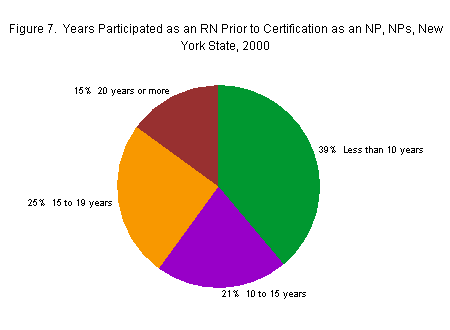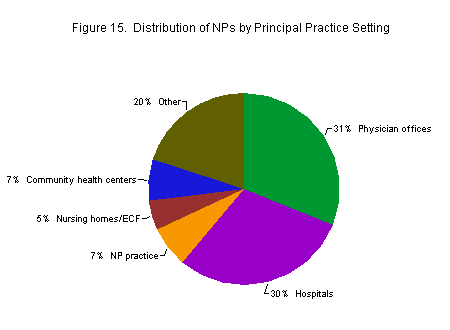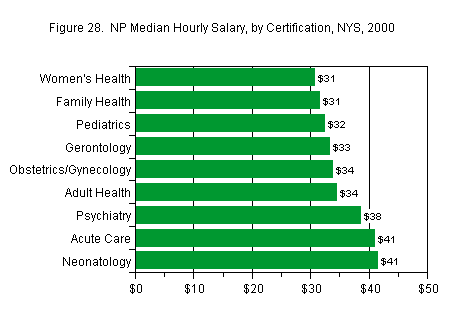|
|||||||
 |
|||||||
|
|
||
National Center for Health Workforce Analysis
Nurse Practitioners
in New York State
A Profile of the Profession
in 2000
November 2004
Prepared for the Department of Health and Human Services, Health Resources and Services Administration, Bureau of Health Professions, National Center for Health Workforce Analysis: Purchase Order No. 01-0532(P)
Table of Contents (for on-line viewing only) Printer-friendly Adobe/pdf
Executive
Summary
Background information
Current NP practice
Scope of practice and reimbursement/provider status
Impression of the job market for NPs
Introduction
Overview of Survey
Summary of Survey Responses
Description of NPs
I. Background
Information
Employment Status
Gender and Race/Ethnicity
Age and Graduation Cohort
Race by age
III.
Current NP Practice
Professional Activities
Specialty Certification
Specialty by race
Specialty distribution by age
Practice Settings
Practice setting by age
Practice setting by specialty
Scope of practice and reimbursement/provider status
Scope of practice by specialty
Income
Income by Age/Graduation Cohort
Income by race
Income by specialty
Location of practice
Location of practice by race
Geographical distribution by age
IV. Impression
of job market for NPs
Job Market Experiences by Age
Job opportunities by specialty
NPs in independent practice
Appendix A: The Survey Instruments
In the fall of 2000, a survey of licensed Nurse Practitioners (NPs) in New York State was conducted under contract from HRSA with the Center for Health Workforce Studies at the University at Albany, State University of New York. The study was intended to produce a snapshot of New York State NPs, with particular emphasis on their educational background, practice patterns, and perceptions of the job market.
This report contains a profile of these characteristics for all NPs, as well as an analysis of variation by age, graduation cohort, specialty certification, and race/ethnicity. A brief examination of the NPs who reported independent solo or group practice is also presented.
Major findings for the profession as a whole are as follows:
- Most NPs (76 percent) worked exclusively as NPs, although 20 percent reported practicing as both an NP and an RN.
- NPs were overwhelmingly female (94.5 percent).
- The majority of NPs were non-Hispanic whites, although racial/ethnic diversity has increased in recent cohorts. Almost all NPs were U.S. citizens, with a small number (1.5 percent) reporting themselves to be permanent non-citizen residents.
- NPs were substantially older than the civilian labor force as a whole, with a median age of 45 versus 39 for the civilian labor force. Their age was comparable to that of registered nurses in New York State in 2000, who had a median age of 44 (BLS, 2000).
Education
- The education production of NPs in New York State has increased dramatically in recent years, with almost 52 percent of NPs graduating from their NP program between 1995 and 1999. Only 22 percent of NPs graduated during the previous five-year period (1990 to 1994), and only 10 percent of NPs graduated during the period of 1985 – 1989.
- Over 90 percent of NPs hold a master’s degree, either alone or in conjunction with an advanced certificate. Seventy-six percent report that they are credentialed by at least one national credentialing association.
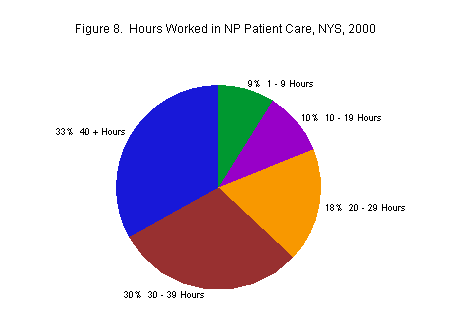
- One-third of NPs work at least 40 hours a week as a NP, although almost 10 percent work fewer than 10 hours a week as an NP.
- The majority of NPs (57 percent) work only in patient care, with the remainder of the NPs reporting at least some hours of administration, teaching, or research. The number of hours in these activities is typically very small, however, with patient care constituting the major activity for the vast majority of NPs.
- NPs were most likely to have a certification in family health (33 percent), adult health (31 percent), pediatrics (14 percent), or psychiatry (6 percent). Very small numbers of NPs specialized in community health, perinatology, oncology, or school health.
- Most NPs (70 percent) work at only one practice site, another 23 percent worked at two practice sites, and 8 percent reported working at three or more sites.
- The type of care provided by NPs at their principal practice site is about equally likely to be primary care versus specialty care.
- The most common principal practice settings for NPs are: physician offices at 31 percent (22 percent group and 9 percent solo practice); hospitals at 30 percent (15 percent ambulatory care, 11 percent inpatient care, 2.4 percent emergency rooms, and 1.8 percent psychiatric hospitals); and NP practice at 7 percent (5 percent group and 2 percent solo practices).
- Slightly more than one-third of NPs work with a collaborating physician whose specialty is family practice (13 percent), general internal medicine (11 percent), or general pediatrics (11 percent). An additional 12 percent work with obstetricians/gynecologists. The specialty certifications of NPs tend to match the specialty of the collaborating physician at their principal practice setting.
- Few NPs report plans to retire, reduce patient care hours, or change the location of their practice in the next 12 months.
- The largest number of NPs (32 percent) work in suburban areas, but almost as many (31 percent) practice in an inner-city area, while another 15 percent practice in a rural area or small town. Sixty-seven percent of rural NPs provide primary care.
Scope of practice and reimbursement/provider status
- Over two-thirds of NPs are Drug Enforcement Agency (DEA) certified to prescribe controlled substances. Only one-quarter have their own Medicaid provider number and only about one-third have a Medicare provider number.
- Ninety percent or more of NPs perform histories and physical exams, order laboratory tests, or make direct referrals to specialists, although less than a third provide on-call services and very few (less than 5 percent) assist in surgeries.
- Almost half of NPs collaborate daily with their designated collaborating physician, and almost one-third report weekly collaboration. Ten percent report collaborating monthly, while 12 percent only do so as required by law (every 3 months).
