Agency for Toxic Substances and Disease Registry
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Learning Objective |
Upon completion of this section, you should be able to
|
Introduction |
According to the American Thoracic Society (2004), “asbestos has been the largest cause of occupational cancer in the United States and a significant cause of disease and disability from nonmalignant disease.” It has been estimated that the cumulative total number of asbestos-associated deaths in the United States may exceed 200,000 by the year 2030 (Nicholson et al. 1982). Depending on the level of exposure, inhalation of asbestos fibers can cause different diseases such as
Any combination of these syndromes (or all four of them) can be present in a single patient. Clinically, it is important to distinguish nonmalignant conditions from malignant diseases; differential diagnosis will be discussed further in later sections of this document. |
Parenchymal Asbestosis |
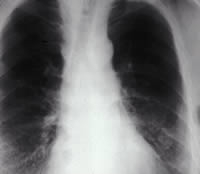
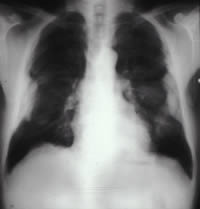
Parenchymal asbestosis is a diffuse interstitial fibrosis resulting from inhalation of asbestos fibers. Asbestos fibers inhaled deep into the lung parenchyma become lodged in the tissue, resulting in diffuse alveolar and interstitial fibrosis. The fibrosis first occurs in the respiratory bronchioles, particularly the subpleural portions of the lower lobes. The fibrosis can progress to include the alveolar walls. Fibrosis tends to progress even after exposure ceases (Khan et al. 2004). This fibrosis can lead to
Parenchymal asbestosis is characterized by the following radiographic changes: fine, irregular opacities in both lung fields (especially in the bases) and septal lines that progress to honeycombing and sometimes, in more severe disease, obscuration of the heart border and hemi-diaphragm, the so-called shaggy heart sign (Khan et al. 2004). Radiographic changes depend on the duration, frequency, and intensity of exposure, however. Patients with parenchymal asbestosis may have elevated levels of antinuclear antibody and rheumatoid factors and a progressive decrease in total lymphocyte count with advancing fibrosis. Parenchymal asbestosis has no unique pathognomonic signs or symptoms, but diagnosis is made by the constellation of clinical, functional, and radiographic findings as outlined by the American Thoracic Society (American Thoracic Society 2004). These criteria include
The table below describes the natural history associated with parenchymal asbestosis. |
| Parameter | Typical Findings |
|---|---|
|
Sufficient exposures |
Usually associated with high-level occupational exposures (Khan et al., 2004). |
|
Latency periods |
Radiographic changes: <20 years. |
Risk of asbestosis |
Asbestosis develops in 49-52% of adults with occupational levels of asbestos exposure (Khan et al. 2004). |
|
Co-morbid conditions |
Increased risk for lung cancer and mesothelioma, though both can occur without parenchymal asbestosis (Weiss 1999; Hillerdal 1999) |
|
Mortality and Morbidity |
Severe asbestosis may lead to respiratory failure over 12-24 years. Many patients with asbestosis die of other causes such as asbestos-associated lung cancer (38%), mesothelioma (9%), and other causes (32%) (Rosenberg 1997, Kamp and Weitzman 1997) |
Asbestos-Related Pleural Abnormalities |
Asbestos-related pleural abnormalities (also called pleural asbestosis) encompass four types of pleural changes
The pleura are more sensitive to asbestos than the lung parenchyma, so the effects of asbestos exposure show here first and occur at much lower doses than the fibrotic changes in the lung (Peacock et al. 2000; Khan et al. 2004). Pleural plaques are well-circumscribed areas of thickening, usually located bilaterally on the parietal pleura. They are usually asymptomatic, though they can cause small reductions in lung function (American Thoracic Society 2004). Pleural plaques are the most common manifestations of asbestos exposure; the highest rate (58%) is found in insulation workers (American Thoracic Society 2004; Peacock et al. 2000). The presence of pleural plaques in the general environmentally exposed population in developed societies is in the range of 0.5%-8% (Khan et al., 2004). Indeed, they are considered a biomarker of asbestos exposure, depending on length from first exposure, rather than a threshold dose like asbestosis (Peacock et al. 2000). Pleural plaques can also form following exposure to:
