|
Treatment
Getting a Second Opinion
Treatment Methods
Treatment Choices by Stage
Many women with breast cancer want to take an active part in making decisions
about their medical care. It is natural to want to learn all you can about your
disease and treatment choices. Knowing more about breast cancer helps many
women cope.
Shock and stress after the diagnosis can make it hard to think of everything you
want to ask your doctor. It often helps to make a list of questions before an
appointment. To help remember what the doctor says, you may take notes or ask
whether you may use a tape recorder. You may also want to have a family member
or friend with you when you talk to the doctor - to take part in the discussion,
to take notes, or just to listen. You do not need to ask all your questions at
once. You will have other chances to ask your doctor or nurse to explain things
that are not clear and to ask for more details.
Your doctor may refer you to a specialist, or you may ask for a referral.
Specialists who treat breast cancer include
surgeons,
medical oncologists,
and
radiation oncologists.
You also may be referred to a
plastic surgeon.
Before starting treatment, you might want a second opinion about your diagnosis
and treatment plan. Many insurance companies cover a second opinion if you or
your doctor requests it. It may take some time and effort to gather medical
records and arrange to see another doctor. You may have to gather your
mammogram films, biopsy slides, pathology report, and proposed treatment plan.
Usually it is not a problem to take several weeks to get a second opinion. In
most cases, the delay in starting treatment will not make treatment less
effective. To make sure, you should discuss this delay with your doctor. Some
women with breast cancer need treatment right away.
There are a number of ways to find a doctor for a second opinion:
-
Your doctor may refer you to one or more specialists. At cancer centers,
several specialists often work together as a team.
-
NCI's Cancer Information Service, at 1-800-4-CANCER, can tell you about nearby
treatment centers. Information Specialists also can provide online assistance
through
LiveHelp at http://www.cancer.gov/cis.
-
A local or state medical society, a nearby hospital, or a medical school can
usually provide the names of specialists.
-
The American Board of Medical Specialties (ABMS) has a list of doctors who have
had training and passed exams in their specialty. You can find this list in the
Official ABMS Directory of Board Certified Medical Specialists. This Directory
is in most public libraries. Also, ABMS offers this information at
http://www.abms.org. (Click on "Who's Certified.")
-
NCI provides a helpful fact sheet called "How To Find a Doctor or Treatment
Facility If You Have Cancer."
Women with breast cancer have many treatment options. These include
surgery,
radiation therapy,
chemotherapy,
hormone therapy,
and
biological therapy.
These
options are described below. Many women receive more than one
type of treatment.
The choice of treatment depends mainly on the stage of the disease. Treatment
options by stage are described below.
Your doctor can describe your treatment choices and the expected results. You
may want to know how treatment may change your normal activities. You may want
to know how you will look during and after treatment. You and your doctor can
work together to develop a treatment plan that reflects your medical needs and
personal values.
Cancer treatment is either
local therapy
or
systemic therapy:
-
Local therapy: Surgery and radiation therapy are local treatments. They
remove or destroy cancer in the breast. When breast cancer has spread to other
parts of the body, local therapy may be used to control the disease in those
specific areas.
-
Systemic therapy: Chemotherapy, hormone therapy, and biological therapy
are systemic treatments. They enter the bloodstream and destroy or control
cancer throughout the body. Some women with breast cancer have systemic therapy
to shrink the tumor before surgery or radiation. Others have systemic therapy
after surgery and/or radiation to prevent the cancer from coming back. Systemic
treatments also are used for cancer that has spread.
Because cancer treatments often damage healthy cells and tissues,
side effects
are common. Side effects depend mainly on the type and extent of the treatment.
Side effects may not be the same for each woman, and they may change from one
treatment session to the next.
Before treatment starts, your health care team will explain possible side
effects and suggest ways to help you manage them. NCI provides helpful booklets
about cancer treatments and coping with side effects. These include
Radiation Therapy and You,
Chemotherapy and You, Biological Therapy, and
Eating Hints for
Cancer Patients.
At any stage of disease,
supportive care
is available to control pain and other
symptoms, to relieve the
side effects of treatment, and to ease emotional
concerns. Information about such care is available on NCI's Web site at
http://www.cancer.gov/cancertopics/coping and from Information
Specialists at 1-800-4-CANCER or
LiveHelp.