Impression of the job market for NPs
- Most NPs in 2000 (54 percent) reported that they did not have a difficult time finding a satisfactory position, and only 10 percent felt that there were no job openings for NPs overall, but the setting-specific evaluations tended to be more negative. The number of NPs that reported no job openings in specific settings ranged from 18 percent in physician offices to 48 percent in home health agencies.
Nurse practitioners (NPs) are registered nurses (RNs) with advanced academic and clinical experience. They may provide a range of health care services, including health maintenance, disease prevention, counseling, assessment, and management of acute or chronic illness. NPs are growing in importance as health care providers as they grow in number and as preparation becomes available in a greater variety of specialties.
The number of trained NPs in the United States has increased substantially over the course of the past decade, growing more than 240 percent between 1992 and 2000 (USDHHS, 2000). The number of annual NP graduates nationwide more than tripled between 1994 and 1998, and despite a slight decline in 1999 and 2000, the number of annual graduates remains at a much higher level than in 1990 (Wing et al., 2003).
NP specialty preparation is generally available in neonatology, obstetrics/gynecology, pediatrics, school health, family health, adult health, women’s health, psychiatry, geriatrics, and acute care, and other specialties are available in certain States. In New York State in 2000, NP specialties included all of the above, plus a small number of NPs with specializations in community health, perinatology, and oncology.
NPs are a potentially important source of health care. Yet, we still know relatively little about how NPs are used in the health care system, especially in terms of their role as extensions or supplements to physician care. There have been some indications that the scope of practice for NPs has expanded in the past several years (Wing et al., 2003). There have also been some indications that they are no longer predominantly primary care providers, but are increasingly providing some specialty services. Both of these developments would increase the importance of NPs as sources of cost-effective health care.
New York State is one of the most populous States in the Nation, and has the second largest number of NPs of any State in the Nation. New York State ranks 10th in the Nation in NPs per capita. It is also a diverse State racially, ethnically, and geographically. The current study examines licensed NPs in New York State in terms of their educational background, practice patterns, and perceptions of the job market. While not nationally representative, the responses of these New York State NPs are valuable information that may tell us a great deal about the role of NPs in the health care system nationwide.
In the fall of 2000 a survey of all licensed NPs in New York State was conducted under contract from HRSA with the Center for Health Workforce Studies at the University at Albany, State University of New York. The study was intended to produce a snapshot of New York State NPs, with particular emphasis on their educational background, practice patterns, and perceptions of the job market. A short survey asking only limited, basic questions was mailed to 75 percent of licensed NPs (6,157), while a detailed survey was mailed to the other 25 percent of NPs (1,724). Both surveys are presented in Appendix A.
In March 2000, a list of all 9,019 NPs certified in the State was provided to the Center by the New York State Education Department (SED) for the purposes of the survey. A careful review of the list revealed that 453 of the names were duplicates; that is 453 NPs were listed more than once because they were certified in more than one specialty. That left a total of 8,638 individuals with NP certificates.
The review of the NP file also revealed that 430 NPs lived in states that were not contiguous to New York. These NPs also were excluded from the survey. This left 8,208 NPs to be surveyed beginning in spring of 2000. A 25 percent sample of NPs was randomly drawn from each certified specialty with the exception of geriatric and mental health NPs who were intentionally over-sampled. This was done to permit an in-depth analysis of these specialties using the “long” survey form. Because there are only several hundred NPs in each of these specialties, it was determined that a 25 percent sample would not provide a sufficiently large base for a specialty-specific analysis. (Other specialty areas, such as family health, pediatrics and adult health were sufficiently large to permit a specialty-specific analysis without over-sampling.)
In June 2000, 8,208 surveys were mailed to all NPs certified in New York and residing in New York or adjacent States. A second mailing was distributed to the non-respondents in September; and a third mailing was distributed in November. Based on the mailings and returns, it was determined that 52 NPs listed in the SED file had moved to a non-neighboring State and that 3 were deceased at the time of the survey. In addition, 272 NPs had moved and not left a forwarding address. Since one of the requirements for licensure is to notify the Education Department of a change in address, these NPs also were excluded from the analysis. This left a file of 7,881 NPs with an active RN license and certified to work as an NP in the State. 5,989 surveys were received, for a total response rate of 76 percent. 1,319 long form surveys were returned, or a 77 percent response rate, and 4,670 short form surveys were returned, or a 76 percent response rate.
Summary of Survey Responses[1]
Employment Status
The vast majority of survey respondents worked as an NP – 76 percent exclusively as an NP, and 20 percent as both an RN and NP. Less than 1 percent worked as an RN but not as an NP, while 0.5 percent did not work as either an RN or NP, and about 2 percent were permanently or temporarily inactive (Figure 1).
Gender and Race/Ethnicity
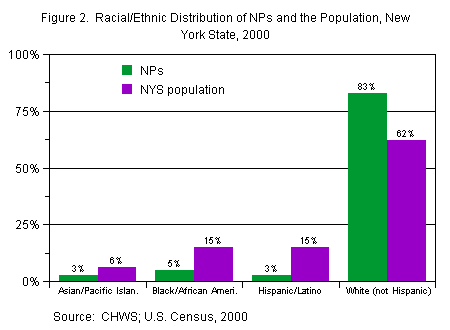
NPs were 94.5 percent female and 5.5 percent male. Almost 83 percent of NPs were non-Hispanic white, while 5 percent were non-Hispanic black, and almost 3 percent were Asian or Pacific Islander. Almost 3 percent were Hispanic/Latino(a) (mostly Puerto Rican). Less than one-half of one percent of NPs were American Indian/Alaskan Native. Over 90 percent were native-born U.S. citizens, and almost all of the remainder were naturalized citizens. Only 1.5 percent of NPs were non-citizen permanent residents. Figure 2 indicates the racial/ethnic distribution of NPs compared to the State as a whole.
Source: CHWS; U.S. Census, 2000
Age and Graduation Cohort
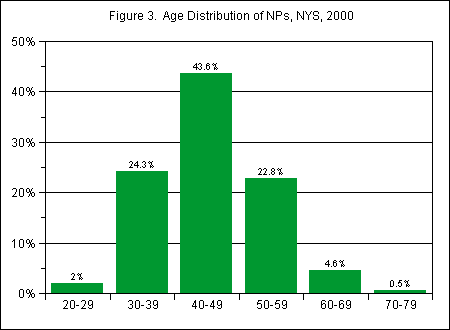
The median age of NPs in 2000 was 45 (compared to 39 for the civilian labor force and 44 for New York State RNs in the same year). The largest age group of NPs was those in their 40s, who constituted almost 44 percent of the total. Only 2 percent of NPs were in their 20s, but more than 5 percent were age 60 or over (Figure 3).
Race by age
Racial distribution changed notably by age, with younger age groups having more racial and ethnic diversity. All of the NPs age 65 and over were non-Hispanic white, but only 71 percent of NPs ages 25 through 34 were non-Hispanic white. Among those ages 25 through 34, non-Hispanic blacks constituted 10 percent of NPs, while Hispanic/Latinos constituted over 6 percent. Asians constituted over 9 percent, and Native Americans were 0.9 percent of NPs. Despite this increasing diversity among the youngest NPs, blacks and Hispanic/Latino(a)s were still underrepresented relative to their share of the U.S. population, although the youngest group of NPs had a more representative share of blacks (10 percent versus 12 percent in the population) than many other health professions. Asian-Americans, however, were becoming increasingly over-represented among younger NPs (Figure 4).