(Chapman et al. 2003; Rockoff and Robin 2002). Benign asbestos pleural effusions are small unilateral effusions, often occurring as blood-stained exudates with various types of blood cells and mesothelial cells (Khan et al., 2004). These effusions are among the earliest manifestations of asbestos exposure; they can occur within 10 years of exposure (Chapman et al., 2003). They are usually asymptomatic. Rarely, they can cause pain, fever, and dyspnea. These effusions typically last for months, and may occasionally recur. Their presence can precede the occurrence of diffuse pleural thickening (Chapman et al. 2003). Diffuse pleural thickening is a noncircumscribed fibrous thickening of the visceral pleura with areas of adherence to the parietal pleura and obliteration of the pleural space. It can be associated with more extensive asbestos exposure than diffuse pleural plaques (Chapman et al. 2003). And, diffuse pleural thickening, in fact, has been reported to occur in 10% of patients with asbestosis (Khan et al. 2004). Diffuse pleural thickening can occur after benign pleural effusions. The fibrotic areas are ill-defined, involving costophrenic angles, apices, lung bases, and interlobar fissures. Diffuse pleural thickening can be associated with mild (or, rarely, moderate to severe) restrictive pulmonary function deficits such as decreased ventilatory capacity. When this occurs, the patient may experience progressive dyspnea and chest pain (Chapman et al. 2003; Rockoff et al. 2002). Rounded atelectasis (or folded lung) occurs when blebs of lung tissue are caught in bands of fibrous pleural tissue with in-drawing of the bronchi and vessels (Khan et al. 2004). This produces a distinctive X-ray appearance: a rounded pleural mass with bands of lung tissue radiating outwards. This condition is usually asymptomatic, though some patients develop dyspnea or dry cough. The course is usually stable or slowly progressive. Folded lung is the least common asbestos-related benign pleural disease, and it is not only associated with asbestosis exposure but can occur following other exposures and medical conditions. However, asbestos exposure is the leading cause of rounded atelectasis, accounting for 29%-86% of cases. It can rarely also co-occur with lung cancer (Stathopoulos et al. 2005). The differential causes of rounded atelectasis includes
The table below shows typical findings and natural history associated with asbestos-related pleural abnormalities. |
| Parameter | Pleural Plaques | Pleural Effusions | Diffuse Pleural Thickening | Rounded Atelectasis |
|---|---|---|---|---|
Typical exposures |
Can occur with short low level exposures or high level occupational exposures. The incidence in the population will increase as exposure increases. |
|
Usually associated with moderate- to high-level exposures. Less specific for asbestos exposure than for pleural plaques |
May occur with occupational level and environmental exposures. Has other causes besides asbestos exposure. |
Average latency periods |
20–30 years |
10 years |
15 years |
N/A |
Co-morbid conditions |
Since the presence of these plaques is an indicator of asbestos exposure, there is an increased incidence of asbestos related diseases associated with them. |
Other asbestos related diseases |
Other asbestos related diseases. Can follow benign pleural effusions. |
Follows benign pleural effusions; can co-exist with other asbestos-related diseases or its other causes. |
Mortality and |
Not fatal/usually asymptomatic; incidental finding. |
Not fatal. Clinical presentation ranges from asymptomatic to pleuritic chest pain and fever. |
Not fatal. If severe, can cause dyspnea. |
Not fatal. Usually asymptomatic; if severe, chest pain, dyspnea, and cough. Usually no functional impairment unless accompanied by other asbestos-related disease. |
|
Source: American Thoracic Society 2004; Chapman et al., 2003; Khan et al. 2004; Stathopoulos et al. 2005) |
||||
Lung Carcinoma |
