|
The eighth cycle of the National Sample
Survey of Registered Nurses (NSSRN) followed
the same basic sample design as its predecessors.
The sample design was originally developed
by Westat, Inc. under a contract with
the Division of Nursing, BHPr, HRSA in
1975-76 and can be best described as a
systematic sample of alphabetic clusters
of names in each State using a ‘nested
alpha segment design’. Prior to sampling,
each State was ranked by the sampling
rate such that the highest priority States
were those with the highest sampling rate
(for the most part, small States). As
a result, the alphabetic clusters of names
for lower priority States are ‘nested’,
or included, within those of higher priority
States. This means that a sample name
selected in one State (such as California)
will also have been selected in every
State with a higher priority (in the case
of California, this is all other States).
This design approach takes into account
two key characteristics of the sampling
frame. First, no single list of all individuals
with licenses to practice as registered
nurses in the United States exists, although
lists of those who have licenses in any
one State are available. Second, a nurse
may be licensed in more than one State.
The advantage of the nested alpha-segment
design is that one can determine the probabilities
of selection and appropriate multiplicity
adjusted weights for those nurses that
are listed in more than one State. In
addition, the design also permits the
use of each sample registered nurses’
data for State estimates of each of her/his
States of licensure.
This appendix provides a brief summary
of the methodology of the NSSRN including
the sampling frame, sample design and
the statistical techniques used in summarizing
the data. It also includes a discussion
of sampling errors, provides the standard
errors for key variables in the study
and presents a simplified methodology
for estimating standard errors.
Sampling Frame
The target population for the eighth
NSSRN included all registered nurses with
an active license in the United States
as of March 2004. A sampling frame was
required to select a probability sample
of nurses from which valid inferences
could be made to the target population.
The sampling frame for the eighth NSSRN
consisted of all registered nurses who
are currently eligible to practice as
an RN in the U.S. This sampling frame
included RNs who have received a specialty
license or have been certified by a State
agency as an advanced practiced nurse
(APNs) such as nurse practitioner, certified
nurse midwives, certified registered nurse
anesthetist, or clinical nursing specialist
and excluded licensed practical nurses
(LPNs)/licensed vocational nurses (LVNs).
State Boards of Nursing in the 50 States
and in the District of Columbia (hereafter
also referred to as a State) provided
files containing the name, address, and
license number of every RN currently holding
an active license in that State. These
files formed the basis of the sampling
frame from which the RNs for each State
were selected. The licensure files provided
by the States were submitted on diskette
or compact disk (twenty States), or electronically
as an attachment to an e-mail message
(twenty-seven States). Three States sent
the data via FTP and another provided
the data on their website. For this study,
States were also asked to identify nurses
for whom the State provided advanced practice
nurse (APN) status. In some cases, the
State identified these nurses on the basic
list provided. However, some APNs were
identified on separate lists and their
APN status was appended to the information
on the RN sampling frame.
Each of the 51 State files was checked
for consistency, names were standardized,
and duplicates and ineligible records
were removed from the State list to prepare
the list for sampling.
Sample Design
The NSSRN 2004, the eighth in the series,
continued to oversample nurses in small
States in order to better support HRSA’s
National Center for Health Workforce Analysis’
State level supply and demand projections
for registered nurses. The basic design
was enhanced by using sample design optimization
methodology developed by Chromy [1]
to determine the sample allocation to
the States that would simultaneously satisfy
variance constraints defined by the 51
States and the total U.S.
In the original sample design, and in
the 1988 redesign, the universe of RNs
was sorted alphabetically by last name
and approximately equal-sized clusters
of RNs were constructed by partitioning
the alphabetically ordered list into 250
alpha-segment clusters with equal (or
nearly equal) numbers of RNs. An alpha-segment
was defined as all alphabetically adjacent
names falling within pre-specified boundaries.
For example, all names beginning with
the lower boundary, up to but not including
the name that defined the upper boundary.
From the frame of 250 equally divided
alpha-segments, a total of 40 alpha-segments
were randomly selected, representing a
16 percent sampling rate overall. Registered
nurses are selected in the sample based
on their name, with an RN being included
in the sample if the name of licensure
falls into one of the alphabetic segments
that are in sample for that State.
Although each State had 40 sample segments,
the sample size of each State differed
in size depending on the State’s sampling
rate. While uniform-sampling rates would
have produced the best national estimates,
the resulting sample sizes for the smallest
States would have been inadequate to support
State-level estimates. Since both national
and State-level estimates are required
for the 2004 NSSRN, as was done is prior
surveys, sampling rates were increased
in the smaller States to obtain larger
State-level sample sizes. While this
disproportionate sampling improved the
precision of estimates in the smaller
States, it also reduced precision of national
estimates due to unequal weighting effects.
.
To accommodate the differing State sampling
rates, a planned variation in the size
of the segments, i.e., “portions of alpha
segments” was used. Each of the 40 alpha-segments
selected for sample was divided into ½-,
¼-, 1/8-, 1/16-, and 1/32- portions.
These fractions indicate the size of the
alpha segment portion relative to the
size of the basic alpha-segment.
The sampling rate for a particular State
was achieved using a combination of the
alpha-segment portions. As a result, each
State contains some sample (i.e., a portion)
from each of the 40 alpha-segments, depending
on the sampling rate for the State. For
example, selecting the entire 40 complete
alpha segments on a State list is expected
to constitute a 16 percent sampling rate
(40 ÷ 250 = 0.16) in the State. This is
because each alpha segment contained an
expected 0.4% of the State’s RN names
(40 X 0.4 percent = 16 percent). Likewise,
the sample for a State with an 8 percent
sampling rate consisted of the 40 ½ portion
selections. Several sampling rates use
a combination of portions for each alpha-segment
in sample (rather than one fractional
portion for all alpha-segments). For
example, a 5 percent sampling rate was
achieved by first randomly dividing the
40 alpha-segments into two groups, the
first containing 30 alpha-segments and
the other containing 10; and by using
the ¼ portions from the first group and
the ½ portions from the second group (0.4
percent x [(30 x ¼) + (10 x ½)] = 5 percent).
To identify and account for nurses appearing
in more than one of the 51 State lists,
the portions were constructed such that
each portion was “nested” (or included)
in the boundaries of the larger portion.
