|
|
|||||
|
|
Biologic characteristics and behavioral traits can influence an individual's risk of developing malaria and, on a larger scale, the intensity of transmission in a population. Genetic FactorsBiologic characteristics present from birth can protect against certain types of malaria. Two genetic factors, both associated with human red blood cells, have been shown to be epidemiologically important. Persons who have the sickle cell trait (heterozygotes for the abnormal hemoglobin gene HbS) are relatively protected against P. falciparum malaria and thus enjoy a biologic advantage. Because P. falciparum malaria has been a leading cause of death in Africa since remote times, the sickle cell trait is now more frequently found in Africa and in persons of African ancestry than in other population groups. Persons who are negative for the Duffy blood group have red blood cells that are resistant to infection by P. vivax. Since the majority of Africans are Duffy negative, P. vivax is rare in Africa south of the Sahara, especially West Africa. In that area, the niche of P. vivax has been taken over by P. ovale, a very similar parasite that does infect Duffy-negative persons. Other genetic factors related to red blood cells also influence malaria, but to a lesser extent. Various genetic determinants (such as the "HLA complex", which plays a role in control of immune responses) may equally influence an individual's risk of developing severe malaria. Acquired ImmunityAcquired immunity greatly influences how malaria affects an individual and a community. After repeated attacks of malaria a person develops a partially protective immunity. Such "semi-immune" persons often can still be infected by malaria parasites but do not develop severe disease, and, in fact, frequently lack any typical malaria symptoms.
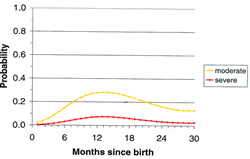
In areas with high P. falciparum transmission (most of Africa south of the Sahara), newborns will be protected during the first few months of life presumably by maternal antibodies transferred to them through the placenta. As these antibodies decrease with time, these young children become vulnerable to disease and death by malaria. If they survive to an older age (2-5 years) they will have reached a protective semi-immune status. Thus in high transmission areas, young children are a major risk group and are targeted preferentially by malaria control interventions. In areas with lower transmission (such as Asia and Latin America), infections are less frequent and a larger proportion of the older children and adults have no protective immunity. In such areas, malaria disease can be found in all age groups, and epidemics can occur.
Pregnancy and MalariaPregnancy decreases immunity against many infectious diseases. Women who have developed protective immunity against P. falciparum tend to lose this protection when they become pregnant (especially during the first and second pregnancies). Malaria during pregnancy is harmful not only to the mothers but also to the unborn children. The latter are at greater risk of being delivered prematurely or with low birth weight, with consequently decreased chances of survival during the early months of life. For this reason pregnant women are also targeted (in addition to young children) for protection by malaria control programs in endemic countries.
Behavioral FactorsHuman behavior, often dictated by social and economic reasons, can influence the risk of malaria for individuals and communities. For example:
Human behavior in endemic countries also determines in part how successful malaria control activities will be in their efforts to decrease transmission. The governments of malaria-endemic countries often lack financial resources. As a consequence, health workers in the public sector are often underpaid and overworked. They lack equipment, drugs, training, and supervision. The local populations are aware of such situations when they occur, and cease relying on the public sector health facilities. Conversely, the private sector suffers from its own problems. Regulatory measures often do not exist or are not enforced. This encourages private consultations by unlicensed, costly health providers, and the anarchic prescription and sale of drugs (some of which are counterfeit products). Correcting this situation is a tremendous challenge, that must be addressed if malaria control is to be successful. Page last modified : April 23, 2004 Content source: Division of Parasitic Diseases National Center for Zoonotic, Vector-Borne, and Enteric Diseases (ZVED)
|
|
|||||||||||||||||||||||||
| Home | Policies and Regulations | Disclaimer | e-Government | FOIA | Contact Us | ||||||
|