|
Tracking a Mystery Disease:
The Detailed Story of Hantavirus Pulmonary Syndrome
The "First" Outbreak
In May 1993, an outbreak of an unexplained pulmonary illness occurred
in the southwestern United States, in an area shared by Arizona,
New Mexico, Colorado and Utah known as "The Four Corners."
A young, physically fit Navajo man suffering from shortness
of breath was rushed to a hospital in New Mexico and died very rapidly.

While reviewing the results of the case, medical personnel discovered that the young
man's fiancee had died a few days before after showing similar symptoms, a piece of
information that proved key to discovering the disease. As Dr. James Cheek of the Indian
Health Service (IHS) noted, "I think if it hadn't been for that initial pair of
people that became sick within a week of each other, we never would have discovered the
illness at all."
An investigation combing the entire Four Corners region was launched by the New Mexico
Office of Medical Investigations (OMI) to find any other people who had a similar case
history. Within a few hours, Dr. Bruce Tempest of IHS, working with OMI, had located five
young, healthy people who had all died after acute respiratory failure.
A series of laboratory tests had failed to identify any of the deaths as caused by a
known disease, such as bubonic plague. At this point, the CDC Special Pathogens Branch was
notified. CDC, the state health departments of New Mexico, Colorado and Utah, the Indian
Health Service, the Navajo Nation, and the University of New Mexico all joined together to
confront the outbreak.
 During the next few weeks, as additional
cases of the disease were reported in the Four Corners area, physicians and other
scientific experts worked intensively to narrow down the list of possible causes. The
particular mixture of symptoms and clinical findings pointed researchers away from
possible causes, such as exposure to a herbicide or a new type of influenza, and toward
some type of virus. Samples of tissue from patients who had gotten the disease were sent
to CDC for exhaustive analysis. Virologists at CDC used several tests, including new
methods to pinpoint virus genes at the molecular level, and were able to link the
pulmonary syndrome with a virus, in particular a previously unknown type of hantavirus. During the next few weeks, as additional
cases of the disease were reported in the Four Corners area, physicians and other
scientific experts worked intensively to narrow down the list of possible causes. The
particular mixture of symptoms and clinical findings pointed researchers away from
possible causes, such as exposure to a herbicide or a new type of influenza, and toward
some type of virus. Samples of tissue from patients who had gotten the disease were sent
to CDC for exhaustive analysis. Virologists at CDC used several tests, including new
methods to pinpoint virus genes at the molecular level, and were able to link the
pulmonary syndrome with a virus, in particular a previously unknown type of hantavirus.
Photo, above: Emergency service personnel transport patient
with HPS to hospital during outbreak in 1993.
Researchers Launch Investigations
to Pin Down the Carrier of the New Virus
Researchers knew that all other known hantaviruses were transmitted to people by
rodents, such as mice and rats. Therefore, an important part of their mission was to trap
as many different species of rodents living in the Four Corners region as possible to find
the particular type of rodent that carried the virus. From June through mid-August of
1993, all types of rodents were trapped inside and outside homes where people who had
hantavirus pulmonary syndrome had lived, as well as in piñon groves and summer sheep
camps where they had worked.  Additional rodents were trapped for comparison in and around nearby
households as well. Taking a calculated risk, researchers decided not to wear protective
clothing or masks during the trapping process. "We didn't want to go in wearing
respirators, scaring...everybody," John Sarisky, an Indian Health Service
environmental disease specialist said. However, when the almost 1,700 rodents trapped were
dissected to prepare samples for analysis at CDC, protective clothing and respirators were
worn. Additional rodents were trapped for comparison in and around nearby
households as well. Taking a calculated risk, researchers decided not to wear protective
clothing or masks during the trapping process. "We didn't want to go in wearing
respirators, scaring...everybody," John Sarisky, an Indian Health Service
environmental disease specialist said. However, when the almost 1,700 rodents trapped were
dissected to prepare samples for analysis at CDC, protective clothing and respirators were
worn.
Photo, right: Protective gear, such as gloves,
gown, and respirator, were worn during activities that required dissection
of rodents.
Among rodents trapped, the deer mouse (Peromyscus maniculatus) was
found to be the main host to a previously unknown type of hantavirus.
Since the deer mouse often lives near people in rural and semi-rural areas—in
barns and outbuildings, woodpiles, and inside people's homes—researchers
suspected that the deer mouse might be transmitting the virus to humans.
About 30% of the deer mice tested showed evidence of infection with hantavirus.
Tests also showed that several other types of rodents were infected, although
in lesser numbers.
The next step was to pin down the connection between the infected deer mice and
households where people who had gotten the disease lived. Therefore, investigators
launched a case-control investigation. They compared "case" households, where
people who had gotten the disease lived, with nearby "control" households.
Control households were similar to those where the case-patients lived, except for one
factor: no one in the control households had gotten the disease.
The results? First, investigators trapped more rodents in case households than in
control households, so more rodents may have been living in close contact with people in
case households. Second, people in case households were more likely than those in control
households to do cleaning around the house or to plant in or hand-plow soil outdoors in
fields or gardens. However, it was unclear if the risk for contracting HPS was due to
performing these tasks, or with entering closed-up rooms or closets to get tools needed
for these tasks.
In November 1993, the specific hantavirus that caused the Four Corners outbreak was
isolated. The Special Pathogens Branch at CDC used tissue from a deer mouse that had been
trapped near the New Mexico home of a person who had gotten the disease and grew the virus
from it in the laboratory. Shortly afterwards and independently, the U.S. Army Medical
Research Institute of Infectious Diseases (USAMRIID) also grew the virus, from a person in
New Mexico who had gotten the disease as well as from a mouse trapped in California.
