|

Slide 14
Hantavirus Pulmonary Syndrome
Clinical Presentation
Clinical Presentation of HPS: Most frequent symptoms include
fever, myalgia, nausea/vomiting, and cough. Other symptoms
include dizziness, arthralgia, and shortness of breath. Rhinorrhea
and sore throat are rarely seen.
|

Slide 15
Hantavirus Pulmonary Syndrome
Physical Examination
Physical Examination Findings of HPS: Typical findings include
fever, tachypnea, tachycardia, hypotension, and crackles or
rales on lung examination. 
|
Slide 16
Hantavirus Pulmonary Syndrome
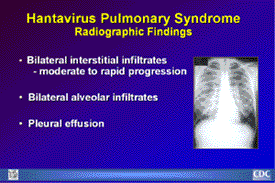
Radiographic Findings
Radiographic Findings of HPS: Findings usually include interstitial
edema, Kerley B lines, hilar indistinctness and peribronchial
cuffing with normal cardiothoracic ratios. HPS begins with
minimal changes of interstitial pulmonary edema and rapidly
progressing to alveolar edema with severe bilateral involvement.
Pleural effusions are common and are often large enough to
be evident radiographically. |
Slide 17
Radiographic Progression of HPS
in the Lungs
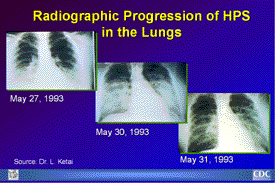
Radiographic Progression of HPS in the Lungs: These chest
X-rays of an HPS patient were taken on May 27, May 30, and
May 31, 1993. Approximately one-third of patients show evidence
of pulmonary edema in the initial radiograph. Forty-eight
hours after the initial radiograph, virtually all patients
demonstrate interstitial edema and two-thirds have developed
extensive bibasilar or perihilar airspace disease (courtesy
of L. Ketai). |
|
Slide 18
Hantavirus Pulmonary Syndrome
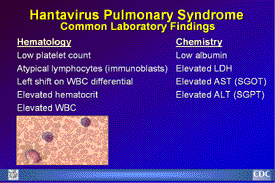
Common Laboratory Findings
Common Laboratory Findings: Notable hematological findings
include low platelet count, immunoblasts, left shift on WBC
differential, elevated WBC, and elevated hematocrit. The large
atypical lymphocyte shown here is an example of one of the
laboratory findings that, when combined with a bandemia and
dropping platelet count, are characteristic of HPS. Notable
blood chemistry findings include low albumin, elevated lactate
dehydrogenase (LDH), elevated aspartate aminotransferase (AST
or SGOT) and elevated alanine aminotransferase (ALT or SGPT).
|
Slide 19
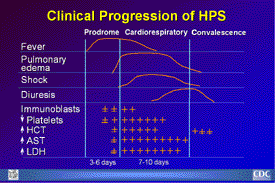
Clinical Progression of HPS
Clinical Course of HPS: Clinical course of HPS starts with
a febrile prodrome that may ultimately lead to hypotension
and end-organ failure. The onset of the immune response precedes
severe organ failure, which is thought to be immunopathologic
in nature. Hypotension does not result in shock until the
onset of respiratory failure, but this may reflect the severe
physiologic impact of lung edema. |

Slide 20
HPS Management
HPS Patient Management: Treatment of patients remains supportive
in nature. Early aggressive intensive care is imperative,
and may include early use of inotropic agents, such as dobutamine,
to augment myocardial contractivity. Patients require early
ventilation and careful monitoring of oxygenation, fluid balance,
and blood pressure. |

Slide 21
ICU Monitoring and Therapy
ICU Monitoring and Therapy: Because of the rapid progression
of the disease, patients should be quickly transferred to
a fully equipped emergency facility when necessary. Patients
should be closely and continually monitored by a physician
so that life-supporting procedures can be performed. Inotropic
agents, mechanical ventilation, early PA catheterization and
judicious volume resuscitation are elements of supportive
care. |
Slide 22
Hantavirus Pulmonary Syndrome
Laboratory-confirmed Diagnosis
Laboratory Confirmation of HPS: HPS can be diagnosed several
ways. CDC uses an enzyme-linked immunosorbent assay (ELISA)
to detect IgM antibodies to SNV and to diagnose acute infections
with other hantaviruses. An IgG test is used in conjunction
with the IgM-capture test. A four fold rise in IgG antibody
titer between acute- and convalescent-phase sera or the presence
of IgM in acute-phase sera are diagnostic for hantaviral disease.
Note that acute-phase serum sent as an initial diagnostic
specimen may not yet have IgG. IgG antibody is long lasting,
and sera of patients retrospectively identified appear to
have retained antibody for many years. The RT-PCR technique
allows for classification of distinct viruses prior to viral
isolation. Immunohistochemical staining is used for postmortem
or retrospective diagnosis. |
Slide 23
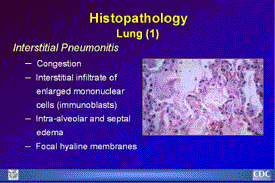
Histopathology
Lung (1)
Histopathology Lungs (1): No single pathognomonic lesion will
permit histopathologic diagnosis of HPS. Lungs are dense and
rubbery, usually weighing twice as much as the average lung.
In most cases there is a mild to moderate interstitial pneumonitis
with variable degrees of congestion, edema, and mononuclear
cell infiltration. Focal hyaline membranes are observed, as
well as extensive intra-alveolar and septal edema. |
Slide 24
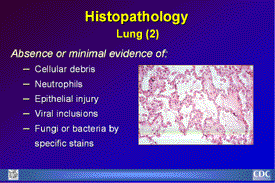
Histopathology
Lung (2)
Histopathology Lungs (2): In typical cases, neutrophils are
scanty and the respiratory epithelium remains intact. There
is no evidence of cellular debris, nuclear fragmentation,
viral inclusions, fungi or bacteria by specific stains.
|
Slide 25
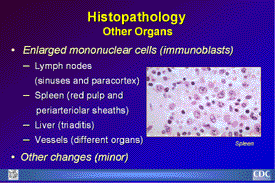
Histopathology
Other Organs
Histopathology of Other Organs: Typical histopathologic findings
that may be seen in lymphoid tissues of HPS patients include
the presence of immunoblasts within the red pulp and periarteriolar
sheaths of the spleen; in the paracortex and sinuses of lymph
nodes; and in the peripheral blood. |

 National
Center for Infectious Diseases
National
Center for Infectious Diseases National
Center for Infectious Diseases
National
Center for Infectious Diseases