As a result, the alpha segment clusters
from the States with lower sampling rates
(typically larger States) were automatically
included in the alpha segment clusters
selected from the States with higher sampling
rates (typically smaller States).
As a result, a RN who was licensed under
the same name in two States with identical
sampling rates was selected (or not
selected) for both States, since the alphabetic
name boundaries defining the portions
are the same for both States. However,
if the RN was licensed under the same
name in two States that are sampled with
different sampling rates, then, if
the RN was sampled in the State with a
lower sampling rate, they were also included
in the sample for the State with the higher
sampling rate (as the alphabetic name
boundaries defining the portions for the
State with the lower sampling rate are
nested within those of the State with
the higher sampling rate). This nesting
property of the sample design maximizes
the chances that the RN will be selected
in all States that they have an active
license in. A nurse that is licensed
in two or more States under the same name
will have a probability of selection corresponding
to the State with the highest sampling
rate.
Sample design optimization techniques
developed by Chromy (1996) were used to
determine how to allocate the sample of
54,000 RNs to the 51 State lists. This
sample size was then converted to a sampling
rate, and the rate was rounded to one
of the admissible rates for the nesting
design. For example, the original rate
for the State of Washington was 1.59%,
the closest admissible rate was 1.5%.
Rates were rounded down only such that
the change in sampling rate still left
their effective sample size at or above
the 1996 NSSRN level.
After determination of frame sizes and
expected sampling rates, the States were
assigned a priority order to properly
determine selection probabilities for
nurses appearing on more than one of the
51 State lists. Traditionally, States
were ordered by size, with larger States
having lower sampling rates and smaller
States having higher sampling rates.
However, as in the 2000 NSSRN, States
were priority ordered based on their sampling
rate. As such, it is mostly, but not
necessarily, the case that States with
larger RN populations had lower sampling
rates.
Essentially the same procedure was followed
for sample selection for all States. Once
a State provided a licensure file containing
all appropriate names of individuals with
active RN licenses and meeting all specifications,
the required sample names in that file
were selected. Regardless of the way
a State alphabetized and standardized
the names in its files, the sample names
were selected according to the standards
established by the survey design. That
is, sample selections ignored blanks and
punctuation in the last names (except
a dash in hyphenated names) and ignored
titles (e.g.,”Sister”).
Registered nurses were selected in the
sample on the basis of name, with an RN
being included in the sample if the name
of licensure fell within a specific alpha-segment
portion as defined by the State sampling
rate. In other words, the sample for
a given State consisted of all RN names
falling into any one of the State’s pre-designated
40 alphabetic portions that corresponded
to the State sampling rate (one portion
from each of the complete 40 alpha-segments
in sample).
The pairs of names that defined the alpha-segment
portion constituted the lower and upper
boundaries corresponding to the sampling
rate. Thus, the membership of the alpha-segment
portion was defined by all names, beginning
with the lower boundary (i.e., the last
name in alphabetical order of all the
names included in that segment), up
to but not including a name that defined
the upper boundary. This latter name
fell into the next alpha-segment. As
was done in the NSSRN 2000, any deviations
of more than 8 percent were candidates
for either an increased or decreased rate.
Because the survey is longitudinal in
nature, a panel structure was constructed
to allow for several of the sample alpha-segments
to be systematically replaced each survey.
Under the original survey design, the
40 sample alpha-segments were arranged
in alphabetical order and then partitioned
into eight groups of five successive alpha-segments
each. One segment from each group was
randomly assigned to each panel, so that
each panel consisted of segments that
spanned the entire alphabet. For each
successive survey, a new panel (consisting
of eight new alpha-segments or 20 percent
of the sample) was entered into the sample,
replacing one of the five panels from
the previous survey. Under this scheme,
a nurse who maintained an active license
in the same State(s) could be retained
in the sample for up to five surveys.
The planned NSSRN 2004 sample size was
54,000 cases, similar to that of the NSSRN
2000, and up from the 45,000 used in previous
studies. Planned sampling rates ranged
from 1.125 percent in several of the largest
States to 15 percent in Wyoming. This
translated into planned sample sizes ranging
from 3,225 RNs in California to approximately
796 in Wyoming. The initial round of
sampling, however, yielded a much smaller
sample than expected due to the variable
size of the alpha-segments in each State.
Thus, a second round of sampling was done
by increasing the sampling rates from
1 to 1.125 in the eleven largest States
and “adding to” the sample selected in
the first round, yielding a total of 56,917
sample cases. After eliminating cross-State
duplications, the expected the sample
size to be fielded was still approximately
54,000 cases.
Table B-1 in Appendix B shows the sampling
rates and sample sizes that were planned
and actually obtained for the 51 States
in the survey. Differences between planned
and actual sampling rates result from
State-specific variation in the distribution
of nurses’ names. States are priority
ordered by sampling rate and size.
Because many nurses are licensed in more
than one State, their names could be selected
in the sample more than once. In accordance
with the sample design, we ensured that
each sampled RN was retained in the outgoing
sample file exactly once to avoid multiple
questionnaires being sent to nurses.
If we identified an exact duplicate, the
nurse in the lower priority State was
coded as a duplicate of the sample member
in the higher priority State. For example,
an Alaska record was coded as a duplicate
to the sample record in Wyoming. Following
data collection, these expected duplicates
were reviewed to ensure that the nurse
reported a license in both of the States.