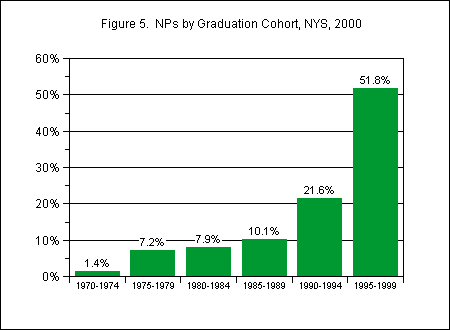
Nearly 29 percent of NPs reported graduating from their NP program between 1960 and 1990, while another 37 percent graduated between 1991 and 1996 and 32 percent graduated between 1997 and 1999. This is consistent with the growth in NP programs and with formal legal recognition of NPs in New York State in 1989 (Figure 5).
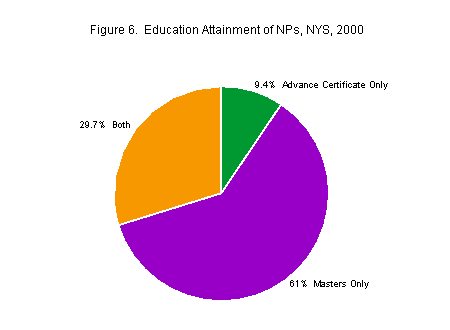
Most NPs (61 percent) had a master’s degree and no advanced certificate, while another 30 percent held both a master’s degree and an advanced certificate. Only about 9 percent of NPs held an advanced certificate only.
Thirty-nine percent of NPs had practiced less than 10 years as an RN prior to obtaining NP certification, while another 21 percent had practiced at least 10 but not more than 15 years as an RN. Fifteen percent of NPs had practiced 20 or more years prior to becoming an NP. The median number of years practiced as an RN prior to NP certification was 12 years.
Twenty-four percent of the respondents reported not having a national NP certification, which is not required by New York State. Among those certified, the most common certifying organization was the American Nurses Credentialing Center (ANCC). Over 52 percent had an ANCC certification, while about 8 percent held a certification from the American Academy of Nurse Practitioners (AANP) and the National Certification Corporation (NCC) certified another 8 percent. Six percent were certified by the National Certification Board of Pediatric NPs/Nurses (NCBNP/N), and 3.5 percent reported certification by some other certifying organization. Those reporting no certification were not different in age from those reporting a certification, but were slightly more likely to hold an advanced degree rather than a master’s degree (12.0 percent versus 8.6 percent).
Professional Activities
Among those who reported working as an NP, about 80 percent worked 20 patient care hours a week or more as an NP. About 9 percent worked fewer than ten patient care hours a week as an NP (over half of these also worked some patient care hours as an RN), while one-third worked forty patient care hours or more as an NP (13 percent of these full-time NPs also worked some RN patient care hours).
Of those NPs who also worked as RNs, 51 percent who reported their RN hours reported fewer than 10 per week. Twenty percent of the NP/RNs who reported their RN hours reported 20 or more RN hours per week, and only 9 percent reported 30 or more RN hours. It should be noted, however, that fully one-third of respondents who reported working as both an NP and an RN did not report any RN hours. The meaning of this isn’t clear; perhaps some respondents reported themselves as both an RN and an NP under the rationale that they had been trained as an RN, although the option given was worded as “Working in positions as both NP and RN”. It is also possible the RN hours of those who worked in both positions were very variable, and therefore some respondents did not feel comfortable reporting a number.
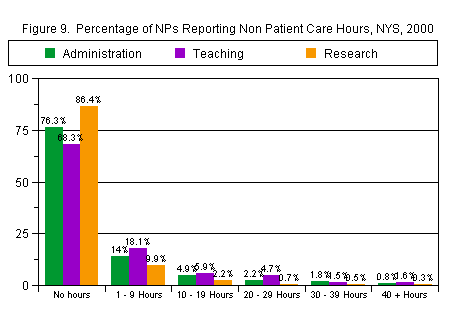
Fifty-seven percent of active patient care NPs reported that they did not engage in any administrative, teaching, or research tasks, although 7 percent reported spending some time in all three. Twenty-four percent of NPs spent some time in administration, although the vast majority of these (61 percent) spent fewer than 10 hours a week on such activities. Only 3 percent reported 40 hours or more a week on administrative activities. Thirty-one percent of NPs spent some time teaching. The majority of teaching NPs (58 percent) spent less than 10 hours a week on teaching activities. Only 14 percent of NPs spent time on research activities, and of those that did, only 2 percent spent 40 hours a week or more on such activities. Seventy-four percent of NPs who did research spent less than 10 hours a week doing so.
Specialty Certification
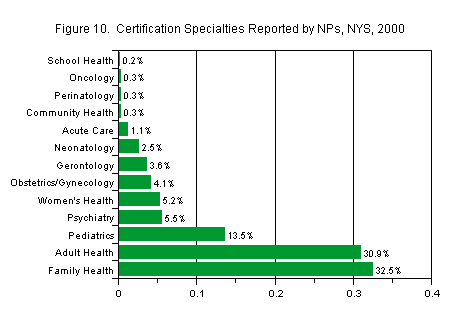
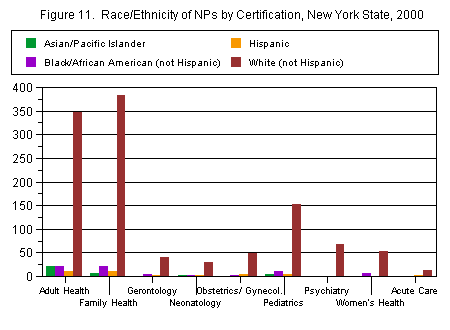
The most common specialty reported by NPs was family health (33 percent), followed by adult health (31 percent). Almost 14 percent reported a specialty in pediatrics. Other areas included women’s health, obstetrics/gynecology, gerontology, neonatology, and acute care. Very small numbers of NPs reported certifications in community health, perinatology, oncology, or school health (Figure 10).
Specialty by race
The highest percentage of most racial/ethnic groups specialized in either adult health or family health, because these were the most popular certifications. Looking at the racial distribution within specialties, some racial/ethnic differences become clear. The specialty with the highest concentration of non-Hispanic whites was psychiatry, at 92 percent, while the specialty with the lowest concentration of non-Hispanic whites was neonatology, at 81 percent. African-Americans were found in the highest numbers in gerontology (11 percent), while no African-American NPs were found in acute care. Acute care, on the other hand, had a large percentage of Puerto Rican NPs (14 percent), while psychiatry had none. Other Hispanics/Latinos were concentrated most heavily in gerontology and obstetrics/gynecology (both 2.4 percent), while no NPs of other Hispanic ancestry were found in women’s health or acute care (Figure 11).
