

|
Search | Index | Home | Glossary | Contact Us |
|
| |
|
|
|
Barry L. Johnson, PhD
Assistant Administrator
Maureen Y. Lichtveld, MD, MPH
Director, Division of Health Education
Managing Editor
Teresa Ramsey
Assistant Editor
Susan Coatsworth
Staff Writers
Susan Coatsworth and Teresa Ramsey
Layout and Graphics
Susan Coatsworth and Sara Cote
 ATSDR Home Page
ATSDR Home Page
Children depend completely on adults for access to medical care.
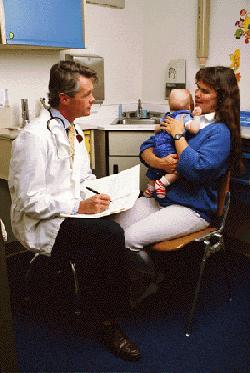
Children are our future, and in America, one in four live within 4 miles of a hazardous waste site according to EPA's data. Children who live near hazardous waste are at greater risk of being exposed to hazardous substances emitted from waste sites and emergency events that could adversely affect their health. Those of us in the field of environmental health consider this to be a public health concern that must be addressed and given high priority.
Children are not small adults; they are more likely to be exposed because they play vigorously outdoors (splashing, digging, and exploring), and they often bring food into contaminated areas and put contaminated hands into their mouths. They are shorter than adults, which means they breathe dust, soil, and heavy vapors close to the ground; they weigh less than adults, which means they get higher doses in proportion to their body weight. Their developing body systems can sustain permanent damage if toxic exposures occur during critical growth stages. Most importantly, children depend completely on adults for decisions about risk management and housing (see related story in this issue, Protecting Children from Lead Exposure), and access to medical care.
The Agency for Toxic Substances and Disease Registry (ATSDR) advocates a comprehensive approach to promoting the environmental health of children. ATSDR's findings, which include more than 10 years of public health assessments, toxicologic investigations, epidemiologic studies, and reviews by expert workgroups, demonstrate that children who live near hazardous waste sites are particularly vulnerable to toxic exposures.
ATSDR's data indicate that increased speech and hearing impairments were reported for children exposed to trichloroethylene in drinking water supplies at 15 sites in Arizona, Illinois, Indiana, Michigan, and Pennsylvania. In communities adjacent to sites throughout the United States, elevated blood lead levels were found in some children who played near the sites, washed hands infrequently, and had other behavioral risk factors. Children were recently found to have reduced lung function as a consequence of breathing materials emitted by smelters.
ATSDR has launched a Child Health Initiative to emphasize policies and projects that promote the health of infants, children, and youth. ATSDR's vision in this initiative is Healthy Children in a Healthy Environment. This initiative is intended to (1) emphasize child health in all of ATSDR's programs and activities, (2) identify new projects that benefit children, and (3) solicit input from and disseminate information to other agencies and organizations. ATSDR's initiative will complement EPA's National Agenda to Protect Children from Environmental Threats (see related story, Infants and Children Now Count, Hazardous Substances & Public Health, volume 6, number 1, winter/spring 1996). ATSDR is mobilizing outside interest in the broad fields of public health and environmental health and seeks to focus attention on human populations and their most vulnerable constituents, especially children. There is an equally compelling need to educate children and their parents, as well as child health providers and child health advocates, to prevent exposure to hazardous substances. The Child Health Initiative is an expression of ATSDR's overall mission and the role of public health in preventing human health risks from hazardous waste sites.
ATSDR is seeking new partnerships to form a closer association between the child health specialties and the environmental professions. For example, the agency seeks to help child health advocates learn environmental science and environmental scientists learn child health. We invite our partner organizations and other interested groups to submit technical reports, case studies, and other experiences, and to suggest additional areas of emphasis.
Environmental health education and disease prevention efforts go hand-in-hand. We hope that you will find the information from this issue's special topic, Children's Health and the Environment, educational and that you will share it with others. We will continue to feature a Children and the Environment article in future issues of our newsletter. Please share with us news of your own efforts in protecting our future, the children, from environmental hazards.
Health officials are evaluating the occurrence of a higher than average incidence of childhood brain cancer in Dover Township, Ocean County, New Jersey. The overall rate of childhood brain and central nervous system cancer in the Toms River section of the township is three times higher than expected. The Agency for Toxic Substances and Disease Registry (ATSDR) is a partner in the investigation.
