
|
 |
"Infection
Control for Viral Haemorrhagic Fevers
In the African Health Care Setting"
Annexes 1-5
|
Annex 1 Standard Precautions for Hospital Infection Control13
|
 |
Standard
Precautions aim to reduce the risk of disease transmission in the health
care setting, even when the source of infection is not known. Standard
Precautions are designed for use with all patients who present in the
health care setting and apply to:
- Blood and most
body fluids whether or not they contain blood
- Broken skin
- Mucous membranes.
To reduce the risk of disease transmission in the health care setting,
use the following Standard Precautions.
- Wash hands immediately
with soap and water before and after examining patients and after any
contact with blood, body fluids and contaminated item--whether or not
gloves were worn. Soaps containing an antimicrobial agent are recommended.
- Wear clean, ordinary
thin gloves anytime there is contact with blood, body fluids, mucous
membrane, and broken skin. Change gloves between tasks or procedures
on the same patient. Before going to another patient, remove gloves
promptly and wash hands immediately, and then put on new gloves.
- Wear a mask, protective
eyewear and gown during any patient-care activity when splashes or sprays
of body fluids are likely. Remove the soiled gown as soon as possible
and wash hands.
- Handle needles
and other sharp instruments safely. Do not recap needles. Make sure
contaminated equipment is not reused with another patient until it has
been cleaned, disinfected, and sterilized properly. Dispose of non-reusable
needles, syringes, and other sharp patient-care instruments in puncture-resistant
containers.
- Routinely clean
and disinfect frequently touched surfaces including beds, bed rails,
patient examination tables and bedside tables.
- Clean and disinfect
soiled linens and launder them safely. Avoid direct contact with items
soiled with blood and body fluids.
-
Place a patient
whose blood or body fluids are likely to contaminate surfaces or other
patients in an isolation room or area.
- Minimize the
use of invasive procedures to avoid the potential for injury and accidental
exposure. Use oral rather than injectable medications whenever possible.
When a specific diagnosis
is made, find out how the disease is transmitted. Use precautions according
to the transmission risk.
- If airborne
transmission:
- Place the
patient in an isolation room that is not air-conditioned or where
air is not circulated to the rest of the health facility. Make sure
the room has a door that can be closed.
- Wear a HEPA
or other biosafety mask when working with the patient and in the
patient's room.
- Limit movement
of the patient from the room to other areas. Place a surgical mask
on the patient who must be moved.
- Place the
patient in an isolation room.
- Wear a HEPA
or other biosafety mask when working with the patient.
- Limit movement
of the patient from the room to other areas. If patient must be
moved, place a surgical mask on the patient.
- If contact
transmission:
- Place the
patient in an isolation room and limit access.
- Wear gloves
during contact with patient and with infectious body fluids or
contaminated items. Reinforce handwashing throughout the health
facility.
- Wear two
layers of protective clothing.
- Limit movement
of the patient from the isolation room to other areas.
- Avoid sharing
equipment between patients. Designate equipment for each patient,
if supplies allow. If sharing equipment is unavoidable, clean
and disinfect it before use with the next patient.
13 Adapted
from Garner JS, Hospital Infection Control Practices Advisory Committee.
Guideline for Isolation Precautions In Hospitals, January 1996. Centers
for Disease Control and Prevention, Public Health Service, US Department
of Health and Human Services, Atlanta,Georgia.
|
Annex 2 Specific Features of VHFs14
|
 |
Geographical and
epidemiological characteristics of VHFs
| Disease |
Geography |
Vector/ Reservoir |
Human Infection |
| Crimean Congo
HF |
-Africa -Balkans
-China (Western)
-Former Soviet
Union (Southern)
-Middle East |
Ticks.
Tick mammal-tick maintenance. |
--Tick bites.
--Squashing ticks.
-- Exposure to aerosols or fomites from slaughtered cattle and sheep
(domestic animals do not show evidence of illness but may become
infected when transported to market or when held in pens for slaughter).