Specialty distribution by age
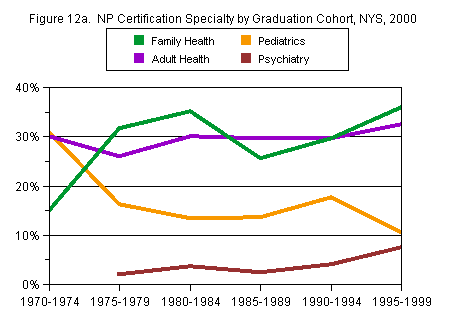
Specialty distribution changed somewhat between the most recent cohorts of NP graduates and earlier cohorts, with family health and psychiatry becoming more popular among the recent cohorts, and obstetrics/gynecology, pediatrics, and women’s health becoming less popular. None of the NPs graduating after 1990 reported certification in oncology, perinatology, or school health. None of those graduating before 1997 reported certifications in community health, and none graduating before 1991 reported certifications in acute care (Figures 12a and 12b).
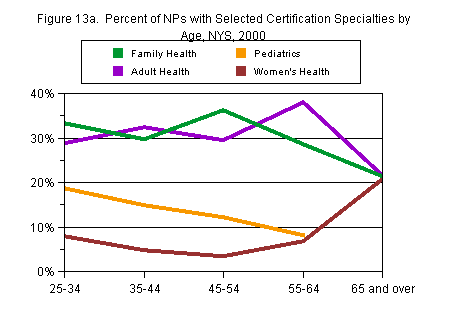
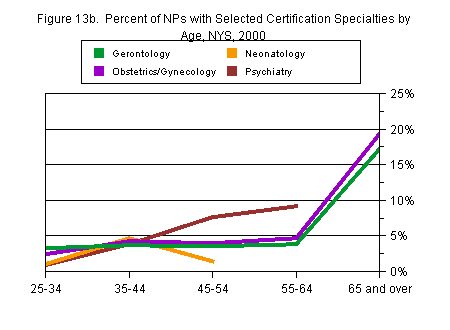
It is especially important with the NP profession, however, to look at graduation year and age separately. Although the youngest NPs are by definition recent graduates, many of the older NPs may be recent graduates as well. Therefore, cohort trends will not necessarily reflect age trends.
In fact, adult health, which had become slightly more popular among the most recent cohorts, was less popular among the youngest NPs. Pediatrics, which had been declining steadily in popularity by graduation cohort, was actually a more popular certification among the younger NPs than the older ones. The reverse was true for psychiatry. Although it had been more popular in recent cohorts of NPs, it had been so primarily among older NPs. Women’s health, declining in popularity by cohort, was somewhat more popular among younger than among middle-aged NPs (Figures 13a and 13b).
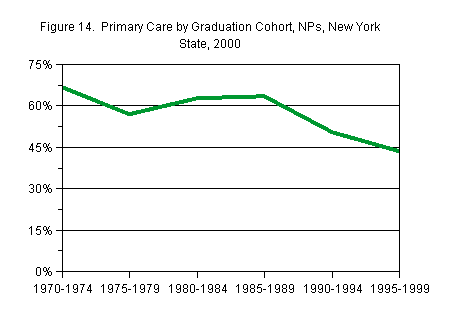
Recent graduation increasingly cohorts were more likely to do specialty care, and less likely to do primary care. In the most recent cohort, the percentage practicing specialty care was larger than the percentage practicing primary care. A similar pattern occurs by age – within most age groups, the numbers practicing primary and specialty care were about equal. Among the oldest age group, however, primary care was much more common than specialty care. Eighty percent of the NPs who were age 65 and older practiced primary care.
Practice Settings
Seventy percent of NPs reported working at only one practice site. Another 23 percent reported working at two practice sites, and 8 percent reported working at three or more. About half of NPs reported that they provided primary care at their first practice site, while the other half reported providing specialty care.
The most common principal practice settings for NPs are M.D. group practices (22 percent), hospital ambulatory care (15 percent), other settings (13 percent), hospital inpatient care (11 percent), M.D. solo practice (9 percent), community health centers (7 percent), nursing homes/extended care facilities (5 percent), NP group practices (5 percent), hospital emergency rooms (2.4 percent), NP solo practices (2 percent), occupational health (2 percent), elementary or high school health services (1.9 percent), hospital psychiatric facilities (1.8 percent), and state or local health departments (1.5 percent). Small numbers of NPs also work in home health agencies, schools of nursing, ambulatory surgical centers, HMO/MCOs, and temporary agencies (Figure 15).
A similar distribution was found for the second practice site of NPs, with 17 percent of those who reported a second practice site working for a group medical practice, 10 percent working in a hospital inpatient setting, and 9 percent working in a hospital ambulatory care setting. Over 8 percent reported that their second practice site was a community health center. More than 5 percent of NPs list that they were in solo practice as a second practice setting.
NPs were most likely to report working for a first practice site with a physician specialty in family practice (13 percent), obstetrics/gynecology (12 percent), general internal medicine (11 percent), and general pediatrics (11 percent). The most popular second practice sites, however, were somewhat different. Of NPs reporting a second practice site, 15 percent reported that the physician at their second site specialized in obstetrics/gynecology, 10 percent reported psychiatry, and 10 percent reported family practice. More than 7 percent of NPs who worked at a second site reported that the physician specialized in geriatrics.
The majority of those with a specialty in adult health (46 percent) worked in either general internal medicine or one of its subspecialties (including 9 percent who worked with geriatricians). Those with a specialty in family health tended to work with family practitioners (31 percent). Fifty-five percent of those with a specialty in gerontology worked with geriatricians (and another 17 percent worked with either general internists or general family practitioners). Eighty-five percent of those with a specialty in pediatrics worked with a pediatrician (either generalist or specialist), while 28 percent of those with a neonatology specialty worked with pediatricians. Seventy-four percent of those specializing in obstetrics or gynecology worked for an obstetrician/gynecologist, as did 86 percent of those with a specialty in women’s health. Ninety-four percent of those with a psychiatry specialty worked with psychiatrists.
Practice setting by age
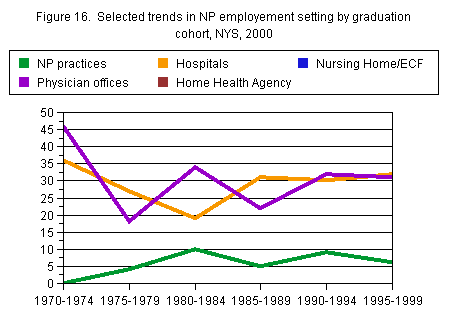
Perhaps the greatest change in practice by graduation cohort was the diversity of practice settings. Those NPs who graduated between 1970 and 1974 reported only four descriptions of their principal practice site: MD group practice, hospital ambulatory care, community health center, and “other”. Recent cohorts, on the other hand, were found in 19 practice settings.
Recent cohorts were also more likely to work in NP group practice, MD solo practices, hospital inpatient settings, home health agencies, nursing homes, and ambulatory surgical centers. They were less likely to be in hospital ambulatory care, in elementary or high school health services, in nursing education programs, community health centers, HMOs/MCOs, state and local health departments, or occupational health. Overall, the trends seem to have been relatively static since at least the 1985-1989 cohort.
Trends by age were less distinct, possibly indicating that the deciding factor in practice patterns was the climate of the profession at the year of one’s graduation. There was a clear trend, however, towards more employment in physician group practices among younger NPs. The likelihood of having one’s own practice appeared to be higher among older NPs. This would be logical, as older NPs might have the greater experience and established patient panel necessary to start a solo practice, but the numbers of NPs who have their own practice was so low as to make a detailed breakdown by age group unreliable.