Data for the period 1979 to 1991 show that 230 Ocean County children were diagnosed with cancer—7% higher than expected. The county had 54 reported cases of brain or central nervous system (CNS) cancers; 39 such cases would have been normal. In Toms River, for children under five, the rate of brain or CNS cancer was statistically elevated compared to state rates (3 cases observed compared to 0.4 cases expected.) Community groups believe that rates may be higher than the available data indicate and have urged officials to update the numbers.
Local, state, and federal health officials worked with community representatives to develop a public health response plan that details how the problem will be investigated. Data on childhood cancer incidence are being updated and analyzed to generate hypotheses about what may have caused the cancers. Childhood cancer clusters are rare. "We don't often get called to investigate [them]," said Jerry Fagliano of the New Jersey Department of Health.
To determine if human exposure to carcinogenic contaminants took place, two Ocean County Superfund sites are being reviewed: Ciba-Geigy, a dye manufacturing plant, and the Reich Farm chemical waste dump. Both are being cleaned up and groundwater decontamination is taking place, but it is known that some local wells have been contaminated. Extensive water quality testing has been conducted on the town's water supply. Investigators are also reviewing toxicological data on contaminants of concern.
The Ocean County Board of Health has appointed a 19-member Ad Hoc Cancer Committee to inform and educate parents, families, and health professionals and to support and advise members of the Citizens Action Committee on Childhood Cancer Cluster (CACCCC) on topics related to childhood cancer in Ocean County. The CACCCC is composed of health professionals and community members, including some parents of children with cancer, and "because of that, they are very good partners," said Elin Gursky, senior assistant commissioner of the New Jersey Department of Health and Senior Services.
ATSDR is conducting a multi-state study comparing brain cancer rates with proximity to hazardous waste sites. New Jersey has been added to the study, which ATSDR anticipates completing in 1997.
Richard Soule, Daniel Symonik, Doug Turgeon
Minnesota Department of Health
121 E. 7th Place
St. Paul, MN 55101
Minnesota investigators report that current guidelines for water testing could result in underestimating the concentration of vinyl chloride. The U.S. Environmental Protection Agency (EPA) recommends that water samples be analyzed for vinyl chloride within 14 days of collection. However, anecdotal reports suggest that water samples analyzed immediately after collection have consistently higher vinyl chloride levels than similar samples held for longer periods. A study conducted by the Minnesota Department of Health (MDH) confirmed the reports.
Vinyl chloride, a common groundwater contaminant near hazardous waste sites, is a potent human carcinogen. According to ATSDR's HazDat database (site data collected since 1980), vinyl chloride is found in groundwater at approximately 20% of the sites found on the National Priorities List. Fifty-three percent of the U.S. population relies on groundwater as a source of drinking water, says the EPA.
Analytical tests for vinyl chloride are an important part of the effort to protect people from exposure to this compound in drinking water. The reported detection limits for analytical tests are typically just sensitive enough to detect the maximum level of vinyl chloride allowed under current Minnesota drinking water guidelines. That leaves little room for error and makes it especially important to determine with confidence whether analytical results accurately reflect actual levels of vinyl chloride.
The study raises the possibility that the practice of holding water samples for even a small portion of the 14-day interval could result in an underestimate of the concentration of vinyl chloride in the water and the health risk to people who consume the water.
The MDH Study: Methodology and Findings
To determine if a significant amount of vinyl chloride is lost from samples that have been held for a 14-day period, MDH tested two types of water samples: laboratory-prepared samples containing a known concentration of vinyl chloride (lab samples) and groundwater samples collected from a single water well contaminated with vinyl chloride (field samples). The concentration in the lab samples was similar to concentrations that had recently been measured in the well (1.5 micrograms per liter [µg/L]).
The relationship between the loss of vinyl chloride and holding time, for both the lab and field samples, is shown in Figure 1. Approximately 40% of the vinyl chloride initially present was lost during the 14-day holding period, with roughly half of the loss (representing 25% of the initial concentration) occurring during the first 2 days. The observed decrease was statistically significant (p<.05). These findings point out the importance of analyzing water samples immediately whenever low levels of vinyl chloride may be present - i.e., when concentrations are in the parts-per-billion range, close to current health-based standards.
In addition to the losses associated with holding time, MDH investigators also observed (1) an initial loss of about 0.22 µg/L (15% of the initial concentration) for both the lab and field samples during the process of drawing and packaging the samples and (2) a loss of up to 0.15 µg/L (10% of the initial concentration) through subsequent handling of the samples. These findings suggest it is important to minimize exposure of the samples to air.
Public Health Implications
Because vinyl chloride is a known and relatively potent human carcinogen when orally ingested, health-based standards for vinyl chloride are set low. The EPA's maximum contaminant level for vinyl chloride - the exposure limit value for public water supply systems - is 2 µg/L. That number is based on analytical detection limits for vinyl chloride in water in 1987, when the standard was set.
