Maternal and Child Health
Importance and Measures
| Type of statistic |
Number |
| Mortality |
| Number of maternal deaths (2004) |
54023 |
| Number of infant deaths (2004) |
27,8962 |
| Demographics |
| Number of children under 18 (2005) |
73,469,98424 |
| Number of babies born in United States (2004) |
4,115,59025 |
| Cost |
| Total cost of health care for children (2002) |
$79 billion26 |
| Cost effectiveness of vision screening for children |
$0-$14,0005 |
| Cost effectiveness of childhood immunization seriesxvii |
cost saving5 |
Note: Statistics may vary from previous years due to revised and updated source statistics or addition of new data sources.
Measures
The NHQR tracks several prevention and treatment measures related to maternal and child health care throughout the report. The core report measures highlighted in this section are:
- Receipt of prenatal care in the first trimester.
- Receipt of all recommended immunizations by young children.
- Dental visits by children.
- Counseling parents about healthy eating in children.
- Hospital admissions for pediatric gastroenteritis.
In addition, one supplemental measure is presented:
- Weight monitoring of overweightxviii children.
xvii The childhood immunization series includes vaccinations for diphtheria-tetanus-pertussis; measles-mumps-rubella; inactivated polio virus; Haemophilus influenzae type B; hepatitis B; and varicella.
xviii Children and youth can be categorized as acceptable, underweight, at risk of overweight, or overweight. Children with body mass index values at or above the 95th percentile of the sex-specific body mass index growth charts are categorized as overweight.
Return to Contents
Findings
Prevention: Prenatal Care in the First Trimester
Pregnant women are at risk for high blood pressure, gestational diabetes, and other disorders. Prenatal care is a preventive service intended to identify and manage risk factors in pregnant women and their unborn children in order to improve the chances of a healthy mother and child during pregnancy, birth, and early childhood. Prenatal care is recommended during the first trimester and throughout pregnancy.
Figure 2.27. Women of all ages delivering live births who received prenatal care in the first trimester of pregnancy, 1998-2004
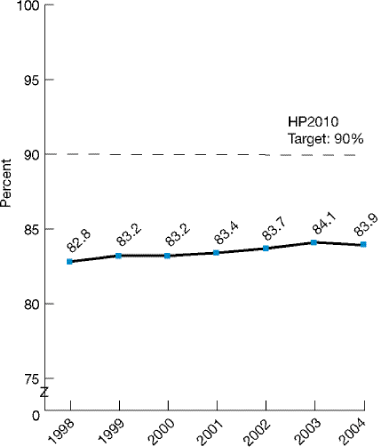
Source: Centers for Disease Control and Prevention, National Center for Health Statistics, National Vital Statistics System—Natality, 1998-2004.
Reference population: Women with live births.
- The percentage of women who received prenatal care in the first trimester of pregnancy increased gradually from 82.8% in 1998 to 83.9% in 2004 (Figure 2.27).
- As of 2004, the percentage of women who received prenatal care in the first trimester of pregnancy had not yet achieved the Healthy People 2010 target of 90%. At the current average annual rate of change, this target is not projected to be met.
Prevention: Receipt of All Recommended Immunizations by Young Children
Immunizations are important for reducing mortality and morbidity. They protect recipients, as well as others in the community who cannot be vaccinated, from illness and disability. Recommended vaccines for children ages 19-35 months include four doses of diphtheria-tetanus-pertussis vaccine, three doses of polio vaccine, one dose of measles-mumps-rubella vaccine, three doses of H. influenzae type B vaccine, and three doses of hepatitis B vaccine.
Figure 2.28. Children ages 19-35 months who received all recommended vaccines, 1998-2005
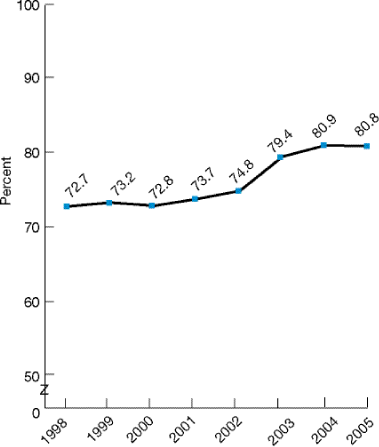
Source: Centers for Disease Control and Prevention, National Center for Health Statistics, National Immunization Survey, 1998-2005.
