Anupam Tyagi PhD and Jill Morris PhD
Figures

|
Figure 1: A basic decision tree depicting the alternative courses of action of (1) continuing with the current practice with no
explicit use of family history (the top “branch” emanating from the square decision node) versus (2) use of a colorectal cancer
(CRC) family history tool for risk stratification and improved screening (the bottom “branch” emanating from the square
decision node). Chance events, represented by branches emanating from circular chance nodes, are assumed to occur with the
probabilities shown under the respective branches. This illustration assumes that the use of family history motivates 100% of
individuals with strong and moderate family histories to get screened.
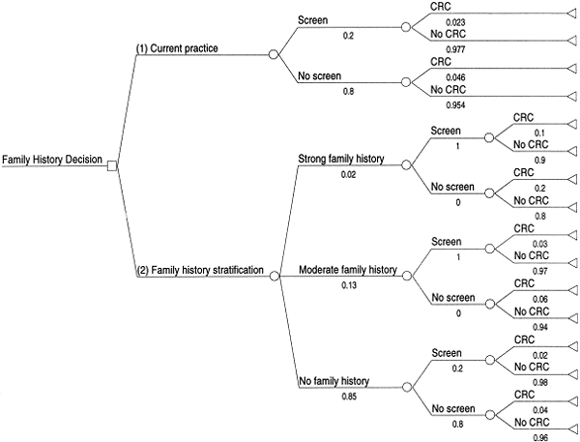

Figure 2: Results of the illustrative decision analysis. The “value added” of using family history (FH) is presented in terms of the
additional colorectal cancer (CRC) cases averted per 100,000 individuals using an FH tool to increase screening among persons
with FH compared with CRC cases averted using current practice (in which 20% of people are screened without regard to FH)
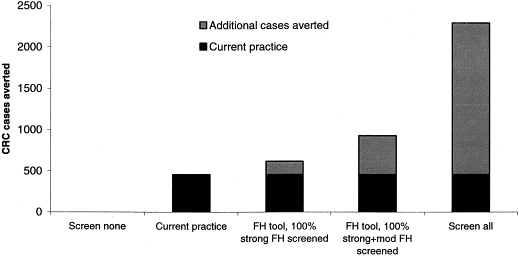

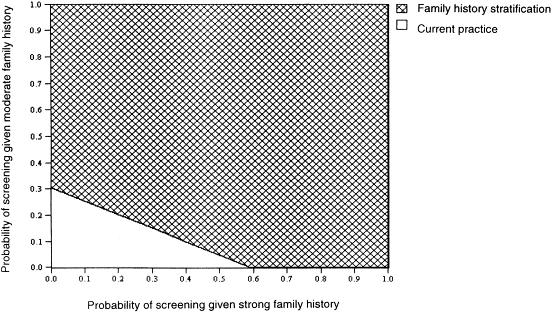
Figure 3: Results from an example sensitivity analysis in which the probability of screening varies from 0 to 1 (analogous to rates
of 0 to 100%) among those with strong family histories (along the x-axis) and moderate family histories (along the y-axis). The
probability of screening under the Current Practice alternative is held constant at 20%. The upper (cross-hatched) region
represents combinations of screening rates for which the Family History Stratification leads to fewer expected CRC cases than
the Current Practice. The smaller (white) region at the lower left represents combinations of screening rates for which the
Current Practice leads to fewer CRC cases. Although this sensitivity analysis varies only the screening rates among those with
family histories, the comparison of the strategies takes into account all cancers, not just cancers among those with family histories.

|





