|
The approximately 200 practicing pediatric
rheumatologists in the United States practice
in a limited number of geographic areas.
As a consequence, other physicians---internist
rheumatologists and primary care providers---may
substitute for pediatric rheumatologists
in some regions. Several studies suggest,
for example, that internist rheumatologists
play a prominent role in the care of children
with these diseases. 1,
4, 21
A 2000 report revealed that one-third
of children with a known rheumatic disease
received their care from an internist
rheumatologist. 27
A study of Medicaid children eligible
for Supplemental Security Income (SSI)
found that only 18 percent of children
with juvenile rheumatoid arthritis (JRA)
saw a pediatric subspecialist and 30 percent
saw an internist subspecialist. 1
Receipt of Care
by North Carolina Medicaid Children with
Juvenile Rheumatoid Arthritis
North Carolina Medicaid claims data provide
an opportunity to characterize physician
utilization among North Carolina Medicaid
enrollees with JRA. North Carolina ranks
33rd in the Nation in the ratio
of children to pediatric rheumatologists.
It is also a predominantly rural State
with pediatric rheumatologists (n=4) located
only in Chapel Hill, Durham, and Greenville.
Pediatric rheumatology care is available
also in bordering areas such as Knoxville,
TN, Richmond, VA, and Norfolk, VA.
Children who had two or more physician
visits with one of the following ICD-9
CM diagnosis codes in a given year were
considered to have JRA: 714.3, 714.30,
714.31, 714.32, and 714.33. Analyses
were limited to children who were continuously
enrolled for one or both of the following
time periods: July 1, 1998 through June
30, 1999 or July 1, 1999 through June
30, 2000.
Physician specialty codes were used to
classify JRA-related physician visits
[vii]
by provider specialty. Unfortunately,
North Carolina Medicaid claims data from
hospital-based physician practices usually
do not identify the specific physician
for whom the claim was generated. For
example, claims from the Private Diagnostic
Clinic at Duke University Medical Center
and those from University of North Carolina
(UNC) Physicians and Associates come from
the overall physician practice without
an individual provider identifier; as
a result, one cannot definitively identify
the treating physician. JRA claims from
these types of physician practices were
classified as visits to pediatric rheumatologists
when, according to the American College
of Rheumatology, the center had a pediatric
rheumatologist available and the primary
diagnosis was JRA.
Internist rheumatologists were identified
in two ways: using the specialty code
specific to rheumatology and comparing
the list of multispecialty and “other”
providers with the American College of
Rheumatology file to identify misclassified
rheumatologists. Internist rheumatologists
may be underrepresented because care received
at physician practices based in medical
centers, like North Carolina Baptist Hospital
or Carolinas Medical Center, do not list
the specific physician seen. Thus, the
“multispecialty” and “other” categories
may also include care provided by internist
rheumatologists.
To avoid including children with a one-time
“rule-out” diagnosis, the analyses included
only children with two or more physician
claims with a diagnosis of JRA. The analysis
included only continuously enrolled children
to ensure that we had all physician claims
for each study child. In 1999 and 2000,
respectively, 67 and 68 continuously enrolled
Medicaid children had two or more physician
visits with a diagnosis of JRA (Table
13). Of these, slightly more than 50
percent had at least one visit to a center
with a pediatric rheumatologist in each
year. [viii]
In both years only 40 percent of all
JRA-related physician visits were to a
pediatric rheumatologist or a medical
center with a pediatric rheumatologist.
General pediatricians and internist rheumatologists
provided 15 to 20 percent of all JRA-related
visits to this population.
