 g) |
LDL-C 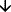 15-30% 15-30%
HDL-C 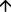 3-5% 3-5%
TG No change or increase |
Gastrointestinal distress
Constipation
Decreased absorption of other drugs |
Absolute:
dysbeta-lipoproteinemia
TG >400 mg/dL
Relative:
TG >200 mg/dL |
| Nicotinic acid |
Immediate release (crystalline) nicotinic acid (1.5-3 gm), extended release nicotinic acid (Niaspan ®) (1-2 g), sustained release nicotinic acid (1-2 g) |
LDL-C 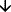 5-25% 5-25%
HDL-C 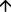 15-35% 15-35%
TG 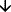 20-50% 20-50% |
Flushing
Hyperglycemia
Hyperuricemia (or gout)
Upper GI distress
Hepatotoxicity |
Absolute:
Chronic liver disease
Severe gout
Relative:
Diabetes
Hyperuricemia
Peptic ulcer disease |
| Fibric acids |
Gemfibrozil (600 mg BID)
Fenofibrate (200 mg)
Clofibrate (1000 mg BID) |
LDL-C 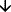 5-20% (may be increased in patients with high TG) 5-20% (may be increased in patients with high TG)
HDL-C 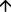 10-20% 10-20%
TG 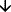 20-50% 20-50% |
Dyspepsia
Gallstones
Myopathy |
Absolute:
Severe renal disease
Severe hepatic disease |
* Cyclosporine, macrolide antibiotics, various anti-fungal agents, and cytochrome P-450 inhibitors (fibrates and niacin should be used with appropriate caution).
Clinical Identification of the Metabolic Syndrome - Any 3 of the Following:
| Risk Factor | Defining Level |
Abdominal obesity*
Men
Women |
Waist circumference**
>102 cm (>40 in)
>88 cm (>35 in) |
| Triglycerides |
 150 mg/dL 150 mg/dL |
HDL cholesterol
Men
Women |
<40 mg/dl
<50 mg/dl |
| blood pressure |
 130/ 130/ 85 mmHg 85 mmHg |
| Fasting glucose |
 110 mg/dL 110 mg/dL |
* Overweight and obesity are associated with insulin resistance and the metabolic syndrome. However, the presence of abdominal obesity is more highly correlated with the metabolic risk factors than is an elevated body mass index (BMI). Therefore, the simple measure of waist circumference is recommended to identify the body weight component of the metabolic syndrome.
** Some male patients can develop multiple metabolic risk factors when the waist circumference is only marginally increased, e.g., 94-102 cm (37-39 in). Such patients may have a strong genetic contribution to insulin resistance. They should benefit from changes in life habits, similarly to men with categorical increases in waist circumference.
Treatment of the metabolic syndrome
- Treat underlying causes (overweight/obesity and physical inactivity):
- Intensify weight management
- Increase physical activity
- Treat lipid and non-lipid risk factors if they persist despite these lifestyle therapies:
- Treat hypertension
- Use aspirin for CHD patients to reduce prothrombotic state
- Treat elevated triglycerides and/or low HDL (as shown in Step 9 below)
ATP III Classification of Serum Triglycerides (mg/dL)
| < 150 | Normal |
| 150-199 | Borderline high |
| 200-499 | High |
 500 500 | Very high |
Treatment of elevated triglycerides ( 150 mg/dL)
150 mg/dL)
- Primary aim of therapy is to reach LDL goal.
- Intensify weight management.
- Increase physical activity.
- If triglycerides are
 200 mg/dL after LDL goal is reached, set secondary goal for non-HDL cholesterol (total - HDL) 30 mg/dL higher than LDL goal.
200 mg/dL after LDL goal is reached, set secondary goal for non-HDL cholesterol (total - HDL) 30 mg/dL higher than LDL goal.
Comparison of LDL Cholesterol and Non-HDL Cholesterol Goals for Three Risk Categories
| Risk Category | LDL Goal (mg/dL) | Non-HDL Goal (mg/dL) |
| CHD and CHD Risk Equivalent (10-year risk for CHD >20%) |
<100 | <130 |
Multiple (2+) Risk Factors and 10-year risk  20% 20% |
<130 | <160 |
| 0-1 Risk Factor | <160 | <190 |
If triglycerides 200-499 mg/dL after LDL goal is reached, consider adding drug if needed to reach non-HDL goal:
- intensify therapy with LDL-lowering drug, or
- add nicotinic acid or fibrate to further lower VLDL.
If triglycerides  500 mg/dL, first lower triglycerides to prevent pancreatitis:
500 mg/dL, first lower triglycerides to prevent pancreatitis:
- very low-fat diet (
 15% of calories from fat)
15% of calories from fat)
- weight management and physical activity
- fibrate or nicotinic acid
- when triglycerides <500 mg/dL, turn to LDL-lowering therapy.
Treatment of low HDL cholesterol (<40 mg/dL)
- First reach LDL goal, then:
- Intensify weight management and increase physical activity.
- If triglycerides 200-499 mg/dL, achieve non-HDL goal.
- If triglycerides <200 mg/dL (isolated low HDL) in CHD or CHD equivalent, consider nicotinic acid or fibrate.
U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES
Public Health Service
National Institutes of Health
National Heart, Lung, and Blood Institute
NIH Publication No. 01-3305
May 2001
500