 
Pregnancy and Thyroid Disease
On this page:
What is thyroid disease?
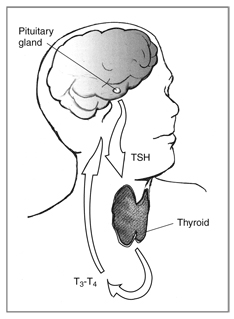
The thyroid gland’s production of thyroid hormones (T3 and T4) is triggered by thyroid-stimulating hormone (TSH), which is made by the pituitary gland.
Thyroid disease is a disorder that results when the thyroid gland produces more or less thyroid hormone than the body needs. Too much thyroid hormone is called hyperthyroidism and can cause many of the body’s functions to speed up. Too little thyroid hormone is called hypothyroidism, in which many of the body’s functions slow down.
[Top]
What is the thyroid?
The thyroid is a small butterfly-shaped gland in the front of the neck below the larynx, or voice box. The thyroid gland makes two thyroid hormones, triiodothyronine (T3) and, in much greater quantities, thyroxine (T4). Thyroid hormones affect metabolism, brain development, breathing, heart and nervous system functions, blood cell formation, body temperature, muscle strength, bone health, skin dryness, menstrual cycles, weight, and cholesterol levels.
Thyroid hormone production is regulated by another hormone called thyroid-stimulating hormone (TSH). TSH is made by the pituitary gland, a pea-sized gland located in the brain.
[Top]
How does pregnancy normally affect thyroid function?
Two pregnancy-related hormones—human chorionic gonadotropin (hCG) and estrogen—cause increased thyroid hormone levels in the blood. Made by the placenta, hCG is similar to TSH and mildly stimulates the thyroid to produce more thyroid hormone. Increased estrogen produces higher levels of thyroid-binding globulin, a protein that transports thyroid hormone in the blood. These normal hormonal changes can sometimes make thyroid function tests during pregnancy difficult to interpret.
Thyroid hormone is critical to normal development of the baby’s brain and nervous system. During the first trimester, the fetus depends on the mother’s supply of thyroid hormone, which it gets through the placenta. At 10 to 12 weeks, the baby’s thyroid begins to function on its own. The baby gets its supply of iodine, which the thyroid gland uses to make thyroid hormone, through the mother’s diet.
Women need more iodine when they are pregnant—about 250 micrograms (μg) a day. In the United States, about 7 percent of pregnant women may not get enough iodine in their diet or through prenatal vitamins.1 Choosing iodized salt—salt supplemented with iodine—over plain salt is one way to ensure adequate intake.
The thyroid gland enlarges slightly in healthy women during pregnancy, but not enough to be detected by a physical exam. A noticeably enlarged gland can be a sign of thyroid disease and should be evaluated. Higher levels of thyroid hormone in the blood, increased thyroid size, and other symptoms common to both pregnancy and thyroid disorders—such as fatigue—can make thyroid problems hard to diagnose in pregnancy.
1Pearce EN. National trends in iodine nutrition: Is everyone getting enough? Thyroid. 2007;17(9):823–827.
[Top]
Hyperthyroidism
What causes hyperthyroidism in pregnancy?
Hyperthyroidism in pregnancy is usually caused by Graves’ disease and occurs in about one of every 500 pregnancies.2 Graves’ disease is an autoimmune disorder, which means the body’s immune system makes antibodies that act against its own healthy cells and tissues. In Graves’ disease, the immune system makes an antibody called thyroid stimulating immunoglobulin, sometimes called TSH receptor antibody, which mimics TSH and causes the thyroid to make too much thyroid hormone.
Although Graves’ disease may first appear during pregnancy, a woman with preexisting Graves’ disease could actually see an improvement in her symptoms in her second and third trimesters. Remission of Graves’ disease in later pregnancy may result from the general suppression of the immune system that occurs during pregnancy. The disease usually worsens again in the first few months after delivery.
Rarely, hyperthyroidism in pregnancy is caused by hyperemesis gravidarum—severe nausea and vomiting that can lead to weight loss and dehydration. This extreme nausea and vomiting is believed to be triggered by high levels of hCG, which can also lead to temporary hyperthyroidism that usually resolves by the second half of pregnancy.