MDH uses a health-based standard of 0.2 µg/L for private drinking water supplies. This standard is roughly equivalent to reported minimum detection limits for vinyl chloride in water. The precision of analytical testing methods is reduced as the concentration being measured approaches the detection limit. For that reason, accuracy of measurement decreases at low concentrations.
Vinyl chloride most commonly enters groundwater at hazardous waste sites as a result of breakdown of trichloroethene, tetrachloroethene, or 1,1,1-trichloroethane. It may be present even if it wasn't originally used or disposed of at the site and could therefore be overlooked as a potential contaminant of concern. Vinyl chloride could also go undetected - and the potential health risks associated with a site could be underestimated - if the analytical techniques used for this compound have an effective detection limit higher than the standard.
The MDH study warns that because significant public health actions - including restrictions on water consumption or the installation of expensive treatment systems - may need to be taken on the basis of limited analytical testing results, it is crucial to obtain the most accurate results possible.
The Minnesota investigators recommended that more than one sample be collected from each well being tested for vinyl chloride if low levels are anticipated. Exposure of the sample to the air should be minimized, and sufficiently sensitive analytical techniques should be used. Analyses should be done as soon as possible. Risk managers and risk assessors should be aware of the uncertainties involved in taking and testing samples of water that may be contaminated with vinyl chloride so they can make informed decisions about possible public health actions.
The MDH study was sponsored by the Agency for Toxic Substances and Disease Registry through a cooperative agreement. A more complete presentation and discussion of this data may be found in Regulatory Toxicology and Pharmacology, volume 23 (3), pp. 209-212. For further information, contact Dan Symonik, research scientist, at (612) 215-0920.
 Homesellers of homes built before 1978 are required
to provide information about lead poisoning caused by exposure to lead-based paint.
Homesellers of homes built before 1978 are required
to provide information about lead poisoning caused by exposure to lead-based paint.
Families now have the right to know about lead-based paint in homes they are buying or renting before a sale is closed or a rental agreement is signed. Real estate agents and property owners with more than four residential dwellings (including single family homes) are required to provide buyers and new tenants with a pamphlet containing information necessary to protect families, especially children, from lead poisoning caused by exposure to lead-based paint.
Lead poisoning is the foremost preventable disease of children in all socioeconomic and demographic strata. However, in many urban communities, more than 50% of young children are lead-poisoned, and many are never diagnosed. For infants and young children, lead exposure has been shown to decrease intelligence (IQ) scores, slow growth, and cause hearing problems. These effects can last as children get older and interfere with successful performance in school. Children are often exposed to lead when their hands come into contact with lead-based paint chips or leaded dust on windowsills and furniture and then their contaminated hands enter their mouths.
The requirements took effect on September 6, 1996, and mark the first phase in a new federal lead prevention program, created by the U. S. Environmental Protection Agency (EPA) and the U.S. Department of Housing and Urban Development, to ensure that families receive basic lead hazard exposure prevention information before purchasing or renting older housing. The new requirement applies to residences built before 1978, the year the sale of residential lead-based paint was banned.
The program requires real estate agents and property owners to disclose to purchasers and new tenants all known lead-based paint and lead-based paint hazards in a residence and provide them with the pamphlet "Protect Your Family from Lead in Your Home." The pamphlet outlines practical, low-cost tips on identifying and controlling lead-paint hazards. Property owners must also provide the same information to tenants renewing their leases after September 6, 1996. Specific notification and disclosure language must be included in the contract or lease, along with signed statements from all parties verifying the requirements have been met. Homebuyers will have a 10-day opportunity to conduct a lead-based paint inspection or risk assessment at their own expense before a contract is finalized. The second phase of the program takes effect on December 6, 1996, when property owners with four or fewer dwellings must comply.
For a copy of the pamphlet, sample disclosure forms, or the regulation, call
the National Lead Information Clearinghouse at (800) 424-LEAD. The EPA pamphlet
and regulation are also available on the Internet at http://www.epa.gov.![]()
In his charge to the workgroup, ATSDR Assistant Administrator Barry L. Johnson, PhD, linked the Child Health Initiative to prior agency accomplishments. For example, ATSDR's 1988 report to Congress described the extent of childhood lead poisoning; since then, ATSDR has worked with EPA and state health departments to study lead exposure and adverse health outcomes in young children living near hazardous waste sites. ATSDR has also supported studies of toxic substances in the breast milk of nursing mothers, reproductive disorders such as birth defects and low birth weight, and neurobehavioral disorders in children and others exposed to mercury or other neurotoxicants. The workgroup will help ATSDR determine how existing knowledge should be used to impove the health of children, identify the key information gaps, and find the best opportunities for coordination with other agencies and nongovernment organizations to protect the health of children.