Table B-1. State Sampling Rates and
Sample Sizes (Priority Ordered)
|
|
Sampling
Rate Percentage |
|
State |
Priority
Order |
Frame
Size |
Planned |
Actual
[2]
|
Actual
Sample Size |
|
TOTAL |
|
3,252,548 |
|
|
56,917 |
|
Wyoming |
1 |
5,309 |
15.00% |
15.60% |
828 |
|
Alaska |
2 |
7,389 |
13.00% |
11.88% |
878 |
|
Vermont |
3 |
8,728 |
10.00% |
9.53% |
832 |
|
District of Columbia |
4 |
17,104 |
10.00% |
9.71% |
1,661 |
|
North Dakota |
5 |
8,139 |
9.00% |
9.74% |
793 |
|
Delaware |
6 |
10,407 |
9.00% |
8.87% |
923 |
|
Montana |
7 |
10,885 |
8.00% |
8.15% |
887 |
|
South Dakota |
8 |
10,773 |
7.00% |
6.88% |
741 |
|
Idaho |
9 |
12,769 |
7.00% |
6.75% |
862 |
|
Hawaii |
10 |
13,548 |
7.00% |
7.44% |
1,008 |
|
Nevada |
11 |
19,201 |
7.00% |
6.25% |
1,200 |
|
Rhode Island |
12 |
17,203 |
5.50% |
5.37% |
923 |
|
New Mexico |
13 |
17,544 |
5.00% |
4.98% |
874 |
|
New Hampshire |
14 |
19,108 |
5.00% |
4.71% |
900 |
|
Utah |
15 |
19,210 |
4.50% |
4.97% |
954 |
|
Maine |
16 |
19,869 |
4.50% |
4.50% |
894 |
|
Nebraska |
17 |
20,100 |
3.50% |
3.56% |
716 |
|
Arkansas |
18 |
27,878 |
3.50% |
3.52% |
982 |
|
West Virginia |
19 |
21,295 |
3.50% |
3.13% |
667 |
|
Mississippi |
20 |
31,734 |
3.00% |
3.13% |
994 |
|
Oklahoma |
21 |
32,185 |
3.00% |
2.93% |
944 |
|
Kansas |
22 |
34,047 |
3.00% |
3.10% |
1,057 |
|
Iowa |
23 |
40,312 |
2.50% |
2.31% |
933 |
|
South Carolina |
24 |
38,265 |
2.50% |
2.47% |
944 |
|
Oregon |
25 |
38,453 |
2.00% |
1.95% |
750 |
|
Louisiana |
26 |
43,299 |
2.00% |
1.75% |
757 |
|
Colorado |
27 |
48,586 |
2.00% |
2.14% |
1,042 |
|
Connecticut |
28 |
52,364 |
2.00% |
1.96% |
1,025 |
|
Alabama |
29 |
46,974 |
1.75% |
1.81% |
852 |
|
Kentucky |
30 |
47,123 |
1.75% |
1.77% |
832 |
|
Arizona |
31 |
51,482 |
1.75% |
1.72% |
887 |
|
Maryland |
32 |
56,922 |
1.50% |
1.47% |
835 |
|
Washington |
33 |
66,397 |
1.50% |
1.44% |
954 |
|
Minnesota |
34 |
66,434 |
1.50% |
1.59% |
1,056 |
|
Wisconsin |
35 |
63,865 |
1.25% |
1.24% |
793 |
|
Tennessee |
36 |
65,827 |
1.25% |
1.29% |
849 |
|
Indiana |
37 |
70,488 |
1.25% |
1.23% |
867 |
|
Missouri |
38 |
74,508 |
1.25% |
1.28% |
953 |
|
Georgia |
39 |
86,369 |
1.25% |
1.26% |
1,086 |
|
Virginia |
40 |
85,705 |
1.25% |
1.21% |
1,036 |
|
North Carolina |
41 |
96,877 |
1.125% |
1.146% |
1,110 |
|
Massachusetts |
42 |
105,206 |
1.125% |
1.350% |
1,420 |
|
New Jersey |
43 |
109,726 |
1.125% |
1.067% |
1,171 |
|
Michigan |
44 |
117,360 |
1.125% |
1.161% |
1,363 |
|
Ohio |
45 |
140,689 |
1.125% |
1.124% |
1,581 |
|
Illinois |
46 |
154,572 |
1.125% |
1.124% |
1,738 |
|
Texas |
47 |
176,652 |
1.125% |
1.066% |
1,883 |
|
Pennsylvania |
48 |
191,628 |
1.125% |
1.037% |
1,988 |
|
Florida |
49 |
201,113 |
1.125% |
1.086% |
2,184 |
|
New York |
50 |
244,288 |
1.125% |
1.061% |
2,592 |
|
California |
51 |
286,639 |
1.125% |
1.018% |
2,918 |
Weighting Procedures
The probability sample design of the
survey permits the computation of unbiased
estimates of characteristics of the RN
population at the National and State level.
These estimates are based on weights that
reflect the complex design and compensate
for the potential risk of nonresponse
bias to the extent feasible. The weights
that are assigned to each sample nurse
may be interpreted as the number of nurses
in the target population that the sample
nurse represents. The sampling weight
for an RN is the reciprocal of the nurse’s
probability of selection in her/his priority
State, adjusted to account for nonresponse
and multiple licenses.
Before computing the weights, the original
State frame sizes (shown above) were adjusted
to account for duplicate licenses within
States and ineligible licenses (i.e.,
frame errors) found in the sample. Most
within-State duplicates were identified
at the time of initial list processing,
but a few were identified after sample
selection. The ineligible licenses were
identified in the process of reconciling
the State and nurse reported licenses.
Some of the inconsistencies between the
State reported data and the nurse reported
data are due to the time period that elapsed
between frame construction and data collection
(a period during which changes and license
expirations naturally occur). Other differences
are due to errors in either the State
list or the nurse’s questionnaire. Cases
that could not be reconciled by Gallup
were sent to the State Boards of Nursing
for resolution.
In both cases, the frame total is computed
by subtracting the estimated number of
ineligible and duplicate licenses from
the State’s original frame count. The
adjusted frame total used to compute the
resulting weights for State i can
be computed as:

where:
Ni = the total number
of licenses on State i list,
 = the estimated
number of within-State duplicates in State
i,and = the estimated
number of within-State duplicates in State
i,and
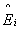 = the estimated
number of frame errors in State i (e.g.,
licenses listed by State that were not
reported by a responding nurse). = the estimated
number of frame errors in State i (e.g.,
licenses listed by State that were not
reported by a responding nurse).
Each responding nurse was assigned a
weight corresponding to their unique ‘priority
State’; that is, the State with the
highest sampling rate from which he or
she was licensed and selected into the
sample.In other words, the weight
is reflective of the probability of selecting
the sampled nurse in their “priority”
State. All nurses with the same priority
State have an equal probability of being
selected and, consequently, have equal
initial sampling weights. The sum of
the weights for all nurse respondents
assigned to a specific priority State
will equal, approximately, the total number
of active licenses on the list (at the
time the sample was drawn) less the number
of those licenses assigned to higher priority
lists.