You may want to talk to your doctor about taking part in a
clinical trial,
a
research study of new treatment methods. The section on "The Promise of Cancer
Research" has more information about clinical trials.
|
You may want to ask your doctor these questions before your treatment begins:
-
What did the hormone receptor test show? What did other lab tests show?
-
Do any lymph nodes show signs of cancer?
-
What is the stage of the disease? Has the cancer spread?
-
What is the goal of treatment? What are my treatment choices? Which do you
recommend for me? Why?
-
What are the expected benefits of each kind of treatment?
-
What are the risks and possible side effects of each treatment? How can side
effects be managed?
-
What can I do to prepare for treatment?
-
Will I need to stay in the hospital? If so, for how long?
-
What is the treatment likely to cost? Will my insurance cover the cost?
-
How will treatment affect my normal activities?
-
Would a clinical trial be appropriate for me?
|
Surgery is the most common treatment for breast cancer. There are several types
of surgery. (See pictures below.) Your doctor can explain each type,
discuss and compare the benefits and risks, and describe how each will change
the way you look:
-
Breast-sparing surgery: An operation to remove the cancer but not the
breast is breast-sparing surgery. It is also called
breast-conserving surgery,
lumpectomy,
segmental mastectomy,
and
partial mastectomy.
Sometimes an
excisional biopsy serves as a lumpectomy because the surgeon removes the whole
lump.
The surgeon often removes the underarm lymph nodes as well. A separate incision
is made. This procedure is called an
axillary lymph node dissection.
It shows
whether cancer cells have entered the lymphatic system.
After breast-sparing surgery, most women receive radiation therapy to the
breast. This treatment destroys cancer cells that may remain in the breast.
-
Mastectomy:
An operation to remove the breast (or as much of the breast
tissue as possible) is a mastectomy. In most cases, the surgeon also removes
lymph nodes under the arm. Some women have radiation therapy after surgery.
Studies have found equal survival rates for breast-sparing surgery (with
radiation therapy) and mastectomy for Stage I and Stage II breast cancer.
Sentinel lymph node biopsy
is a new method of checking for cancer cells in the
lymph nodes. A surgeon removes fewer lymph nodes, which causes fewer side
effects. (If the doctor finds cancer cells in the axillary lymph nodes, an
axillary lymph node dissection usually is done.) Information about ongoing
studies of sentinel lymph node biopsy is in the section on "The
Promise of Cancer Research." These studies will learn the lasting effects of
removing fewer lymph nodes.
|
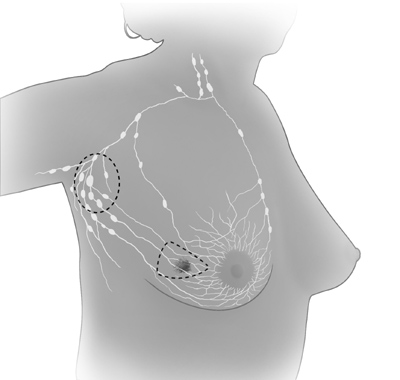
| In breast-sparing surgery, the surgeon removes the tumor in the breast and some
tissue around it. The surgeon may also remove lymph nodes under the arm. The
surgeon sometimes removes some of the lining over the chest muscles below the
tumor. |
|
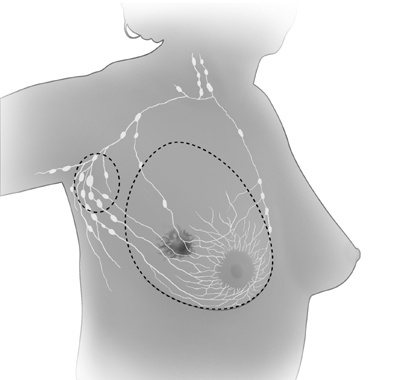
| In
total
(simple)
mastectomy,
the surgeon removes the whole breast. Some lymph
nodes under the arm may also be removed. |
|
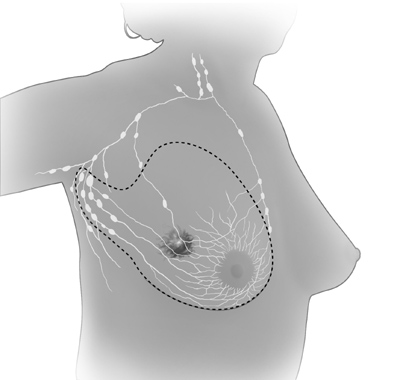
| In
modified radical mastectomy,
the surgeon removes the whole breast, and most
or all of the lymph nodes under the arm. Often, the lining over the chest
muscles is removed. A small chest muscle also may be taken out to make it
easier to remove the lymph nodes. |
You may choose to have
breast reconstruction.
