|
|
|
|||||||||||

|
|||||||||||||||||||||||||||||||||||||||||||||
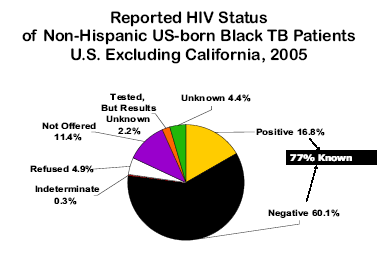
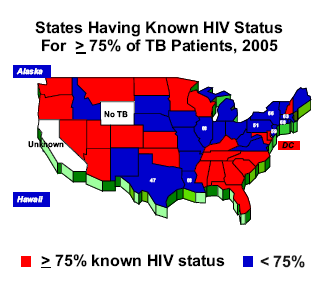
TB Challenge: Partnering to Eliminate TB in African AmericansReported Tuberculosis and HIV-infection, 2005Suzanne Marks, MPH, MA and Elvin Magee, MPH, MSIn this article, we discuss the need for improvements in HIV testing and reporting and potential populations who may most benefit from these improvements. More persons might accept HIV testing if rapid HIV diagnostics and opt-out testing were used. Prevention, early diagnosis, and access to care for both diseases are especially important for African-Americans, substance abusers, homeless persons, and inmates due to the high burden of both HIV and TB in these groups. Once HIV is diagnosed, TB can be prevented through targeted efforts to diagnose and treat latent TB infection before TB disease develops. Globally, tuberculosis (TB) is the leading killer of people who are HIV-infected. In the United States, patients with TB disease and the human immunodeficiency virus (HIV) have over five times the odds of dying during anti-TB treatment and over three times the odds of being diagnosed with TB disease at death as HIV-uninfected patients. This underscores the importance of prevention, early diagnosis, and treatment for both TB and HIV. HIV is also the most important known risk factor for progression to TB disease from latent TB infection (LTBI). Two to eight percent of HIV-infected persons with LTBI progress to TB disease each year within 5 years after infection, versus a total of eight percent of HIV-uninfected persons with LTBI over a time period of 60 years. Highly active antiretroviral therapy (HAART) has been shown to reduce the risk of developing TB disease in HIV-infected persons, and reduces TB relapse and death in patients with TB disease. TB disease is an AIDS-defining opportunistic condition. If individuals are diagnosed with TB disease, provider knowledge of HIV infection and use of HIV medications is critical for optimal patient management and for referrals to care to prevent mortality and additional morbidities. CDC has recommended HIV testing of all TB patients since 1989. Routine HIV testing has been recommended since 2001, since targeted testing based on provider assessment of patient risk behaviors fails to identify a substantial number of HIV-infected persons. This is because often the TB patients do not perceive themselves to be at risk for HIV or do not disclose their risks. Routine HIV testing of all TB patients can also reduce the stigma associated with testing. CDC's revised HIV testing guidelines issued in September 2006 call for “opt-out” HIV testing of all persons in clinic settings. Opt-out testing means that the provider should perform HIV testing after notifying the patient that: 1) the test will be performed, and 2) the patient may elect to decline or defer testing. Our study objective was to describe the recent status of reported HIV infection in TB patients, HIV/TB comorbidity, and the characteristics of HIV/TB patients in the United States. We analyzed data reported for 2005 on HIV status from the National TB Surveillance System. California data were excluded because the state shares with CDC only the results of AIDS and TB registry matches. HIV-positive or HIV-negative status is defined as “known.” HIV prevalence equal to or greater than one percent of any specific population is considered high. In 2005, 69 percent of all TB patients had known HIV status. Of the remaining 31 percent, nearly half were not offered HIV testing and a quarter refused testing when offered. A greater percentage of non-Hispanic black TB patients had known HIV status (79 percent). For US-born non-Hispanic blacks, 77 percent had known HIV status. Black females were more likely than black males to have had unknown HIV status.
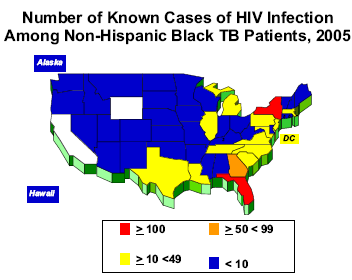
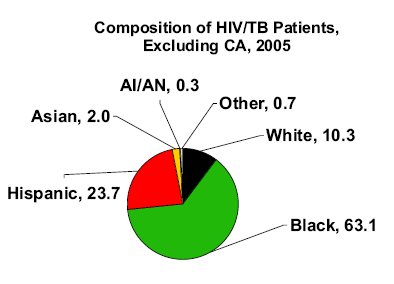
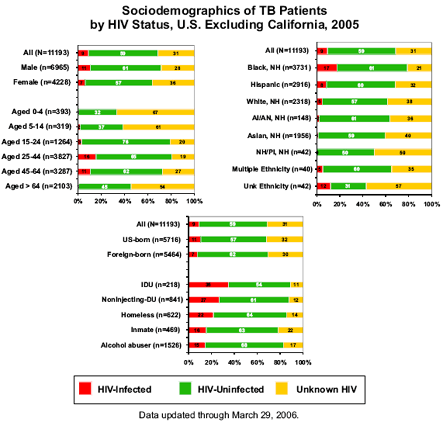
Black TB patients had the highest known prevalence of HIV infection of the major race/ethnic groups: 17% vs. 8% of Hispanics, 5% of whites, 2% of American Indian/Alaska Natives, and 1% of Asians. And, because of the high prevalence of both TB and HIV among blacks, nearly two-thirds (63%) of patients having both TB and HIV disease were black.
The graphs below show reported data on the socio-demographics of TB patients by HIV status.
TB patients having exceptionally high (higher than the average 9%) rates of HIV-infection included males, those aged 25-44, those aged 45-64, non-Hispanic blacks, those of unknown race/ethnicity, US-born persons, injection drug users (IDUs), non-injection drug users, homeless persons, inmates, and alcohol abusers. Substance abuse, homelessness, and incarceration are factors associated with both HIV and TB incidence and transmission of disease. In summary, nearly one-third of all TB patients and one-fifth of non-Hispanic black TB patients had unknown HIV status in 2005. HIV prevalence was high in nearly all TB patient groups, with some having exceptionally high HIV prevalence. Improvements in HIV testing and reporting are needed. The use of “opt-out” HIV testing and rapid HIV tests (with results available in < 20 minutes) may facilitate improvements in knowledge of HIV status. TB can be prevented through targeted efforts aimed at diagnosing and treating latent TB infection before TB disease develops, especially in substance abusers, homeless persons, and inmates. And, TB relapse and mortality may be avoided by early access to HIV care and support services. Because of the high burden of both HIV and TB in the African-American community, prevention, early diagnosis, and access to care are especially important for this population.
Last Reviewed: 05/18/2008 |
|
|
If you would like to order any of the DTBE publications please visit the online order form. You will need Adobe Acrobat™ Reader v5.0 or higher to read pages that are in PDF format. Download the Adobe Acrobat™ Reader. If you have difficulty accessing any material on the DTBE Web site because of a disability, please contact us in writing or via telephone and we will work with you to make the information available. Division of Tuberculosis Elimination
Centers for Disease Control & Prevention |