The weights were computed sequentially
for each State A, B, etc., where A was
the highest-priority State, and B the
next-highest-priority State. The weight
for an RN sampled from the highest priority
State, State A, was the ratio of the adjusted
count of licenses in the sampling frame
for State A to the number of eligible
respondents licensed in State A. For
State B, and the remaining States, the
numerator and denominator of this ratio
were adjusted to account for State A and
other higher-priority States. To describe
the basic method, the following terms
are defined:
N(i) = total number of licenses
for State i (adjusted for within-State
duplicates and frame errors)
m(i) = number of eligible
respondents for State i that
did not have a license in a higher-priority
State
n(i,j) = number of eligible
respondents with a license in both State
i and State j [note n(i,i)
denotes the number of eligible respondents
with a license only in State i]
W(i) = the adjusted weight
for eligible respondents who were assigned
to the higher priority State i
The weight for State A was computed as
follows:
W(A) = N(A) / m(A).
For the State B weight, W(B), the numerator
was the adjusted frame count of licenses
for State B, N(B), after removing
the estimated total count of State B nurses
who were also licensed in State A (i.e.,
W(A) n(A,B)). Similarly, the numerator
of W(C) excluded State C nurses who were
also licensed in either State A or State
B (i.e., W(A) n(A,C) + W(B) n(B,C)).
That is, for the State B weight and the
State C weight, the computations were:
W(B) = [N(B) - W(A) n(A,B)] / m(B)
W(C) = [N(C) - W(A) n(A,C) - W(B) n(B,C)]
/ m(C) .
In either case, the denominator was the
number (m(B) or m(C)) of respondents in
the State not licensed in a higher-priority
State.
In general, the numerator of a State
I weight, W(I), was the total adjusted
frame count of RN licenses in State I
after removing the estimated total count
of State I nurses also licensed
in higher-priority States. The denominator,
m(I), was the number of State I respondents
not licensed in a higher-priority State.
This weighting scheme incorporated both
a nonresponse adjustment that inflated
the respondents’ data to account for those
that did not respond to the survey and
a duplication adjustment to account for
duplication in the sampling frame across
States. These final analysis weights
will serve to differentially weight responding
nurses to reflect the level of disproportionality
in the final respondent sample relative
to the population.
Estimation Procedure
Final NSSRN estimates can be computed
using the final set of sampling weights,
Wk (for sample nurse k).
For example, an estimate of the total
number of RNs working in a particular
State is based on the following indicator
variable, Xk:
Xk = 1 if nurse k worked in
a particular State,
= 0 otherwise.
The desired estimated total may then
be written as

the sum being over all sample nurses.
Estimates of ratios and averages are
obtained as the ratio of estimated totals.
Sampling and Nonsampling
Errors
To the extent that samples are sufficiently
large, relatively precise estimates of
characteristics of the licensed RN population
of the United States can be made because
of the underlying probability structure
of the sample data. Such estimates are,
sometimes, an imperfect approximation
of the truth. Several sources of error
could cause sample estimates to differ
from the corresponding true population
value. These sources of error are commonly
classified into two major categories:
sampling errors and nonsampling errors.
A probability sample such as the one
used in this study is designed so that
estimates of the magnitude of the sampling
error can be computed from the sample
data. In addition, nonsystematic components
of nonsampling error are also reflected
in the sampling error estimates.
Nonsampling Errors
Some sources of error, such as unusable
responses to vague or sensitive questions;
no responses from some nurses; and errors
in coding, scoring, and processing the
data are, to a considerable extent, beyond
the control of the sampling statistician.
They are called “nonsampling errors” and
also occur in cases where there is a complete
enumeration of a target population, such
as the U.S. Census. Among the activities
that were directed at reducing nonsampling
errors to the lowest level feasible for
this survey included careful planning,
keeping nonresponses to the lowest feasible
level, and coding and processing of the
sample data.
If nonsampling errors are random, in
the sense that they are independent and
tend to be compensating from one respondent
to another, then they do not cause bias
in estimates of totals, percents, or averages.
Furthermore, the contribution from such
nonsampling errors will automatically
be included in the sampling errors that
are estimated from the sample data. However,
correlations or relationships in cross-tabulations
are often decreased by such errors, and
sometimes substantially. Thus, random
errors that tend to be compensated for
in estimates of simple aggregates or averages
may (but not necessarily will) introduce
systematic errors or biases in measures
of relationships or cross-tabulations.
Nonsampling errors that are systematic
(rather than random and compensating)
are a source of bias for sample estimates.
Such errors are not reduced by increasing
the size of the sample, and the sample
data do not provide an assessment of the
magnitude of these errors. Systematic
errors are reduced in this study by such
efforts as careful wording of questionnaire
items, respondent motivation, and well-designed
data-collection and data-management procedures.
However, such errors sometimes occur in
subtle ways and are less subject to design
control than is the case for sampling
errors.
Nonresponse to the survey is one of the
largest sources of nonsampling error because
a characteristic being estimated may differ,
on average, between respondents and nonrespondents.
For this reason, considerable effort has
been expended in this survey to obtain
a high response rate by respondent motivation
and follow-up procedures. A high response
rate reduces both random and systematic
nonsampling errors. After taking into
account duplicates and frame errors, the
overall response rate to this survey was 70.47
percent. State-level response rates ranged
from 61.98 percent to 81.57 percent except
for the District of Columbia where the
response rate (46.12 percent) was significantly
lower.
Sampling Errors
All sample survey estimates are subject
to sampling error. The magnitude of the
sampling error for an estimate, as indicated
by measures of variability such as its
variance or its standard error (the square
root of its variance), provides a basis
for judging the precision of the sample
estimates.
Systematic sampling, which was the selection
procedure used in choosing the alpha-segments
for this study, is convenient from certain
practical points of view, including providing
for panel rotation. However, it does
not permit unbiased estimation of the
variability of survey estimates unless
some assumptions are made. Thus, standard
errors were estimated based upon the assumption
that the systematic sample of 40 alpha-segments
is equivalent to a stratified random sample
of two alpha-segments from each of 20
strata of adjacent alpha-segments. Ordinarily,
this assumption should lead to overestimates
of the sampling error for systematic sampling,
but in this case (with alpha-segments
as the sampling units) the magnitude of
the overestimate is believed to be trivial.