This is
plastic surgery
to
rebuild the shape of the breast. It may be done at the same time as a
mastectomy or later. If you are considering reconstruction, you may wish to
talk with a plastic surgeon before having a mastectomy. More information is in the "Breast Reconstruction" section.
The time it takes to heal after surgery is different for each woman. Surgery
causes pain and tenderness. Medicine can help control the pain. Before surgery,
you should discuss the plan for pain relief with your doctor or nurse. After
surgery, your doctor can adjust the plan if you need more relief. Any kind of
surgery also carries a risk of infection, bleeding, or other problems. You
should tell your health care provider right away if you develop any problems.
You may feel off balance if you've had one or both breasts removed. You may
feel more off balance if you have large breasts. This imbalance can cause
discomfort in your neck and back. Also, the skin where your breast was removed
may feel tight. Your arm and shoulder muscles may feel stiff and weak. These
problems usually go away. The doctor, nurse, or
physical therapist
can suggest
exercises to help you regain movement and strength in your arm and shoulder.
Exercise can also reduce stiffness and pain. You may be able to begin gentle
exercises within days of surgery.
Because nerves may be injured or cut during surgery, you may have numbness and
tingling in your chest, underarm, shoulder, and upper arm. These feelings
usually go away within a few weeks or months. But for some women, numbness does
not go away.
Removing the lymph nodes under the arm slows the flow of
lymph
fluid. The fluid
may build up in your arm and hand and cause swelling. This swelling is
lymphedema.
Lymphedema can develop right after surgery or months to years
later.
You will need to protect your arm and hand on the treated side for the rest of
your life:
-
Avoid wearing tight clothing or jewelry on your affected arm
-
Carry your purse or luggage with the other arm
-
Use an electric razor to avoid cuts when shaving under your arm
-
Have shots, blood tests, and blood pressure measurements on the other arm
-
Wear gloves to protect your hands when gardening and when using strong
detergents
-
Have careful manicures and avoid cutting your cuticles
-
Avoid burns or sunburns to your affected arm and hand
You should ask your doctor how to handle any cuts, insect bites, sunburn, or
other injuries to your arm or hand. Also, you should contact the doctor if your
arm or hand is injured, swells, or becomes red and warm.
If lymphedema occurs, the doctor may suggest raising your arm above your heart
whenever you can. The doctor may show you hand and arm exercises. Some women
with lymphedema wear an elastic sleeve to improve lymph circulation.
Medication, manual lymph drainage (massage), or use of a machine that gently
compresses the arm may also help. You may be referred to a physical therapist
or another specialist.
More information about lymphedema is available on NCI's Web site at http://www.cancer.gov
and from Information Specialists at 1-800-4-CANCER or
LiveHelp.
|
You may want to ask your doctor these questions before having surgery:
-
What kinds of surgery can I consider? Is breast-sparing surgery an option for
me? Which operation do you recommend for me? Why?
-
Will my lymph nodes be removed? How many? Why?
-
How will I feel after the operation? Will I have to stay in the hospital?
-
Will I need to learn how to take care of myself or my incision when I get home?
-
Where will the scars be? What will they look like?
-
If I decide to have plastic surgery to rebuild my breast, how and when can that
be done? Can you suggest a plastic surgeon for me to contact?
-
Will I have to do special exercises to help regain motion and strength in my
arm and shoulder? Will a physical therapist or nurse show me how to do the
exercises?
-
Is there someone I can talk with who has had the same surgery I'll be having?
|
Radiation therapy (also called radiotherapy) uses high-energy rays to kill
cancer cells. Most women receive radiation therapy after breast-sparing
surgery. Some women receive radiation therapy after a mastectomy. Treatment
depends on the size of the tumor and other factors. The radiation destroys
breast cancer cells that may remain in the area.
Some women have radiation therapy before surgery to destroy cancer cells and
shrink the tumor. Doctors use this approach when the tumor is large or may be
hard to remove. Some women also have chemotherapy or hormone therapy before
surgery.