--Nosocomial epidemics have occurred.
|
| Dengue HF,
Dengue Shock Syndrome (DHF/DSS) |
All Tropic and
subtropical Regions |
Aedes aegypti
mosquitoes. Mosquito-human mosquito maintenance. Transmission
occurs with the frequent geographic transport of viruses by travelers. |
Increased worldwide
distribution of the mosquito and the movement of dengue viruses in
travelers is increasing the areas that are becoming infected. |
| Ebola HF
and Marburg HF |
Africa |
Unknown. |
--Virus is
spread by close contact with an infected person.
--Route of infection of the first case is unknown.
--Infected non human primates sometimes provide transmission link
to humans.
--Aerosol transmission is suspected in some monkey infections.
|
| Lassa Fever |
West Africa |
Mice.
The Mastomys genus of the mouse. |
--Transmitted
by aerosols from rodent to man.
-- Direct contact with infected rodents or their droppings, urine,
or saliva.
--Person - to person contact.
Note: The reservoir rodent is very common in Africa and the
disease is a major cause of severe febrile illness in West Africa
|
| Rift Valley
Fever |
Sub-Saharan
Africa |
Floodwater
mosquitoes.
Maintained between mosquitoes
and domestic animals, particularly
sheep and cattle. |
--Mosquito
bite.
--Contact with blood of infected sheep, cattle, or goats.
--Aerosols generated from infected domestic animal blood.
--No person -to person transmission observed.
|
| Yellow Fever |
--Africa
--South America |
Aedes aegypti
mosquitoes.
Mosquito - monkey - mosquito maintenance. Occasional human
infection occurs when unvaccinated humans enter forest. In an urban
outbreak, virus maintained in infected Aedes aegypti mosquitoes and
humans. |
--Mosquito
bite.
-- In epidemics, mosquitoes amplify transmission between humans.
--Fully developed cases cease to be viremic. Direct person-to person
transmission is not believed to be a problem although the virus
is highly infectious (including aerosols) in the laboratory.
|
14 Peters CJ, Zaki SR, Rollin
PE. Viral Hemorrhagic Fevers, Chapter 10 in Atlas of Infectious Diseases,
vol 8, vol ed Robert Fekety, book ed GL Mandell. Philadelphia: Churchill
Livingstone. 1997: pp10.1-10.26.
Common Clinical
Features of VHFs
| Disease |
Incubation
Period |
Case
Fatality |
Characteristic
Features |
| Crimean
Congo HF |
3-12
days |
15%-30% |
Most severe
bleeding and ecchymoses (a purplish patch caused by blood coming
from a vessel into the skin) of all the HF.
|
| Ebola
HF and Marburg HF |
2-21
days |
25%-90% |
--Most fatal
of all HF.
-- Weight loss.
--Exhaustion and loss of strength.
--A maculopapular (a lesion with a broad base) rash is common
--Post infection events have included hepatitis, uveitis and orchitis.
|
| Lassa
Fever |
5-16
days |
Approximately
15%
|
--Exhaustion
and loss of strength.
--Shock.
--Deafness develops during recovery in 20% of cases.
|
| Rift
Valley Fever |
2-5
days (uncomplicated disease; incubation for HF may differ) |
50%
of severe cases (about 1.5% of all infections) |
--Shock.
-- Bleeding.
--Reduced or no urine production.
--Jaundice.
--Inflammation of the brain.
--Inflammation of the blood vessels in the retina of the eye.
|
| Yellow
Fever |
3-6
days |
20% |
-- Acute febrile
period followed by a brief period of remission.