Regarding the sample as consisting of
20 pairs of alpha-segments (thus obtaining
20 degrees of freedom) for variance estimation,
the probability is approximately 0.95
that the statistic of interest differs
from the value of the population characteristic
that it estimates by not more than 2.086
standard deviations.
Specifically, a 95 percent confidence
interval for an estimated statistic
 takes the form: takes the form:

where 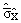 is the estimated
standard error for is the estimated
standard error for  . .
Direct Variance Estimation
Similar to prior cycles of the NSSRN,
direct estimates of sampling variance
were obtained for a set of important variables
for each State and for the United States
using the jackknife variance estimation
procedure with 20 replicates of the sample.
Variance estimates using the jackknife
approach require the computation of a
set of weights for the full sample and
a set for each replicate using the established
weight computation procedure (i.e., 20
additional sets of weights). Having 20
sets of weights permits construction of
20 replicate estimates to compare with
the estimate produced from all of the
data; each replicate estimate is based
on about 39/40ths of the data.
Each replicate was formed from 19 pairs
of alpha-segments (38 alpha-segments total)
and 1 alpha-segment from the 20th pair.
Alpha-segments were randomly removed from
each pair to form the replicate estimates.
This procedure was performed 20 times,
once for each pair of alpha-segments.
Thus, actual respondent count in the included
segments for a particular replicate was
approximately 39/40ths of the
full respondent sample and was weighted
to represent the full population.
The variance of  , Var , Var  , is estimated
by computing: , is estimated
by computing:

where:
 = an estimated
total for replicate i associated
with alpha-segment pair i, and = an estimated
total for replicate i associated
with alpha-segment pair i, and
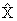 =
an estimated total obtained over the full
sample. =
an estimated total obtained over the full
sample.
If the estimate of interest is a ratio
of two estimated totals (e.g., the total
number of RNs resident in Florida between
25 and 29 years old to the total number
of RNs resident in Florida), the variance
estimate for the estimated ratio would
be of the following form:

Following the example, the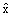 and and  measurements
would be full sample and replicate estimates,
respectively, of the number of RNs resident
in Florida who were 25 to 29 years old,
while measurements
would be full sample and replicate estimates,
respectively, of the number of RNs resident
in Florida who were 25 to 29 years old,
while  and and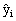 would be the
corresponding estimates of the total number
of RNs resident in Florida. The variance
of any other statistic, simple or complex,
can be similarly estimated by computing
the statistic for each replicate. would be the
corresponding estimates of the total number
of RNs resident in Florida. The variance
of any other statistic, simple or complex,
can be similarly estimated by computing
the statistic for each replicate.
The jackknife variance estimator can
use either the full sample estimate, 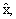 or the average
of the replicate estimates. While usually
little difference exists between the two
estimates, the estimator, or the average
of the replicate estimates. While usually
little difference exists between the two
estimates, the estimator, 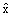 was used which
tends to provide more conservative estimates
of variance. was used which
tends to provide more conservative estimates
of variance.
Direct estimates of the variance were
computed for a variety of variables.
These variables were chosen not only due
to their importance, but also to represent
the range of expected design effects.
The average of these design effects (on
a State-by-State basis) provides the basis
for the variance estimate for variables
not included in the set for which direct
variance estimates were computed. Table
B-2 in Appendix B presents direct estimates
of the standard error (the square root
of the variance) for a selected set of
variables. Table B-3 in Appendix B shows
the estimated population of nurses in
each State and the standard error of these
population totals.
Design Effects and
Generalized Variances
The generalized variance is a model-based
approximation of the sampling variance
estimate, which is less computationally
complex than the direct variance estimator
but is also less accurate. The generalized
variance equations use the national-level
or State-level estimates of the design
effect and, for some estimates, the coefficient
of variation (CV) to estimate the sampling
variance. The design effect, F, for an
estimated proportion  is determined
by taking the ratio of the estimated sampling
variance, is determined
by taking the ratio of the estimated sampling
variance, obtained by
the jackknife method, to the sampling
variance of the obtained by
the jackknife method, to the sampling
variance of the  in a simple
random sample of the same size. This design
effect, F, can be computed as follows: in a simple
random sample of the same size. This design
effect, F, can be computed as follows:

where n is the unweighted number of respondents
used to determine the denominator of  . .
Direct estimates of the design effect
were computed for a set of variables for
each State. The median of the design
effects was then computed for each State
and the nation. These median design effects
can be used in formulas for estimating
generalized variances or standard errors.
This procedure uses median design effects
for a class of estimates instead of calculating
direct estimates (with a resulting economy
in time and costs), at the sacrifice generally
of some accuracy in the variance estimates.
A generalized standard error estimate
for an estimated proportion,  for a State
or for the United States, is provided
by the equation: for a State
or for the United States, is provided
by the equation:
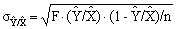 (1) (1)
where n is the number of survey respondents
used to determine the estimate 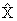 . The multiplier
F, the median² design effect,
depends upon the State for which the estimated
proportion was generated. The median
design effects are listed on Table B-4
in Appendix B. . The multiplier
F, the median² design effect,
depends upon the State for which the estimated
proportion was generated. The median
design effects are listed on Table B-4
in Appendix B.
Generalized estimates of standard errors
can also be computed for estimated
numbers (or totals) of RNs in a State
with a particular characteristic  (such as those
employed in hospitals). The estimate (such as those
employed in hospitals). The estimate
 is a subtotal
of the estimate is a subtotal
of the estimate  , the estimated
total of RNs working and/or living in
the State. Note that the standard error
and coefficient of variation of , the estimated
total of RNs working and/or living in
the State. Note that the standard error
and coefficient of variation of
 (represented
by (represented
by 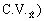 were determined
for the nation and for each State (see
Table B-3). were determined
for the nation and for each State (see
Table B-3).