Table
13: Number of Medicaid-Enrolled Children
with JRA in North Carolina and Distribution
of JRA-related Physicians Visits
|
|
July
1, 1998 to June 30, 1999 |
July
1, 1999 to June 30, 2000 |
|
Number
of Children |
|
|
|
Continuously
enrolled children with 2 or more
MD visits with a JRA diagnosis |
67 |
68 |
|
Seen at a pediatric rheumatology
center for JRA |
36 |
39 |
|
Percent
of all JRA-related physician visits
by MD types |
|
Internist
Rheumatology |
15.4 |
15.4 |
|
Pediatric
Rheumatology |
43.4 |
40.7 |
|
Pediatrics |
19.0 |
19.3 |
|
Ophthalmology |
5.2 |
7.0 |
|
Family
Practice |
3.4 |
3.0 |
|
Multispecialty
clinic |
4.0 |
8.0 |
|
Radiology |
2.4 |
2.6 |
|
Orthopedics |
2.4 |
0.9 |
|
Other |
4.7 |
1.5 |
North Carolina Medicaid data were also
used to characterize the JRA-related physician
management of children. Using only visits
with a JRA diagnosis, children were classified
into groups based on the involvement in
their care of a primary care physician
(PCP), pediatric rheumatologist and/or
an internist rheumatologist. Children
seen by a family practice physician or
a pediatrician, but not seen by any rheumatologists,
were classified as “PCP only;” those with
JRA-related claims from pediatric rheumatologists
only or internist rheumatologists only
were classified accordingly. Those with
JRA-related claims from both a PCP and
a pediatric rheumatologist were classified
as having their care co-managed by these
providers and those seen by both a PCP
and an internist rheumatologist were similarly
classified.
Physician management of JRA care was
fairly evenly distributed across types
in 1999, with “PCP Only,” “PCP with a
Pediatric Rheumatologist,” and “Internist
Rheumatologist Only” each accounting for
around 20 percent of visits (Table 14).
“Pediatric Rheumatologist Only” was the
most common management type, accounting
for over 30 percent of children with JRA.
In FY 2000 the percentage of children
treated exclusively by a PCP declined
nearly 6 percentage points and the percent
being co-managed increased by nearly the
same amount. While these figures suggest
that more than one-half of Medicaid enrolled
children with JRA in North Carolina have
been seen at a center with a pediatric
rheumatologist on staff, one cannot ascertain
that the visits to these centers involved
a visit to a pediatric rheumatologist.
Nonetheless, it is clear that primary
care providers and internist rheumatologists
play an important role in the care of
Medicaid-enrolled children with JRA.
Table
14: Classification of JRA-related Physician
Care among Medicaid-Enrolled Children
with JRA, North Carolina
|
Classification
of JRA Care |
July
1, 1998 to June 30, 1999
(%) |
July
1, 1999 to June 30, 2000
(%) |
|
PCP
only |
19.4 |
13.2 |
|
PCP
with Pediatric Rheumatologist |
20.9 |
26.5 |
|
PCP
with Internist Rheumatologist |
0.0 |
1.5 |
|
Pediatric
Rheumatologist Only |
32.8 |
30.9 |
|
Internist
Rheumatologist Only |
17.9 |
17.7 |
|
Other |
9.0 |
10.3 |
Internist Rheumatologists
as Providers of Pediatric Rheumatology
Care
A 2002 study of physician members of
the ACR (n=4,673) divided these specialists
into three groups: those who treat pediatric
patients only, internist rheumatologists
who treat adults only, and internist rheumatologists
who treat both adults and children. After
restricting the sample to physicians who
provide at least some patient care (n=4,304),
224 were classified as pediatric only
providers, 3,030 as internist rheumatologist
who treated adults only and 1,050 as internist
rheumatologists who also treated children.
Of the 3,141 counties in the United States,
623 (20 percent) have an internist or
pediatric rheumatologist involved in patient
care on at least a part-time basis (Figure
4).
