|
 Printer-Friendly Version Printer-Friendly Version
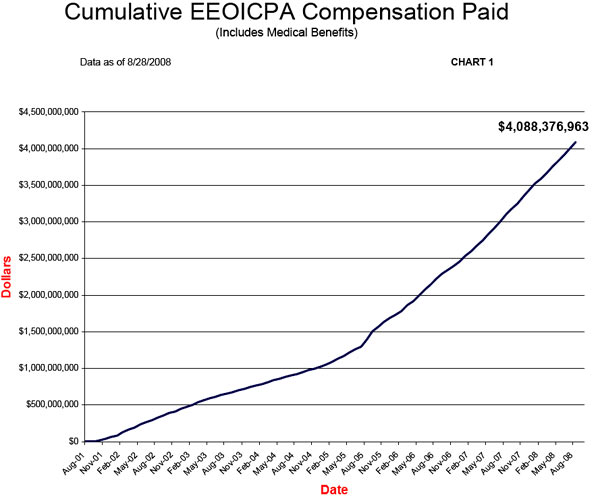
- Payouts under EEOICPA have exceeded $4B (see chart 1).
- Chart 2 illustrates the strides being made in case processing. Dose reconstruction, however, is handled by NIOSH (under the Department of Health and Human Services), not DOL.
- In addition to processing the over $4B in payments to claimants, DOL has engaged in a comprehensive effort to assist anyone who might be eligible under EEOICPA. This has included hundreds of town hall meetings and traveling resource center events. DOL has not only provided information to those who have requested it, but has also actively sought out those who might be in need of such assistance.
The following charts contain new data highlighting the positive performance of the Department of Labor’s (DOL) management of the Energy Employees Occupational Illness Compensation Program Act (EEOICPA). This information is important to those employees, their families, and other interested parties, and is crucial to understanding the state of this important program. This strong performance extends to cases from the former Rocky Flats Plant near Denver, Colorado, which have received particular attention.
In 2000, when EEOICPA was enacted, estimates varied over how many workers would qualify, and thus how much money would be paid out to claimants. But eight years later, DOL has served a far larger audience than even the proponents of the statute predicted at the time. And DOL’s efforts are accelerating, all the while conforming to congressional statutory mandates and the requirements of the National Institute for Occupational Safety and Health (or NIOSH, an agency of the Department of Health and Human Services), DOL’s partner in administering the law.
Performance Highlights
First, DOL has paid over $4 billion for over 43,000 claims, and the pace of those payments is accelerating, not slowing. As shown in Chart 1, total payouts under this eight-year old program have exceeded $4 billion, about $1 billion of which was issued in the last 12 months. These totals far exceed Congress’ expectations at the time of enactment.
Second, DOL has been very successful in rapidly implementing the EEOICPA benefits programs: both the original “Part B” (enacted by Congress in 2000 covering nuclear weapons workers for radiation induced cancer, beryllium disease, and silicosis in certain miners), and the 2004 “Part E” (covering Department of Energy contractor employees for all medical conditions caused by toxic exposures). These complex programs were created from scratch, with many thousands of claims already in-hand, before an infrastructure existed to handle them. Chart 2 below shows how DOL has moved as quickly as possible to reduce the claim backlogs – not once, but twice – and to address the needs of these workers and their families.

| |
Note: Cases at NIOSH for a dose reconstruction must complete that process before DOL can take final action on them. |
We acknowledge that during the start-up periods as we worked through the large initial backlogs, many cases took longer to decide than those families would have liked. However, in spite of the complexity of the cases themselves, DOL expects to achieve “steady-state” for both Parts B and E by October 2008: the number of cases pending an initial determination at DOL will be approximately equal to the number of cases received in the most recent six months. New cases coming in will receive prompt and sympathetic service from DOL.
Cases that require a dose reconstruction by NIOSH have averaged more than two years to complete, and over 7,000 are still pending there. We sympathize with families who have to wait for that complicated process to be completed, but it was dictated by Congress. DOL can only move forward with such cases after NIOSH has completed its work.
Third, DOL exerts considerable effort to help people file claims, navigate our system, and deal with a statute that is complex – with multiple facets and requirements. For example, we advise those approved under Part B of the program who may also be eligible for benefits under Part E about their additional potential eligibility. Likewise, when Part E claimants are approved for their initial benefit, we also tell them what they need to do to claim impairment or wage-loss benefits.
Because the Department was concerned that some workers were not following up to claim those benefits, we initiated a series of extraordinary efforts to make sure those claimants knew their rights. Specifically, DOL’s Resource Centers were tasked to contact all those who might be eligible for such benefits (including new Part E beneficiaries), and to directly assist them in filing for and pursuing those benefits. These efforts, plus ongoing counseling and assistance for all who request it, are in addition to hundreds of public town hall, “traveling resource center” and roundtable meetings DOL has conducted in all the affected communities to get information about these complex programs to all who need it. From the beginning, DOL has actively set out to help people develop and support their claims, and we continue to improve our tools for doing so.
Fourth, DOL strives in every case to administer this program in accord with the law and relevant regulations. Inevitably, some claims will be judged to fall outside the legal eligibility criteria, but the program affords claimants with reasonable and prompt vehicles for disputing negative decisions. A comprehensive and easy-to-access review process is available via our Final Adjudication Branch if a claimant believes the initial (“recommended”) determination was incorrect. Claimants may request reconsideration of such decisions, and they may appeal our final decisions to Federal district court if they believe the outcome was incorrect, or that the regulations and procedures do not faithfully carry out the law. These review and appeal processes are there to correct individual or even systemic errors, and they work. The fact that exceedingly few cases have been appealed to Federal court indicates that DOL is abiding by the parameters Congress put into law when it enacted EEOICPA.
In summary, the Department is effectively administering the EEOICPA program, as enacted by Congress and modified by HHS Special Exposure Cohort declarations. Worker advocates, claimant groups, and some Congressional members have expressed the desire to broaden eligibility beyond the limits originally established by Congress and HHS. Their arguments for legislative changes such as adding more extensive SEC coverage, including additional cancers under the SEC presumptions, broadening the eligibility criteria for Part E survivors to include adult children, and other amendments, are a normal part of the political process. However, DOL’s responsibility is to adjudicate claims fairly and promptly under the existing law. With respect to those aspects of the program under DOL authority, that is exactly what is happening.
| |
|