Practice setting by specialty
The practice settings of NPs varied by specialty. Those with certifications in adult health were most likely to work in a medical group practice (18 percent), or in hospital inpatient (15 percent) or ambulatory services (16 percent). Those in family health were most likely to serve in medical group practices (24 percent) or medical solo practices (11 percent), although a large number were found in community health centers (almost 9 percent). Those with certifications in gerontology were most commonly found in nursing homes and extended care facilities (34 percent), followed by hospital ambulatory care. The vast majority of neonatal NPs (84 percent) worked in hospital inpatient settings, while the remainder 16 percent) worked in medical group practices. Those certified in obstetrics/gynecology were most often found (37 percent) in medical group practices, and community health centers (12 percent), and almost 10 percent were found in NP group practices.
The most common setting for pediatric NPs (32 percent) was in medical group practices, while most psychiatric NPs were in psychiatric hospitals or community health centers. Those specializing in women’s health were equally likely to be found in medical group practice or in hospital ambulatory practice (27 percent). The majority of acute care NPs (57 percent) were found in hospital inpatient settings (Table 1).
Table 1. Broad Practice Settings for NPs, by Certification, NYS, 2000
|
NP Practice |
Physician Practice |
Hospital |
Nursing |
Community Health Center |
|
|---|---|---|---|---|---|
| Adult Health |
5.5 percent |
29.0 percent |
37.3 percent |
7.3 percent |
1.5 percent |
| Family Health |
7.3 percent |
35.1 percent |
23.7 percent |
3.5 percent |
8.7 percent |
| Gerontology |
6.3 percent |
12.5 percent |
20.8 percent |
33.3 percent |
2.1 percent |
| Neonatology |
0.0 percent |
15.6 percent |
84.4 percent |
0.0 percent |
0.0 percent |
| Obstetrics/ Gynecology |
9.3 percent |
42.6 percent |
9.3 percent |
1.9 percent |
13.0 percent |
| Pediatrics |
4.9 percent |
37.5 percent |
29.9 percent |
1.1 percent |
8.2 percent |
| Psychiatry |
15.6 percent |
7.8 percent |
28.1 percent |
4.7 percent |
17.2 percent |
| Women's Health |
5.6 percent |
36.1 percent |
31.9 percent |
0.0 percent |
13.9 percent |
| Acute Care |
0.0 percent |
0.0 percent |
73.3 percent |
0.0 percent |
0.0 percent |
Scope of practice and reimbursement/provider status
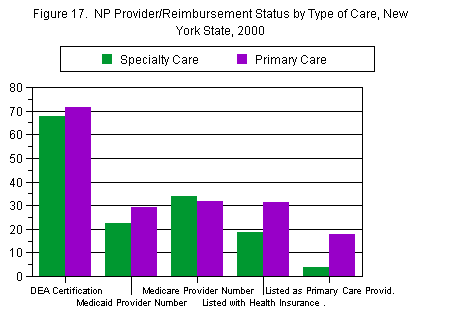
Sixty-eight percent of NPs reported that they were Drug Enforcement Agency (DEA) certified to prescribe controlled substances, 25 percent had their own Medicaid provider number, and 32 percent had their own Medicare provider number. Twenty-four percent were listed as a participating practitioner with a health insurance plan, and only 10 percent were listed as a “primary care practitioner” with a managed care plan (Figure 17).
These numbers depended in part upon whether the NP reported providing primary or specialty care at the primary practice site. Although there were few differences by DEA certification and having a Medicaid or Medicare provider number, primary care NPs were more likely than specialty care NPs to be listed as a participating practitioner with a health insurance plan (31 percent versus 19 percent), and to be listed as a primary care provider with a managed care plan (18 percent versus 4 percent).
Although 47 percent of NPs had no hospital privileges, 15 percent could see inpatients and write both notes and orders, while over 7 percent had admitting privileges. Ninety-three percent of NPs performed histories and physical examinations, 94 percent ordered laboratory tests, 90 percent made direct referrals to specialists, and 32 percent provided on-call services. Fewer than 5 percent reported that they assisted physicians in the operating room.
Scope of practice by specialty
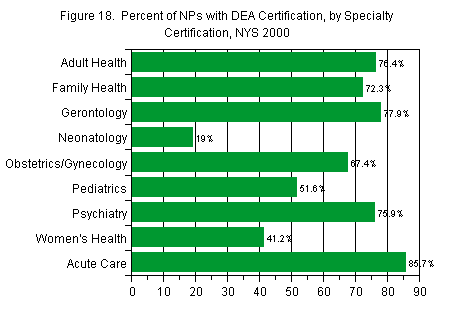
Although a majority of NPs were DEA certified to prescribe controlled substances, this varied substantially by specialty, as shown in Figure 18. NPs in acute care were most likely to have this privilege (86 percent), followed by those in gerontology (78 percent) and in adult health and psychiatry (both 76 percent). Least likely to have such privileges were those in neonatology (19 percent) and women’s health (41 percent).
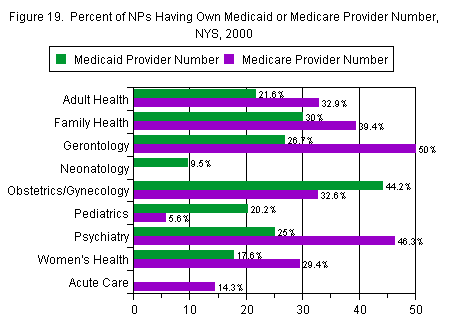
Most likely to have a Medicaid provider number were NPs in obstetrics/gynecology (44 percent), followed by family health (30 percent). No acute care NPs had their own Medicaid number, and only 9.5 percent of those in neonatology did. A slightly different pattern emerged in regard to Medicare provider numbers. Not unexpectedly, the NPs most likely to have such a number were those in gerontology (50 percent). More surprising is that psychiatric NPs were second most likely to have a Medicare number, at 46 percent. No neonatology NPs had such a number, and only 5.6 percent of pediatric NPs did (Figure 19).
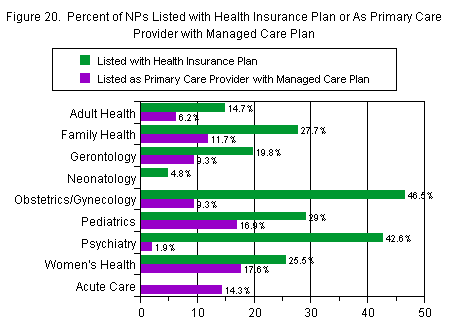
NPs in obstetrics/gynecology were most likely to be listed with a health insurance plan (47 percent), followed by those in psychiatry (43 percent). Least likely were those in acute care (none), and those in neonatology (4.8 percent). Those in women’s health care were most likely to be listed as a PCP with a managed care plan (18 percent), followed by those in pediatrics (17 percent). Those in neonatology (0 percent) and psychiatry (1.9 percent) were least likely (Figure 20).