How does hyperthyroidism affect the mother and baby?
Uncontrolled hyperthyroidism during pregnancy can lead to
- congestive heart failure
- preeclampsia—a dangerous rise in blood pressure in late pregnancy
- thyroid storm—a sudden, severe worsening of symptoms
- miscarriage
- premature birth
- low birthweight
If a woman has Graves’ disease or was treated for Graves’ disease in the past, the thyroid-stimulating antibodies she produces may travel across the placenta to the baby’s bloodstream and stimulate the fetal thyroid. If the mother is being treated with antithyroid drugs, hyperthyroidism in the baby is less likely because these drugs also cross the placenta. But if she was treated for Graves’ disease with surgery or radioactive iodine, both of which destroy all or part of the thyroid, she can still have antibodies in her blood even though her thyroid levels are normal. Women who received either of these treatments for Graves’ disease should inform their doctor so the baby can be monitored for thyroid-related problems later in the pregnancy.
Hyperthyroidism in a newborn can result in rapid heart rate that can lead to heart failure, poor weight gain, irritability, and sometimes an enlarged thyroid that can press against the windpipe and interfere with breathing. Women with Graves’ disease
and their newborns should be closely monitored by their health care team.
How is hyperthyroidism in pregnancy diagnosed?
Hyperthyroidism is diagnosed through a careful review of symptoms, as well as blood tests to measure TSH, T4, and T3 levels.
Some symptoms of hyperthyroidism are common features in normal pregnancies, including increased heart rate, heat intolerance, and fatigue. Other symptoms are more indicative of hyperthyroidism: rapid and irregular heartbeat, a fine tremor, unexplained weight loss or failure to have normal pregnancy weight gain, and the severe nausea and vomiting associated with hyperemesis gravidarum.
If a woman’s symptoms suggest hyperthyroidism, her doctor will probably first perform the ultrasensitive TSH test. This test detects even tiny amounts of TSH in the blood and is the most accurate measure of thyroid activity available. Generally,
below-normal levels of TSH indicate hyperthyroidism. Low TSH levels may also occur in a normal pregnancy, however, especially in the first trimester. If TSH levels are low, another blood test is performed to measure T4 and T3.
Elevated levels of free T4—the portion of thyroid hormone not attached to thyroid-binding proteins—confirm the diagnosis. Rarely, free T4 levels are normal in a woman with hyperthyroidism but T3 levels are high. Because of normal pregnancy-related changes in thyroid function, test results must be interpreted with caution.
If a woman has Graves’ disease or has had surgery or radioactive iodine treatment for the disease, her doctor may also test her blood for the presence of thyroid-stimulating antibodies.
How is hyperthyroidism treated during pregnancy?
Mild hyperthyroidism in which TSH is low but free T4 is normal does not require treatment. More severe hyperthyroidism is treated with propylthiouracil or sometimes methimazole (Tapazole), drugs that interfere with thyroid hormone production. Antithyroid drugs cross the placenta in small amounts and can decrease fetal thyroid hormone production, so the lowest possible dose should be used to avoid hypothyroidism in the baby.
Rarely, surgery to remove all or part of the thyroid gland is considered for women who cannot tolerate propylthiouracil or methimazole. Radioactive iodine treatment is not an option for pregnant women because it can damage the fetal thyroid gland.
2Casey BM, Leveno KJ. Thyroid disease in pregnancy. Obstetrics & Gynecology. 2006;108(5):1283–1292.
[Top]
Hypothyroidism
What causes hypothyroidism in pregnancy?
Hypothyroidism in pregnancy is usually caused by Hashimoto’s disease and occurs in one to three of every 1,000 pregnancies.3 Like Graves’ disease, Hashimoto’s disease is an autoimmune disorder. In Hashimoto’s disease, the immune system makes antibodies that attack cells in the thyroid and interfere with their ability to produce thyroid hormones. White blood cells also invade the thyroid and decrease thyroid hormone production.