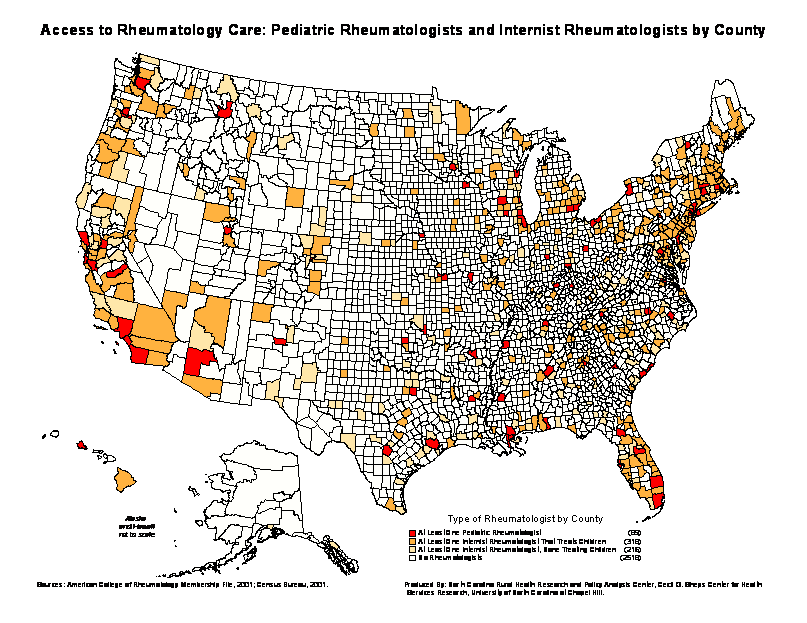
[D]
As Table 15 shows, the authors found
that approximately 50 percent of the population
under age 18 of the United States lived
within 50 miles of a pediatric rheumatologist.
When the parameters were expanded to include
internist rheumatologists who treat adults
and children, the percentage of children
living within 50 miles of a provider of
pediatric rheumatology care (i.e., an
internist who treats children or a pediatric
rheumatologist) increased to 90 percent.
This indicates that internist rheumatologists
are more geographically diffuse than pediatric
rheumatologists and, therefore, their
involvement in the treatment of children
substantially reduces the distances that
must be traveled to obtain care.
Table
15: Percent of the Population Living
within Selected Distances of Rheumatology
Providers by Rheumatology Provider Type
|
|
Percent
of Pediatric Population |
Percent
of U.S. Population |
| Miles
to Nearest Provider |
Pediatric
Rheumatologist Only |
Pediatric
or Internist Rheumatologist who
Treats Children |
Any
Rheumatologist |
| Less
than 10 |
22.7 |
53.2 |
70.4 |
| 10
to 50 |
31.4 |
34.9 |
25.2 |
| 51
to 100 |
19.4 |
8.7 |
3.7 |
| 101
to 200 |
18.4 |
2.5 |
0.5 |
| 200
or more Miles |
8.0 |
0.7 |
0.01 |
Source: Mayer ML, Mellins ED, Sandborg
CI. Access to pediatric rheumatology care
in the United States. Arthritis Rheum
2003; 49:759-65
A survey of California rheumatologists
found that children under the age of 18
represented a small percentage of internist
rheumatologists’ patients. 22
Respondents were asked how many patients
they treat by age group (under 18 years,
and 18 years and older); in addition a
separate question asked if they “treat
pediatric rheumatology patients.” Among
internist rheumatologists who reported
treating pediatric patients, approximately
3 percent of their patients are under
the age of 18. While the number of pediatric
patients seen by individual internist
rheumatologists is small, collectively
they treat a large number of patients
under 18. Using self-reported data on
patient volume, this survey estimated
that, as a group, internist rheumatologists
who report treating children saw a total
of 217 under 18 patients per week. In
addition, many internist rheumatologists
who reported not treating pediatric patients
did, in fact, report treating patients
under the age of 18. These providers,
as a group, treat approximately 202 patients
under the age of 18 in a week. Collectively,
internist rheumatologists were seeing
almost as many patients as were pediatric
rheumatologists who treated an estimated
550 patients under 18 per week.
Factors Influencing
Internist Rheumatologists Involvement
in the Care of Children
Distance to the nearest pediatric rheumatologist
appears to be an important determinant
of internist rheumatologists’ involvement
in the care of children. The aforementioned
2002 national study of ACR members found
that, controlling for a variety of other
factors such as practice type and non-clinical
professional activities, 6
distance to pediatric rheumatology care
was significantly related to internist
rheumatologists’ involvement in the care
of children. Moreover, a study found that
internist-rheumatologists in Washington
State found those who reported treating
children lived a significantly greater
average distance from a pediatric rheumatology
referral center than those who referred
children (101 miles vs. 21 miles) and
distance was the most frequently reported
reason (66 percent) for not referring
a child to a pediatric rheumatologist.