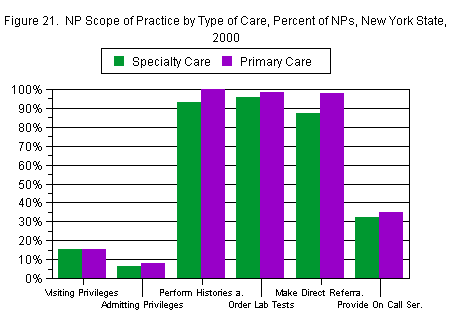
Scope of practice also depended in part upon the type of care provided, as shown in Figure 21. There was little difference in terms of visiting or admitting privileges, performing exams, ordering lab tests, or providing on call services (although primary care NPs were slightly more likely to do all of these), but primary care NPs were more likely to make direct referrals to specialists (98 percent versus 88 percent).
Although over half of NPs 52 percent reported that none of their patients were from their own panel of patients, and 57 percent billed under a physician’s name, 24 percent reported that 80 percent to 100 percent of their patients were from their own panel.
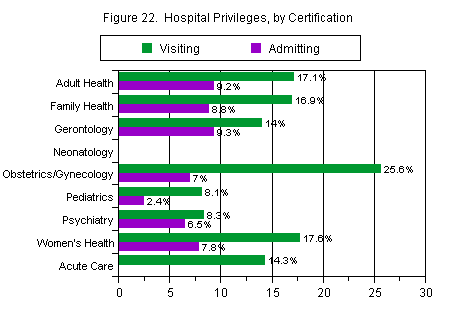
The NPs most likely to have hospital visiting privileges and be able to write notes and orders, as shown in Figure 22, were those in obstetrics/gynecology (26 percent) and in women’s health (18 percent). Those least likely to have such privileges were in neonatology (0 percent) and in pediatrics (8.1 percent). A different pattern emerges for admitting privileges, however. NPs in gerontology and adult health were most likely to have these privileges (9.3 percent and 9.2 percent respectively). Those in neonatology and pediatrics were once again least likely to have such privileges (at 0 percent and 2.4 percent respectively), along with those in acute care (also 0 percent).
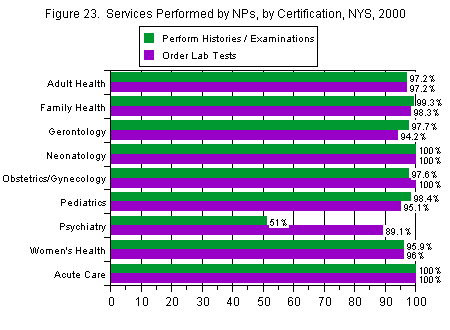
Those in neonatology and acute care (both 100 percent) and in family health (99 percent) were most likely to perform histories and physical examinations, while those in psychiatry (51 percent), women’s health (96 percent) and adult health (97 percent) were least likely. Those in obstetrics and gynecology, neonatology, and acute care (all 100 percent) were most likely to order laboratory tests, while those in psychiatry (89 percent), gerontology (94 percent), and pediatrics (95 percent) were least likely (Figure 23).
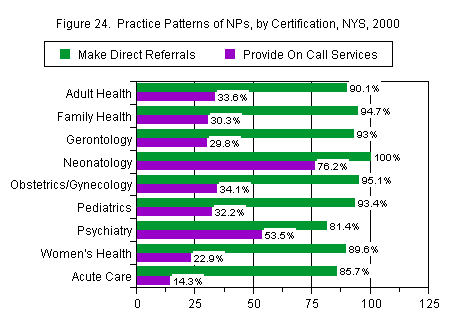
Those most likely to make direct referrals as part of their NP practice were those in neonatology (100 percent), followed by those in family health (95 percent). Least likely to do so were those in psychiatry (81 percent) and acute care (86 percent). NPs in neonatology and psychiatry were the most likely to provide on call services (76 percent and 54 percent respectively), while many fewer acute care (14 percent) or women’s health (23 percent) NPs did so (Figure 24).
Almost half (47 percent)
collaborated with their designated collaborating physician daily, and
almost one-third (31 percent) did so weekly, although 10 percent did so
monthly and 12 percent only did so every 3 months (the minimum frequency
of collaboration required by law), as shown in Figure 25.  [D]
[D]
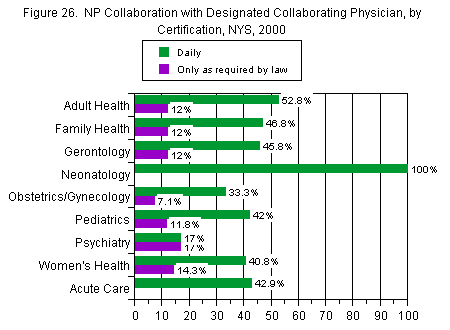
Those most likely to collaborate with their designated collaborating physician on a daily basis, as shown in Figure 26, were those NPs in neonatology (100 percent), and adult health (53 percent). Those least likely to do so were those in psychiatry (17 percent) and obstetrics/gynecology (33 percent). At the other end of the spectrum, a substantial number of NPs only collaborated to the minimum extent required by law – every three months. NPs who were most likely to report this pattern were those in women’s health (14 percent) and those in family health and gerontology (both 12 percent). Those least likely to follow this pattern of collaboration were those in neonatology and acute care (both 0 percent).
Income
NPs earned a median salary of $60,000 [2] in 2000. Given variations in hours worked, however, an hourly salary is a more accurate measure of the actual earning power of NPs. In 2000, NPs earned a median of $33.65 per hour (annual salary divided by hours worked per week). Seventy-five percent of NPs earned more than $45,000 or $27.88 per hour, while 25 percent earned more than $70,000 per year or $40.86 per hour). Sixty-four percent reported that they were paid on an annual salary basis, while 31 percent were paid hourly.
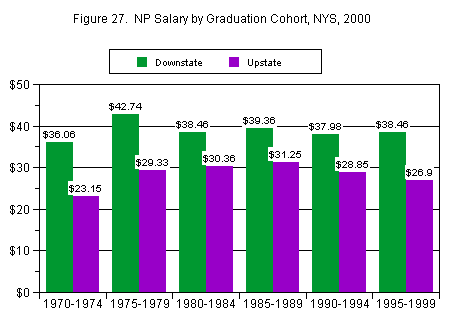
These figures mask dramatic variation by geography, however. NPs in New York City earn substantially more than NPs living in upstate New York. Median salary in downstate New York was $70,000, or $38.46 per hour. Median salary in upstate New York was $50,000, or $28.14 per hour.
Income also varies by setting. The highest rates per hour were commanded by those working in nursing education programs ($76.77), ambulatory surgical centers ($54.29), HMO/MCOs ($46.24), and NP solo practice ($45.15). The lowest rates per hour were earned by those working in State or local health departments ($27.92), or in elementary or high school health services ($29.22), followed by those in M.D. group practice ($30.22) or NP group practice ($31.25).
Income by Age/Graduation Cohort
The highest median hourly salaries were among those who graduated from their NP program between 1975 and 1979 ($39.47) [3] , while the lowest hourly salaries were earned by the 1970 to 1974 cohort ($29.23). Median hourly salary for the most recent graduates (1995-1999) was $33.66. Overall, there was not a clear linear pattern in terms of graduation cohort, with years in practice seeming to have little effect upon salary. Again, however, these figures varied by geography as shown in Figure 27.