Reference population: U.S. civilian noninstitutionalized population: children ages 19-35 months.
Note: The vaccines included in this measure are based on the corresponding Healthy People 2010 objective, which does not include varicella vaccine or vaccines added to the recommended schedule after 1998 for children up to 35 months of age. More information can be found in the Measure Specifications Appendix.
- From 1998 to 2005, the percentage of children ages 19-35 months who received all recommended vaccines increased from 72.7% to 80.8% (Figure 2.28).
Prevention: Children's Dental Care
According to the National Institute of Dental and Craniofacial Research, presence of dental caries is the single most common chronic disease of childhood, occurring five to eight times as frequently as asthma, the second most common chronic disease in children.27 Regular dental visits help to improve overall oral health and prevent dental caries.
Figure 2.29. Children ages 2-17 with a dental visit in the past year, 2000-2004
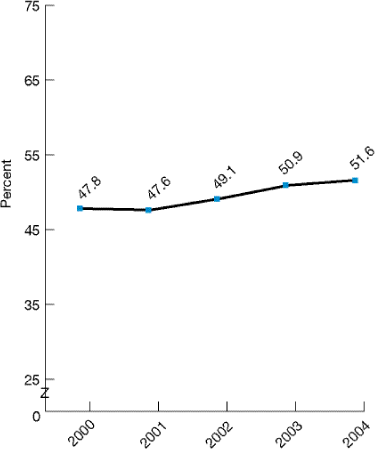
Source: Agency for Healthcare Research and Quality, Medical Expenditure Panel Survey, 2000-2004.
Reference population: U.S. civilian noninstitutionalized population: children ages 2-17.
Note: Rates are age adjusted. Dental visit is based on event data.
- The percentage of children ages 2-17 who visited a dentist in the past year improved from 47.8% in 2000 to 51.6% in 2004 (Figure 2.29).
Prevention: Counseling Parents About Healthy Eating in Children
Childhood represents a period when healthy, life-long habits of diet and exercise can be formed, and physicians play an important role in encouraging these healthy behaviors in children. Overweight and obesity during childhood often persist into adulthood, with consequences that are numerous and costly. Unfortunately, the prevalence of overweight and obesity among children has risen dramatically in recent decades.28
The American Academy of Pediatrics recommends that pediatricians discuss and promote healthy diets with their patients.28
Figure 2.30. Children ages 2-17 for whom a doctor or other health care provider ever gave advice about healthy eating, by age group, 2001-2004
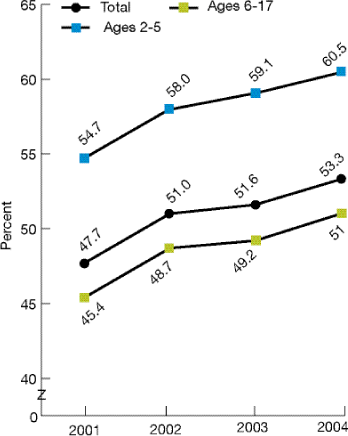
Source: Agency for Healthcare Research and Quality, Medical Expenditure Panel Survey, 2001-2004.
Reference population: U.S. civilian noninstitutionalized population: children ages 2-17.
Note: Rates are age adjusted.
- Parents of only just over half of all children reported receiving advice on healthy eating. However, from 2001 to 2004, the proportion of children for whom a doctor or other health care provider ever gave advice about healthy eating improved from 47.7% to 53.3% (Figure 2.30).
- The proportion of children for whom a doctor or other health care provider ever gave advice about healthy eating rose from 2001 to 2004 for both age groups—children ages 2-5 (from 54.7% to 60.5%) and children ages 6-17 (from 45.4% to 51.0%).
- In all four data years, advice about healthy eating from a doctor or health provider was less likely for children ages 6-17 than for children ages 2-5.