--Toxic phase follows remission with jaundice and renal failure in
severe cases. |
Specific Clinical
Findings in Different VHFs
| 1
abnormally low number of platelets in the circulating blood |
+
occasional or mild |
| 2
white blood cell count |
++ commonly seen and may be severe |
| 3
jaundice |
+++
characteristic |
|
4 shaking |
S
characteristic and seen in severe cases |
|
5 difficulty speaking and pronouncing words due
to problems with the muscles used for speaking |
 occasionally or
mildly increased
occasionally or
mildly increased |
  commonly decreased
commonly decreased |
|
6 disease of the brain |
E
May develop true encephalitis |
A Summary of Prevention
and Treatments of VHFs
| Disease |
Prevention |
Treatment |
| Crimean Congo
HF |
--Tick avoidance.
--Avoid contact with acutely infected animals, especially slaughtering.
--Use VHF Isolation Precautions when a case is suspected. |
--Ribavirin
is effective in reducing mortality.
--Ribavirin should be used based on in vitro sensitivity and of
limited South African experience.
|
| Dengue HF,
Dengue Shock Syndrome (DHF/DSS) |
--Mosquito control
of Aedes aegypti.
--Vaccines currently under investigation for probable use in travellers
but unlikely to be a solution to hyperendemic dengue transmission
that leads to dengue HF. |
--Supportive
care. It is effective and greatly reduces mortality. |
| Ebola HF
and Marburg HF |
--Standard Precautions
including needle sterilization in African hospitals are particularly
important.
--Use VHF Isolation Precautions when a case is suspected.
--Avoid unprotected contact with suspected patients or infectious
body fluids.
--Avoid contact with monkeys and apes. |
--None other
than supportive care, which may be of limited utility.
--Antiviral therapies urgently needed. |
| Lassa Fever |
--Rodent control.
--Use VHF Isolation Precautions when a case is suspected. |
--Ribavirin
is effective in reducing mortality.
--Use Ribavirin in higher risk patients, e.g. if aspartate aminotransferase
(AST) is greater than 150. |
| Rift Valley
Fever |
--Vaccination
of domestic livestock prevents epidemics in livestock but not sporadic,
endemic infections of humans.
--Human vaccine safe and effective, but in limited supply.
--Veterinarians and virology workers in sub-Saharan Africa are candidates
for vaccine.
|
--Supportive
care.
--Use Ribavirin in haemorrhage fever patients (based on studies
in experimental animals).
|
| Yellow Fever |
-- Mosquito
control of Aedes aegypti would eliminate urban transmission
but forest transmission remains.
--Vaccine is probably the safest and most effective in the world. |
-- Supportive
care. |
|
History
of Viral Haemorrhagic Fevers Seen in Your Area
|
Major
Signs and Symptoms
|
Transmission
Route
|
| |
|
|
| |
|
|
| |
|
|
| |
|
|
|
Annex 3 Planning and Setting Up the Isolation Area
|
 |
Checklist: Supplies
for a Changing Room
Storage Outside
the Changing Room:
| 1.
Shelf or cabinet with lock |
____ |
| 2.
Supply of clean scrub suits, gowns, aprons, gloves, masks, headcovering,
and eyewear |
____ |
| 3.
Covered shelf for storing disinfected boots |
____ |
| 4.
Bucket for collecting non-infectious waste |
____ |
Inside the Changing Room:
| 1.
Hooks, nails, or hangers for hanging reusable gowns, scrub suits |
_____ |
2. Roll of plastic tape |
_____ |
| 3.
Handwashing supplies: bucket or pan, clean water, soap, one-use towels |
_____ |
| 4.
Bucket or pan, 1:100 bleach solution for disinfecting gloved hands |
_____ |
| 5.
Container with soapy water for collecting discarded gloves |
_____ |
| 6.
Container with soapy water for collecting used instruments to be sterilized* |
_____ |
| 7.
Container with soapy water for collecting reusable gowns, masks, sheets
to launder* |
_____ |
*Place outside the changing room if the changing room
is too small
If large amounts
of waste on floor:
Sprayer, bucket or shallow pan with 1:100 bleach solution for disinfecting
boots
Checklist: Supplies
for Patient Area
| 1.