4
A survey of California rheumatologists
found that internist rheumatologists practicing
between 10 and 50 miles from the closest
pediatric rheumatologist were significantly
more likely than those within 10 miles
of a pediatric rheumatologist to treat
children. The odds of treating pediatric
patients among those practicing 50 or
more miles from the nearest pediatric
rheumatologist were nearly 7 times higher
than among those practicing within 10
miles of a pediatric rheumatologist. 22
The AF/ACR Survey conducted in 2004 found
that internist rheumatologists involved
in the care of children practiced a significantly
greater distance from a pediatric rheumatologist,
on average, than those who do not treat
children (66.2 vs. 46.1 miles, p=0.017).
In multivariable analyses that controlled
for provider characteristics, such as
age and distribution of work hours, distance
did not maintain its significance. These
results should be interpreted with caution,
however, as it is estimated that the response
rate among internist rheumatologists in
this survey was less than 20 percent.
Among California internist rheumatologists
who treat children, 79 percent indicated
that personal expertise in pediatric rheumatology
motivated them to treat children. Patient
preferences and distance to the nearest
pediatric rheumatologist also were selected
as motivating factors by 73.3 percent
and 65.8 percent, respectively, of internist
rheumatologists who treated children.
Among internist rheumatologists who do
not treat children, the overwhelming majority
(85.2 percent) refrain from seeing children
because of inadequate personal expertise
in pediatric rheumatology. Most internist
rheumatologists (70.3 percent) also cited
the availability of nearby pediatric rheumatology
care as a reason for their decision not
to treat children with rheumatic diseases.
Among Washington State rheumatologists,
the most common factor in an internist
rheumatologist’s decision not to refer
a child to a pediatric rheumatologist
was distance (66 percent), with the second
most common reason cited as inconvenience
to the child’s family (60 percent).
Data from the California survey also
suggested that practice setting may play
a role in internist rheumatologists’ involvement
in the care of children; those practicing
in multispecialty clinics were significantly
more likely to be involved in the care
of pediatric patients than those who practiced
in other settings. Interestingly, when
queried about their reasons for treating
pediatric patients, 46.2 percent of those
in multispecialty practices cited insurance
barriers to referral versus only 28.8
percent of those in other practice settings.
It is possible that physicians in these
types of groups may be more involved in
independent practice associations (IPA).
IPAs may be less likely to include pediatric
subspecialists and providers may face
disincentives to referring outside their
network of providers, 28,
29
which might explain the somewhat increased
tendency, among those in multispecialty
settings, to report insurance barriers
as a motivating reason for treating children.
Comments from Internist
Rheumatologists
While quantitative analyses are useful
in summarizing survey data, qualitative
data can provide rich and varied insights
into the context of physician practice
decisions. A sample of comments from
California rheumatologists surveyed suggests
that some internist rheumatologists treat
children only because of the lack of available
pediatric providers and appear to be uncomfortable
with their involvement in the care of
these patients. In contrast, other internist
rheumatologists feel they are fully capable
of meeting the needs of this population
and are not called upon to do so often
enough. The following comments are from
this survey.
Distance/Access
- “There is a major shortage of
pediatric rheumatologists. I treat
some pediatric populations out of inaccessibility
to pediatric rheumatologists – I would
like to not treat any or get more training.”
- "I love kids, and feel that
we desperately need more pediatric rheumatologists
but with no pediatric experience in
residency, only 12 clinics in fellowship,
I am unprepared to see kids. I could
easily handle mild JRA cases with MTX/NSAIDs
[methotrexate/non-steroidal anti-inflammatory
agents], pain injections, but the biggest
hold back is my comfort with diseases
of children. Legally and medically,
I would be asking for trouble.”
- “Straight forward pediatric rheum
[atology] or older pediatric patients
I am comfortable taking care of. If
there is an element of doubt, I refer
to Children Hosp LA.”