Most lung cancers are associated with exposure to tobacco smoke. Smokers have a 13-fold higher risk than nonsmokers for lung cancer, and people with long-term passive exposure to tobacco smoke are at 1.5 times higher risk for lung cancer than are people who are never exposed to tobacco smoke. Lung cancer currently accounts for 28% of all cancer deaths in the United States (Minna 2005). Exposure to asbestos is associated with all major histological types of lung carcinoma (adenocarcinoma, squamous cell carcinoma, and oat-cell carcinoma). It is estimated that 4%-12% of lung cancers are related to occupational levels of exposure to asbestos (Henderson et al. 2004). It is estimated that 20%-25% of heavily exposed asbestos workers will develop bronchogenic carcinomas (Khan et al., 2004). Whether asbestos exposure will lead to lung cancer depends on several factors
Most asbestos-related lung cancers reflect the dual influence of asbestos exposure and smoking (Henderson et al. 2004). Smoking and asbestos exposure have a multiplicative effect on the risk of lung cancer (Lee 2001; Henderson et al. 2004; ATSDR 2001). Asbestos as the sole contributing factor for an individual patient can be difficult to prove especially when the patient has other risk factors for lung cancer. The presence of parenchymal asbestosis is an indicator of high-level asbestos exposure, but lung cancer can occur without asbestosis. One of the best known sets of criteria to guide the clinician regarding whether asbestos contributed to lung cancer in an asbestos-exposed individual is the Helsinki criteria. For these criteria, some of the markers for attributing asbestos exposure as a contributing factor to lung cancer are
The table below shows typical findings associated with lung carcinoma. |
| Parameter | Typical Findings |
|---|---|
Typical exposures |
Large cumulative exposure (short-term, high-level exposures or long-term, moderate-level exposures). |
Latency periods |
20–30 years |
Clinical presentation |
Only 5%-15% of patients are asymptomatic when diagnosed. Most present with cough, hemoptysis, wheeze, dyspnea (Minna, 2005). |
Co morbid conditions |
Asbestosis, other asbestos-related diseases. Paraneoplastic syndromes associated with lung cancer. |
Mortality |
Same as lung carcinoma with other causes - 14% five year survival rate (British Thoracic Society 2001). |
Pleural Mesothelioma |
Diffuse malignant mesothelioma is a tumor arising from the thin serosal membrane of the body cavities, arising from the pleura, peritoneum, tunica vaginalis testis, and ovaries. It is a rare neoplasm, accounting for less than 5% of pleural malignancies. There are three histological types of malignant mesothelioma: epithelial, mixed, and sarcomatous. Of malignant mesotheliomas, 80% affect the pleura, and 20% of all malignant mesotheliomas affect the peritoneum (Khan et al. 2004). Peritoneal mesothelioma is discussed in the next section. In most cases, the tumor is rapidly invasive locally (Lee et al. 2000). Patients with malignant pleural mesothelioma can have sudden onset of pleural effusion or thickening, dyspnea, and chest pain. By the time symptoms appear, the disease is most often rapidly fatal (British Thoracic Society 2001). Pleural mesothelioma is a signal tumor for asbestos exposure; other causes are uncommon. The risk of mesothelioma does depend on the amount of asbestos exposure (Weill et al. 2004). All types of asbestos can cause mesothelioma, but some researchers believe that the amphibole form is more likely to induce mesothelioma than the serpentine form (ATSDR 2001a). In 2000, about 3,000 people in the United States died of mesothelioma (Lee et al. 2000; Khan et al. 2004) According to the National Cancer Institute’s SEER data, there was an increase in the incidence of mesothelioma in the United States from the early 1970s to the mid-1990s, as disease developed in people exposed during peak asbestos exposure years (1940–1970). Mesothelioma incidence has probably started to decline in the United States, although it may still be increasing in Europe and Australia because of more abundant and prolonged use of asbestos in these countries than in the United States (Weill et al. 2004). The table below shows typical findings associated with pleural mesothelioma. |
| Parameter | Typical Findings |
|---|---|
Typical exposures |
Short-term, high-level exposures or chronic low-level exposures, especially to amphibole asbestos; incidence increases in dose-related manner (Hillerdal 1999). |
Latency periods |
10–57 years (30–40 years typical). |
Clinical presentation |
Frequently presents with chest pain accompanied by pleural mass or pleural effusion on chest X-ray (British Thoracic Society 2001). |
Mortality |
High . The typical 1-year survival rate is <30%. |
Key Points |
|
Progress Check |