"The workgroup should also consider primary prevention issues, such as promotion of healthy environments," said workgroup member Joy E. Carlson, MPH, director of the Children's Environmental Health Network, Emeryville, California. "ATSDR's Child Health Initiative can help mobilize outside interest in the broad field of children's environmental health." The workgroup's initial findings will be presented to the BSC at its November 1996 meeting in Atlanta.
For more information about ATSDR's Child Health Initiative, please contact Robert W. Amler, MD, Chief Medical Officer, at 1600 Clifton Road, Mailstop E28, Atlanta, Georgia 30333; telephone (404) 498-0004.
Needleman HL, Landrigan PJ. Raising children toxic free: how to keep your child safe from lead, asbestos, pesticides, and other environmental hazards. New York: Avon Books, 1994 (259 pp. $12 US and $16 Canada; soft cover).
Parents who are concerned about the many environmental chemical hazards that confront their children now have a reference guide, written in plain English, that explains the nature of the hazards and provides useful tips for reducing children's risks. The book is authored by two former members of the American Academy of Pediatrics committee on environmental hazards: Herbert L. Needleman, MD, professor of psychiatry and pediatrics, University of Pittsburgh School of Medicine; and Philip J. Landrigan, MD, professor and chair of the department of community and occupational medicine, Mt. Sinai School of Medicine, New York. Both authors are internationally recognized experts on pediatrics and environmental health and have served as consultants for numerous environmental health studies and projects conducted by the Agency for Toxic Substances and Disease Registry (ATSDR).
In his foreword, T. Berry Brazelton, MD, renowned pediatrician and authority on parenting and infant development, notes that the book "gives parents the tools and the information they need to evaluate environmental threats, so that they can make informed decisions about how to deal with them in a rational manner." The book is indexed and contains several useful appendices, including an annotated listing of major environmental organizations in the United States and a household toxicant inventory that readers can self-administer. The inventory was developed for the Children's Environmental Health Network by Sophie J. Balk, MD, assistant professor of pediatrics, Albert Einstein College of Medicine, with partial funding from ATSDR.
Environmental health scientists at ATSDR conduct health studies at various Superfund sites nationwide to evaluate the health effects of hazardous substances on exposed populations. The following health studies are available to the public through the National Technical Information Service (NTIS):
To order these health studies and others prepared by ATSDR, contact NTIS, Sills Building, 5285 Port Royal Road, Springfield, Virginia 22151; telephone (703) 487-4650; fax (703) 321-8547. For more information on health studies activities, contact Sharon Campolucci, deputy director, Division of Health Studies, ATSDR, 1600 Clifton Road, NE, Mailstop E31, Atlanta, Georgia 30333; telephone (404) 639-6200.
The National Institute of Environmental
Health Sciences (NIEHS)![]() has established a new information service for people who want to know how environmental
issues might be affecting them personally. If you want to know about the impact
of radon, global warming, ozone, oxygenated fuels, household or agricultural pesticides,
lawn products, or other environmental factors and how they may affect you and
your family, you can reach a real person who can answer your questions and provide
further information by calling the EnviroHealth hotline at (800) NIEHS-94 from
9 am to 8 pm Eastern Time weekdays or recording your questions during off-hours.
You can reach the services via e-mail at envirohealth@niehs.nih.gov,
has established a new information service for people who want to know how environmental
issues might be affecting them personally. If you want to know about the impact
of radon, global warming, ozone, oxygenated fuels, household or agricultural pesticides,
lawn products, or other environmental factors and how they may affect you and
your family, you can reach a real person who can answer your questions and provide
further information by calling the EnviroHealth hotline at (800) NIEHS-94 from
9 am to 8 pm Eastern Time weekdays or recording your questions during off-hours.
You can reach the services via e-mail at envirohealth@niehs.nih.gov,![]() or fax your questions to (919) 361-9408. EnviroHealth is managed by a board-certified
toxicologist.
or fax your questions to (919) 361-9408. EnviroHealth is managed by a board-certified
toxicologist.
Respiratory Protection Program, November 18-20, 1996, Birmingham, Alabama. This 3-day course is designed for safety professionals, industrial hygienists, occupational health nurses, chemists, laboratory supervisors, and other staff who may have to monitor worker exposure. Participants will learn how to operate direct reading air sampling devices. Tuition $510.