1 bed with clean mattress or sleeping mat and at least a bottom sheet
and blanket for each bed |
_____ |
| 2.
Plastic sheeting to cover mattress or sleeping mat |
_____ |
| 3.
1 thermometer, 1 stethoscope, and 1 blood pressure cuff for each patient
or for each patient area |
_____ |
| 4.
1 puncture-resistant container for collecting non-reusable needles,
syringes, and discarded sharp instruments |
_____ |
| 5.
1 bedside table or shelf |
_____ |
6. 1 large wall clock with a second hand |
_____ |
| 7.
Pan with 1:100 bleach solution or alcohol and one-use towels for disinfecting
the thermometer and stethoscope between use with each patient |
_____ |
| 8.
Bucket or pan, 1:100 bleach solution, one-use towels for disinfecting
gloved hands between patients |
_____ |
| 9.
Supplies for disinfecting patient excreta (bedpan, urinal, 1:10 bleach
solution) |
_____ |
| 10.
Sprayer, 1:100 bleach solution, clear water, and mop for disinfecting
spills on floor and walls |
_____ |
| 11.
Container with soapy water for collecting discarded gloves |
_____ |
| 12.
Screens (or sheets hung from ropes or lines) placed between VHF patients'
beds |
_____ |
| 13.
Extra supply of gowns and gloves |
_____ |
| 14.
Container for collecting infectious waste to be burned |
_____ |
Use the grid on the
next page to draw the layout of an isolation area in your own health facility.
Be sure to include:
- Area for patient
isolation
- Changing room for
health care workers to use for changing clothes
- Area for cleaning
and laundering VHF-contaminated supplies
- Changing area for
cleaning staff who handle VHF-contaminated waste but who do not do direct
patient-care activities.
Planning Grid: Layout for Isolation Area in Your Health
Facility
|
Annex 4 Adapting VHF Isolation Precautions for a Large Number of Patients |
 |
The recommendations
in this manual assume 1 or 2 VHF cases have occurred in a non-outbreak
situation. When more than 1 or 2 VHF patients present in the health facility,
additional precautions need to be taken. When Ebola haemorrhagic fever
occurs, initially there may be as many as 10 cases.
When a VHF is suspected,
develop a case definition based on the VHF that has occurred. Use it to
identify new cases during the outbreak.
For example, the current case definition for suspecting Ebola haemorrhagic
fever (EHF) is:
|
Anyone presenting
with fever and signs of bleeding such as:
- Bleeding
of the gums
- Bleeding
from the nose
- Red eyes
- Bleeding
into the skin (purple coloured patches in the skin)
- Bloody or
dark stools
- Vomiting
blood
- Other unexplained
signs of bleeding
Whether or
not there is a history of contact with a suspected case of EHF.
OR
Anyone living
or deceased with:
- Contact
with a suspected case of EHF AND
- A history
of fever, with or without signs of bleeding.
OR
Anyone living
or deceased with a history of fever AND 3 of the following
symptoms:
- Headache
- Vomiting
- Loss of
appetite
- Diarrhoea
- Weakness
or severe fatigue
- Abdominal
pain
- Generalized
muscle or joint pain
- Difficulty
swallowing
- Difficulty
breathing
- Hiccups
OR
Any unexplained
death in an area with suspected cases of EHF.
|
The current case definition for suspecting Lassa fever is:
|
Unexplained
fever at least 38°C or 100.4°F for one week or more.
And 1 of the following:
- No response
to standard treatment for most likely cause of fever (malaria,
typhoid fever)
- Readmitted
within 3 weeks of inpatient care for an illness with fever
And
1 of the following:
- Edema or
bleeding
- Sore throat
and retrosternal pain/vomiting
- Spontaneous
abortion following fever
- Hearing
loss following fever
|
Prepare Your Health
Facility
If there are more than 2 suspected VHF patients, take
steps immediately to adapt the VHF Isolation Precautions for a large number
of patients.