To calculate the standard error of a
total, one must first compute the relative
variance (or square of the coefficient
of variation) of the ratio of 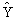 to to  (called (called
 . The relative
variance can be calculated as: . The relative
variance can be calculated as:

where F is the design effect for the
State of interest and n is the number
of respondents to the survey that were
weighted to obtain the estimate

Then, from the relative variance of the
ratio, one can approximate the relative
variance of the total  denoted denoted
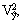 by using: by using:

This approximation is based on the first-order
Taylor series approximation to the variance
of a product and the assumption of zero
correlation between the estimate of ratio
and the denominator of the ratio.
Finally, the standard error of the total
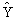 can be estimated
by multiplying the estimate by the square
root of the relative variance defined
above. The standard error of can be estimated
by multiplying the estimate by the square
root of the relative variance defined
above. The standard error of   is thus estimated
as: is thus estimated
as:
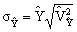 (2) (2)
The standard error of an estimated percentage
for a region of the United States depends
upon a linear combination of the variance
of the same estimated percentages for
the States making up that particular region.
The estimated proportion for the region
is:

Here, h is the number of States in region
R, and 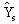 and and
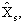 are estimates
for a particular State. The formula used
to approximate the standard error of an
estimated proportion for a region is: are estimates
for a particular State. The formula used
to approximate the standard error of an
estimated proportion for a region is:
 (3) (3)
where 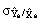 represents
the standard error of the estimated proportion represents
the standard error of the estimated proportion
 for the States
and the standard errors are estimated
from equation (1) or from direct estimation. for the States
and the standard errors are estimated
from equation (1) or from direct estimation.
The direct standard error for an estimated
number for a region of the United States
also depends upon a linear combination
of the variance of the same estimated
numbers for the States that make up the
region. The formula used is
 (4) (4)
where the standard error  of the estimated
number of the estimated
number 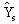 is available
either from the direct procedures or
from equation (2). is available
either from the direct procedures or
from equation (2).
Table B-2. Estimates and Standard
Errors (S.E.) For Selected Variables of
U.S. Registered Nurse Population
|
Description |
Estimated
Number |
S.E.
of Estimated Number |
Estimated
Percent |
S.E.
of Estimated Percent |
|
UNITED STATES, Total Number Of
Nurses |
2,909,357 |
7,000 |
|
|
|
|
|
Basic Nursing Education |
|
|
|
|
|
Diploma Program |
733,377 |
9,749 |
25.21 |
0.32 |
|
Associate Degree |
1,227,256 |
16,571 |
42.18 |
0.54 |
|
Baccalaureate Degree |
887,114 |
13,366 |
30.49 |
0.47 |
|
Master’s Degree |
14,979 |
1,412 |
0.51 |
0.05 |
|
Doctorate |
532 |
271 |
0.02 |
0.01 |
|
Not Reported |
46,098 |
2,568 |
1.58 |
0.09 |
|
|
|
Employed in Nursing |
|
|
|
|
|
Yes |
2,421,351 |
10,124 |
83.23 |
0.27 |
|
No |
488,006 |
7,792 |
16.77 |
0.27 |
|
|
|
Racial/Ethnic Background |
|
|
|
|
|
White (non-hispanic) |
2,380,529 |
28,004 |
81.82 |
0.89 |
|
Black/African American (non-hispanic) |
122,495 |
16,737 |
4.21 |
0.57 |
|
Asian (non-hispanic) |
84,383 |
15,540 |
2.90 |
0.54 |
|
American Indian/Alaskan Native
(non-hispanic) |
9,453 |
972 |
0.32 |
0.03 |
|
Native Hawaiian/Pacific Islander
(non-hispanic) |
5,594 |
1,091 |
0.19 |
0.04 |
|
Two or more races (non-hispanic) |
41,244 |
2,641 |
1.42 |
0.09 |
|
Hispanic/Latino (White) |
38,530 |
7,745 |
1.32 |
0.27 |
|
Hispanic/Latino (Black/African
American) |
2,924 |
633 |
0.10 |
0.02 |
|
Hispanic/Latino (Two or more races) |
3,096 |
741 |
0.11 |
0.03 |
|
Hispanic, Other |
3,460 |
921 |
0.12 |
0.03 |
|
Not Reported |
217,651 |
5,689 |
7.48 |
0.19 |
|
|
|
Employment Status in 2004 |
|
|
|
|
|
Employed In Nursing Full Time |
1,696,807 |
12,210 |
58.32 |
0.44 |
|
Employed In Nursing Part Time |
720,283 |
11,059 |
24.76 |
0.35 |
|
Employed In Nursing, Full/Part
Time Unknown |
