
|
 |
| What
is Marburg hemorrhagic fever? |
 |
 |
 |
| |
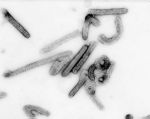
Negative stain
image of an isolate of Marburg virus, showing filamentous particles
as well as the characteristic "Shepherd's Crook."
Magnification approximately 100,000 times. Image courtesy of
Russell Regnery, Ph.D., DVRD, NCID, CDC. Go to high-resolution
version. |
Marburg hemorrhagic
fever is a rare, severe type of hemorrhagic fever which affects both humans
and non-human primates. Caused by a genetically unique zoonotic (that
is, animal-borne) RNA virus of the filovirus family, its recognition led
to the creation of this virus family. The four species of Ebola virus
are the only other known members of the filovirus family.
Marburg virus was
first recognized in 1967, when outbreaks of hemorrhagic fever occurred
simultaneously in laboratories in Marburg and Frankfurt, Germany and in
Belgrade, Yugoslavia (now Serbia). A total of 37 people became ill; they
included laboratory workers as well as several medical personnel and family
members who had cared for them. The first people infected had been exposed
to African green monkeys or their tissues. In Marburg, the monkeys had
been imported for research and to prepare polio vaccine.
| Where
do cases of Marburg hemorrhagic fever occur? |
 |
Recorded cases of
the disease are rare, and have appeared in only a few locations. While
the 1967 outbreak occurred in Europe, the disease agent had arrived with
imported monkeys from Uganda. No other case was recorded until 1975, when
a traveler most likely exposed in Zimbabwe became ill in Johannesburg,
South Africa – and passed the virus to his traveling companion and
a nurse. 1980 saw two other cases, one in Western Kenya not far from the
Ugandan source of the monkeys implicated in the 1967 outbreak. This patient’s
attending physician in Nairobi became the second case. Another human Marburg
infection was recognized in 1987 when a young man who had traveled extensively
in Kenya, including western Kenya, became ill and later died.
In 1998, an outbreak occurred in Durba, Democratic Republic of
the Congo. Cases were linked to individuals working in a gold mine. After
the outbreak subsided, there were still some sporadic cases that occurred
in the region.
| Where
is Marburg virus found? |
 |
Marburg virus is
indigenous to Africa. While the geographic area to which it is native
is unknown, this area appears to include at least parts of Uganda and
Western Kenya, and perhaps Zimbabwe. As with Ebola virus, the actual animal
host for Marburg virus also remains a mystery. Both of the men infected
in 1980 in western Kenya had traveled extensively, including making a
visit to a cave, in that region. The cave was investigated by placing
sentinels animals inside to see if they would become infected, and by
taking samples from numerous animals and arthropods trapped during the
investigation. The investigation yielded no virus. The sentinel animals
remained healthy and no virus isolations from the samples obtained have
been reported.
| How
do humans get Marburg hemorrhagic fever? |
 |
Just how the animal
host first transmits Marburg virus to humans is unknown. However, as with
some other viruses which cause viral hemorrhagic fever, humans who become
ill with Marburg hemorrhagic fever may spread the virus to other people.
This may happen in several ways. Persons who have handled infected monkeys
and have come in direct contact with their fluids or cell cultures, have
become infected. Spread of the virus between humans has occurred in a
setting of close contact, often in a hospital. Droplets of body fluids,
or direct contact with persons, equipment, or other objects contaminated
with infectious blood or tissues are all highly suspect as sources of
disease.
| What
are the symptoms of the disease? |
 |
After an incubation
period of 5-10 days, the onset of the disease is sudden and is marked
by fever, chills, headache, and myalgia. Around the fifth day after the
onset of symptoms, a maculopapular rash, most prominent on the trunk (chest,
back, stomach), may occur. Nausea, vomiting, chest pain, a sore throat,
abdominal pain, and diarrhea then may appear. Symptoms become increasingly
severe and may include jaundice, inflammation of the pancreas, severe
weight loss, delirium, shock, liver failure, and
multi-organ dysfunction.