Doctors use two types of radiation therapy to treat breast cancer. Some women
receive both types:
-
External radiation: The radiation comes from a large machine outside the
body. Most women go to a hospital or clinic for treatment. Treatments are
usually 5 days a week for several weeks.
-
Internal radiation
(implant radiation): Thin plastic tubes (implants)
that hold a
radioactive
substance are put directly in the breast. The implants
stay in place for several days. A woman stays in the hospital while she has
implants. Doctors remove the implants before she goes home.
Side effects depend mainly on the dose and type of radiation and the part of
your body that is treated.
It is common for the skin in the treated area to become red, dry, tender, and
itchy. Your breast may feel heavy and tight. These problems will go away over
time. Toward the end of treatment, your skin may become moist and "weepy."
Exposing this area to air as much as possible can help the skin heal.
Bras and some other types of clothing may rub your skin and cause soreness. You
may want to wear loose-fitting cotton clothes during this time. Gentle skin
care also is important. You should check with your doctor before using any
deodorants, lotions, or creams on the treated area. These effects of radiation
therapy on the skin will go away. The area gradually heals once treatment is
over. However, there may be a lasting change in the color of your skin.
You are likely to become very tired during radiation therapy, especially in the
later weeks of treatment. Resting is important, but doctors usually advise
patients to try to stay as active as they can.
Although the side effects of radiation therapy can be distressing, your doctor
can usually relieve them.
|
You may want to ask your doctor these questions before having radiation therapy:
-
How will radiation be given?
-
When will treatment start? When will it end? How often will I have treatments?
-
How will I feel during treatment? Will I be able to drive myself to and from
treatment?
-
How will we know the treatment is working?
-
What can I do to take care of myself before, during, and after treatment?
-
Will treatment affect my skin?
-
How will my chest look afterward?
-
Are there any long-term effects?
-
What is the chance that the cancer will come back in my breast?
-
How often will I need checkups?
|
Chemotherapy uses anticancer drugs to kill cancer cells. Chemotherapy for
breast cancer is usually a combination of drugs. The drugs may be given as a
pill or by
injection
into a vein
(IV). Either way, the drugs enter the
bloodstream and travel throughout the body.
Women with breast cancer can have chemotherapy in an outpatient part of the
hospital, at the doctor's office, or at home. Some women need to stay in the
hospital during treatment.
Side effects depend mainly on the specific drugs and the dose. The drugs affect
cancer cells and other cells that divide rapidly:
-
Blood cells: These cells fight infection, help your blood to clot, and
carry oxygen to all parts of the body. When drugs affect your blood cells, you
are more likely to get infections, bruise or bleed easily, and feel very weak
and tired. Years after chemotherapy, some women have developed leukemia (cancer
of the blood cells).
-
Cells in hair roots: Chemotherapy can cause hair loss. Your hair will
grow back, but it may be somewhat different in color and texture.
-
Cells that line the
digestive tract:
Chemotherapy can cause poor
appetite, nausea and vomiting, diarrhea, or mouth and lip sores.
Your doctor can suggest ways to control many of these side effects.
Some drugs used for breast cancer can cause tingling or numbness in the hands
or feet. This problem usually goes away after treatment is over. Other problems
may not go away. In some women, the drugs used for breast cancer may weaken the
heart.
Some anticancer drugs can damage the
ovaries.
The ovaries may stop making
hormones. You may have symptoms of menopause. The symptoms include hot flashes
and vaginal dryness. Your menstrual periods may no longer be regular or may
stop. Some women become
infertile
(unable to become pregnant). For women over
the age of 35,
infertility
is likely to be permanent.
On the other hand, you may remain
fertile
during chemotherapy and be able to
become pregnant. The effects of chemotherapy on an unborn child are not known.
You should talk to your doctor about birth control before treatment begins.
Some breast tumors need hormones to grow. Hormone therapy keeps cancer cells
from getting or using the natural hormones they need. These hormones are
estrogen and progesterone. Lab tests can show if a breast tumor has hormone
receptors. If you have this kind of tumor, you may have hormone therapy.
This treatment uses drugs or surgery:
-
Drugs: Your doctor may suggest a drug that can block the natural
hormone. One drug is
tamoxifen,
which blocks estrogen. Another type of drug
prevents the body from making the female hormone
estradiol.