4,261 |
523 |
0.15 |
0.02 |
|
Not Employed In Nursing |
488,006 |
7,793 |
16.77 |
0.27 |
|
|
|
Graduation Year |
|
|
|
|
|
Before 1961 |
150,147 |
4,332 |
5.16 |
0.15 |
|
1961 To 1965 |
146,805 |
4,047 |
5.05 |
0.14 |
|
1966 To 1970 |
203,313 |
4,150 |
6.99 |
0.14 |
|
1971 To 1975 |
300,072 |
7,685 |
10.31 |
0.26 |
|
1976 To 1980 |
378,607 |
7,543 |
13.01 |
0.25 |
|
1981 To 1985 |
385,145 |
7,064 |
13.24 |
0.24 |
|
1986 To 1990 |
321,070 |
6,472 |
11.04 |
0.22 |
|
1991 To 1995 |
406,125 |
5,902 |
13.96 |
0.22 |
|
1996 To 2000 |
367,557 |
6,094 |
12.63 |
0.20 |
|
After 2000 |
196,086 |
5,069 |
6.74 |
0.17 |
|
Not Reported |
54,430 |
2,524 |
1.87 |
0.09 |
|
|
|
Employment Setting |
|
|
|
|
|
Hospital |
1,360,847 |
13,063 |
46.77 |
0.43 |
|
Nursing Home Extended Care |
153,172 |
3,369 |
5.26 |
0.12 |
|
Nursing Education |
63,444 |
2,879 |
2.18 |
0.10 |
|
Public Health/Community Health |
259,911 |
4,347 |
8.93 |
0.15 |
|
School Health Service |
78,022 |
3,095 |
2.68 |
0.10 |
|
Occupational Health |
22,447 |
1,820 |
0.77 |
0.06 |
|
Ambulatory Care (Except Nurse Owned/Operated) |
265,273 |
5,346 |
9.12 |
0.18 |
|
Nurse Owned/Operated Ambulatory
Care Setting |
12,500 |
1,112 |
0.43 |
0.04 |
|
Insurance Claims/Benefits |
43,641 |
1,976 |
1.50 |
0.07 |
|
Planning/ Regul /Licensing Agency |
8,733 |
933 |
0.30 |
0.03 |
|
Other |
103,310 |
3,974 |
3.55 |
0.13 |
|
Not Reported |
538,058 |
8,227 |
18.49 |
0.29 |
|
|
|
Type of Position |
|
|
|
|
|
Administrator Or Assistant Administrator |
125,011 |
2,522 |
4.30 |
0.08 |
|
Consultant |
35,617 |
1,707 |
1.22 |
0.06 |
|
Supervisor |
74,201 |
2,976 |
2.55 |
0.10 |
|
Instructor/Faculty |
62,255 |
2,403 |
2.14 |
0.08 |
|
Head Nurse Or Assistant Nurse |
148,210 |
3,880 |
5.09 |
0.13 |
|
Staff Nurse |
1,431,053 |
11,735 |
49.19 |
0.39 |
|
Nurse Practitioner |
84,042 |
3,424 |
2.89 |
0.12 |
|
Nurse Midwife |
7,274 |
990 |
0.25 |
0.03 |
|
Clinical Specialist |
28,623 |
1,900 |
0.98 |
0.07 |
|
Nurse Clinician |
32,954 |
1,908 |
1.13 |
0.07 |
|
Certified Nurse Anesthetist |
27,287 |
1,452 |
0.94 |
0.05 |
|
Research |
19,263 |
1,250 |
0.66 |
0.04 |
|
Private Duty |
11,762 |
1,280 |
0.40 |
0.04 |
|
Informatic Nurse |
8,570 |
929 |
0.29 |
0.03 |
|
Home Health |
45,621 |
1,834 |
1.57 |
0.06 |
|
Survey Or Auditors/Regulator |
12,097 |
1,031 |
0.42 |
0.04 |
|
Patient Coordinator |
138,404 |
3,205 |
4.76 |
0.11 |
|
Other |
82,352 |
3,226 |
2.83 |
0.11 |
|
Not Reported |
534,760 |
7,774 |
18.38 |
0.27 |
|
|
|
Highest Nursing Education |
|
|
|
|
|
Diploma In Nursing |
510,209 |
8,062 |
17.54 |
0.27 |
|
Associate Degree In Nursing Or
Related Field |
981,238 |
14,852 |
33.73 |
0.49 |
|
Baccalaureate In Nursing |
922,696 |
12,963 |
31.71 |
0.45 |
|
Baccalaureate In Related Field |
71,580 |
1,946 |
2.46 |
0.07 |
|
Masters In Nursing |
256,415 |
5,251 |
8.81 |
0.18 |
|
Masters In Related Field |
94,386 |
3,057 |
3.24 |
0.10 |
|
Doctorate In Nursing |
11,548 |
645 |
0.40 |
0.02 |
|
Doctorate In Related Field |
14,552 |
1,192 |
0.50 |
0.04 |
|
Not Reported |
46,733 |
2,300 |
1.61 |
0.08 |
|
|
|
Age of Nurse |
|
|
|
|
|
<25 |
61,778 |
1,486 |
2.12 |
0.05 |
|
25 To 29 |
171,659 |
3,751 |
5.90 |
0.13 |
|
30 To 34 |
243,182 |
5,572 |
8.36 |
0.19 |
|
35 To 39 |
289,525 |
6,598 |
9.95 |
0.23 |
|
40 To 44 |
408,248 |
6,721 |
14.03 |
0.23 |
|
45 To 49 |
508,708 |
7,695 |
17.49 |
0.26 |
|
50 To 54 |
463,565 |
9,646 |
15.93 |
0.32 |
|
55 To 59 |
338,078 |
6,534 |
11.62 |
0.22 |
|
60 To 64 |
210,196 |
5,764 |
7.22 |
0.20 |
|
65+ |
185,254 |
5,092 |
6.37 |
0.17 |
|
Not Reported |
29,165 |
1,525 |
1.00 |
0.05 |
|
|
|
Marital Status and Children
|
|
|
|
|
|
Married, Children < 6 |
225,572 |
5,474 |
7.75 |
0.19 |
|
Married, Children > = 6 |
650,793 |
8,062 |
22.37 |
0.28 |
|
Married, Children All Ages |
162,791 |
3,393 |
5.60 |
0.11 |
|
Married, No Children |
994,588 |
10,942 |
34.19 |
0.34 |
|
Married, Children Unknown |
16,916 |
1,275 |
0.58 |
0.04 |
|
Widowed/ Separated/ Divorced, Children
< 6 |
13,300 |
1,023 |
0.46 |
0.04 |
|
Widowed/ Separated/ Divorced, Children
> = 6 |
137,283 |
4,514 |
4.72 |
0.15 |
|
Widowed/ Separated/ Divorced, Children
All Ages |
14,683 |
898 |
0.50 |
0.03 |
|
Widowed/ Separated/ Divorced, No
Children |
355,309 |
8,582 |
12.21 |
0.29 |
|
Widowed/ Separated/ Divorced, Children
Unknown |
5,795 |
817 |
0.20 |
0.03 |
|
Never Married, Children < 6 |
9,131 |
1,063 |
0.31 |
0.04 |
|
Never Married, Children > =
6 |
18,657 |
1,606 |
0.64 |
0.06 |
|
Never Married, Children All Ages |
2,854 |
609 |
0.10 |
0.02 |
|
Never Married, No Children |