Hypothyroidism in pregnancy can also result from existing hypothyroidism that is inadequately treated or from prior destruction
or removal of the thyroid as a treatment for hyperthyroidism.
How does hypothyroidism affect the mother and baby?
Some of the same problems caused by hyperthyroidism can occur in hypothyroidism. Uncontrolled hypothyroidism during pregnancy can lead to
- congestive heart failure
- preeclampsia
- anemia—a disorder in which the blood does not carry enough oxygen to the body’s tissues
- miscarriage
- low birthweight
- stillbirth
Because thyroid hormones are crucial to fetal brain and nervous system development, uncontrolled hypothyroidism—especially during the first trimester—can lead to cognitive and developmental disabilities in the baby.
How is hypothyroidism in pregnancy diagnosed?
Like hyperthyroidism, hypothyroidism is diagnosed through a careful review of symptoms and measurement of TSH and T4 levels.
Symptoms of hypothyroidism in pregnancy include extreme fatigue, cold intolerance, muscle cramps, constipation, and problems with memory or concentration. High levels of TSH and low levels of free T4 generally indicate hypothyroidism. Because of normal
pregnancy-related changes in thyroid function, test results must be interpreted with caution.
The TSH test can also identify subclinical hypothyroidism—a mild form of hypothyroidism that has no apparent symptoms. Subclinical hypothyroidism occurs in two to three of every 100 pregnancies.4 Test results will show high levels of TSH and normal free T4. Experts have not reached a consensus as to whether asymptomatic pregnant women should be routinely screened for hypothyroidism. But if subclinical hypothyroidism is discovered during pregnancy, treatment is recommended to help ensure a healthy pregnancy.
How is hypothyroidism treated during pregnancy?
Hypothyroidism is treated with synthetic thyroxine, which is identical to the T4 made by the thyroid gland. Women with pre-existing hypothyroidism will need to increase their prepregnancy dose of thyroxine to maintain normal thyroid function. Thyroid function should be checked every 6 to 8 weeks during pregnancy. Synthetic thyroxine is safe for the fetus and necessary for its well-being if the mother has hypothyroidism.
3Ibid.
4The Endocrine Society. Management of thyroid dysfunction during pregnancy and postpartum: an Endocrine Society clinical practice guideline. The Journal of Clinical Endocrinology & Metabolism. 2007;92(8):S1–S47.
[Top]
Postpartum Thyroiditis
What is postpartum thyroiditis?
Postpartum thyroiditis is an inflammation of the thyroid gland that appears 1 to 8 months after giving birth and affects about 8 percent of women who delivered within the previous year.5 Thyroiditis can cause stored thyroid hormone to leak out of the inflamed gland and raise hormone levels in the blood.
Postpartum thyroiditis is believed to be an autoimmune condition and causes mild hyperthyroidism that usually lasts 1 to 2 months. Many women then develop hypothyroidism lasting 6 to 12 months before the thyroid regains normal function. In some women, the thyroid is too damaged to regain normal function and their hypothyroidism is permanent, requiring lifelong treatment with synthetic thyroid hormone.
Postpartum thyroiditis sometimes goes undiagnosed because the symptoms are mistaken for postpartum blues—the exhaustion and moodiness that sometimes follow delivery. If symptoms of fatigue and lethargy do not go away within a few months or a woman develops
postpartum depression, she should talk with her doctor. She may have developed a permanent thyroid condition and will need to take medication.
5Nicholson WK, Robinson KA, Smallridge RC, Ladenson PW, Powe NR. Prevalence of postpartum thyroid dysfunction: a quantitative review. Thyroid. 2006;16(6):573–582.
[Top]
Points to Remember
Pregnancy causes normal changes in thyroid function but can also lead to thyroid disease. If uncontrolled during pregnancy, hyperthyroidism—too much thyroid hormone in the blood—can be dangerous to the mother and cause health problems such as congestive heart failure and poor weight gain in the baby. Mild hyperthyroidism in pregnancy does not require treatment. More severe hyperthyroidism is usually treated with drugs that interfere with thyroid hormone production. If uncontrolled during pregnancy, hypothyroidism—too little thyroid hormone in the blood—also threatens
the mother’s health and can lead to developmental disabilities in the baby. Hypothyroidism in pregnancy is safely and easily treated with synthetic thyroid hormone. Postpartum thyroiditis—inflammation of the thyroid gland—causes a brief period of hyperthyroidism, often followed by hypothyroidism that usually resolves within a year. Sometimes the hypothyroidism is permanent.
