| Ambient Particulate Air Pollution, Heart Rate Variability, and Blood Markers of Inflammation in a Panel of Elderly Subjects C. Arden Pope III,1 Matthew L. Hansen,1,2 Russell W. Long,3,4 Karen R. Nielsen,5 Norman L. Eatough,3 William E. Wilson,6 and Delbert J. Eatough3 1Department of Economics, Brigham Young University, Provo, Utah, USA; 2Case Western Reserve University School of Medicine, Cleveland, Ohio, USA; 3Department of Chemistry and Biochemistry, Brigham Young University, Provo, Utah, USA; 4Human Exposure and Atmospheric Sciences, U.S. Environmental Protection Agency, Research Triangle Park, North Carolina, USA; 5Department of Radiation Oncology, University of Utah School of Medicine, Salt Lake City, Utah, USA; 6Office of Environmental Information, U.S. Environmental Protection Agency, Research Triangle Park, North Carolina, USA Abstract
Epidemiologic studies report associations between particulate air pollution and cardiopulmonary morbidity and mortality. Although the underlying pathophysiologic mechanisms remain unclear, it has been hypothesized that altered autonomic function and pulmonary/systemic inflammation may play a role. In this study we explored the effects of air pollution on autonomic function measured by changes in heart rate variability (HRV) and blood markers of inflammation in a panel of 88 elderly subjects from three communities along the Wasatch Front in Utah. Subjects participated in multiple sessions of 24-hr ambulatory electrocardiographic monitoring and blood tests. Regression analysis was used to evaluate associations between fine particulate matter [aerodynamic diameter 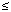 2.5 µm (PM2.5) ] and HRV, C-reactive protein (CRP) , blood cell counts, and whole blood viscosity. A 100-µg/m3 increase in PM2.5 was associated with approximately a 35 (SE = 8) -msec decline in standard deviation of all normal R-R intervals (SDNN, a measure of overall HRV) ; a 42 (SE = 11) -msec decline in square root of the mean of the squared differences between adjacent normal R-R intervals (r-MSSD, an estimate of short-term components of HRV) ; and a 0.81 (SE = 0.17) -mg/dL increase in CRP. The PM2.5-HRV associations were reasonably consistent and statistically robust, but the CRP association dropped to 0.19 (SE = 0.10) after excluding the most influential subject. PM2.5 was not significantly associated with white or red blood cell counts, platelets, or whole-blood viscosity. Most short-term variability in temporal deviations of HRV and CRP was not explained by PM2.5 ; however, the small statistically significant associations that were observed suggest that exposure to PM2.5 may be one of multiple factors that influence HRV and CRP. Key words: cardiovascular disease, C-reactive protein, ECG monitoring, heart rate variability, inflammation, particulate air pollution, PM2.5. Environ Health Perspect 112:339-345 (2004) . doi:10.1289/ehp.6588 available via http://dx.doi.org/ [Online 12 November 2003] 2.5 µm (PM2.5) ] and HRV, C-reactive protein (CRP) , blood cell counts, and whole blood viscosity. A 100-µg/m3 increase in PM2.5 was associated with approximately a 35 (SE = 8) -msec decline in standard deviation of all normal R-R intervals (SDNN, a measure of overall HRV) ; a 42 (SE = 11) -msec decline in square root of the mean of the squared differences between adjacent normal R-R intervals (r-MSSD, an estimate of short-term components of HRV) ; and a 0.81 (SE = 0.17) -mg/dL increase in CRP. The PM2.5-HRV associations were reasonably consistent and statistically robust, but the CRP association dropped to 0.19 (SE = 0.10) after excluding the most influential subject. PM2.5 was not significantly associated with white or red blood cell counts, platelets, or whole-blood viscosity. Most short-term variability in temporal deviations of HRV and CRP was not explained by PM2.5 ; however, the small statistically significant associations that were observed suggest that exposure to PM2.5 may be one of multiple factors that influence HRV and CRP. Key words: cardiovascular disease, C-reactive protein, ECG monitoring, heart rate variability, inflammation, particulate air pollution, PM2.5. Environ Health Perspect 112:339-345 (2004) . doi:10.1289/ehp.6588 available via http://dx.doi.org/ [Online 12 November 2003]
Address correspondence to C.A. Pope III, 142 FOB, Brigham Young University, Provo, UT 84602 USA. Telephone: (801) 422-2157. Fax: (801) 422-0194. E-mail: cap3@email.byu.edu The U.S. Environmental Protection Agency (U.S. EPA) through its Office of Research and Development partially funded and collaborated in the research described here under IMPACT Cooperative Agreement CR827364 and STAR grant R82799301 with Brigham Young University. However, the views expressed in this article are those of the authors and do not necessarily reflect the views or policies of the U.S. EPA. Mention of trade names or commercial products does not constitute U.S. EPA endorsement or recommendation for use. The authors declare they have no competing financial interests. Received 11 July 2003 ; accepted 12 November 2003.
The full version of this article is available for free in HTML or PDF formats. |

