Respiratory Diseases - America's Children and the Environment: A First View of Available Measures
Respiratory Outcomes in Children: Asthma and Chronic Bronchitis
Asthma is the most common chronic disease among children and is a costly disease in both human and monetary terms.41 Children with asthma may need to limit daily activities to control or prevent asthma attacks and often require long-term use of medications. Extreme exacerbation of asthma can lead to emergency room visits, hospitalizations, and sometimes death. The tendency to develop asthma can be inherited, but not all children with asthma have a family history of the disease. Exposures to indoor and outdoor sources of biological and chemical environmental contaminants have been shown to cause asthma or exacerbate existing asthma. Exposures to outdoor air pollutants, such as particulate matter, have been shown to exacerbate asthma. Chronic bronchitis also is a condition in children that has been associated with exposure to air pollutants, including particulate matter and ozone.42-43

- Between 1990 and 1995, the number of children with asthma increased by about 30 percent, from 5.8 percent in 1990 to 7.5 percent in 1995. The number of children with asthma in the United States increased by 75 percent from 1980 to 1994. A slight decrease in asthma rates occurred between 1995 and 1996.
- The number of children with chronic bronchitis increased slightly from 5.4 percent in 1990 to 5.7 percent in 1996.
- Some environmental factors may cause children to develop asthma, but the causes of asthma are not completely understood. In a recent report, the Institute of Medicine identified house dust mites as an agent known to cause asthma, and cockroaches and tobacco smoke as other indoor sources suspected to cause asthma.41
- Other environmental factors may increase the severity or frequency of asthma in children who have the disease. Children with asthma are particularly sensitive to outdoor air pollution such as ozone, particulate matter, and sulfur dioxide. These pollutants can exacerbate asthma, possibly leading to an increased use of medication, visits to doctors' offices, and trips to emergency rooms. In severe cases asthma can lead to hospital admissions and even death.
Prevalence of Asthma by Race and Income
Children of lower-income families and children of color are more likely to have asthma. These children often have less access to medical care, which can increase the severity and impact of their illness. Data for 1997-1998 show that the percentage of children with asthma differs by racial and ethnic groups, and by poverty level.
In 1997, the method for measuring asthma among children was changed. Estimates for the percentage of children with asthma are lower in 1997-1998 than in 1996, but it is not clear whether this is due to an actual decrease in the percentage of children with asthma or the change in how asthma is measured.

- In 1997-98, 5.4 percent of all children had asthma.
- Non-Hispanic Black children living in families with incomes below the poverty level have the highest rates of asthma of any group: 8.3 percent of children.
- Approximately 5 percent of both White non-Hispanic children and Hispanic children have asthma.
- Children living in families with incomes below the poverty level had higher rates of asthma, 6.2 percent, than those children living in families at or above the poverty level, 5.3 percent.
Asthma Hospitalizations
The rate of children hospitalized for asthma is another important measure because it represents the most severe cases-those in which asthma could not be controlled on an outpatient or emergency department basis.
Only a fraction of children with asthma are admitted to the hospital. Hospitalization for asthma can be related to a number of factors, including air pollution and lack of access to primary health care. Studies conducted in the northeastern United States indicate that air pollution during the summer was associated with approximately 6-24 percent of all hospital admissions for asthma.44
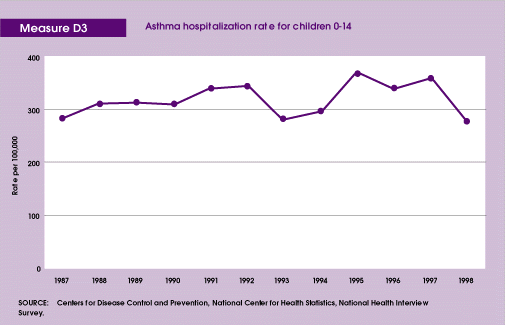
- The asthma hospitalization rate for children aged 0-14 increased from 284 per 100,000 in 1987 to 369 per 100,000 in 1995, and then dropped to 277 per 100,000 in 1998.
- Children aged 0-14 represent 38 percent of asthma hospitalizations for all ages (children and adults) during 1998.45
- Asthma hospitalizations accounted for 7 percent of all hospitalizations for children aged 0-14 in 1998, and asthma was the fourth leading cause of non-injury-related hospital admissions.45
- Outdoor air pollutants such as particulate matter and ozone are associated with increased emergency room visits and hospital admissions.42-43
- Exposure to two other important air pollutants, nitrogen dioxide and sulfur dioxide, has been shown to decrease lung function in asthmatics.46
![[logo] US EPA](https://webarchive.library.unt.edu/eot2008/20081108082951im_/http://www.epa.gov/epafiles/images/logo_epaseal.gif)