[Top]
Hope through Research
Researchers are investigating the development,
signs and symptoms, and genetics of thyroid function disorders to further understand
thyroid diseases. Scientists continue to study treatment options for pregnant women with thyroid disorders, as well as long-term outcomes for mothers and their children. For information about current studies, see www.ClinicalTrials.gov.
The U.S. Government does not endorse or favor any specific commercial product or company. Trade, proprietary, or company names appearing in this document are used only because they are considered necessary in the context of the information provided. If a product is not mentioned, the omission does not mean or imply that the product is unsatisfactory.
[Top]
For More Information
For more information, contact the following organizations:
American Association of Clinical Endocrinologists
245 Riverside Avenue, Suite 200
Jacksonville, FL 32202
Phone: 904–353–7878
Fax: 904–353–8185
Email: info@aace.com
Internet: www.aace.com
American Thyroid Association
6066 Leesburg Pike, Suite 550
Falls Church, VA 22041
Phone: 1–800–THYROID (849–7643) or 703–998–8890
Fax: 703–998–8893
Email: admin@thyroid.org
Internet: www.thyroid.org
The Endocrine Society
8401 Connecticut Avenue, Suite 900
Chevy Chase, MD 20815
Phone: 1–888–363–6274 or 301–941–0200
Fax: 301–941–0259
Email: societyservices@endo-society.org
Internet: www.endo-society.org
The Hormone Foundation
8401 Connecticut Avenue, Suite 900
Chevy Chase, MD 20815–5817
Phone: 1–800–HORMONE (467–6663)
Fax: 301–941–0259
Email: hormone@endo-society.org
Internet: www.hormone.org
National Graves’ Disease Foundation
P.O. Box 1969
Brevard, NC 28712
Phone: 1–877–NGDF123 (643–3123) or 828–877–5251
Email: nancy@ngdf.org
Internet: www.ngdf.org
The National Endocrine and Metabolic Diseases Information Service collects resource information about endocrine and metabolic diseases for the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) Reference Collection. This database provides titles, abstracts, and availability information for health information and health education resources. The NIDDK Reference Collection is a service of the National Institutes of Health.
You may view the results of the automatic search on pregnancy and thyroid disease.
If you wish to perform your own search of the database, you may access and search the NIDDK Reference Collection.
This publication may contain information about medications used to treat a health condition. When this publication was prepared, the NIDDK included the most current information available. Occasionally, new information about medication is released. For updates or for questions about any medications, please contact the U.S. Food and Drug Administration at 1–888–INFO–FDA (463–6332), a toll-free call, or visit their website at www.fda.gov. Consult your doctor for more information.
[Top]
The National Endocrine and Metabolic Diseases Information Service
6 Information Way
Bethesda, MD 20892–3569
Phone: 1–888–828–0904
TTY: 1–866–569–1162
Fax: 1–703–738–4929
Email: endoandmeta@info.niddk.nih.gov
Internet: http://endocrine.niddk.nih.gov/
The National Endocrine and Metabolic Diseases Information Service is an information dissemination service of the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). The NIDDK is part of the National Institutes of Health, which is part of the U.S. Department of Health and Human Services.
The NIDDK conducts and supports biomedical research. As a public service the NIDDK has established information services to increase knowledge and understanding about health and disease among patients, health professionals and the public.
Publications produced by the NIDDK are carefully reviewed by both NIDDK scientists and outside experts. This publication was reviewed by Lewis Braverman, M.D., Boston Medical Center, and Linda Barbour, M.D., M.S.P.H., University of Colorado Denver.
This publication is not copyrighted. The Clearinghouse encourages users of this publication to duplicate and distribute as many copies as desired.
NIH Publication No. 08–6234
June 2008
[Top]
|