- “Because of the shortage of pediatric
rheumatologists, I do not mind seeing
old pediatric patients (> 13 yrs)
if I have to. But I definitely prefer
not to treat anyone under 13 years of
age because my training in internal
medicine did not prepare me to treat
pediatric patients.”
- “I rarely receive referrals from
‘peds’ [general pediatricians] for questionable
reasons. ‘Peds’ may feel we are incapable
of treating children with rheumatic
disorders even with training/experience.”
- “The major obstacle to the treatment
of pediatric rheumatology cases in our
area is the hesitance by the local pediatricians.
They all seem to shy away from the care
of really sick children and prefer not
to be involved in their care. Thus,
they almost always refer them out of
the area, causing great inconvenience
and, often, suboptimal care for the
patients. I would strongly suggest
that pediatricians be made aware that
most rheumatologists are quite experienced
and able to care for pediatric rheumatology
patients.”
- “Pediatricians were never taught
to do joint exams. Therefore, they
don't recognize a swollen joint when
they see it, so the child gets referred
to an orthopedist, who does the "only"
sensible thing: they "cast"
it. Weeks later the cast comes off,
oops, now we have a contracture. So
they refer to the university where the
child disappears - where the child never
gets referred back to me (unless HMO
insists). I like kids and could do
your follow-ups locally, save the ‘ped
rheum’ time (and the pts/family time
for appointments). But you never ask
and patients are never even referred
back to me.”
Practice Constraints
- “Because my office is not set
up for children, I only deal with teens
who like being treated like an adult....
I am more at ease with prescriptions.”
- “Too busy with adult patients
to see pediatric patients. Not really
interested in seeing pediatric patients.”
- “In Fresno…there are two excellent
pediatric rheum [atology] MDs but there
is a shortage of adult rheum [atologist]s.”
- “I choose not to tx [treat] pediatric
patients as I never did a pediatric
rotation in my training. Even if I
had done one month of ped [iatric] rheum
[atology] training, I probably would
not treat this population due to professional
liability concerns (I wouldn't be Board
certified in pediatric rheumatology).
Currently, I have a five month waiting
period to see adult patients - I have
little incentive to see pediatric patients
as well.”
Additional comments, not presented here,
underscore the finding of the quantitative
analysis that internist rheumatologists
generally restrict their involvement in
pediatric rheumatology to the care of
adolescents and suggest that some of these
providers also limit their involvement
to children with mild forms of the more
common rheumatic diseases.
It is important to note that while many
internist rheumatologists currently treat
a small number of children and adolescents
with rheumatic disease, their role in
caring for the under-18 population may
decrease in coming years. The aging of
the “baby-boomer” generation will increase
adult demand for the services of internist
rheumatologists and limit their availability
to care for children.
Role of Primary
Care Physicians in Treating Children with
Rheumatic Diseases
A 2001 national survey of physicians’
involvement in the care of children with
rheumatic diseases and factors contributing
to current referral patterns within pediatric
rheumatology found that 11 percent of
pediatricians and 38 percent of family
practitioners had not seen any suspected
or confirmed cases in the 5 years prior
to the survey. 30
Only 3 percent and 1 percent of pediatricians
and family practitioners, respectively,
saw more than 10 cases; only one percent
of respondents diagnose and treat patients
with JRA on their own. 30
Forty-two percent of pediatricians and
32 percent of family practitioners refer
all JRA diagnosis and management to subspecialists.
Most of the respondents indicated that
they refer patients to a pediatric rheumatologist
(92 percent of pediatricians and 76 percent
of family physicians); a substantial percent
of family physicians indicated, however,
they refer to general rheumatologists
(37 percent). This may be because many
are located in rural areas where access
to a pediatric rheumatologist may be limited.
30
In analyzing survey responses from general
pediatricians and family physicians, Freed
et al. 30
found that 42 percent of pediatricians
and 19 percent of family practitioners
felt comfortable diagnosing JRA, but only
18 percent of pediatricians and 12 percent
of family practitioners felt they were
adequately trained to diagnose and treat
JRA. Only 10 percent and 4 percent of
pediatricians and family practitioners,
respectively, described themselves as
current on the latest JRA treatments.