Sampling and Evaluating Airborne Asbestos Dust-NIOSH 582, November 18-22, 1996, Birmingham, Alabama. This 5-day course teaches asbestos air sampling using Phase Contrast Microscopy according to NIOSH method 7400, Revision 3, issue 2. Tuition $750.
For more information about these and other available courses, contact Cherie Hunt, The Deep South Center for Occupational Health and Safety, University of Alabama, School of Public Health, Birmingham, Alabama 35294-2010; telephone (205) 934-7178.
Comprehensive Industrial Hygiene Review, March 10-14, 1997, Boston, Massachusetts. This course provides a comprehensive review of the industrial hygiene field for individuals preparing to take the American Board of Industrial Hygiene core and comprehensive examinations. Curriculum topics include toxicology, radiation, heat stress, personal protective equipment, ergonomics, biosafety, noise, ventilation, management, hazardous waste operations, air sampling, indoor air quality, and chemistry. Test-taking techniques and practice tests are included as are lectures and extensive problem sets on each topic and a computer lab for individual study. Tuition $995.
Analyzing Risk: Science, Assessment and Management, March 18-21, 1997, Boston, Massachusetts. This course is designed for industrial, regulatory, and public health professionals challenged to evaluate the risks associated with environmental and occupational hazards. The class covers the scientific underpinnings of risk assessment in toxicology and epidemiology, the scientific methods of computing risk estimates, the new mechanistic and distributional approaches, and the role of assessments in managing risks and communicating with decision makers and the public. Participants will learn skills in risk assessment, risk management, and risk communication by examining complex problems involving chemicals and radiation. Tuition $1,045.
For more information, contact Harvard School of Public Health, 677 Huntington Avenue LL-23, Boston, Massachusetts 02115-6023; telephone (617) 432-1171; fax (617) 423-1969.
Toxicology for Non-Toxicologists, January 16, 1997, Seattle, Washington. This course is for community members interested in learning more about chemical agents in their homes, workplaces, and environment, and health professionals who advise workers or community members about exposures to potentially hazardous substances. Topics include the basic principles of toxicology and risk assessment.
Advances in Occupational and Environmental Medicine, March 21, 1997, Seattle, Washington. This annual conference is for occupational health and primary care physicians, internists, epidemiologists, and occupational health nurses, and will discuss the current issues in occupational and environmental medicine.
For more information contact the Northwest Center for Occupational Health and Safety, Department of Environmental Health, School of Public and Community Medicine, University of Washington, 4225 Roosevelt Way, NE, Room 100, Seattle, Washington 98105-6099; telephone (206) 543-1069; e-mail: ce@u.washington.edu.
November 15-17, 1996; The 47th Annual Meeting of the Society for Public Health Education, New York, New York. Contact: Elaine Auld, 1015 Fifteenth Street, NW, Suite 410, Washington, DC 20005; telephone (202) 408-9804; fax (202) 408-9815.
November 17-21, 1996; American Public Health Association 124th Annual Conference, New York, New York. Contact: APHA, 1015 15th Street, NW, Washington, DC 20005; telephone (202) 789-5670; fax (202) 274-4577.
January 13-14, 1997; International Society of Regulatory Toxicology and Pharmacology, Assessing the Risks of Adverse Endocrine-Mediated Effects, Research Triangle Park, North Carolina. Contact: Dr. C. Jelleff Carr, 6546 Belleview Drive, Columbia, Maryland 21046-1054; telephone (410) 992-9083; fax (410) 740-9181.
February 19-22, 1997; Learning Disabilities Association Annual Conference, Chicago, Illinois. Contact: LDA, 4156 Library Road, Pittsburgh, Pennsylvania 15234-1349; telephone (412) 341-1515; fax (412) 344-0224.
February 21-23, 1997; First National Research Conference on Children's Environmental Health,Washington, DC. Contact: Carol Harris, Children's Environmental Health Network, 5900 Hollis Street, Suite E, Emeryville, CA 94608; telephone (510) 450-3818; fax (510) 450-3773.
February 22-24, 1997; American Organization of Nurse Executives Annual Conference, Phoenix, Arizona. Contact: AONE Exhibit Office, Beacon-Hedland Management, Inc., 475 Frontage Road, Suite 101, Burr Ridge, Illinois 60521; telephone (630) 323-7028; fax (630) 323-6989.
Send comments or questions to atsdr-hsph@cdc.gov.
This page last updated on
September 2, 2003
Contact Name: Wilma López/ WLópez@cdc.gov
ATSDR Home | Search | Index | Glossary | Contact Us
About ATSDR | News Archive | ToxFAQs | Public Health Assessments
Privacy Policy |
External Links Disclaimer
| Accessibility
U.S.
Department of Health and Human Services