Because many of the
signs and symptoms of Marburg hemorrhagic fever are similar to those of
other infectious diseases, such as malaria or typhoid fever, diagnosis
of the disease can be difficult, especially if only a single case is involved.
| What laboratory tests are used to diagnose Marburg hemorrhagic fever? |
 |
Antigen-capture enzyme-linked
immunosorbent assay (ELISA) testing, IgM-capture ELISA, real-time polymerase chain
reaction (RT-PCR), and virus isolation can be used to confirm a case of Marburg
hemorrhagic fever within a few days of the onset of symptoms. The IgG-capture
ELISA is appropriate for testing persons later in the course of disease
or after recovery. The disease is readily diagnosed by immunohistochemistry,
virus isolation, or RT-PCR of blood or tissue specimens from deceased patients.
| Are
there complications after recovery? |
 |
Recovery from Marburg
hemorrhagic fever may be prolonged and accompanied by orchititis (inflammation of one or both testes), recurrent
hepatitis (inflammation of the liver), transverse myelitis ( inflammation of the spinal cord), uvetis (inflammation of the eye), or parotitis (inflammation of the parotid gland).
| Is
the disease ever fatal? |
 |
Yes. For a complete listing of the case fatality rates for previous outbreaks, please see the “History of Outbreaks” table.
| How
is Marburg hemorrhagic fever treated? |
 |
A specific treatment
for this disease is unknown. However, supportive hospital therapy should
be utilized. This includes balancing the patient’s fluids and electrolytes,
maintaining their oxygen status and blood pressure, replacing lost blood
and clotting factors and treating them for any complicating infections.
Sometimes treatment
also has used transfusion of fresh-frozen plasma and other preparations
to replace the blood proteins important in clotting. One controversial
treatment is the use of heparin (which blocks clotting) to prevent the
consumption of clotting factors. Some researchers believe the consumption
of clotting factors is part of the disease process.
| Who
is at risk for the illness? |
 |
People who have close
contact with a human or non-human primate infected with the virus are
at risk. Such persons include laboratory or quarantine facility workers
who handle non-human primates that have been associated with the disease.
In addition, hospital staff and family members who care for patients with
the disease are at risk if they do not use proper barrier
nursing techniques.
| How
is Marburg hemorrhagic fever prevented? |
 |
Due to our limited
knowledge of the disease, preventive measures against transmission from
the original animal host have not yet been established. Measures for prevention
of secondary transmission are similar to those used for other hemorrhagic
fevers. If a patient is either suspected or confirmed to have Marburg
hemorrhagic fever, barrier nursing techniques
should be used to prevent direct physical contact with the patient. These
precautions include wearing of protective gowns, gloves, and masks; placing
the infected individual in strict isolation; and sterilization or proper
disposal of needles, equipment, and patient excretions.
In conjunction with
the World Health Organization, CDC has developed practical, hospital-based
guidelines, titled Infection Control for Viral
Haemorrhagic Fevers In the African Health Care Setting. The manual
can help health-care facilities recognize cases and prevent further hospital-based
disease transmission using locally available materials and few financial
resources.
| What
needs to be done to address the threat of Marburg hemorrhagic fever? |
 |
Marburg hemorrhagic
fever is a very rare human disease. However, when it does occur, it has
the potential to spread to other people, especially health care staff
and family members who care for the patient. Therefore, increasing awareness
among health-care providers of clinical symptoms in patients that suggest
Marburg hemorrhagic fever is critical. Better awareness can help lead
to taking precautions against the spread of virus infection to family
members or health-care providers. Improving the use of diagnostic tools
is another priority. With modern means of transportation that give access
even to remote areas, it is possible to obtain rapid testing of samples
in disease control centers equipped with Biosafety Level 4 laboratories
in order to confirm or rule out Marburg virus infection.
A fuller understanding
of Marburg hemorrhagic fever will not be possible until the ecology and
identity of the virus reservoir are established. In addition, the impact
of the disease will remain unknown until the actual incidence of the disease
and its endemic areas are determined.
| Suggested Reading |
 |
Bausch DG, Matthias B, Grein T, et al. Risk Factors for Marburg Hemorrhagic Fever, Democratic Republic of the Congo. Emerg Infect Dis. 2003;9(12):1531-1537
CDC. Notice to Readers Update: Management of Patients with Suspected Viral Hemorrhagic Fever United States. MMWR 1995;44(25):475-479
|
 |
 |
 |
| Contact Us |
|
|
 |
 |
|
| Related
Links |
|
|
 |
 |
|
| Glossary |
| Unsure
about some of the terms used on this page? Visit our glossary
of terms for help. |
 |
 |
|
|
 |