234,208 |
5,167 |
8.05 |
0.18 |
|
Never Married, Children Unknown |
3,897 |
680 |
0.13 |
0.02 |
|
Not Reported |
63,581 |
2,497 |
2.19 |
0.09 |
|
|
|
Mean Gross Annual Salary for
Full-Time RNs |
57,784.86 |
180.85 |
|
|
|
|
|
Mean Hours Worked per year |
2,160.00 |
5.63 |
|
|
|
|
|
Mean Hours Worked in Last Full
Workweek |
38.55 |
0.13 |
|
|
Table B-3. Direct Estimates of State
Nurse Population, Standard Error,
and Coefficient of Variation by State,
2000
| State |
2004
Estimated State Nurse
Population |
Standard Error |
Coefficient of Variation
(in Percent) |
|
United States |
2,909,357 |
7,001 |
0.24 |
|
Alabama |
42,894 |
472 |
1.10 |
|
Alaska |
7,567 |
420 |
5.54 |
|
Arizona |
48,284 |
910 |
1.89 |
|
Arkansas |
23,818 |
569 |
2.39 |
|
California |
255,858 |
1,734 |
0.68 |
|
Colorado |
43,719 |
695 |
1.59 |
|
Connecticut |
42,894 |
1,199 |
2.80 |
|
DC |
9,352 |
324 |
3.47 |
|
Delaware |
12,118 |
675 |
5.57 |
|
Florida |
169,460 |
2,168 |
1.28 |
|
Georgia |
78,898 |
1,070 |
1.36 |
|
Hawaii |
11,146 |
387 |
3.47 |
|
Idaho |
11,068 |
256 |
2.32 |
|
Illinois |
138,092 |
1,236 |
0.90 |
|
Indiana |
64,396 |
858 |
1.33 |
|
Iowa |
37,777 |
614 |
1.63 |
|
Kansas |
29,892 |
790 |
2.64 |
|
Kentucky |
42,971 |
812 |
1.89 |
|
Louisiana |
39,449 |
731 |
1.85 |
|
Maine |
17,785 |
465 |
2.61 |
|
Maryland |
53,061 |
759 |
1.43 |
|
Massachusetts |
89,358 |
972 |
1.09 |
|
Michigan |
103,697 |
1,406 |
1.36 |
|
Minnesota |
60,214 |
621 |
1.03 |
|
Mississippi |
27,303 |
517 |
1.89 |
|
Missouri |
66,551 |
973 |
1.46 |
|
Montana |
9,416 |
149 |
1.58 |
|
Nebraska |
20,026 |
604 |
3.01 |
|
Nevada |
16,206 |
427 |
2.63 |
|
New Hampshire |
18,473 |
493 |
2.67 |
|
New Jersey |
92,425 |
1,476 |
1.60 |
|
New Mexico |
15,027 |
435 |
2.89 |
|
New York |
215,309 |
2,377 |
1.10 |
|
North Carolina |
92,391 |
1,238 |
1.34 |
|
North Dakota |
7,966 |
206 |
2.58 |
|
Ohio |
133,064 |
1,224 |
0.92 |
|
Oklahoma |
29,268 |
574 |
1.96 |
|
Oregon |
34,946 |
713 |
2.04 |
|
Pennsylvania |
164,433 |
1,834 |
1.12 |
|
Rhode Island |
13,847 |
337 |
2.44 |
|
South Carolina |
35,204 |
741 |
2.11 |
|
South Dakota |
10,223 |
213 |
2.09 |
|
Tennessee |
62,266 |
989 |
1.59 |
|
Texas |
168,368 |
1,363 |
0.81 |
|
Utah |
18,169 |
413 |
2.27 |
|
Vermont |
7,137 |
254 |
3.56 |
|
Virginia |
73,526 |
1,361 |
1.85 |
|
Washington |
59,761 |
913 |
1.53 |
|
West Virginia |
17,742 |
452 |
2.55 |
|
Wisconsin |
62,044 |
640 |
1.03 |
|
Wyoming |
4,498 |
122 |
2.72 |
Table B-4. Median Design Effects
for Percentages Estimated from
the Eighth National Sample Survey of
Registered Nurses, 2004
|
State |
Median
Design Effect |
|
United States |
1.63 |
|
Alabama |
1.06 |
|
Alaska |
1.24 |
|
Arizona |
1.01 |
|
Arkansas |
0.98 |
|
California |
1.11 |
|
Colorado |
1.04 |
|
Connecticut |
1.05 |
|
Delaware |
0.97 |
|
DC |
1.33 |
|
Florida |
1.08 |
|
Georgia |
1.03 |
|
Hawaii |
0.99 |
|
Idaho |
0.98 |
|
Illinois |
1.01 |
|
Indiana |
1.02 |
|
Iowa |
1.10 |
|
Kansas |
0.98 |
|
Kentucky |
1.08 |
|
Louisiana |
1.04 |
|
Maine |
1.04 |
|
Maryland |
1.16 |
|
Massachusetts |
1.02 |
|
Michigan |
0.95 |
|
Minnesota |
1.01 |
|
Mississippi |
1.01 |
|
Missouri |
1.05 |
|
Montana |
0.99 |
|
Nebraska |
0.99 |
|
Nevada |
1.07 |
|
New Hampshire |
1.09 |
|
New Jersey |
1.00 |
|
New Mexico |
1.04 |
|
New York |
1.04 |
|
North Carolina |
1.01 |
|
North Dakota |
0.97 |
|
Ohio |
1.05 |
|
Oklahoma |
1.02 |
|
Oregon |
1.03 |
|
Pennsylvania |
0.98 |
|
Rhode Island |
1.00 |
|
South Carolina |
1.03 |
|
South Dakota |
1.06 |
|
Tennessee |
0.98 |
|
Texas |
1.04 |
|
Utah |
1.02 |
|
Vermont |
0.98 |
|
Virginia |
1.13 |
|
Washington |
1.07 |
|
West Virginia |
0.93 |
|
Wisconsin |
1.07 |
|
Wyoming |
0.95 |
[1] Chromy,
James R. “Design Optimization with Multiple
Objectives”. American Statistical Association
of the Section on Survey Research Methods,
Arlington, VA., pp A4-199
[2] Since
the actual distribution of names differs
for each State from the frame distribution
used to develop the 250 alpha-segments,
some variation occurs between the planned
and actual sampling rates.
²The median
design effect was based on all design
effects for estimates of proportions computed
on selected variables. Using a median
instead of mean value avoids the effects
of extreme estimates of standard errors,
which can occur for some relatively rare
attributes. In prior years, an average
(mean) design effect was computed for
selected variables. Given that the distribution
of design effects is skewed to the right,
it is expected that the true median be
less than the true mean.
|