Estradiol is a form
of estrogen. This type of drug is an
aromatase inhibitor.
If you have not gone
through menopause, your doctor may give you a drug that stops the ovaries from
making estrogen.
-
Surgery: If you have not gone through menopause, you may have surgery to
remove your ovaries. The ovaries are the main source of the body's estrogen. A
woman who has gone through menopause does not need surgery. (The ovaries
produce less estrogen after menopause.)
The side effects of hormone therapy depend largely on the specific drug or type
of treatment. Tamoxifen is the most common hormone treatment. In general, the
side effects of tamoxifen are similar to some of the symptoms of menopause. The
most common are hot flashes and vaginal discharge. Other side effects are
irregular menstrual periods, headaches, fatigue, nausea, vomiting, vaginal
dryness or itching, irritation of the skin around the vagina, and skin rash.
Not all women who take tamoxifen have side effects.
It is possible to become pregnant when taking tamoxifen. Tamoxifen may harm the
unborn baby. If you are still menstruating, you should discuss birth control
methods with your doctor.
Serious side effects of tamoxifen are rare. However, it can cause blood clots
in the veins. Blood clots form most often in the legs and in the lungs. Women
have a slight increase in their risk of stroke.
Tamoxifen can cause cancer of the uterus. Your doctor should perform regular
pelvic exams. You should tell your doctor about any unusual vaginal bleeding
between exams.
When the ovaries are removed, menopause occurs at once. The side effects are
often more severe than those caused by natural menopause. Your health care
provider can suggest ways to cope with these side effects.
Biological therapy helps the
immune system
fight cancer. The immune system is
the body's natural defense against disease.
Some women with breast cancer that has spread receive a biological therapy
called Herceptin® (trastuzumab).
It is a
monoclonal antibody. It is made in the
laboratory and binds to cancer cells.
Herceptin is given to women whose lab tests show that a breast tumor has too
much of a specific protein known as HER2. By blocking HER2, it can slow or stop
the growth of the cancer cells.
Herceptin is given by vein. It may be given alone or with chemotherapy.
The first time a woman receives Herceptin, the most common side effects are
fever and chills. Some women also have pain, weakness, nausea, vomiting,
diarrhea, headaches, difficulty breathing, or rashes. Side effects usually
become milder after the first treatment.
Herceptin also may cause heart damage. This may lead to heart failure.
Herceptin can also affect the lungs. It can cause breathing problems that
require a doctor at once. Before you receive Herceptin, your doctor will check
for your heart and lungs. During treatment, your doctor will watch for signs of
lung problems.
|
You may want to ask your doctor these questions before having chemotherapy,
hormone therapy, or biological therapy:
-
What drugs will I be taking? What will they do?
-
If I need hormone treatment, would you recommend drugs or surgery to remove my
ovaries?
-
When will treatment start? When will it end? How often will I have treatments?
-
Where will I go for treatment? Will I be able to drive home afterward?
-
What can I do to take care of myself during treatment?
-
How will we know the treatment is working?
-
Which side effects should I tell you about?
-
Will there be long-term effects?
|
Your treatment options depend on the stage of your disease and these factors:
-
The size of the tumor in relation to the size of your breast
-
The results of lab tests (such as whether the breast cancer cells need hormones
to grow)
-
Whether you have gone through menopause
-
Your general health
Below are brief descriptions of common treatments for each stage. Other
treatments may be appropriate for some women. Clinical trials can be an option
at all stages of breast cancer. "The Promise of Cancer Research" section
has information about clinical trials.
Stage 0
Stage 0 breast cancer refers to lobular carcinoma in situ (LCIS) or ductal
carcinoma in situ (DCIS):
-
LCIS: Most women with LCIS do not have treatment. Instead, the doctor may
suggest regular checkups to watch for signs of breast cancer.
Some women take tamoxifen to reduce the risk of developing breast cancer.
Others may take part in studies of promising new preventive treatments.
Having LCIS in one breast increases the risk of cancer for both breasts. A very
small number of women with LCIS try to prevent cancer with surgery to remove
both breasts. This is a
bilateral prophylactic mastectomy. The surgeon usually
does not remove the underarm lymph nodes.