Prevention: Weight Monitoring of Overweight Children
Pediatricians are advised to monitor body mass index and excessive weight gain in children in order to recognize and address cases of overweight and obesity.28 When health care providers alert young patients and their parents about their overweight status, a new opportunity is created to develop healthy dietary and exercise habits that may be carried into adulthood.29
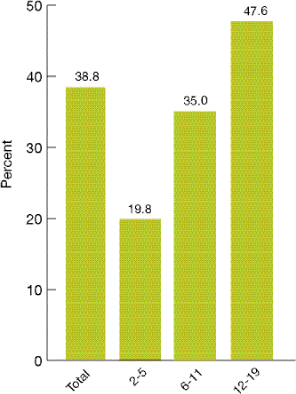
Figure 2.31. Overweight children and adolescents ages 2-19 whose parents were told by a doctor or health professional that the child was overweight, by age group, 1999-2004
Source: Centers for Disease Control and Prevention, National Center for Health Statistics, National Health and Nutrition Examination Survey, 1999-2004.
Reference population: Civilian noninstitutionalized population ages 2-19.
Note: Overweight children are identified using age- and sex-specific reference data from the 2000 Centers for Disease Control and Prevention body mass index (BMI) for age growth charts. Children and youth can be categorized as acceptable, underweight, at risk of overweight, or overweight. Children with BMI values at or above the 95th percentile of the sex-specific BMI growth charts are categorized as overweight.
- During 1999-2004, 38.8% of overweight children and teens ages 2-19 were told by a doctor or health professional that they were overweight (Figure 2.31).
- During 1999-2004, overweight children ages 2-5 (19.8%) and 6-11 (35.0%) were less likely than overweight children ages 12-19 (47.6%) to be told by a provider that they were overweight.
Treatment: Hospital Admissions for Pediatric Gastroenteritis
Pediatric gastroenteritis can develop into a life-threatening condition due to dehydration, especially among infants. Proper outpatient treatment of gastroenteritis may prevent hospitalization, and lower hospitalization rates may reflect access to better quality care.
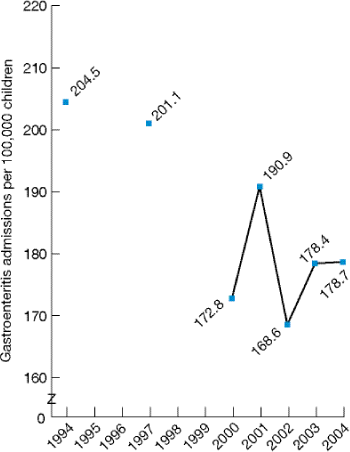
Figure 2.32. Hospital admissions for pediatric gastroenteritis per 100,000 population, 1994, 1997, and 2000-2004
Source: Agency for Healthcare Research and Quality, Healthcare Cost and Utilization Project, Nationwide Inpatient Sample, 1994, 1997, and 2000-2004.
Denominator: U.S. population under age 18.
Note: Adjusted by age and gender to the total U.S. population for 2000 as the standard population. Data were analyzed for two selected historical years (1994, 1997) and annually with each NHQR (2000-2004).
- From 1994 to 2004, admissions for pediatric gastroenteritis fell from 204.5 to 178.7 per 100,000 children (Figure 2.32).
Return to Contents
Mental Health and Substance Abuse
Importance and Measures
| Type of statistic |
Number |
| Mortality |
| Rank among causes of death in the United States—suicide (2004) |
11th2 |
| Alcohol-related motor vehicle deaths (2005) |
16,88530 |
| Students grades 9-12 who have seriously considered suicide (2005) |
16.9%31 |
| Prevalence |
| People 12 and over with alcohol and/or illicit drug dependence or abuse (2005) |
22.2 million (9.1%)32 |
| Adults age 18 and over with serious psychological distress (2005) |
24.6 million (11.3%)32 |
| Adults age 18 and over with serious psychological distress and substance dependence or abuse (2005) |
5.2 million (21.3%)32 |
| Adults with a major depressive episode during the past year (2005) |
15.8 million (7.3%)32 |
| Lifetime prevalence of major depressive disorder (2005) |
30.8 million (14.2%)32 |
| Lifetime prevalence of dysthymic disorder |
2.5%32 |
| 12-month prevalence estimates (2001-2003) for adults with: |
| Any mental disorder |
28.1%33 |
| Anxiety disorders |
18.7%33 |
| Mood disorders |
9.7%33 |
| Impulse-control disorders |
10.4%33 |
| Substance abuse disorders |
7.2%33 |
| Cost |
| Direct medical expenditures for substance abuse and mental disorders (2001 est.) |
$104 billion34 |
| Cost effectiveness of problem drinking screening and brief counseling |
$14,000-$35,000/QALY5 |
Note: Statistics may vary from previous years due to revised and updated source statistics or addition of new data sources.