Bivariate analyses indicated that PCPs
who reported having inadequate training
in diagnosing JRA were twice as likely
to refer patients as those who described
their training as adequate, implying that
improvements in training may enhance primary
care providers willingness to be involved
in the care of children with rheumatic
diseases. 30
Reported Pediatric
Referral Sources
The 2003 survey of California internist
rheumatologists asked providers to indicate
which groups had referred children with
rheumatic diseases to them. Compared
with internist rheumatologists who did
not report treating children, internist
rheumatologists who did report treating
children were significantly more likely
to be contacted by all referral sources
(Figure 5). 22
It is not clear if internist rheumatologists
decide to treat children because they
are asked to, or if these providers have
a reputation for treating children and,
as a consequence, are more frequently
approached for treatment. It is also
notable that internist rheumatologists
who do not treat children frequently reported
being contacted about seeing a pediatric
patient with a known or suspected rheumatic
condition despite their unwillingness
to treat children.
In their National survey, Freed and colleagues
found that internist rheumatologists reported
that their primary referral sources of
JRA patients were family physicians, followed
by pediatricians, then orthopedists.
Seventeen percent of internist rheumatologists
reported that they never refer JRA patients
to another specialist, and 11 percent
reported referring all of their juvenile
patients. Ninety-six percent of all referrals
from internist rheumatologists were to
a pediatric rheumatologist. 30
Figure
5: Percentage of Internist Rheumatologists
Reporting Requests to See Pediatric Patients
by Requesting Source

[D]
Comfort in Treating
Children
Freed and colleagues found that 88 percent
of internist rheumatologists reported
they are “adequately trained to diagnose
JRA” and 72 percent felt they were “adequately
trained to manage JRA.” 30
Internist rheumatologists reported, nonetheless,
that they often referred these patients
to pediatric rheumatologists. Factors
that were considered most important in
the referral decision were age of patient,
parental request, and refractory clinical
course.31
In a focus group composed of internist
rheumatologists, several indicated that
they would begin treating a patient with
JRA and only refer them to a specialist
if there was no improvement. Most agreed
that proximity to such a specialist also
played a large role in the decision to
refer.
There is evidence that internist rheumatologists
limit their involvement in the care of
children to adolescents. California internist
rheumatologists were significantly less
likely to treat children ages 0-5 and
6-11 than pediatric rheumatologists. 22
Patients ages 16-17, on average, represent
over 50 percent of internist rheumatologists’
pediatric patients. The diseases treated
did not differ significantly, however,
between these providers; for both pediatric
and internist rheumatologists the majority
of patients had JRA or SLE.
Compared to pediatric rheumatologists
significantly fewer California internist
rheumatologists were comfortable treating
each of 18 listed conditions. 22
The majority of internist rheumatologists
were comfortable treating the JRA subtypes,
SLE, dermatomyositis, and spondylarthropathy;
however, less than half of those responding
were comfortable treating Kawasaki’s disease,
Wegener’s granulomatosis, polyarteritis
nodosa, reflex sympathetic dystrophy,
psychogenic rheumatism, and fever of unknown
origin. Most Washington State internist
rheumatologists similarly reported comfort
with treating children with common diseases
such as JRA; however, the percentage of
surveyed physicians who reported comfort
treating rarer diseases that typically
affect younger children was much lower.
4
Analyses of the recent AF/ACR survey
by the Arthritis Foundation and the ACR
had similar findings. Internist rheumatologists
who treat children were less likely than
those who do not treat children to report
that there is an age below which they
are uncomfortable diagnosing or treating
pediatric patients. Even among those
who treat children the majority do report
being uncomfortable diagnosing (78.3 percent)
and treating (80.3 percent) children below
a certain age. The average age below
which they are uncomfortable diagnosing
is lower for those who treat children
than those who do not (9.5 years vs. 14.9
years, respectively, p<0.001). Likewise,
the minimum average age at which a provider
feels comfortable treating a child with
a rheumatic disease is lower for those
internist rheumatologists who treat children
than among those who do not (9.8 years
vs. 15.3 years, respectively, p<0.001).