The new virus was called Muerto Canyon virus—later changed to Sin Nombre virus
(SNV)—and the new disease caused by the virus was named hantavirus pulmonary
syndrome, or HPS.
The isolation of the virus in a matter of months was remarkable. This success was
based on close cooperation of all the agencies and individuals involved in investigating
the outbreak, years of basic research on other hantaviruses that had been conducted at CDC
and USAMRIID, and on the continuing development of modern molecular virologic tests. To
put the rapid isolation of the Sin Nombre virus in perspective, it took several decades
for the first hantavirus discovered, the Hantaan virus, to be isolated.
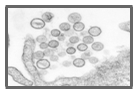
 Thin-section
electron micrograph of Sin Nombre virus isolate, a causative agent of
hantavirus pulmonary syndrome (HPS). From the 1993 outbreak of HPS
in the southwestern United States. Electron micrograph. Thin-section
electron micrograph of Sin Nombre virus isolate, a causative agent of
hantavirus pulmonary syndrome (HPS). From the 1993 outbreak of HPS
in the southwestern United States. Electron micrograph.
HPS Not Really a New Disease
As part of the effort to locate the source of the virus, researchers located and
examined stored samples of lung tissue from people who had died of unexplained lung
disease. Some of these samples showed evidence of previous infection with Sin Nombre
virus—indicating that the disease had existed before the "first" known
outbreak—it simply had not been recognized!
Other early cases of HPS have been discovered by examining samples of tissue belonging
to people who had died of unexplained adult respiratory distress syndrome. By this method,
the earliest known case of HPS that has been confirmed has been the case of a 38-year-old
Utah man in 1959.
Interestingly, while HPS was not known to the epidemiologic and medical
communities, there is evidence that it was recognized elsewhere. The Navajo
Indians, a number of whom contracted HPS during the 1993 outbreak, recognize
a similar disease in their medical traditions, and actually associate
its occurrence with mice. As strikingly, Navajo medical beliefs concur with public health recommendations
for preventing the disease.
Why Did the Outbreak Occur in the Four Corners
Area?
But why this sudden cluster of cases? The key answer to this question is
that, during this period, there were suddenly many more mice than usual.
The Four Corners area had been in a drought for several years. Then, in
early 1993, heavy snows and rainfall helped drought-stricken plants and
animals to revive and grow in larger-than-usual numbers. The area's deer
mice had plenty to eat, and as a result they reproduced so rapidly that
there were ten times more mice in May 1993 than there had been in May
of 1992. With so many mice, it was more likely that mice and humans would
come into contact with one another, and thus more likely that the hantavirus
carried by the mice would be transmitted to humans.
Person-to-Person Spread of HPS Decided Unlikely
"Although person-to-person spread [of HPS] has not been documented with any of the
other known hantaviruses, we were concerned [during this outbreak] because we were dealing
with a new agent," said Charles Vitek, a CDC medical investigator.
Researchers and clinicians investigating the ongoing outbreak were not the only groups
concerned about the disease. Shortly after the first few HPS patients died and it became
clear that a new disease was affecting people in the area, and that no one knew how it was
transmitted, the news media began extensive reporting on the outbreak. Widespread concern
among the public ensued.
Unfortunately, the first victims of the outbreak were Navajo. News reports focused on
this fact, and the misperception grew that the unknown disease was somehow linked to
Navajos. As a consequence, Navajos found themselves at the center of intense media
attention and the objects of the some people's fears.
By later in the summer of 1993, the media frenzy had quieted somewhat,
and the source of the disease was pinpointed. Researchers determined
that, like other hantaviruses, the virus that causes HPS is not
transmitted from person to person the way other infections, such
as the common cold, may be. The exception to this is an outbreak
of HPS in Argentina in 1996. Evidence from this outbreak suggests
that strains of hantaviruses in South America may be transmissable
from person to person.
To date, no cases of HPS have been reported in the United States in which
the virus was transmitted from one person to another. In fact, in a study
of health care workers who were exposed to either patients or specimens
infected with related types of hantaviruses (which cause a different disease
in humans), none of the workers showed evidence of infection or illness.
HPS Since the First Outbreak
After the initial outbreak, the medical community nationwide was asked to report any
cases of illness with symptoms similar to those of HPS that could not be explained by any
other cause. As a result, additional cases have been reported.
Since 1993, researchers have discovered that there is not just one hantavirus that
causes HPS, but several. In June 1993, a Louisiana bridge inspector who had not traveled
to the Four Corners area developed HPS. An investigation was begun. The patient's tissues
were tested for the presence of antibodies to hantavirus. The results led to the
discovery of another hantavirus, named Bayou virus, which was linked to a carrier, the
rice rat (Oryzomys palustris). In late 1993, a 33-year-old Florida man came down
with HPS symptoms; he later recovered. This person also had not traveled to the Four
Corners area. A similar investigation revealed yet another hantavirus, named the Black
Creek Canal virus, and its carrier, the cotton rat (Sigmodon hispidus). Another
case occurred in New York. This time, the Sin Nombre-like virus was named New York-1, and
the white-footed mouse, Peromyscus leucopus, was implicated as the carrier.
More recently, cases of HPS stemming from related hantaviruses have been
documented in Argentina, Brazil, Canada, Chile, Paraguay, and Uruguay,
making HPS a pan-hemispheric disease
References
Information for this page was developed using the CDC video Preventing Hantavirus
Disease and resource articles listed in the bibliography.
|

 National
Center for Infectious Diseases
National
Center for Infectious Diseases National
Center for Infectious Diseases
National
Center for Infectious Diseases