Measures
The NHQR tracks measures for the treatment of diagnosable mental disorders in general, substance abuse, and major depression. Mental health treatment is defined as counseling, inpatient care, outpatient care, or prescription medications for problems with emotions or anxiety and does not include alcohol or drug treatment. Because improved outcomes are correlated with treatment completion and length of stay in substance abuse treatment, the measure of the quality of substance abuse treatment presented in this report is the rate of persons who complete all parts of their treatment plan. This section highlights three core measures of mental health and substance abuse treatment:
- Suicide death rate.
- Receipt of treatment for illicit drug use.
- Receipt of treatment for depression.
Return to Contents
Findings
Prevention: Suicide Deaths
Suicide is often the result of untreated depression and may be prevented when its warning signs are detected and treated.
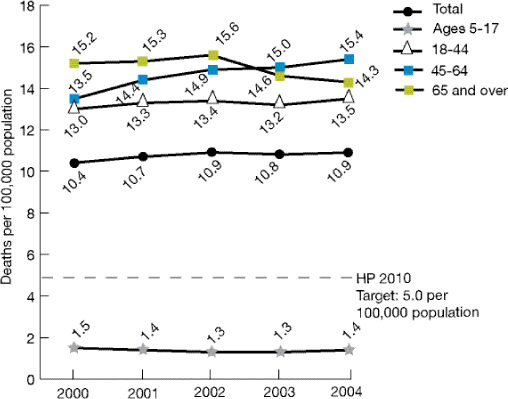
Figure 2.33. Suicide deaths per 100,000 population, 2000-2004
Source: Centers for Disease Control and Prevention, National Center for Health Statistics, National Vital Statistics System—Mortality, 2000-2004.
Reference population: Age 5 and over.
Note: Total rate is age adjusted to the 2000 U.S. standard population.
- From 2000 to 2004, the suicide death rate increased for the population as a whole (from 10.4 to 10.9 deaths per 100,000 population), moving further away from the Healthy People 2010 target of 5.0 suicide deaths per 100,000 population (Figure 2.33).
- From 2000 to 2004, the rate of suicide deaths per 100,000 population for children ages 5-17 remained relatively stable. During the same period, the rate decreased for adults age 65 and over (from 15.2 to 14.3) and increased for adults ages 45-64 (from 13.2 to 15.4).
- In all five data years, the rate of suicide deaths was higher for adults age 65 and over than for adults ages 18-44, and lower for children ages 5-17 than for adults ages 18-44.
- Continuation of these or similar rates could account for at least 160,000 deaths resulting from suicide over the period from 2005 to 2010.
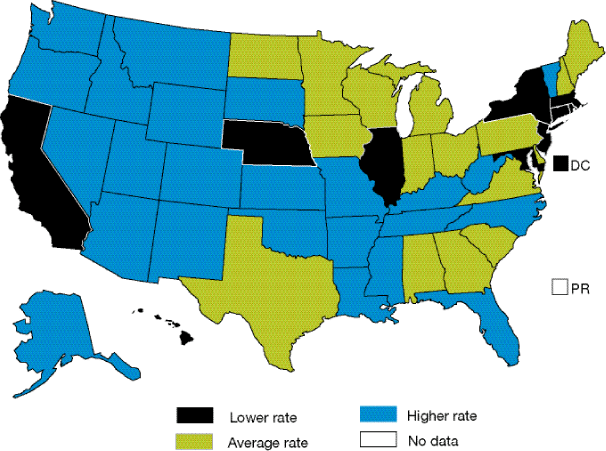
Figure 2.34. State variation: Suicide deaths per 100,000 population, 2004
Source: Centers for Disease Control and Prevention, National Center for Health Statistics, National Vital Statistics System—Mortality, 2004.
Key: Above average = rate is significantly above the reporting States average in 2004. Below average = rate is significantly below the reporting States average in 2004.
Reference population: U.S. population.
Note: Rates are age adjusted to the 2000 standard population. The "reporting States average" is the average of all reporting States (51 in this case, including the District of Columbia), which is a separate figure from the national average.
- The State rates of suicide deaths per 100,000 population ranged from a low of 5.7 to a high of 23.4 (Figure 2.34).