Income by race
The highest median hourly salaries were reported by Asian, Puerto Rican, and African-American NPs ($39.84, $40.60, and $40.84) [4]
The lowest were reported by non-Hispanic whites and non-Puerto Rican Hispanics (both $32.69). There were too few Native American NPs to discuss salary reliably. The apparent salary advantage of being Asian, Puerto Rican, or African American was, however, due almost completely to geographical distribution as shown in Figure 27. All of the Asian NPs, 96 percent of the African-American NPs, and 92 percent of the Puerto Rican NPs practiced in the downstate area (where salaries are substantially higher on average), compared to only 50 percent of the non-Hispanic white NPs. Hourly salaries were very similar across ethnicity in the downstate area, with the exception of Hispanic/Latinos other than Puerto Rican, who earned substantially less than the others.
Income by specialty
The highest median hourly salary was reported by neonatology NPs ($41.40) [5] , followed by acute care NPs ($40.87). The lowest was reported women’s health ($30.59), and family health ($31.42) NPs (Figure 28).
Once again, variation existed in salary by geographical location, with neonatology, psychiatry, and acute care the highest-paid specialties in downstate New York, while psychiatry, obstetrics/gynecology, and neonatalogy ranked highest in upstate New York. Gerontology, which ranks sixth out of nine specialties overall, ranked eighth out of nine downstate and last of nine upstate. More geriatric NPs practice downstate where salaries are higher, therefore artificially inflating their overall median salary (Table 2).
Table 2. Median Hourly Salaries for NPs by Certification, Downstate versus Upstate New York, 2000
| Adult Health |
Downstate |
$39.47 |
|---|---|---|
| Upstate |
$28.85 |
|
| Family Health |
Downstate |
$36.81 |
| Upstate |
$27.40 |
|
| Gerontology |
Downstate |
$36.94 |
| Upstate |
$24.52 |
|
| Neonatology |
Downstate |
$42.31 |
| Upstate |
$29.81 |
|
| Obstetrics/Gynecology |
Downstate |
$39.42 |
| Upstate |
$30.05 |
|
| Pediatrics |
Downstate |
$38.46 |
| Upstate |
$26.71 |
|
| Psychiatry |
Downstate |
$40.94 |
| Upstate |
$31.25 |
|
| Women's Health |
Downstate |
$32.05 |
| Upstate |
$28.13 |
Despite having a median age of 45 (compared to 39 for the civilian labor force), very few NPs reported plans to retire (1.8 percent) or reduce their NP patient care hours (3 percent) in the next 12 months. The numbers of those who planned to move their practice to another county (2.7 percent) or to move to another State (2.3 percent) were also small. Although almost 34 percent reported having been at their current position at their principal NP practice for less than 2 years (not surprisingly, since 32 percent had graduated in the 3 years before the survey), over 12 percent had been at their position for more than 10 years.
Location of practice
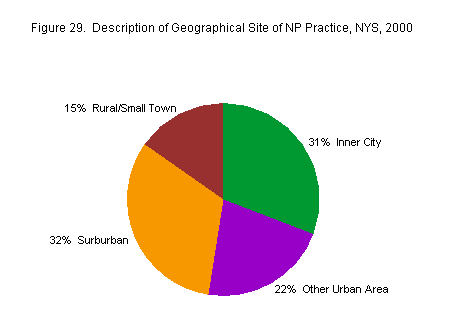
Although 32 percent of NPs practiced in a suburban area, almost as many (31 percent) reported that they practiced in an inner city area. Twenty-two percent practiced in a non-inner city urban area, while 15 percent practiced in a rural area or small town (Figure 29).
Location of practice by race
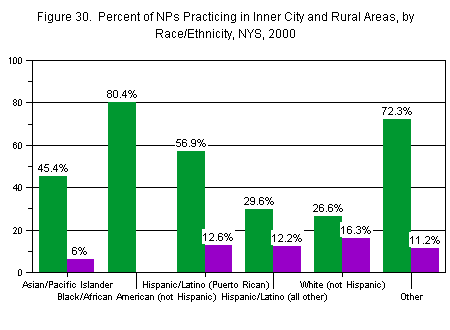
The location of an NP’s principal practice site was strongly associated with race/ethnicity. Over 80 percent of African-American NPs reported that they worked in an inner-city area, compared to less than 27 percent of non-Hispanic whites. A large share of Puerto Rican NPs (57 percent) and Asian NPs (45 percent) also worked in inner city areas. Fewer non-Puerto Rican Hispanics (30 percent) and no Native Americans worked in the inner city.
Almost 81 percent of Native American NPs worked in a small town or rural settings (there were, however, too few Native American respondents for this to be reliable). Whites were also likely to work in a small town or rural environment, at 16 percent. No African-American NPs and only 6 percent of Asian NPs worked in such environments, although almost 13 percent of Puerto Ricans and 12 percent of other Hispanics did so (Figure 30).
Geographical distribution by age
More recent graduates were more likely than earlier graduates to practice in the New York City and Nassau-Suffolk Health Service Area (HSA), and also slightly more likely to practice in the Northeastern New York HSA. They were less likely than older cohorts to practice in other New York HSAs. They were somewhat more likely to practice in inner cities and in suburbs than older cohorts, but were less likely to practice in other urban areas and in rural areas.
Type of care provided also varied by geographical site of practice, as shown in Figure 31. NPs were substantially more likely to provide primary care in rural areas (67 percent) than in any other type of area. They were most likely to provide specialty care in a non-inner city urban area (64 percent).
IV. Impression of job market for NPs
Fifty-four percent of NPs reported that they did not have a difficult time finding a satisfactory position as an NP, although 38 percent said that they did. Among those who reported such difficulties, the most common reason given was an overall lack of practice opportunities for NPs (32 percent), although 26 percent faulted their geographic location, and 17.5 percent felt that there was a lack of opportunities in their desired specialty (Table 3).
Table 3. Reasons Given for Having a Difficult Time Finding a Satisfactory NP Position, NYS, 2000
| Overall lack of practice opportunities |
31.9 percent |
| Lack of practice opportunities for NPs in desired geographic locations |
25.9 percent |
| Lack of practice opportunities for NPs in desired specialty |
17.5 percent |
| Lack of practice opportunities for NPs in desired practice setting |
15.0 percent |
| Inadequate salary/compensation offered |
14.4 percent |
| Family/spouse considerations |
4.2 percent |
| Other |
4.6 percent |
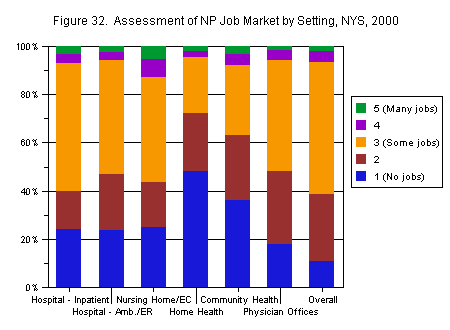
While a majority of NPs reported that they did not have difficulty finding a position, their assessments of job opportunities in their specialty within a 50-mile radius of their principal practice appeared bleak. When the respondents were asked to rate opportunities on a scale of 1 (no job openings) to 5 (many job openings), 24 percent reported no openings in either hospital setting, 25 percent reported no openings in nursing homes, and 48 percent reported no openings in home health agencies. Thirty-six percent reported no opportunities in community health, and 18 percent reported no opportunities in physician offices. (It should be noted, however, that large numbers of respondents reported “don’t know” for their setting-specific evaluations; the numbers reported here include only valid responses.) Their overall assessment, however, was somewhat better. Only 10 percent of respondents reported no job openings overall (Figure 32).