- Reinforce the
use of Standard Precautions --especially handwashing-- throughout the
health facility. Make sure there is a reliable supply of soap and clean
water in areas where health facility staff have contact with patients
suspected as having a VHF.
- Make sure adequate
supplies of protective clothing are available.
- Set up a temporary
area that is separate from the rest of the facility where febrile patients
can wait to be seen by a health care worker. Also use this area for
patients who have been seen by a health care worker and who are waiting
to go to the isolation area.
Make sure the temporary admission area contains a supply of protective
clothing, buckets with disinfectants in them for collecting disposable
waste, and disinfectants for cleaning and disinfecting spills of infectious
materials.
- Identify a family
liaison person from the health facility staff who can spend time with
families to answer questions, provide information about the VHF and
its transmission. If family members help provide care when relatives
are in hospital, make sure they know how to use protective clothing
when they are with the patient in the isolation area. Help families
with arrangements for cooking, washing and sleeping.
- Designate a separate
building or ward for placing patients with the same disease together
in a single isolation area. Select and isolate a toilet or latrine for
disposal of disinfected patient waste and other liquid waste.
- Restrict access
to the building or ward set aside as the isolation area. Set up walkways
from the temporary area to the isolation area by tying ropes along the
walkway and hanging plastic sheets from them.
- Prepare a list
of health facility staff authorized to enter the isolation area. Station
a guard at the entry to the isolation area, and provide the guard with
the list of authorized persons. The guard will use the list to limit
access to the isolation area to authorized health facility staff and,
if necessary, the caregiving family member.
- Provide the guard
with a sign-in sheet for recording who goes into the isolation area
and the time of entry and departure.
- Prepare a large
quantity of disinfectant solutions each day (bleach solutions and detergent
solutions). Store the disinfectants in large containers. Ask cleaning
staff to change the disinfectants when they become bloody or cloudy
or when the chlorine odour is no longer detectable.
- Obtain additional
patient supplies. Make sure each patient has a bed and mattress or sleeping
mat. Designate medical equipment for use with each VHF patient (for
example, a thermometer, a stethoscope, and a blood-pressure cuff for
each patient). If there are not enough items available to provide one
per patient, be sure to clean and disinfect the items before use with
the next patient.
- Make sure schedules
are carried out as planned for collecting, transporting and burning
infectious waste daily. Make sure that burning is supervised and that
security of the burning site is maintained.
- Initiate community
education activities.
|
Annex 5 Making Protective Clothing |
 |
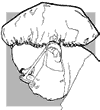 |
A
homemade
headcover |
Instruction on
Making Headwear
Materials needed:
Elastic 3/4 meter
Cotton cloth 51 cm2 (20 square inches)
1. Cut a round piece
of cotton cloth that is 46 to 50 cm (18 to 20 inches) in diameter.
2. Sew elastic on
the edge and shape a circle 18 cm (7 inches) in diameter.
Instruction on
Making Gown
Materials needed:
1.5 meters cotton cloth to make one gown
Instruction
on Making Aprons
Materials needed (to make 2 aprons):
1 1/4 meters plastic sheeting or plastic cloth used for covering tables
91 cm (36 inches) sewing tape
Instruction on
Making a Cotton Mask
1 meter cotton cloth to make at least 2 masks
50 cm in second colour
to make the inside of the masks
1. Cut 4 pieces of
cotton cloth to the size shown.
2. Cut 1 piece from
a different colour. Use it as the inside of the mask.
3. Sew the 5 pieces
together and gather or pleat the vertical sides to 13 cm (5 inches) long.
Sew all pieces in place. 28 to 30 cm (11 to 12 inches) 20 cm (8 inches)
13 cm (5 inches)
4. Sew on ties.
|
 |
 |
 |
| Infection
Control For VHFs Manual |
|
|
 |
 |
|
| Sections
on this page |
|
|
 |
 |
|
|
 |
