 |
 |
| Malaria
Home > |
 |
Laboratory
Diagnosis of Malaria in the United States
|
 |
 |
Image
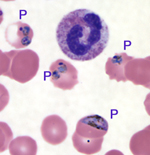
from a blood smear from a 48-year old woman who developed Plasmodium
falciparum malaria after travel to the Dominican
Republic. Examination under the microscope at 1000-fold
magnification shows four of the red blood cells infected
by parasites (“P”). (CDC photo) |
The Importance of Laboratory Diagnosis
Each year in the United States over
a thousand persons come
down with malaria.
Most are travelers who became infected while visiting a malaria
risk area without taking the necessary precautions.
Because malaria can be a severe, even fatal disease, these patients
must receive a prompt and accurate diagnosis, permitting a timely
treatment. The clinical diagnosis, where malaria is suspected
based on the history, symptoms and clinical findings, must always
be confirmed by a laboratory diagnosis.
Microscopy
Microscopy is
the established method for laboratory diagnosis of malaria. A
drop of the patient’s blood is collected by fingerprick,
or from a larger venous blood specimen. It is then spread on
a glass slide (“blood smear”), dipped in a reagent
that stains the malaria parasites (Giemsa stain), and examined
under a microscope at a 1000-fold magnification. Malaria
parasites are
recognizable by their physical features and by the appearance
of the red blood cells that they have infected. These characteristics
often allow the laboratorians to identify the
type (species) of parasite causing the infection, a finding that will guide
the treatment.
The laboratorian can also assess the percentage
of red blood cells that are infected, a measure of severity
of the infection.
 |
A laboratorian
at the Georgia Public Health Laboratory performs PCR, a
back-up diagnostic test for malaria; CDC has assisted state
public health laboratories in introducing PCR techniques
for malaria and other parasitic diseases. (CDC photo) |
Other Laboratory Tests
In addition to microscopy, other methods have been developed
recently for detection of malaria parasites. Parasite antigens
and other products can be detected by rapid “dipstick” tests,
and parasite DNA can be detected by polymerase chain reaction
(PCR). PCR is
currently the most accurate test and can identify low levels
of infection not detectable by other methods.
Serology detects
antibodies against malaria parasites. Such antibodies are produced
by the immune response of the infected person and can persist
in the blood for several months after the infection is over.
Thus, serology measures a person’s past experience with
malaria, but does not necessarily detect current infections.
While microscopy is a routine test, PCR and serology can be
performed only in specialized reference laboratories, and the
kits for “dipstick” tests are not yet approved by
the Food and Drug Administration (FDA) for use in the United
States.
 |
Microscopy
is the established method for laboratory confirmation of
malaria; here, a laboratorian at CDC’s reference
diagnostic laboratory for parasitic diseases. (CDC
photo) |
Laboratories Working Together
The microscopic diagnosis of malaria is initially made in hospitals
or commercial laboratories. When unsure about the diagnosis,
these laboratories can send their specimens to the Department
of Health of their state for further review. If needed, the state
laboratories can request additional diagnostic assistance from
the national reference laboratory at CDC’s Division of
Parasitic Diseases. Every year CDC performs malaria laboratory
tests (microscopy, PCR, serology) on approximately 300 specimens
sent by state health departments or other laboratories.
This close collaboration between laboratories is valuable because
malaria is rarely seen in the United States. Consequently, laboratorians
are too often unfamiliar with malaria parasites and may fail
to detect malaria parasites or to identify correctly the infecting
species of parasites. Being able to send specimens to
a more specialized laboratory allows laboratories to provide
more accurate diagnoses and to improve their diagnostic skills.
 |
Participants
at a training workshop on bloodborne diseases in Albuquerque,
New Mexico (August 2005) practice their skills at blood
smears. (CDC
photo) |
Strengthening the Laboratory Diagnosis of Malaria in the United
States
In addition to its reference functions, CDC offers training
workshops on diagnosis of bloodborne diseases (malaria and babesiosis)
for laboratory personnel throughout the United States. CDC also
provides Wed-based training through DPDx,
a Web site for laboratory identification of parasites of public
health concern. The Web site contains information about diagnosis
of malaria as well as other parasites, and sends out diagnostic
quizzes at monthly intervals to a list of over 1,300 subscribers.
DPDx also allows telediagnosis,
where outside laboratories can send by email to CDC digital images
of their microscopy findings, and receive feedback from CDC staff
within minutes or hours. Services offered by DPDx are free of
charge; for more information contact dpdx@cdc.gov.
Page last modified : September
21,
2005
Content source: Division of Parasitic Diseases
National Center for Zoonotic, Vector-Borne, and Enteric Diseases (ZVED)
|
 |
|