As expected, internist rheumatologists
who care for children are significantly
more likely than those who do not treat
children to report being comfortable treating
pediatric rheumatic diseases. As shown
in Table 16, internist rheumatologists
who treat children are most uncomfortable
treating Kawasaki’s disease (67.1 percent),
periodic fevers (54.3 percent), somatiform
disorders (46.9 percent), and pediatric
vasculitis (42.1 percent). Those who
do not treat children are significantly
more likely than those who treat children
to report being uncomfortable treating
all reported illnesses.
Table
16. Comparison of Internist Rheumatologists
By Involvement in Care of Children AF/ACR
Survey (N=523)
|
|
Treats
children |
Does
not treat children |
| Uncomfortable
treating in children: |
| Pediatric
vasculitis (%) |
35.6*** |
55.6 |
| Kawasaki’s
disease (%) |
56.8** |
70.5 |
| Systemic
onset JRA (%) |
20.1*** |
45.3 |
| Polyarticular
JRA (%) |
9.0*** |
39.3 |
| Pauciarticular
JRA (%) |
9.3*** |
39.7 |
| SLE
(%) |
17.3*** |
39.7 |
| Scleroderma
(%) |
23.5*** |
46.2 |
| Osteoporosis
(%) |
32.9*** |
47.4 |
| Periodic
fevers (%) |
47.4*** |
65.8 |
| Myositis
(%) |
22.2*** |
41.5 |
| Somatiform
disorders (%) |
40.5*** |
60.7 |
| Other
illnesses (%) |
3.8 |
6.8 |
| **p<0.01,
***p<0.001; from Pearson χ2
for binary variables; from two-sided,
two sample t-test of mean differences
for continuous variables |
Practice Guidelines
Freed and colleagues also explored the
need for continuing education for general
practice physicians and internist rheumatologists
who are likely to treat children with
rheumatic diseases. In a survey 71 percent
of pediatricians, 73 percent of family
physicians, and 73 percent of the internist
rheumatologists indicated that they saw
a need for a JRA practice guideline to
be disseminated to physicians within their
specialty; 30
among focus groups, however, the results
were less consistent. Most pediatricians
agreed that practice guidelines were not
necessary because they usually refer potential
JRA patients to specialists; they indicated
that even if guidelines were available
they would most likely not use them.
Opinions from the family physicians were
mixed; some were skeptical of the benefit
of guidelines because they see potential
JRA cases so infrequently. Those family
physicians who were likely to play a significant
role in the management of JRA care thought
that guidelines would be especially relevant
and helpful. Of the internist rheumatologists
who participated in a focus group, most
agreed that a guideline would be helpful
to keep them updated on recent developments
in the treatment of JRA patients.
Summary
Internist rheumatologists play a prominent
role in the care of children with rheumatic
diseases; evidence suggests that the lack
of available pediatric rheumatologists
influences the involvement of internist
rheumatologists in the care of children.
Nonetheless, studies suggest that they
may limit their involvement to the care
of adolescents and those with mild cases.
The practice locations of internist rheumatologists
are more geographically diffuse than those
of pediatric rheumatologists and, as such,
their involvement in the care of children
with rheumatic disease certainly decreases
the distances that children need to travel
for care. Efforts to enhance the ability
of internist rheumatologists to provide
quality care to children with rheumatic
diseases may help ameliorate the current
shortage.
In contrast to internist rheumatologists,
primary care providers appear to play
a smaller role. Primary care providers’
lack of involvement in the care of children
with rheumatic diseases may reflect the
lack of pediatric rheumatology training
available in many pediatric residency
programs, especially those programs with
a high percentage of trainees who enter
primary care practice. Enhanced training
of primary care providers may enable them
to perform initial evaluation on children
with suspected rheumatic diseases and
minimize the number of unnecessary referrals,
which increase the demand for pediatric
rheumatology care. Moreover, enhanced
training of primary care providers may
increase their willingness and ability
to co-manage the care of children with
rheumatic diseases and ease some of the
patient care burden affecting pediatric
rheumatologists.
|