-
DCIS: Most women with DCIS have breast-sparing surgery followed by radiation
therapy. Some women choose to have a total mastectomy. Underarm lymph nodes are
not usually removed. Women with DCIS may receive tamoxifen to reduce the risk
of developing invasive breast cancer.
Stages I, II, IIIA, and Operable IIIC
Women with Stage I, II, IIIA, and operable (can treat with surgery) IIIC breast
cancer may have a combination of treatments. Some may have breast-sparing
surgery followed by radiation therapy to the breast. This choice is common for
women with Stage I or II breast cancer. Others decide to have a mastectomy.
With either approach, women (especially those with Stage II or IIIA breast
cancer) often have lymph nodes under the arm removed. The doctor may suggest
radiation therapy after mastectomy if cancer cells are found in 1 to 3 lymph
nodes under the arm, or if the tumor in the breast is large. If cancer cells
are found in more than 3 lymph nodes under the arm, the doctor usually will
suggest radiation therapy after mastectomy.
The choice between breast-sparing surgery (followed by radiation therapy) and
mastectomy depends on many factors:
-
The size, location, and stage of the tumor
-
The size of the woman's breast
-
Certain features of the cancer
-
How the woman feels about saving her breast
-
How the woman feels about radiation therapy
-
The woman's ability to travel to a radiation treatment center
Some women have chemotherapy before surgery. This is
neoadjuvant therapy
(treatment before the main treatment). Chemotherapy before surgery may shrink a
large tumor so that breast-sparing surgery is possible. Women with large Stage
II or IIIA breast tumors often choose this treatment.
After surgery, many women receive
adjuvant therapy.
Adjuvant therapy is
treatment given after the main treatment to increase the chances of a cure.
Radiation treatment can kill cancer cells in and near the breast. Women also
may have systemic treatment such as chemotherapy, hormone therapy, or both.
This treatment can destroy cancer cells that remain anywhere in the body. It
can prevent the cancer from coming back in the breast or elsewhere.
Stages IIIB and Inoperable IIIC
Women with Stage IIIB (including inflammatory breast cancer) or inoperable
Stage IIIC breast cancer usually have chemotherapy. (Inoperable cancer means it
cannot be treated with surgery.)
If the chemotherapy shrinks the tumor, the doctor then may suggest further
treatment:
-
Mastectomy: The surgeon removes the breast. In most cases, the lymph
nodes under the arm are removed. After surgery, a woman may receive radiation
therapy to the chest and underarm area.
-
Breast-sparing surgery: The surgeon removes the cancer but not the
breast. In most cases, the lymph nodes under the arm are removed. After
surgery, a woman may receive radiation therapy to the breast and underarm area.
-
Radiation therapy instead of surgery: Some women have radiation therapy
but no surgery. The doctor also may recommend more chemotherapy, hormone therapy, or both. This
therapy may help prevent the disease from coming back in the breast or
elsewhere.
Stage IV
In most cases, women with Stage IV breast cancer have hormone therapy,
chemotherapy, or both. Some also may have biological therapy. Radiation may be
used to control tumors in certain parts of the body. These treatments are not
likely to cure the disease, but they may help a woman live longer.
Many women have supportive care along with anticancer treatments. Anticancer
treatments are given to slow the progress of the disease. Supportive care helps
manage pain, other symptoms, or side effects (such as nausea). It does not aim
to extend a woman's life. Supportive care can help a woman feel better
physically and emotionally. Some women with advanced cancer decide to have only
supportive care.
Recurrent Breast Cancer
Recurrent cancer is cancer that has come back after it could not be detected.
Treatment for the recurrent disease depends mainly on the location and extent
of the cancer. Another main factor is the type of treatment the woman had
before.
If breast cancer comes back only in the breast after breast-sparing surgery,
the woman may have a mastectomy. Chances are good that the disease will not
come back again.
If breast cancer recurs in other parts of the body, treatment may involve
chemotherapy, hormone therapy, or biological therapy. Radiation therapy may
help control cancer that recurs in the chest muscles or in certain other areas
of the body.
Treatment can seldom cure cancer that recurs outside the breast. Supportive
care is often an important part of the treatment plan. Many patients have
supportive care to ease their symptoms and anticancer treatments to slow the
progress of the disease. Some receive only supportive care to improve their
quality of life.
Back to Top
< Previous Section | Next Section > |