- In 2004, 11 Statesxix had rates of suicide deaths that were lower than the reporting States average of 10.8 per 100,000 population, with a combined average rate of 7.8 per 100,000 population. No State has yet reached the Healthy People 2010 goal of 5.0 per 100,000 population.
- In 2004, 24 Statesxx had rates of suicide deaths that were higher than the reporting States average, with a combined average rate of 15.3 per 100,000 population.
- Michigan is the only State that showed a significant change in the rate of suicide deaths from 1999 to 2004. Over this period, the rate of suicide deaths in Michigan increased from 9.9 to 10.8 per 100,000 population.
xix The States are California, Connecticut, District of Columbia, Hawaii, Illinois, Maryland, Massachusetts, Nebraska, New Jersey, New York, and Rhode Island.
xx The States are Alaska, Arizona, Arkansas, Colorado, Florida, Idaho, Kansas, Kentucky, Louisiana, Mississippi, Missouri, Montana, Nevada, New Mexico, North Carolina, Oklahoma, Oregon, South Dakota, Tennessee, Utah, Vermont, Washington, West Virginia, and Wyoming.
Treatment: Receipt of Needed Treatment for Illicit Drug Use
Substance abuse is a medical problem that requires timely treatment, not only because of its health effects but also because drug use is associated with other adverse effects, such as violent behavior. In addition, because overall health care costs may be reduced by effective substance abuse and mental health treatment,35, 36appropriate receipt and completion of treatment have both clinical and economic implications.
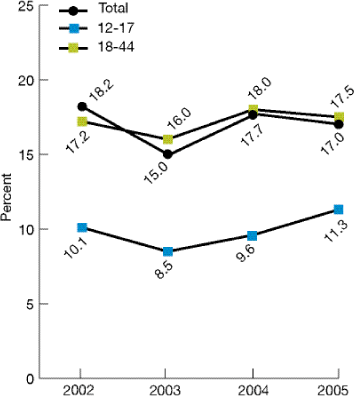
Figure 2.35. Persons ages 12-44 who received needed treatment for illicit drug use, 2002-2005
Source: Substance Abuse and Mental Health Services Administration, National Survey on Drug Use and Health, 2002-2005.
Reference population: Civilian noninstitutionalized population ages 12-44 who needed treatment for any illicit drug use.
Note: Treatment refers to treatment at a specialty facility, such as a drug and alcohol inpatient and/or outpatient rehabilitation facility, inpatient hospital care, or a mental health center.
- Overall, 17.0% of persons ages 12-44 who met criteria for needing treatment for illicit drug use actually received it in 2005. This rate has not changed significantly since 2002 (Figure 2.35).
- Of people who needed treatment for illicit drug use in 2005, only 17.5% of adults ages 18-44 and 11.3% of children ages 12-17 received it. These rates remain statistically unchanged from 2002.
- In all four data years, children ages 12-17 who needed illicit drug treatment were less likely than adults ages 18-44 to receive such treatment.
Treatment: Receipt of Treatment for Depression
Almost 10% of the U.S. population will have a major depressive episode in their lifetime. Treatment can be very effective in reducing symptoms and associated illnesses and returning individuals to a productive lifestyle.
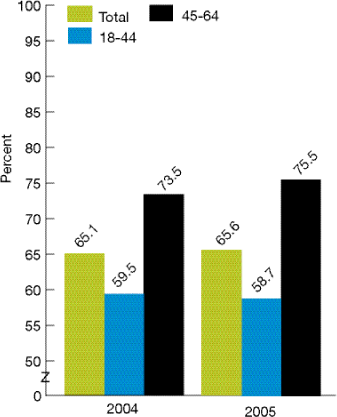
Figure 2.36. Adults ages 18-64 with a history of major depressive episode in the past year who received treatment for depression in the past year, by age group, 2004 and 2005
Source: Substance Abuse and Mental Health Services Administration, National Survey on Drug Use and Health, 2004 and 2005.
Reference population: U.S. civilian noninstitutionalized population ages 18-64.
- In 2005, 65.6% of adults ages 18-64 with a major depressive episode received treatment for depression (Figure 2.36). There was no significant improvement in this measure compared with 2004.
- In 2005, among adults who experienced a major depressive episode, those ages 45-64 (75.5%) were more likely than those ages 18-44 (58.7%) to receive treatment for depression. The 45-64 age group was also more likely to receive treatment in 2004.

