Stem Cell Basics
- Introduction
- What are the unique properties of all stem cells?
- What are embryonic stem cells?
- What are adult stem cells?
- What are the similarities and differences between embryonic and adult stem cells?
- What are the potential uses of human stem cells and the obstacles that must be overcome before these potential uses will be realized?
- Where can I get more information?
III. What are embryonic stem cells?
A. What stages of early embryonic development are important for generating embryonic stem cells?
Embryonic stem cells, as their name suggests, are derived from embryos. Specifically, embryonic stem cells are derived from embryos that develop from eggs that have been fertilized in vitro—in an in vitro fertilization clinic—and then donated for research purposes with informed consent of the donors. They are not derived from eggs fertilized in a woman's body. The embryos from which human embryonic stem cells are derived are typically four or five days old and are a hollow microscopic ball of cells called the blastocyst. The blastocyst includes three structures: the trophoblast, which is the layer of cells that surrounds the blastocyst; the blastocoel, which is the hollow cavity inside the blastocyst; and the inner cell mass, which is a group of approximately 30 cells at one end of the blastocoel.
B. How are embryonic stem cells grown in the laboratory?
Growing cells in the laboratory is known as cell culture. Human embryonic stem cells are isolated by transferring the inner cell mass into a plastic laboratory culture dish that contains a nutrient broth known as culture medium. The cells divide and spread over the surface of the dish. The inner surface of the culture dish is typically coated with mouse embryonic skin cells that have been treated so they will not divide. This coating layer of cells is called a feeder layer. The reason for having the mouse cells in the bottom of the culture dish is to give the inner cell mass cells a sticky surface to which they can attach. Also, the feeder cells release nutrients into the culture medium. Recently, scientists have begun to devise ways of growing embryonic stem cells without the mouse feeder cells. This is a significant scientific advancement because of the risk that viruses or other macromolecules in the mouse cells may be transmitted to the human cells.
Over the course of several days, the cells of the inner cell mass proliferate and begin to crowd the culture dish. When this occurs, they are removed gently and plated into several fresh culture dishes. The process of replating the cells is repeated many times and for many months, and is called subculturing. Each cycle of subculturing the cells is referred to as a passage. After six months or more, the original 30 cells of the inner cell mass yield millions of embryonic stem cells. Embryonic stem cells that have proliferated in cell culture for six or more months without differentiating, are pluripotent, and appear genetically normal are referred to as an embryonic stem cell line.
Once cell lines are established, or even before that stage, batches of them can be frozen and shipped to other laboratories for further culture and experimentation.
C. What laboratory tests are used to identify embryonic stem cells?
At various points during the process of generating embryonic stem cell lines, scientists test the cells to see whether they exhibit the fundamental properties that make them embryonic stem cells. This process is called characterization.
As yet, scientists who study human embryonic stem cells have not agreed on a standard battery of tests that measure the cells' fundamental properties. Also, scientists acknowledge that many of the tests they do use may not be good indicators of the cells' most important biological properties and functions. Nevertheless, laboratories that grow human embryonic stem cell lines use several kinds of tests. These tests include:
- growing and subculturing the stem cells for many months. This ensures that the cells are capable of long-term self-renewal. Scientists inspect the cultures through a microscope to see that the cells look healthy and remain undifferentiated.
- using specific techniques to determine the presence of surface markers that are found only on undifferentiated cells. Another important test is for the presence of a protein called Oct-4, which undifferentiated cells typically make. Oct-4 is a transcription factor, meaning that it helps turn genes on and off at the right time, which is an important part of the processes of cell differentiation and embryonic development.
- examining the chromosomes under a microscope. This is a method to assess whether the chromosomes are damaged or if the number of chromosomes has changed. It does not detect genetic mutations in the cells.
- determining whether the cells can be subcultured after freezing, thawing, and replating.
- testing whether the human embryonic stem cells are pluripotent by 1) allowing the cells to differentiate spontaneously in cell culture; 2) manipulating the cells so they will differentiate to form specific cell types; or 3) injecting the cells into an immunosuppressed mouse to test for the formation of a benign tumor called a teratoma. Teratomas typically contain a mixture of many differentiated or partly differentiated cell types—an indication that the embryonic stem cells are capable of differentiating into multiple cell types.
D. How are embryonic stem cells stimulated to differentiate?
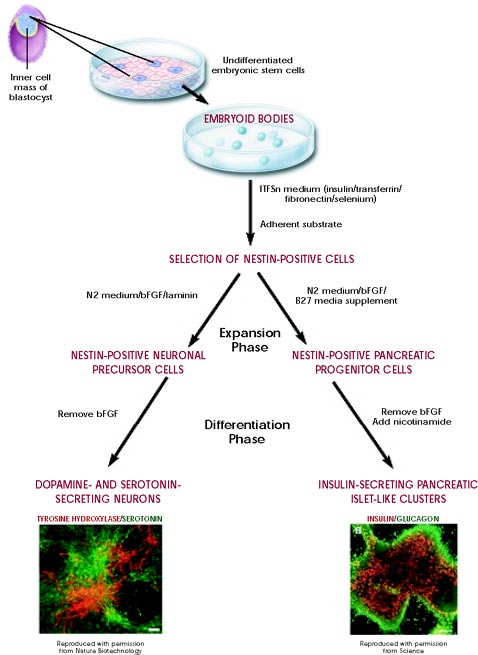
Figure 1. Directed differentiation of mouse embryonic stem cells. Click here for larger image.
As long as the embryonic stem cells in culture are grown under certain conditions, they can remain undifferentiated (unspecialized). But if cells are allowed to clump together to form embryoid bodies, they begin to differentiate spontaneously. They can form muscle cells, nerve cells, and many other cell types. Although spontaneous differentiation is a good indication that a culture of embryonic stem cells is healthy, it is not an efficient way to produce cultures of specific cell types.
So, to generate cultures of specific types of differentiated cells—heart muscle cells, blood cells, or nerve cells, for example—scientists try to control the differentiation of embryonic stem cells. They change the chemical composition of the culture medium, alter the surface of the culture dish, or modify the cells by inserting specific genes. Through years of experimentation scientists have established some basic protocols or "recipes" for the directed differentiation of embryonic stem cells into some specific cell types (Figure 1). (For more examples of directed differentiation of embryonic stem cells, see Chapters 5–9 and Appendices B and C of the NIH report Stem Cells: Scientific Progress and Future Research Directions.)
If scientists can reliably direct the differentiation of embryonic stem cells into specific cell types, they may be able to use the resulting, differentiated cells to treat certain diseases at some point in the future. Diseases that might be treated by transplanting cells generated from human embryonic stem cells include Parkinson's disease, diabetes, traumatic spinal cord injury, Purkinje cell degeneration, Duchenne's muscular dystrophy, heart disease, and vision and hearing loss.
 Previous | III. What are embryonic stem cells? | Next
Previous | III. What are embryonic stem cells? | Next 