Job Market Experiences by Age
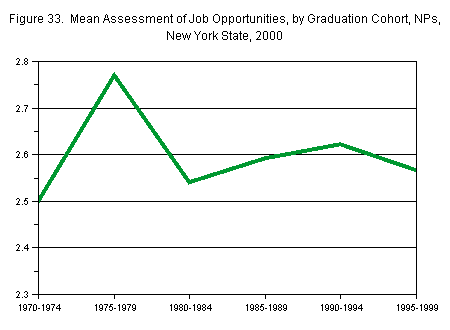
Perceptions of the job market for NPs varied by graduation cohort, with those who graduated between 1995 and 1999 expressing more negative attitudes (Figure 33). Asked to express their perceptions of the job market on a scale of 1 to 5, with 1 representing no jobs and 5 representing many jobs, the mean assessment for this cohort was 2.57, the lowest assessment since the 1980 to 1984 graduation cohort (2.54).
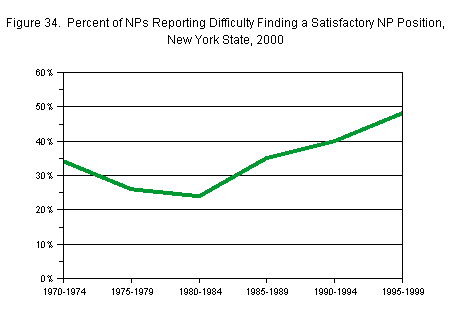
Recent NP graduates also reported steadily increasing difficulties in finding satisfactory positions. Only 24 percent of those graduating between 1980 and 1984 reported difficulty in finding a position, but this had risen to 48 percent in the 1995 to 1999 cohort (Figure 34).
Job opportunities by specialty
Perceived job openings by setting were rated on a scale of 1 to 5, with 1 representing no job openings, 3 representing some job openings, and 5 representing many job openings. Overall, as shown in Figure 35, neonatologists saw the best job opportunities for themselves (mean score of 3.3, and 19 percent believed that many jobs were available), while acute care NPs saw the least (mean score of 2.4). Pediatric NPs were most likely to report no jobs, however (17 percent).
Examining evaluations by certification rather than by setting, adult health NPs felt their opportunities were best in nursing homes and hospital inpatient settings. Family health NPs and geriatric NPs also believed that their opportunities were best in nursing homes. Neonatology and psychiatry NPs clearly felt that they had the most opportunity in hospital inpatient settings (pediatric NPs did also, but the mean score they assigned to inpatient settings was only slightly higher than for other settings), while ob/gyn and women’s health NPs evaluated their opportunities in physician offices most positively. The responses of acute care NPs were difficult to evaluate, because many acute care NPs responded “don’t know” to several settings, making the number of valid responses in those settings too small to be meaningful. They reported good opportunities for themselves in both types of hospital settings, and in physician offices, with the score for hospital ambulatory/emergency care slightly higher than for the other two.
The NPs reporting the highest mean score for job opportunities in hospital inpatient settings were neonatologists (3.06), although gerontologists were most likely to report many jobs in this setting (7.6 percent). The group that clearly perceived the least opportunity in this setting is NPs in obstetrics/gynecology, who gave a mean score of only 1.83, and 52 percent of whom believed that there were no jobs in hospital inpatient settings.
The NPs reporting the highest mean score for job opportunities in hospital ambulatory care/emergency care were those whose specialties were in adult health (2.48), although gerontology NPs were the most likely to report many jobs in this setting (5 percent). NPs in women’s health appeared to have the least opportunities in this setting, with 42 percent reporting no jobs available, and a mean score of only 2.0.
The highest mean score for jobs opportunities in nursing homes was reported by NPs in gerontology (2.79), followed by adult health (2.70). In terms of the likelihood of reporting many jobs, however, those with certifications in adult health reported the greatest opportunity in nursing homes, with 8.6 percent reporting many jobs, followed by psychiatric NPs at 5.5 percent. Geriatric NPs were also likely to report many jobs available in this setting (5.3 percent). The lowest mean score was for obstetric/gynecological NPs (1.62), although neonatologists were those most likely to report no jobs available, at 67 percent.
There was relatively little variation in the average scores given by NPs to job opportunities in home health agencies. The highest mean score was given by those in pediatrics (2.1), while the lowest was in obstetrics/gynecology (1.4). Although 69 percent of ob/gyn NPs perceived no job opportunities in home health, 5.4 percent of pediatric NPs perceived many job opportunities.
Psychiatric NPs perceived the greatest opportunities in community health settings, with a mean score of 2.4, while neonatologist perceived the least (mean score of 1.8). Neonatologists were also the most likely to perceive no jobs in community health. Those most likely to perceive many jobs in community health were those in adult health and women’s health (6.8 percent and 6.7 percent respectively).
Ob/gyn NPs believed themselves to have the highest job opportunities in physician offices (2.7), while acute care NPs believed themselves to have the lowest (2.2). Neonatologists, however, were the most likely to report no jobs in this setting (33 percent), while those in adult health were most likely to report many jobs (3.8 percent).
NPs in independent practice
Eight percent of NPs reported being in group or solo NP practice at either their principal and/or secondary practice site. These NPs were most likely to be in family health (37 percent), adult health (23 percent), or psychiatry (17 percent), and 54 percent reported having at least one other practice site. Their median age (45) was the same as that for all NPs, and they were slightly more likely to be male (6.4 percent versus 5.4 percent for all NPs).
They were 90 percent white compared to 87 percent for all NPs, and held similar educational credentials. They had practiced as NPs for a median 5 years, and as RNs for a median 12.0 years.
They were more likely to have DEA certification to prescribe controlled substances (74 percent versus 68 percent), more likely to have a Medicaid provider number (41 percent versus 23 percent), and more likely to have a Medicare provider number (48 percent versus 30 percent). They were more likely to be listed with a health plan (42 percent versus 23 percent) and to be listed as a PCP with a managed care plan (13 percent versus 10 percent).
The appeared, on average, to be slightly more likely to have hospital-related privileges: they were more likely to have visiting privileges and be permitted to write notes and orders (18 percent versus 15 percent), and they were more likely to have admitting privileges (12 percent versus 7 percent). They were less likely to perform histories and physical examinations (88 percent versus 96 percent), were slightly more likely to order lab tests (99 percent versus 97 percent), and were more likely to be able to make direct referrals to specialists (97 percent versus 92 percent) and to provide on-call services (50 percent versus 32 percent). They collaborated with their designated collaborating physician somewhat less often, with 16 percent only meeting the minimum legal requirement compared to 12 percent of all NPs who observed only the minimum requirement.
Appendix A: The Survey Instruments [S1]
[1] All data presented are weighted data.
[2] These figures exclude extreme outliers (those reporting earnings more than three standard deviations above the mean, or more than $277,010 annually).
[3] These figures exclude extreme outliers (those reporting earnings more than three standard deviations above the mean, or more than $277,010 annually).
[4] These figures exclude extreme outliers (those reporting earnings more than three standard deviations above the mean, or more than $277,010 annually).
[5] These figures exclude extreme outliers (those reporting earnings more than three standard deviations above the mean, or more than $277,010 annually).
[S1] Unless someone has an electronic copy of the survey instruments, I will have to scan them and attached the scanned copies.